Clear Sky Science · en
Sclerostin deficiency sensitizes white adipocytes to thermogenic signals that induce beiging in mice
Why warming up your fat could cool down disease
Most of us think of bone and body fat as separate worlds: one gives us structure, the other stores energy. This study in mice reveals that bone and fat are in constant chemical conversation, and that a protein made by bone cells can decide whether our "white" fat just sits there storing calories or transforms into a more active, calorie-burning "beige" fat. Understanding this hidden dialogue could open new ways to tackle obesity, diabetes, and bone loss at the same time.
A quiet messenger from bone
Deep inside bones, specialized cells release a small protein called sclerostin into the bloodstream. Doctors already target sclerostin with drugs to strengthen bone in patients at risk for fractures. Earlier work showed that mice lacking sclerostin are not only very strong-boned, but also leaner and more sensitive to insulin. Their subcutaneous fat, especially around the hips (inguinal white fat), contains tiny, multi-compartment fat cells resembling "beige" fat, which can burn fuel to make heat. These clues led the researchers to ask whether sclerostin normally acts as a brake on the body’s ability to convert white fat into beige fat when exposed to cold or to drugs that mimic nerve signals to fat.
Cold signals, bone signals, and fat ignition
The team exposed normal mice and mice lacking the sclerostin gene (Sost-/-) to a drug that activates a specific fat-cell receptor (β3-adrenergic receptor), or to mild cold. In normal animals, these thermogenic signals increased sclerostin production in bone and raised its level in blood. This rise was linked to a loss of spongy bone but only modest changes in subcutaneous fat. In contrast, sclerostin-deficient mice showed a much stronger response: their inguinal fat took up more glucose, released more fatty acids, shrank in size, and filled with beige-like cells packed with mitochondria, the cell’s power plants. Key thermogenic genes switched on more strongly in these mice, especially in subcutaneous fat, while classic brown fat was largely unchanged.
Fine-tuning fat burning through a shared switch
To understand how sclerostin exerts this control, the researchers focused on β-catenin, a protein involved in the Wnt signaling pathway that sclerostin normally suppresses in bone. In fat, activating β-catenin after birth drove white cells toward a beige-like state and heightened their response to β3-adrenergic signals, but this effect disappeared when mice were housed at a warm, thermoneutral temperature where the body no longer needs extra heat. Conversely, deleting β-catenin specifically in fat cells of sclerostin-deficient mice erased their beige fat, restored larger white fat cells, and reversed improvements in insulin and fatty acid levels. These experiments suggest that, when sclerostin is low, β-catenin in fat cells becomes an important internal lever that makes white fat more responsive to thermogenic cues.
