Clear Sky Science · en
Granulomas microenvironment-guided sono-immunotherapy to treat and prevent recurrence of tuberculosis
Why this new tuberculosis approach matters
Tuberculosis still infects a quarter of the world’s population and can return even after long courses of antibiotics. This study describes a targeted “sonic plus immune” therapy that aims not only to kill tuberculosis bacteria hiding deep in the lungs, but also to retrain the immune system so the disease is far less likely to come back. It combines insights from patient samples with a smart nanoparticle drug that is activated by medical ultrasound.
The hidden battlefield inside lung nodules
When tuberculosis germs invade, immune cells in the lung wall themselves off into tight knots of tissue called granulomas. These structures are meant to cage the bacteria, but they also create a sheltered niche where the microbes can lie low and dodge antibiotics. By reanalyzing single-cell RNA sequencing data from human lung tissue, the researchers compared ordinary non-tuberculous granulomas with true tuberculous granulomas and with healthy lung. They found that in tuberculous lesions, key “first responder” cells—macrophages and dendritic cells—had switched into a muted state. Molecular pathways that normally sense bacteria and sound the alarm were dialed down, while genes that dampen immune activity were turned up.
When the immune system hits the brakes
The team then looked at blood samples from people with drug-resistant versus drug-sensitive tuberculosis, and from patients whose disease either recurred or stayed cured. Across these groups, the same pattern emerged: genes and pathways that negatively regulate immunity were more active in those with drug resistance and relapse. Signals that should help immune cells recognize and clear bacteria were weaker. This suggested that failure of treatment is not only about the drugs or the bacteria, but also about an immune environment that has been pushed into an overly restrained, “tolerant” mode, particularly inside granulomas.
