Clear Sky Science · en
Paper-based fluorescent assay for blood typing and antibody titer determination using long-term ambient-stored bioengineered RBCs
Why Testing Blood Quickly Matters
When someone needs an emergency transfusion or a transplant, doctors must know two things fast: the person’s blood type and whether their blood carries high levels of certain antibodies that could cause dangerous reactions. Today, these tests usually depend on refrigerated blood cell reagents, specialized lab equipment, and experts who interpret subtle visual changes by eye. This new study introduces a pocket-sized, paper-based test that uses specially engineered red blood cell shells and fluorescent signals to deliver lab-grade blood typing and antibody measurements at room temperature in just a few minutes.
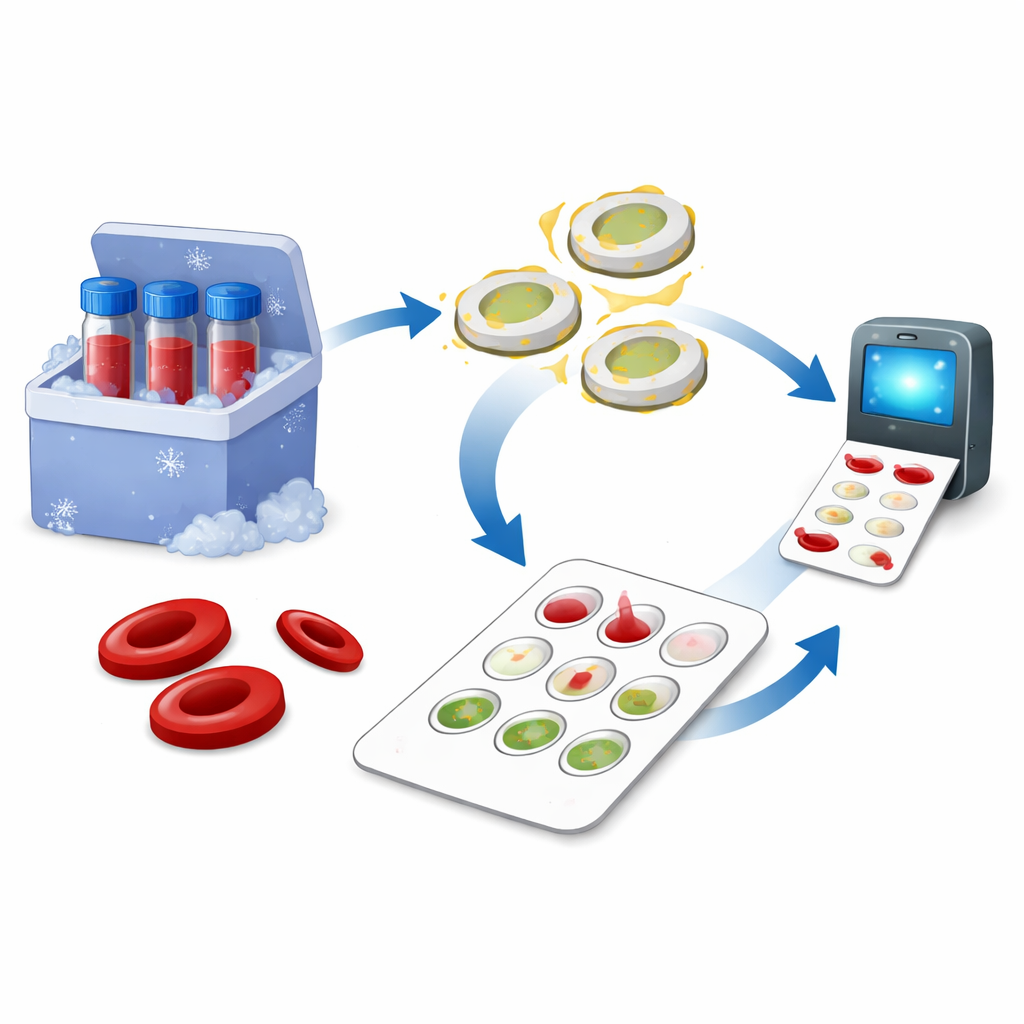
Turning Red Blood Cells into Stable Test Tools
Traditional tests rely on fresh red blood cells, which spoil quickly and must be kept cold. The researchers reasoned that the most important part of a red blood cell for blood typing is its outer membrane, where the A, B, and other blood group markers sit. They developed a gentle way to remove the cell’s inner contents, including the red hemoglobin, while keeping the membrane and its blood type markers largely intact. These empty “ghost” cells were then coated with tiny fluorescent nanoparticles, turning each cell membrane into a bright, trackable probe. Finally, the team freeze-dried this material so it could be stored as a dry powder at room temperature and easily rehydrated when needed.
How the New Paper Test Works
The heart of the device is a small plastic card holding a foldable paper pad with built-in channels and filters. Before use, the engineered fluorescent cell membranes are preloaded and dried in tiny reaction wells. To run a test, a small amount of patient plasma is added and mixed for about five minutes. If the plasma contains antibodies against A or B blood group markers, they cause the fluorescent membranes to clump together. When the card is folded, the mixture flows through a layered filter: larger clumps are caught on top, smaller ones below, and free particles are washed away. A handheld fluorescence reader then shines light on the filter and measures how brightly it glows. Brighter signals mean more clumping and, therefore, higher antibody levels, allowing the device to determine both ABO type and antibody strength in a single run.
