Clear Sky Science · en
The interface of aging and salt in driving salt-sensitive hypertension: a comparative study in aged and young rats
Why Salt and Aging Matter for Your Blood Pressure
Most of us know that eating too much salt can raise blood pressure, but salt does not affect everyone in the same way, and its impact can change as we age. This study used specially bred rats that are very prone to salt-related high blood pressure to ask a simple question with big implications for people: does a salty diet push blood pressure and damage the kidneys differently in the young and the old?
Different Blood Pressure Surprises in Young and Old
The researchers compared young adult rats with older rats that roughly model late middle age. All were given either a normal-salt diet or a very high-salt diet for five weeks. In both age groups of salt-sensitive rats, blood pressure went up on the salty diet, showing clear "salt sensitivity." But the size of the rise was very different. Young rats had a dramatic jump in blood pressure, while older rats showed a much smaller increase, even though they were just as genetically prone to salt-driven hypertension. In a control strain that is naturally more resistant to salt, blood pressure hardly changed, underscoring that genetics and age interact strongly with diet.
Heart and Arteries: Stronger Push in the Young
To find out why blood pressure reacted so differently, the team used ultrasound scans to look at the heart and major arteries. In young salt-sensitive rats, a high-salt diet made the heart pump more forcefully: stroke volume and cardiac output rose sharply, and measures of how well the heart squeezes improved. Their arteries also showed signs of higher resistance to blood flow, a combination that drives blood pressure up. Older rats, in contrast, started out with weaker heart pumping and stiffer arteries. When they ate more salt, their hearts and vessels did not respond as vigorously—stroke volume and cardiac output rose only modestly, and the change in vascular resistance was blunted. That muted mechanical response helps explain why their blood pressure rose less, even though they were still salt-sensitive.
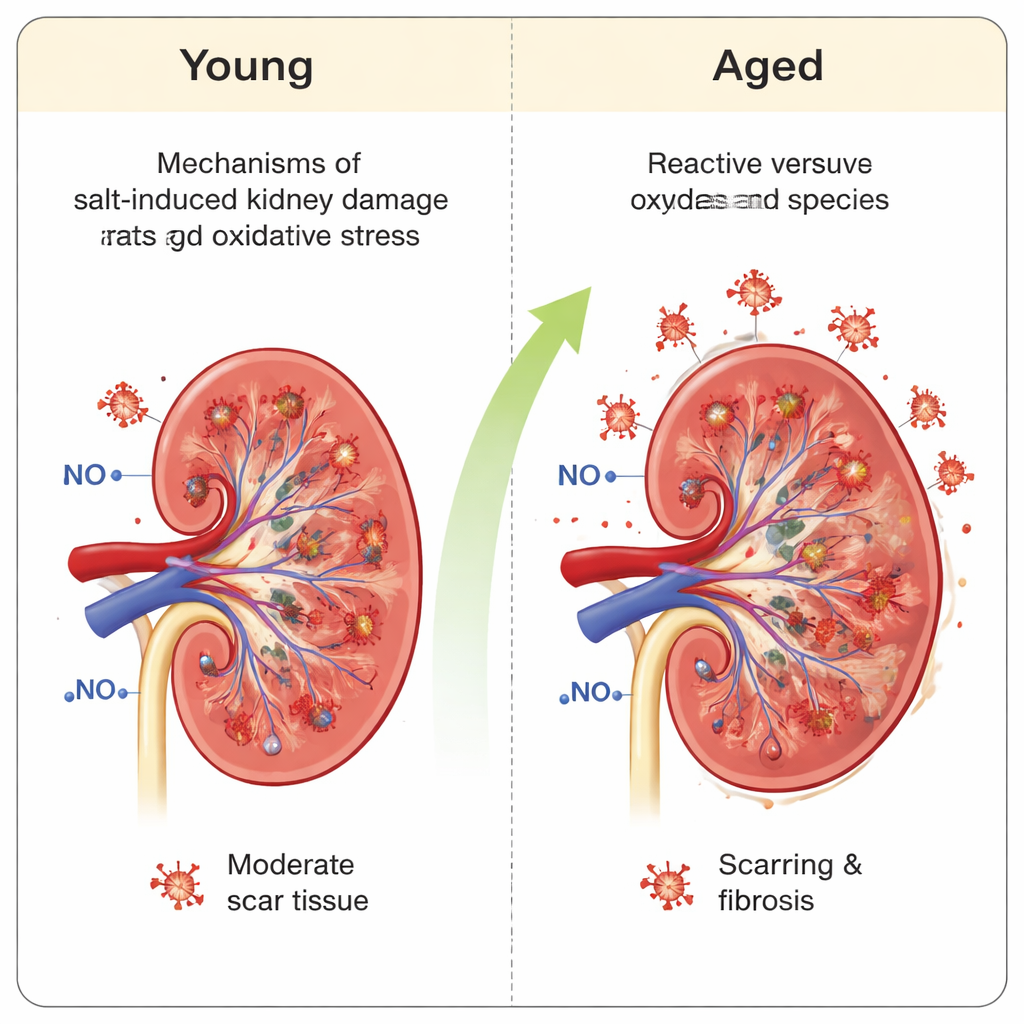
Hidden Chemical Stress in the Kidneys
Blood pressure is only part of the story. The kidneys, which help control both salt balance and blood pressure, came under heavy chemical stress in both young and old rats. A salty diet boosted levels of reactive oxygen species—damaging molecules that signal oxidative stress—in the blood and kidneys. At the same time, several antioxidant defenses, including protective enzymes and glutathione, were weaker. Young rats showed a sharp drop in these defenses when salt was added, tipping their system suddenly toward oxidative damage. Older rats, however, already had low antioxidant capacity before the diet change. High salt did not lower it much further, but because they started from a worse baseline, their kidneys remained under high oxidative stress.