Designing a sound-activated helper particle
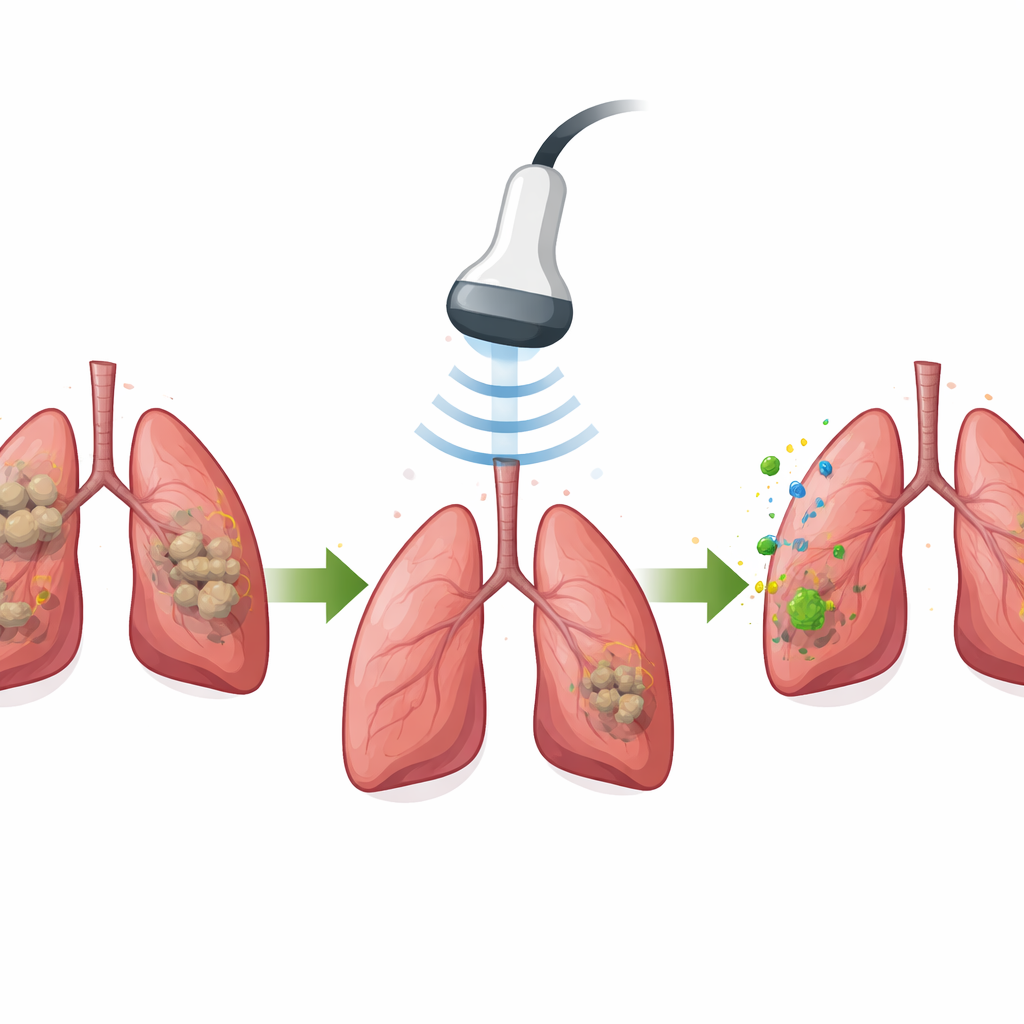
Guided by this picture of immune paralysis, the researchers engineered a nanoparticle called manSNI. It is built from an organic semiconducting polymer that can generate bursts of reactive oxygen species (ROS) when exposed to ultrasound, plus a mannose coating that helps it home to macrophages, and a small immune-activating molecule that stimulates a Toll-like receptor on these cells. In test tubes, manSNI particles clustered in the lysosomes of infected macrophages and, under ultrasound, produced enough ROS to destroy more than 99% of tuberculosis model bacteria, even when the ultrasound had to pass through several centimeters of tissue. The ROS also ruptured bacterial membranes, spilling bacterial proteins that can act as antigens.
Turning a cold granuloma into a hot immune hub
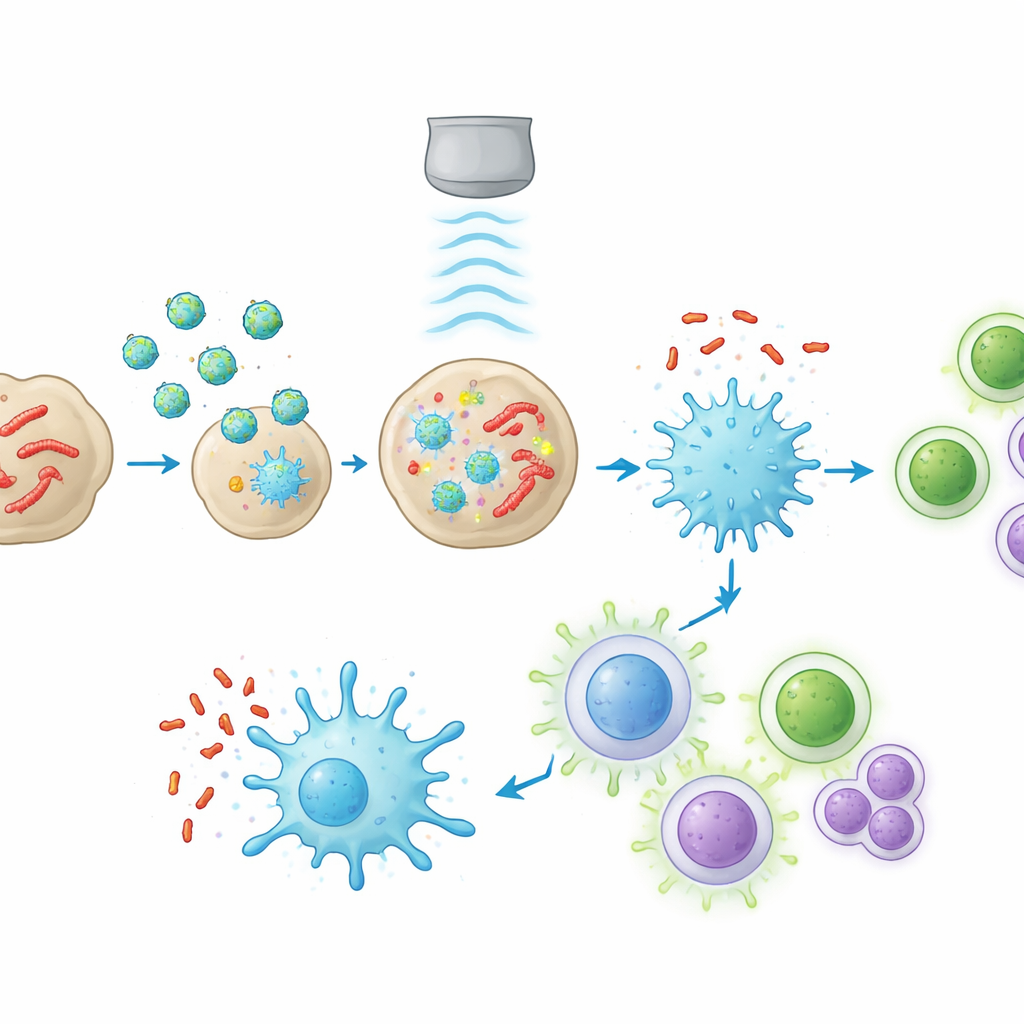
In mice with tuberculosis-like lung disease, manSNI accumulated far better in granulomas than similar particles lacking the mannose targeting group. When the lungs were briefly exposed to ultrasound, bacterial counts in the lung dropped almost to zero. At the same time, the local immune landscape was transformed. Macrophages shifted toward a pro-inflammatory, bacteria-fighting state; dendritic cells matured and moved antigen information to nearby lymph nodes; and tuberculosis-specific T cells and antibody-producing B cells expanded. Gene-expression analysis of lung tissue showed that several key sensing and defense pathways, previously found to be suppressed in human granulomas, were now strongly reactivated.
