Clear Sky Science · en
Preclinical and clinical obesity: prevalence, associations to cardiometabolic risk and response to lifestyle intervention in NHANES and the EPIC-Potsdam and TULIP studies
Why this matters for everyday health
Many people are told they have “obesity” based on a body mass index (BMI) number, but that label does not explain how sick they are or how much they might benefit from treatment. This study asks a simple but important question: among adults with obesity, who already has clear health damage, who is still in an earlier stage, and how much can lifestyle changes shift people toward lower risk?
Two stages of obesity: early strain and clear damage
An international expert group recently suggested splitting obesity into two stages. First comes “confirmed obesity,” where a high BMI is backed up by other body measurements such as waist size or body fat scans. Within this group, people are then labeled as having either “preclinical obesity,” meaning extra body fat without obvious organ problems, or “clinical obesity,” where there are clear signs that the weight is hurting the heart, blood sugar control, kidneys, breathing, or daily functioning. The new study tests how this classification works in large groups of adults from the United States and Germany, and what it means for future disease and for response to lifestyle programs.
Most adults with obesity already show health problems
Using recent data from the US National Health and Nutrition Examination Survey (NHANES) and the EPIC-Potsdam study in Germany, the researchers found that practically every adult with BMI-defined obesity also had at least one other indicator of excess body fat. In other words, extra confirmation beyond BMI added little new information. More striking, more than four out of five adults with confirmed obesity met at least one clinical sign that obesity was already harming the body. The share with “clinical obesity” climbed with age and with higher BMI class, but was high even in many people with milder obesity and in younger adults.
Different risks for heart disease and diabetes
To see how these categories translate into real-world illness, the team followed participants in the EPIC-Potsdam study over time. People with clinical obesity had a nearly eightfold higher risk of developing type 2 diabetes and almost a threefold higher risk of cardiovascular disease, compared with adults without obesity who did not meet clinical criteria. Even those in the “preclinical obesity” group—extra fat but no major clinical signs—had a clearly raised diabetes risk, though their heart disease risk was not higher than that of people without obesity who nevertheless had other clinical problems, such as high blood pressure. This pattern suggests that obesity-related damage to blood sugar control can appear earlier than damage leading to heart attacks and strokes.
