Clear Sky Science · en
Transdermal testosterone gel vs placebo in women with diminished ovarian reserve prior to in vitro fertilization: a randomized, clinical trial
Why this study matters to people trying to conceive
Many women who turn to in vitro fertilization (IVF) do so later in life, when their natural supply of eggs has already declined. For this group, often labeled as having a “diminished ovarian reserve,” every egg matters—and so does every promise of a treatment that might boost their chances. Testosterone gel has quietly become a popular add-on therapy in fertility clinics, promoted as a way to coax the ovaries into producing more eggs. This large clinical trial asks a simple but crucial question: does it actually help?
Hope in a hormone gel
Doctors have long known that androgens—hormones like testosterone—play a role in early egg development inside the ovary. Animal studies suggest that small amounts may help tiny follicles grow and make them more responsive to fertility drugs. On this basis, many clinics began prescribing testosterone gel to women with a low egg reserve before IVF, hoping to increase the number of eggs collected and ultimately improve pregnancy rates. Yet the existing human studies were small, inconsistent, and often lacked rigorous controls, leaving patients and clinicians with more belief than proof.
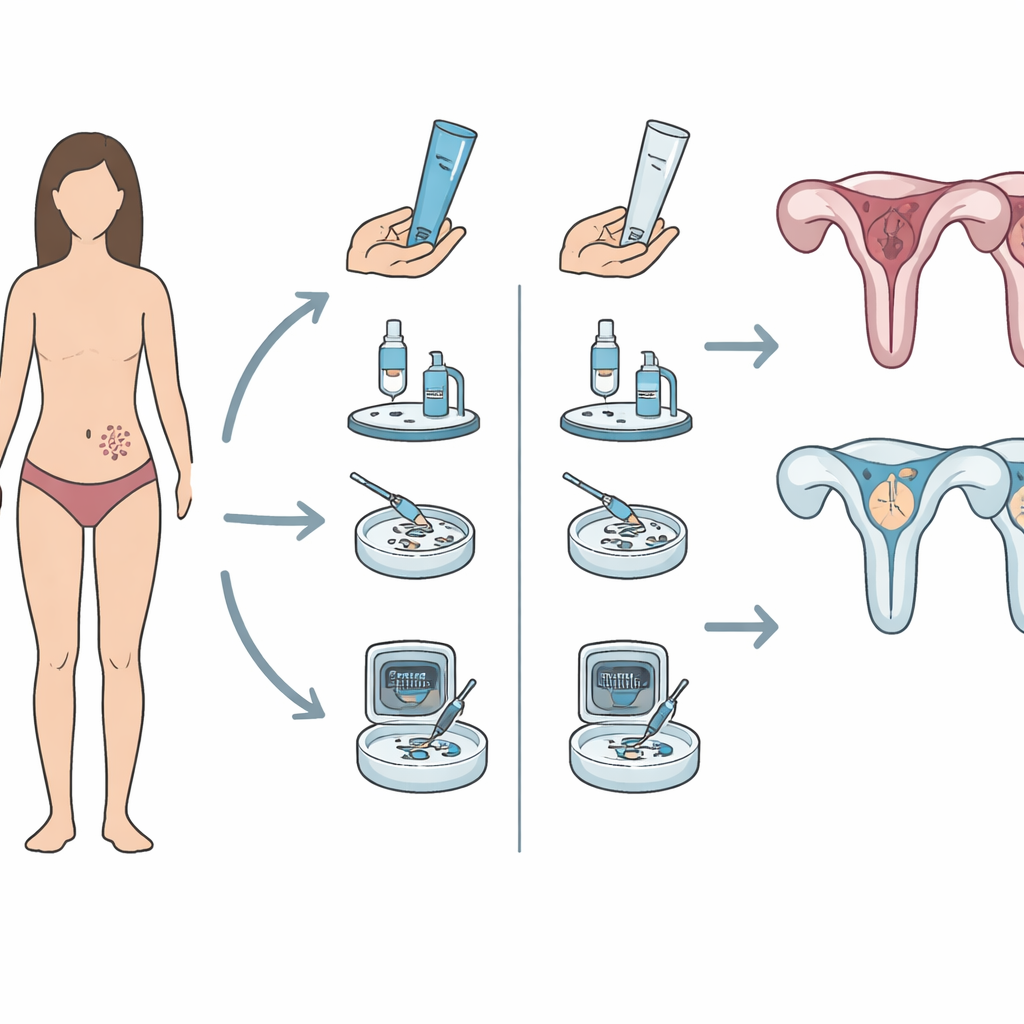
Putting the idea to a fair test
To provide clear answers, researchers launched the T-TRANSPORT trial across 10 fertility clinics in four European countries. They enrolled 290 women aged 18 to 43 who all met strict criteria for diminished ovarian reserve, meaning they had very few eggs visible on ultrasound or had produced only a small number of eggs in previous IVF cycles. Participants were randomly assigned, like drawing lots, to receive either a once-daily testosterone gel or an identical-looking placebo gel for about nine weeks before starting a standard IVF stimulation protocol. Neither the women, their doctors, nor the statisticians analyzing the data knew who received which treatment until the study was over.
What the trial actually found
The key outcome was whether women achieved a clinical pregnancy after the first fresh embryo transfer—that is, a pregnancy with a heartbeat seen on ultrasound at seven weeks or later. Among the 288 women included in the main analysis, pregnancy occurred in about 16 percent of those given testosterone and 15 percent of those given placebo, a difference so small it could easily be due to chance. The number of eggs collected, the number of mature eggs, the quality and number of embryos, and the chances of miscarriage, live birth, or pregnancy complications were also similar in both groups. In other words, raising testosterone levels with the gel did not translate into better IVF results.
Safety, side effects, and stopping early
The study also closely tracked side effects. Overall, just over half of the women in both groups reported at least one adverse event, but serious problems were rare, and none occurred in the testosterone group. The main noticeable difference was increased hair growth, reported about twice as often by women on testosterone gel compared with placebo, though this seldom led anyone to stop treatment. An independent monitoring committee performed a planned check partway through the trial. Their calculations showed that even if the study continued to its full size, the chances of eventually finding a meaningful benefit from testosterone were very low. To avoid exposing more women to an ineffective add-on, the trial was stopped early for futility.
What this means for patients and clinics
For women facing IVF with a low egg reserve, these results are sobering but empowering. This large, carefully controlled trial—making up almost half of all patients ever studied on this question—found no evidence that using transdermal testosterone gel before IVF improves the odds of getting pregnant or taking home a baby. At the same time, it did add mild androgenic side effects, such as extra hair growth. While the study was not designed to rule out very small benefits, it strongly suggests that routine use of testosterone gel as an IVF “booster” is unlikely to change outcomes in a meaningful way. For patients, this means one less costly, hope-raising but unproven add-on; for clinicians, it offers solid data to guide more transparent, evidence-based counseling about what truly helps—and what probably does not—in the difficult journey of infertility treatment.
Citation: Polyzos, N.P., Leathersich, S.J., Martínez, F. et al. Transdermal testosterone gel vs placebo in women with diminished ovarian reserve prior to in vitro fertilization: a randomized, clinical trial. Nat Commun 17, 2713 (2026). https://doi.org/10.1038/s41467-026-69557-z
Keywords: diminished ovarian reserve, in vitro fertilization, testosterone gel, fertility treatment add-ons, randomized clinical trial