Clear Sky Science · en
Vascular invasion-associated gene expression is detectable in pre-surgical biopsies of stage I lung adenocarcinoma
Why This Matters for People With Early Lung Cancer
Many people today are diagnosed with small lung tumors that can be removed surgically. Yet some of these early cancers quietly spread and return, while others never do. Doctors know that one warning sign is when cancer cells sneak into nearby blood vessels, a change called vascular invasion, but this is extremely hard to see under the microscope before or even during surgery. This study shows that tiny samples of a lung tumor already carry a telltale gene activity pattern that reveals whether the cancer has likely invaded blood vessels and is more prone to come back, opening the door to more personalized surgery and follow-up care.
The Hidden High-Risk Subset of Early Lung Tumors
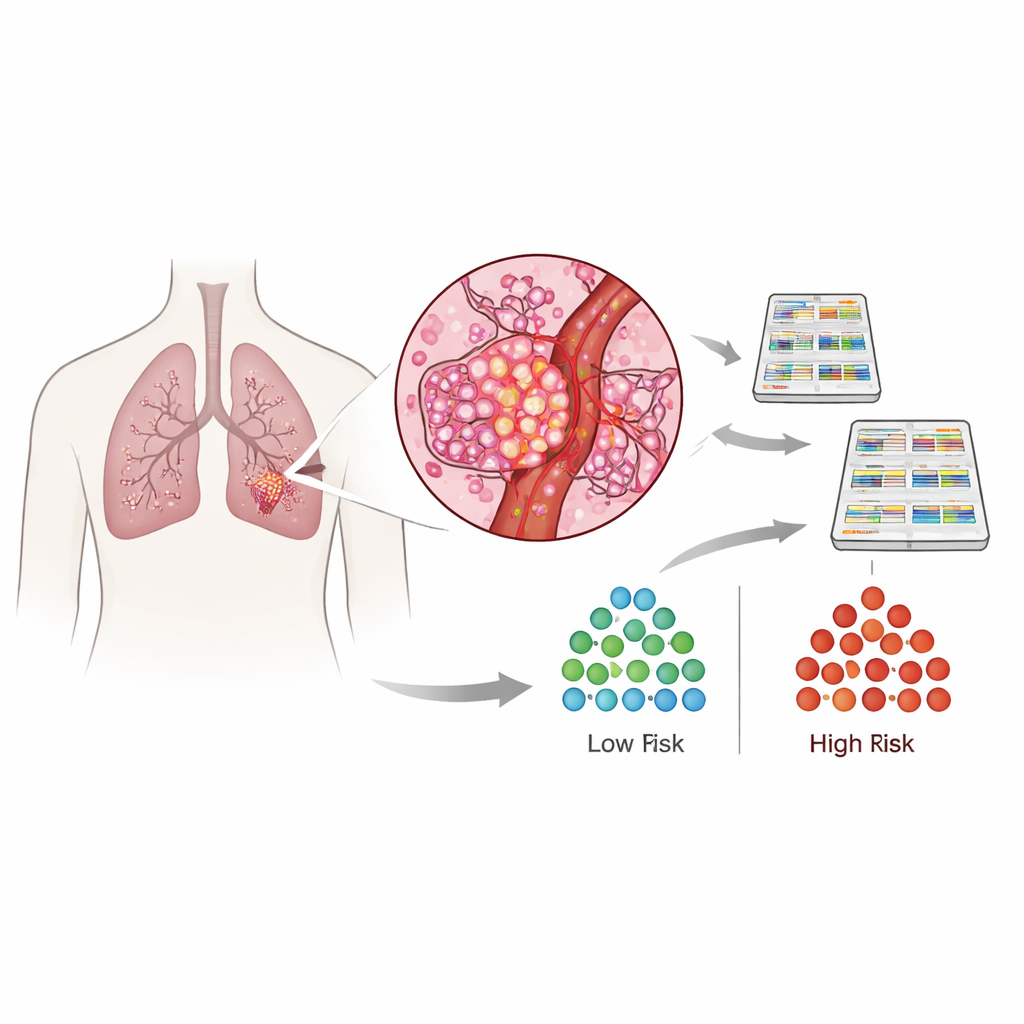
The researchers focused on stage I lung adenocarcinoma, a common form of lung cancer often caught while still small and apparently confined to the lung. Within this group, a major threat is microscopic vascular invasion: clusters of tumor cells that have broken into small veins or arteries, providing a direct route to distant organs. Current grading systems do not fully capture this risk, and pathologists can easily miss these tiny foci, especially in routine slides or in thin biopsy samples taken before surgery. As a result, some patients who might benefit from a larger operation or added drug treatment are not recognized in time. The team set out to find a molecular fingerprint of vascular invasion that could be detected reliably and in very small amounts of tissue.
