Clear Sky Science · en
Acinetobacter baumannii’s lifestyle includes soil-dwelling colonization of decaying plant material and airborne spread
Why this hospital germ’s wild side matters to you
Acinetobacter baumannii is best known as a hard-to-kill hospital germ that shrugs off many antibiotics. This study shows that the same microbe also lives a rich life outdoors—in soil, decaying plants, animals, and even the air. By uncovering where it comes from and how it travels, the work helps explain why this bacterium is so tough and why it repeatedly finds its way into hospitals around the world.

Hidden life in fields, rivers, and bird nests
The researchers started with an unexpected clue: white stork nestlings in Poland often carried A. baumannii in their upper airways, far from any hospital. By following the birds’ diet and surroundings, the team traced the bacterium not to insects or fish, but mainly to small mammals, earthworms, and—most importantly—moist soils rich in rotting plant material along rivers and in compost heaps. Forest soils, even along streams, rarely harbored the bacterium, whereas riverbanks outside forests sometimes acted as “hot spots” where many different strains coexisted side by side.
From rotting plants to the open air
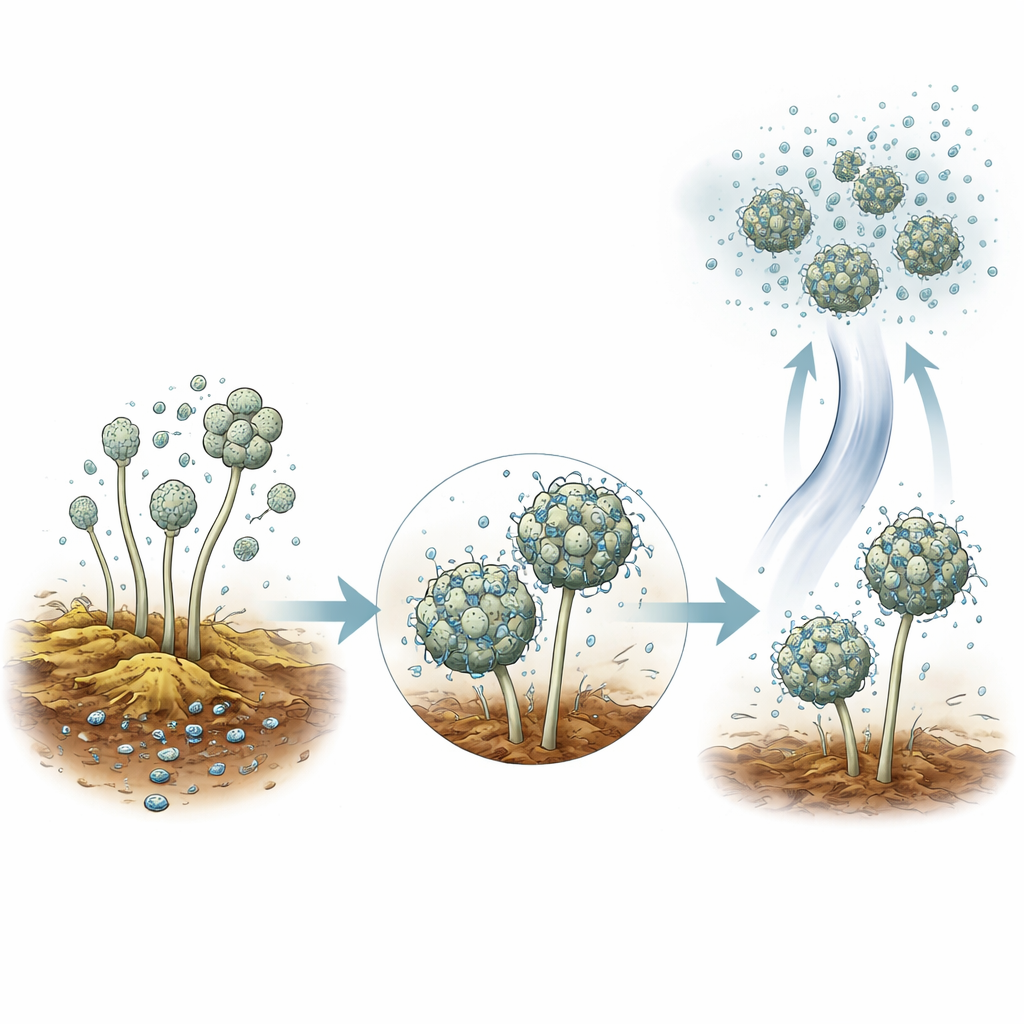
Careful field experiments showed that A. baumannii is drawn to decaying plant matter. When the authors placed sterilized plant scraps in gardens, the material became colonized within a few weeks—even when it was raised above the soil and only accessible through the air. Air traps set just above active compost piles also collected the bacterium. In laboratory work, the team found that A. baumannii readily sticks to spores of common molds such as Aspergillus and Penicillium. Bacteria gradually coated the spores and even slowed their ability to germinate. Because fungal spores easily become airborne from compost and soils, this close partnership offers a simple way for the bacterium to hitch rides into the atmosphere.
Global travelers with ancient roots
To see how these wild strains relate to hospital strains, the team sequenced 401 new genomes from storks, soil, plants, worms, rodents, and other sources, and compared them with hundreds of publicly available genomes. The resulting family tree revealed a remarkable spread: environmental, animal, and human clinical isolates were scattered across the same branches, often differing by only a few DNA changes. Some near-identical relatives were found on different continents, implying that the same lineages had crossed oceans within just a few decades. Based on the rate at which mutations accumulate, the authors estimate that A. baumannii as a species is surprisingly young—on the order of 15,000 years—and underwent rapid diversification around the time humans began large-scale farming and clearing of forests.
A vast toolkit, but little human fingerprint in nature
By combining all the genomes, the researchers estimated that the species’ combined gene set—or pan-genome—contains roughly 51,000 distinct gene families, more than double previous estimates. This huge genetic toolbox likely underlies its ability to adapt to extreme dryness, radiation, disinfectants, and antibiotics. Yet most wildlife and soil isolates carried only a small number of recognized resistance genes and few mobile DNA elements, in contrast to hospital strains that are loaded with such features. That pattern suggests the natural populations being sampled are still relatively untouched by modern antibiotic use, offering a “baseline” view of the species before full hospital adaptation.
What this means for hospitals and public health
The study paints A. baumannii not as a purely man-made problem, but as a naturally airborne, plant- and soil-associated bacterium that has only recently begun to exploit hospitals and livestock facilities as new habitats. Its partnership with fungi, tolerance of harsh conditions, and vast genetic diversity make it well suited for long-distance atmospheric travel and rapid evolution. For a layperson, the takeaway is that infection control cannot focus only on patient-to-patient spread inside hospitals. Seasonal surges, mold-contaminated indoor environments, composting facilities, and broader land-use changes all shape when and how this resilient germ enters human settings—and understanding its outdoor lifestyle is key to staying ahead of future drug-resistant strains.
Citation: Wilharm, G., Skiebe, E., Michalska, A. et al. Acinetobacter baumannii’s lifestyle includes soil-dwelling colonization of decaying plant material and airborne spread. Nat Commun 17, 2316 (2026). https://doi.org/10.1038/s41467-026-70072-4
Keywords: Acinetobacter baumannii, airborne bacteria, soil microbiome, antibiotic resistance, One Health