Clear Sky Science · en
Opposite effects of chronic HIV infection and antiretroviral medication on organismal and organ-specific biological aging
Why this research matters for long-term HIV health
People living with HIV now often enjoy near-normal life spans thanks to modern drug combinations, yet they still face higher rates of heart disease, liver problems, cancers, and other conditions usually linked to old age. This study asks a pressing question for patients and clinicians alike: does HIV itself make the body grow older faster, and can some HIV medicines actually slow this hidden aging? By tracking thousands of blood proteins and chemical tags on DNA, the researchers map how HIV and its treatments together shape the pace of aging throughout the body and in specific organs.
Measuring the body’s hidden clock
Chronological age is simply the number of years since birth, but “biological age” reflects how worn our organs and tissues really are. The team built detailed aging “clocks” using patterns of proteins circulating in the blood, originally calibrated in healthy volunteers. They created one overall body clock and several organ-focused clocks for the brain, blood vessels, liver, and intestine, then checked these against well-known DNA methylation clocks—chemical marks on DNA that change in predictable ways with age. In more than 2,000 adults with well-controlled HIV, these protein-based ages closely matched both true age and DNA-based ages, and were linked to real-world health problems and risk of death. 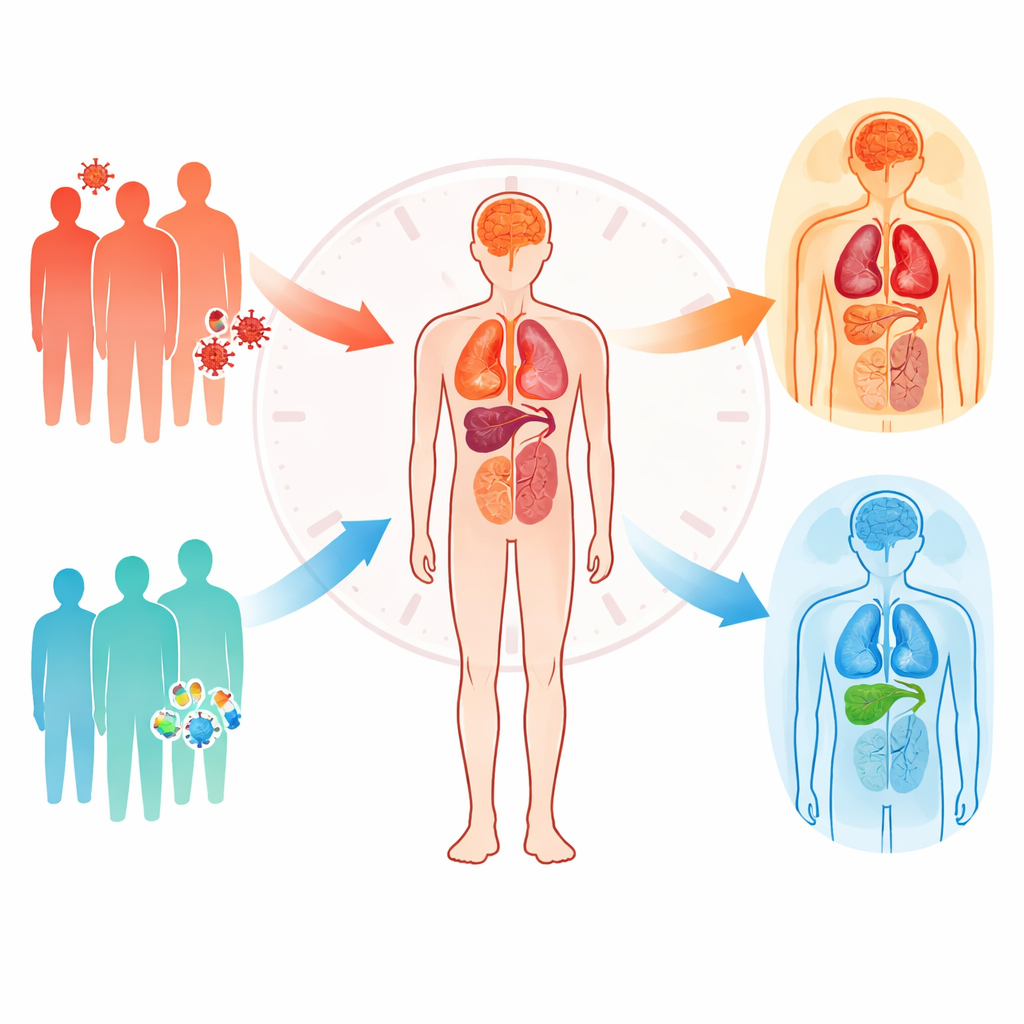
HIV infection speeds aging while viral control helps
When the researchers compared these aging scores to each person’s actual age, they found that many people with HIV were “older” biologically than their birth certificates would suggest. This acceleration appeared clearly in whole-body and brain-focused clocks, while some organ clocks, such as those for the liver and intestine, showed more