Clear Sky Science · en
Small intestinal microbial fiber metabolism dysfunction in celiac disease
Why the Gut’s Fiber Factory Matters in Celiac Disease
Celiac disease is usually explained as a problem with gluten, the protein in wheat, rye, and barley. But this study asks a different question: what happens to the tiny organisms living in the small intestine, and how they handle dietary fiber, when someone has celiac disease? The answers suggest that a “broken” fiber factory in the upper gut may slow healing, and that the right kind of fiber plus the right microbes could one day become part of treatment.
Gluten Trouble and a Missing Support Team
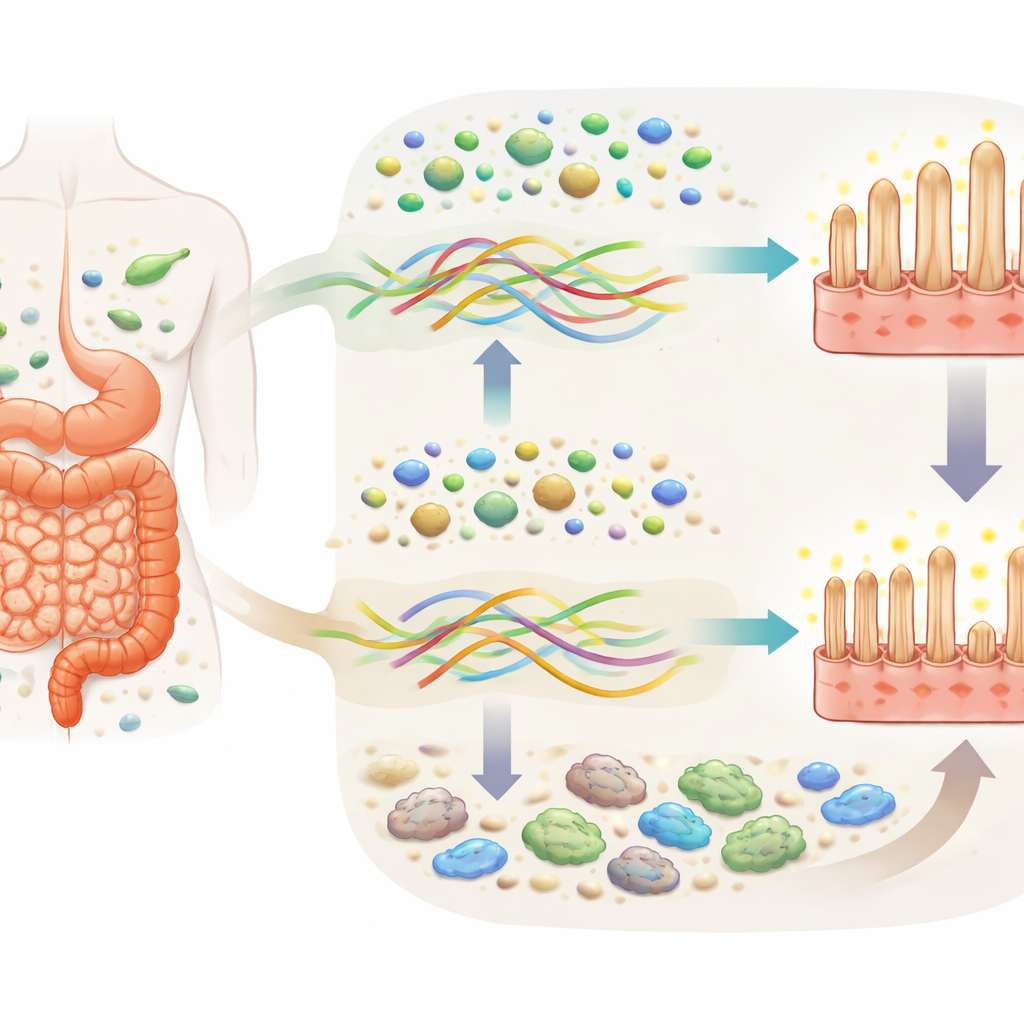
Celiac disease is an immune condition in which eating gluten triggers inflammation and injury in the first part of the small intestine. This area, called the duodenum, normally has fingerlike projections (villi) that absorb nutrients. In celiac disease, these villi shrink and the lining fills with activated immune cells. Most people improve on a strict gluten-free diet, but recovery can be slow and incomplete. At the same time, many gluten-free products are low in fiber, raising concerns about how this might affect gut microbes that rely on fiber as their main fuel.
A Weakened Fiber-Using Microbiome
The researchers collected fluid from the duodenum and stool samples from three groups: people newly diagnosed with celiac disease, patients with celiac disease doing well on a gluten-free diet, and healthy controls. They mapped which bacteria were present and used computational tools and gene tests to estimate what those microbes could do. In both newly diagnosed and treated celiac patients, the small-intestinal community was less diverse and contained fewer fiber-degrading bacteria from a group called Prevotellaceae. Genes that help break down starches and inulin-like fibers were also reduced. Importantly, these shortfalls appeared even when people’s fiber intake was not dramatically different, pointing to an intrinsic loss of microbial capacity rather than just low fiber on the plate.