Reading Vascular Invasion From Tumor Gene Activity
Using RNA sequencing on 162 surgically removed tumors, the scientists measured which genes were turned on or off across each cancer. They identified 474 genes whose activity clearly distinguished tumors with vascular invasion from those with more harmless growth patterns. These genes fell into four clusters. Three clusters were more active in blood-vessel–invading tumors and were linked to fast cell division, the ability of cells to loosen and move through tissue, the building of new blood vessels, and adaptation to oxygen-poor conditions. The remaining cluster was less active in these aggressive tumors and was associated with cell adhesion, growth control, and immune surveillance, features that normally help hold cancer in check. This suggested that vascular invasion is not just a tiny local event, but reflects a broad shift in the tumor’s overall biology.
Mapping Risk Signals Across the Tumor Landscape
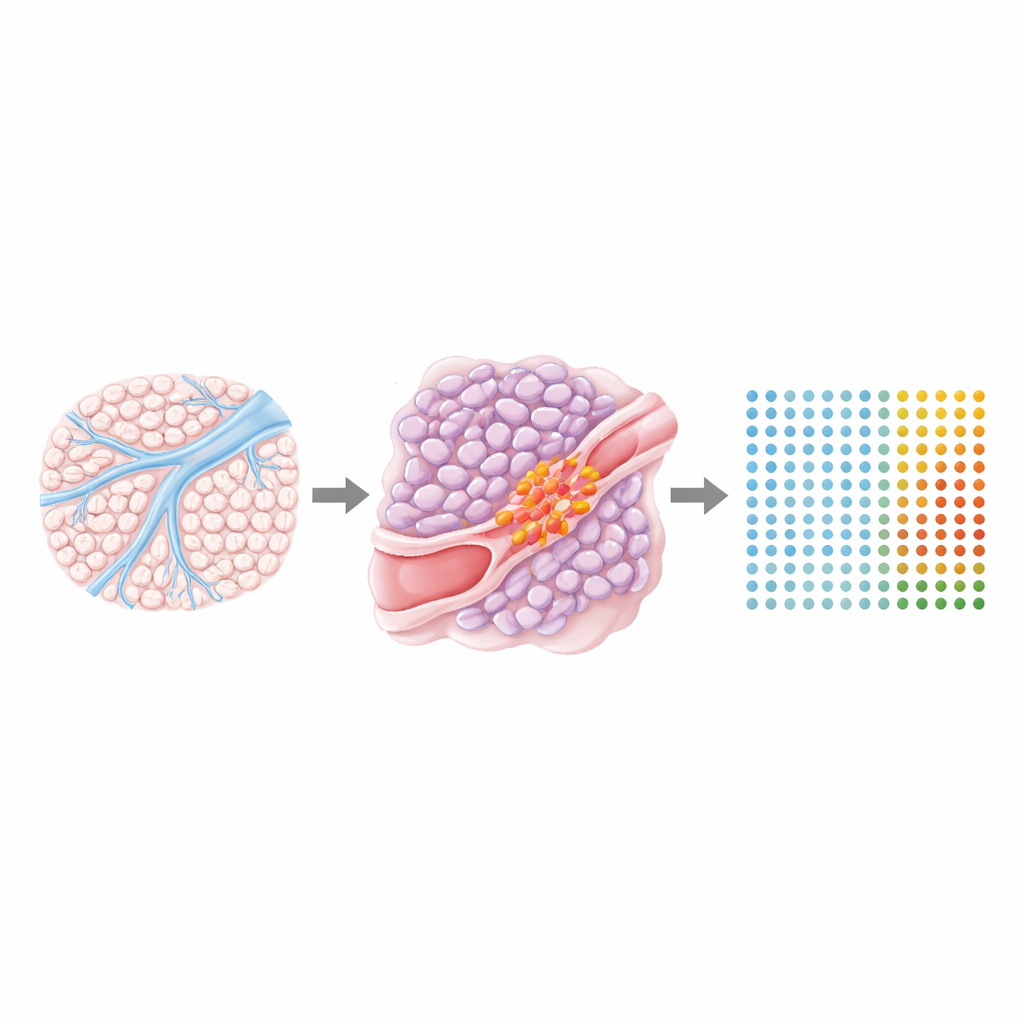
To see where these gene patterns live inside the tumor, the team used spatial transcriptomics, a technology that records gene activity at thousands of tiny spots across a tissue slice while preserving its microscopic image. They analyzed 15 lung cancers, some with and some without vascular invasion, and overlaid gene activity maps with detailed pathology annotations. The high-risk gene clusters were strongly expressed not only at the sites where cancer filled a blood vessel, but also in nearby high-grade tumor regions and in dense, scar-like tissue called desmoplastic stroma that forms around invasive nests. A separate cluster marking less aggressive behavior was enriched in more orderly tumor patterns and in normal-looking lung. This confirmed that the vascular-invasion signature extends well beyond the invaded vessel itself and is shaped by both the cancer cells and the surrounding support cells, particularly specialized fibroblasts that remodel tissue.
Building a Practical Predictor for Doctors