complex patterns. Individuals with a history of more severe immune damage—very low CD4 counts, higher recent viral loads, or more advanced HIV stage—tended to have greater age acceleration. Those who had kept virus levels undetectable for years showed less acceleration, and a rare group of “elite controllers,” who suppress HIV without drugs, even showed hints of slower aging across several measures. Importantly, the size of the total HIV reservoir—the dormant virus still hiding in immune cells—tracked with faster biological aging, underscoring that lingering virus continues to shape health even when standard tests show “undetectable.”
Organ aging, complications, and the gut–heart connection
Next, the team asked whether these aging signals are just bystanders or actually contribute to disease. They found that older “brain age” scores were linked to nervous system problems such as epilepsy, Parkinson’s disease, and other brain disorders that occur more often in people with HIV. Older “artery age” scores went hand in hand with blood clots and other cardiovascular problems. Overall multi-organ age predicted risk of death over two years, suggesting these measures capture meaningful vulnerability. Using a genetic technique called Mendelian randomization, the researchers could go a step further and test cause-and-effect. They found evidence that premature aging of the intestine helps drive cardiovascular disease. Blood markers of a leaky gut—molecules that indicate bacterial products escaping from the gut into the bloodstream—rose alongside intestinal aging scores, supporting a picture in which an aging intestinal barrier fuels long-lasting inflammation and clogged arteries. 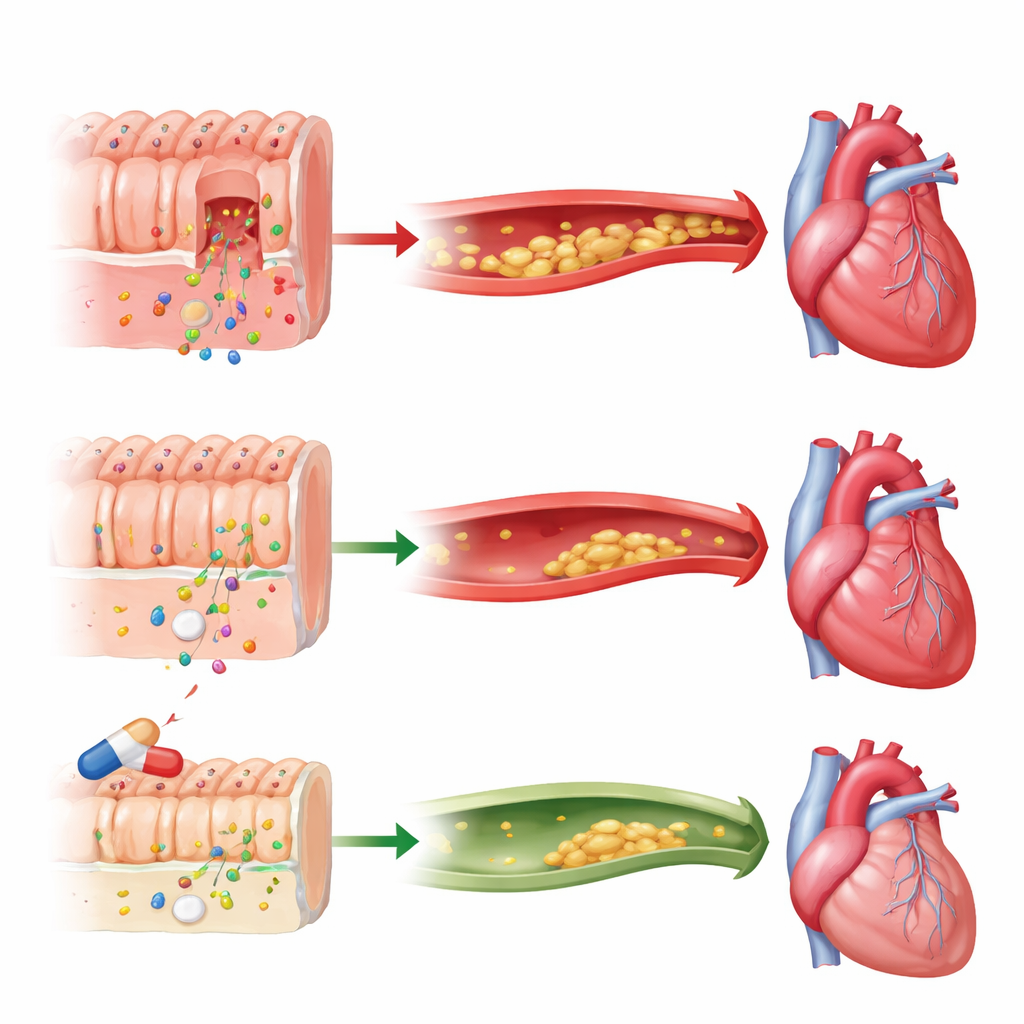
HIV drugs: some accelerate, some protect