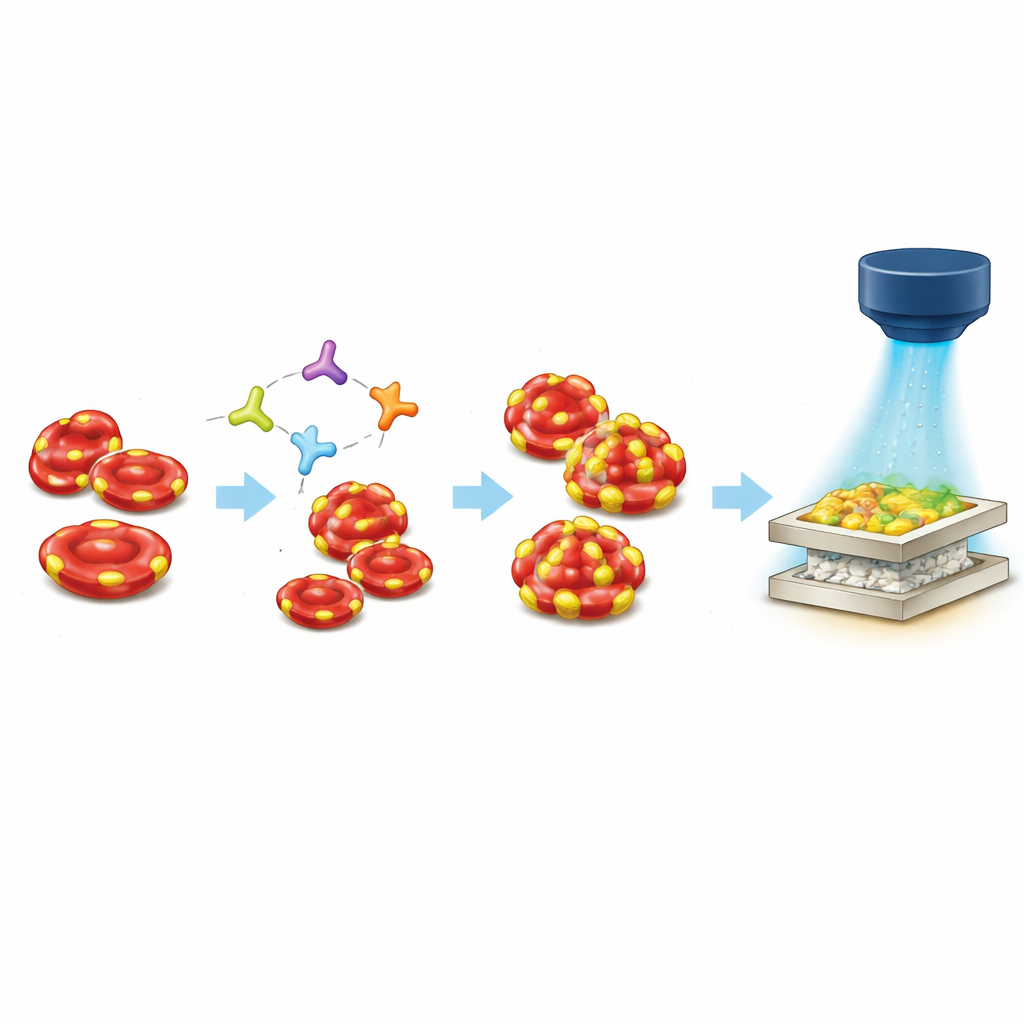
Making the Reagents Last for Years
A major hurdle for point-of-care blood testing is how fragile conventional red blood cell reagents are. Ice crystals and long storage times can damage the membrane proteins that carry blood type markers, making them unreliable. By removing most of the water along with the cell interior and then freeze-drying the fluorescent membranes in a protective mixture, the team reduced ice damage and preserved the critical surface markers. In tests over two years at room temperature, the engineered reagents kept their ability to clump with matching antibodies and maintained stable fluorescence, while standard liquid red blood cell reagents stored in the refrigerator failed within months.
From Lab Bench to Real Patients
The researchers then checked whether their system could perform as well as a widely used hospital method called the gel microcolumn assay. In a registered clinical study of 641 patient samples, the new paper-based test correctly identified ABO blood types in every case. For measuring antibody “titer” — essentially, how concentrated the anti-A or anti-B antibodies are — the fluorescence-based readings strongly matched the gel method, with most results falling within one step of the standard semi-quantitative scale. The test also proved robust against common sample problems such as moderate hemolysis (broken red cells), typical cholesterol levels, and moderate jaundice, behaving similarly to existing clinical reagents.
What This Could Mean for Care
To a layperson, the key takeaway is that this work turns fragile, refrigerated blood cell reagents into long-lasting, brightly glowing test tools that sit on paper. The result is a simple, handheld card-and-reader system that can quickly tell both a person’s ABO blood type and how strong their relevant antibodies are, using only a small plasma sample and no complex machinery. With room-temperature stability of at least two years and near-laboratory accuracy, this approach could make safe, informed transfusion decisions more accessible in ambulances, rural clinics, battlefields, and overloaded hospitals alike, while also paving the way for future tests that measure other blood group antibodies just as easily.
Citation: Li, Y., Zhang, Y., Liang, S. et al. Paper-based fluorescent assay for blood typing and antibody titer determination using long-term ambient-stored bioengineered RBCs. Nat Commun 17, 2386 (2026). https://doi.org/10.1038/s41467-026-69213-6
Keywords: blood typing, point-of-care testing, red blood cells, fluorescent assay, blood transfusion safety