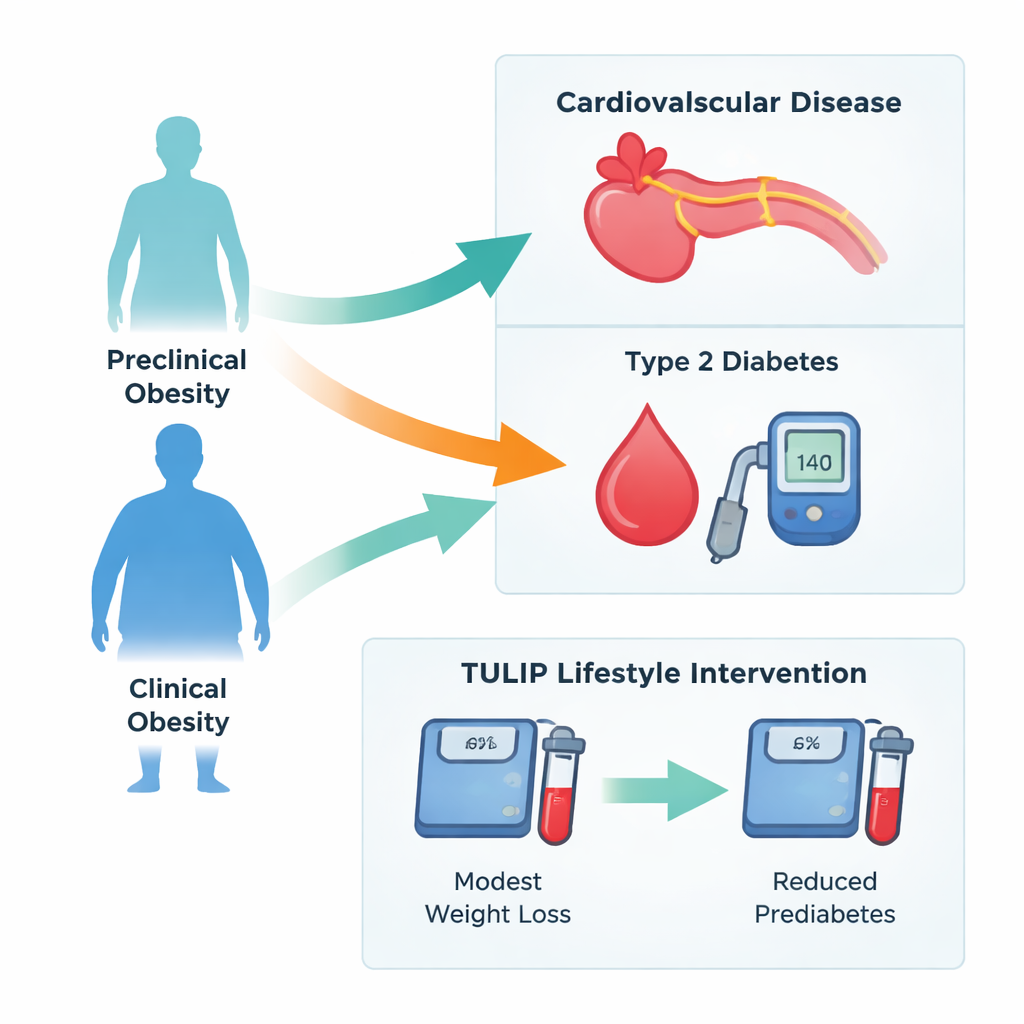
When labels miss high-risk metabolism
The experts’ original definition of “unhealthy metabolism” in obesity required a strict combination of high blood sugar, high triglycerides, and low “good” HDL cholesterol. The new analyses show that this narrow rule may place many people with harmful metabolic changes into the supposedly milder, preclinical group. When the authors relaxed this rule to count any one of these problems, almost everyone with confirmed obesity would be labeled as having clinical obesity. This matters because the study also shows that moderately high blood sugar and blood fats can already translate into much higher long-term risk, arguing that waiting for a full cluster of abnormalities may delay needed treatment.
Lifestyle change can move people out of clinical obesity
The researchers also looked at the TULIP lifestyle program in Germany, in which adults with obesity received nine months of coaching on diet and physical activity. Participants who lost more than 3% of their body weight—modest but achievable in everyday life—saw the share with clinical obesity drop from 71% to 57%. Levels of blood fats fell, and the proportion with prediabetes dropped from about one in two to less than one in three. Interestingly, younger age and lower fat in the liver predicted a better chance of moving out of clinical obesity, while the exact starting BMI or the amount of weight lost were less important than expected.
What this means for patients and clinicians
Put simply, the study shows that by the time most adults meet BMI criteria for obesity, many already have clear health damage and much higher chances of future heart disease and diabetes. Relying on extra body measurements or very strict metabolic cutoffs may give false reassurance to people who are, in fact, at high risk. At the same time, the findings offer hope: even modest, well-supported lifestyle changes can shift a meaningful number of people from clinical back toward preclinical obesity, especially when started earlier and before too much fat builds up in organs like the liver. The authors argue that refining how we define “clinical obesity” could help doctors better identify who stands to gain the most from timely lifestyle or medical treatment.
Citation: Schiborn, C., Hu, F.B., Stefan, N. et al. Preclinical and clinical obesity: prevalence, associations to cardiometabolic risk and response to lifestyle intervention in NHANES and the EPIC-Potsdam and TULIP studies. Nat Commun 17, 1935 (2026). https://doi.org/10.1038/s41467-026-69738-w
Keywords: obesity stages, cardiometabolic risk, type 2 diabetes, lifestyle intervention, BMI and body fat