Fiber Intake, Everyday Diet, and Gut Chemicals
To understand how diet might shape these changes, the team estimated fiber intake with food questionnaires and analyzed plant DNA in stool to see what kinds of plants people were actually eating. Many participants in all groups ate less fiber than public health guidelines suggest, and those with treated celiac disease often relied more on rice and less on gluten-containing grains. Yet this did not fully explain the microbial differences. When the scientists measured short-chain fatty acids—small molecules made when microbes digest fiber—they found that people with active celiac disease had the lowest levels, while treated patients showed partial recovery. This pattern supports the idea that the gut’s fiber-processing machinery is damaged in celiac disease but can improve somewhat after gluten is removed.
Testing Fiber and Helpful Bacteria in Mice
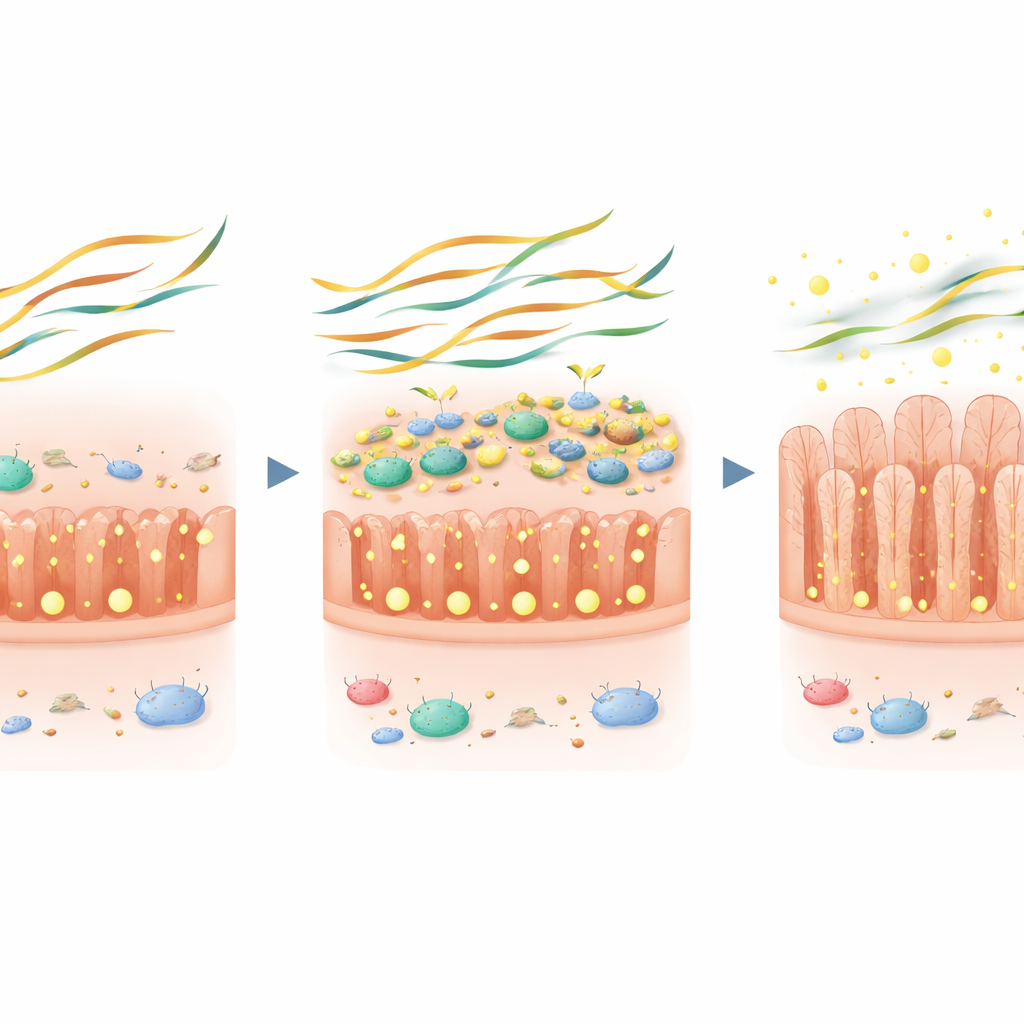
To probe cause and effect, the team turned to mice that carry a human celiac risk gene and can be sensitized to gluten. After inducing gluten-related gut damage, they placed mice on a gluten-free diet alone or a gluten-free diet enriched with either inulin (a soluble plant fiber) or a resistant starch. Mice given inulin had higher levels of short-chain fatty acids in the small intestine and faster healing of their gut lining, with fewer inflammatory cells and taller villi. Resistant starch had more modest benefits. When the same fiber was fed to germ-free mice, it produced little benefit, showing that microbes are required. Finally, when germ-free mice were colonized with a cocktail of Prevotella strains and then fed inulin, their small intestines produced more of these helpful fatty acids, confirming that specific fiber-loving bacteria can restore this lost function.
What This Could Mean for People with Celiac Disease
Taken together, the findings suggest that celiac disease is not just a story about gluten and the immune system. It also involves a disruption of the small intestine’s “fiber economy,” in which key bacteria and their fiber-processing tools go missing. The study points to a future in which tailored fibers like inulin, combined with the right microbial partners, might be used alongside a gluten-free diet to speed healing of the gut lining. While more clinical trials are needed before changing treatment guidelines, this work highlights that supporting the small intestine’s resident microbes could become an important part of caring for people with celiac disease.
Citation: Wulczynski, M., Constante, M., Galipeau, H.J. et al. Small intestinal microbial fiber metabolism dysfunction in celiac disease. Nat Commun 17, 2698 (2026). https://doi.org/10.1038/s41467-026-70644-4
Keywords: celiac disease, gut microbiome, dietary fiber, short-chain fatty acids, Prevotella