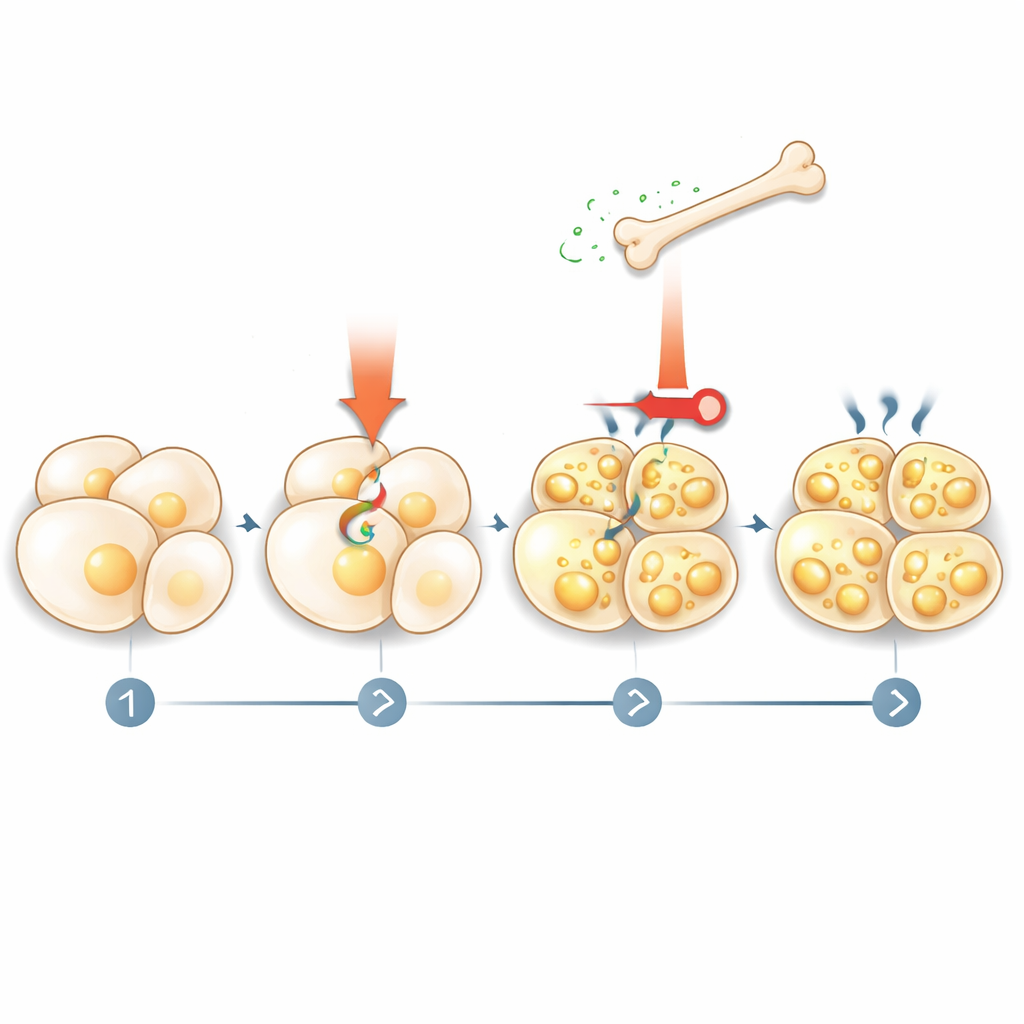
How fat talks back to bone
The story did not end with bone telling fat what to do. The team found that thermogenic stimulation activates fat breakdown (lipolysis), releasing fatty acids into the blood. These fatty acids, in turn, act on bone cells via a nuclear receptor called PPARγ, boosting sclerostin production. When the researchers blocked lipolysis in fat cells or removed PPARγ from bone cells, cold-mimicking drugs could no longer raise sclerostin levels. This reveals a feedback loop: thermogenic signals trigger fat to release fuel, this fuel instructs bone to secrete more sclerostin, and sclerostin then feeds back to restrain further fat activation and beiging.
Pairing bone and fat drugs for metabolic health
Finally, the researchers tested whether interrupting this loop could help in a disease-like setting. Obese mice on a high-fat diet received a low dose of mirabegron (a β3-adrenergic drug already used for bladder problems), an antibody that neutralizes sclerostin (romosozumab, approved for osteoporosis), or both. While either drug alone had modest effects, the combination reduced fat mass in key depots, shifted fat toward smaller, more active cells, lowered insulin, triglycerides, and cholesterol, and preserved bone strength. Warm housing, which reduces the body’s need for heat, largely erased the metabolic benefits of sclerostin loss, underlining that this pathway matters most when thermogenic signals are present.
What this means for future treatments
In plain terms, this work shows that bone is not just a passive scaffold but an active regulator of how much energy fat cells burn. Sclerostin functions like a volume knob that keeps thermogenic fat activity, and thus fuel use, in check. Turning that knob down—by genetics or by drugs—makes certain white fat stores more eager to switch into a heat-producing mode when the body is nudged by cold or specific medications. Because the same intervention can strengthen bone and improve metabolic health in mice, carefully designed combinations of bone- and fat-targeted therapies might one day help treat obesity, diabetes, and osteoporosis together, rather than one disease at a time.
Citation: Choquette, G.M., Kim, S.P., Wilkinson, K.J. et al. Sclerostin deficiency sensitizes white adipocytes to thermogenic signals that induce beiging in mice. Nat Commun 17, 2394 (2026). https://doi.org/10.1038/s41467-026-69227-0
Keywords: sclerostin, beige fat, bone–fat crosstalk, thermogenesis, metabolic disease