Building lasting protection against relapse and reinfection
Clearing the first infection is only part of the challenge; many patients experience tuberculosis again, either from lingering bacteria or from new exposure. In long-term mouse studies, the authors compared a standard antibiotic (rifampicin) with manSNI plus ultrasound. Both regimens initially wiped out detectable bacteria, but relapse was common after antibiotics alone, while it was rare after sono-immunotherapy. Animals receiving manSNI developed higher levels of tissue-resident memory T cells in the lung, central and effector memory T cells in lymphoid organs, and long-lived memory B cells and antibodies in the blood. When these mice were deliberately re-exposed to tuberculosis model bacteria, most resisted reinfection or showed only mild, transient lesions.
What this could mean for future tuberculosis care
To a non-specialist, the main takeaway is that this work offers a two-pronged strategy: directly destroy bacteria hiding in hard-to-reach lung nodules, and at the same time reset the local immune environment from “off” to “on.” The approach uses ultrasound—already common in clinics—to noninvasively activate a precisely targeted nanoparticle that both kills germs and acts like a built-in vaccine booster. While the experiments were done in mice and with safer model strains rather than the most dangerous tuberculosis bacteria, the results suggest a path toward shorter, more effective treatments that not only cure tuberculosis but also greatly reduce the odds that it will return.
Citation: Wang, W., Li, F., Mo, W. et al. Granulomas microenvironment-guided sono-immunotherapy to treat and prevent recurrence of tuberculosis. Nat Commun 17, 2595 (2026). https://doi.org/10.1038/s41467-026-69420-1
Keywords: tuberculosis, sono-immunotherapy, nanoparticles, granulomas, ultrasound therapy