Key Role of a Gas That Relaxes Blood Vessels
The study also focused on nitric oxide, a tiny gas made in blood vessels and kidneys that helps them relax and acts as a natural antioxidant. In young salt-sensitive rats, a high-salt diet cut nitric oxide levels and reduced activity of nitric oxide–producing enzymes, especially in the kidney medulla, the region crucial for salt handling. This loss of a natural vasodilator likely contributed to rising blood pressure. Older rats, in contrast, had consistently low kidney nitric oxide from the start, reflecting age-related decline in this protective pathway. High salt did not change their levels much, but that also meant they lacked the flexibility to adjust blood vessel tone when challenged by extra salt.
When Lower Blood Pressure Hides Greater Kidney Harm
Perhaps the most worrying finding was that older salt-sensitive rats suffered worse kidney damage despite a smaller jump in blood pressure. Blood and urine tests showed more evidence of kidney dysfunction, and microscopic examination revealed more scarring of the tiny filters and more fibrous tissue in the kidney tissue between them. In young rats, a salty diet also damaged the kidneys, but the scarring and fibrosis were noticeably less severe. Together, the results suggest that with aging, the body’s ability to buffer salt-induced damage, especially in the kidneys, weakens even if blood pressure readings look less alarming.
What This Means for People Watching Their Salt
For a layperson, the take-home message is that a salty diet can be harmful in different ways at different ages. In youth, extra salt may cause a strong spike in blood pressure by making the heart pump harder and the vessels clamp down, while also disturbing the balance between harmful oxidants and protective nitric oxide. In older age, the heart and vessels may respond less dramatically, so blood pressure appears less salt-sensitive, yet the kidneys—already running on reduced antioxidant reserves and lower nitric oxide—may be more easily scarred by the same salty load. Although these findings come from rats, they support the idea that limiting salt early in life can prevent long-term programming of high blood pressure, and that continued moderation in salt intake is especially important with aging to protect vulnerable kidneys, even if the blood pressure cuff does not show a large immediate reaction.
Citation: Zeng, L., Xu, L., Chen, M. et al. The interface of aging and salt in driving salt-sensitive hypertension: a comparative study in aged and young rats. npj Aging 12, 32 (2026). https://doi.org/10.1038/s41514-026-00331-7
Keywords: salt-sensitive hypertension, aging and blood pressure, oxidative stress, kidney damage, nitric oxide