Because treatment itself might affect aging, the authors examined how years of exposure to specific antiretroviral medicines related to the aging clocks. The story was not one-size-fits-all. Certain older drugs with known toxicities, such as stavudine, aligned with faster aging in several organs. In contrast, longer use of some widely used nucleoside and non‑nucleoside reverse transcriptase inhibitors, including lamivudine, emtricitabine, rilpivirine, and nevirapine, was linked to slower biological aging, especially at the whole-body and intestinal levels. Tenofovir taken in its older form (TDF) showed mixed but often favorable ties with overall aging, whereas its newer version (TAF) was associated with faster aging of the liver and brain clocks. These patterns remained even after accounting for the fact that drugs are given in combinations, suggesting that particular agents may independently push aging forward or pull it back.
What this means for people living with HIV
The study paints a nuanced picture: chronic HIV infection, even under good viral control, tends to make the body age faster, and this acceleration is closely tied to the amount of virus hiding in immune cells and to long-term risks such as heart and brain disease. At the same time, some HIV medicines appear to counteract this process, while others may worsen it in specific organs. For patients, this work highlights why strict viral suppression and careful choice of drug regimen matter not only for today’s lab results but also for tomorrow’s heart, brain, and gut health. For clinicians and researchers, these protein and DNA-based aging scores offer promising tools to monitor hidden wear and tear, refine treatment plans, and ultimately aim for longer, healthier lives for people living with HIV.
Citation: Zhang, Y., Matzaraki, V., Vadaq, N. et al. Opposite effects of chronic HIV infection and antiretroviral medication on organismal and organ-specific biological aging. Nat Commun 17, 2572 (2026). https://doi.org/10.1038/s41467-026-69412-1
Keywords: HIV and aging, biological age, antiretroviral therapy, proteomic aging clocks, cardiovascular complications