From the larger gene set the researchers distilled a 48-gene predictor and trained a machine-learning model to separate vascular-invasion–positive from negative tumors. In their original patient group and in an independent validation set, this predictor correctly distinguished the two types of tumors with high accuracy and also tracked with the likelihood that cancer would return after surgery. Notably, the predictor did not simply mirror existing microscopic grading features and showed little overlap with changes linked to invasion through lymph vessels, underscoring that blood-vessel invasion is a distinct process. By examining multiple regions within the same tumors, the team found that predictor scores were remarkably stable despite known patchiness inside cancers, suggesting that a single small sample can be informative.
From Needle Biopsy to Tailored Surgery
The most clinically exciting test was whether this gene-based score could be read from routine pre-surgical biopsies, which capture only a sliver of the tumor and rarely show an invaded vessel directly. In a pilot group of 24 patients, the predictor measured in biopsy tissue closely matched scores from the later surgical specimens and accurately forecasted which tumors would show vascular invasion at resection. When accounting for how common vascular invasion is in stage I disease, a low predictor score in a biopsy corresponded to a very high chance that the tumor truly lacked vascular invasion. This means that, after further validation, such a test could help identify patients who are safe candidates for smaller lung-sparing operations, while flagging others who might need more extensive surgery or additional treatments, moving lung cancer care closer to true precision surgery.
Citation: Steiner, D., Sultan, L., Sullivan, T. et al. Vascular invasion-associated gene expression is detectable in pre-surgical biopsies of stage I lung adenocarcinoma. Nat Commun 17, 2581 (2026). https://doi.org/10.1038/s41467-026-70600-2
Keywords: lung adenocarcinoma, vascular invasion, gene expression signature, spatial transcriptomics, biopsy-based risk prediction