Clear Sky Science · en
A primary auditory cortex-anterior cingulate cortex circuit underlying cross-modal visceral pain modulation
Why Sounds Might Soothe the Stomach
Many people with irritable bowel syndrome or other gut problems notice that stress makes their pain worse, while calming music can sometimes make it feel better. This study explores a surprisingly specific question behind that everyday experience: how do sounds—from soothing music to simple noise—reach into the brain and change the way we feel pain coming from our internal organs, especially the gut?
A Hidden Bridge Between Hearing and Pain
The researchers focused on two key brain areas in mice. One is the primary auditory cortex, which helps the brain process sounds. The other is the anterior cingulate cortex, a region known to shape how strongly we feel pain and how upsetting it seems. The team suspected that these two areas might be connected in a way that lets sound influence gut pain. To test this, they used a mouse model of early-life stress that mimics some features of irritable bowel syndrome, including lasting oversensitivity to pain from the colon. They then combined modern brain-mapping, recording, and light-based control techniques to trace and control signals between hearing and pain regions.
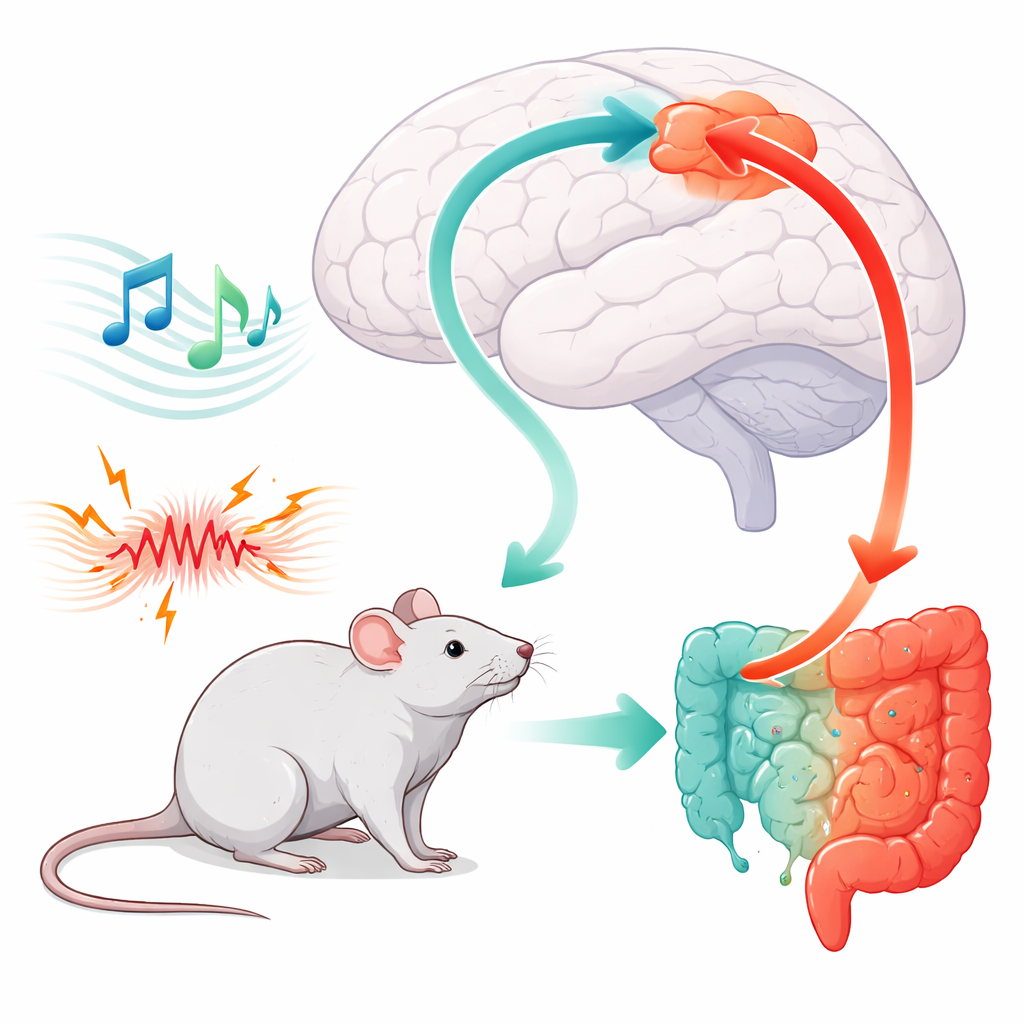
How Early Stress Rewires a Pain Circuit
The scientists first showed that the auditory cortex does not directly “hear” gut pain; its cells barely responded when the colon was gently stretched. Yet, in mice that had early-life gut inflammation, pain responses were exaggerated and the auditory cortex became unusually active. Closer inspection revealed an imbalance: calming inhibitory cells there were less active, while excitatory cells were more active. This imbalance sent stronger drive to the anterior cingulate cortex, whose own excitatory cells turned out to be crucial for amplifying visceral pain. When the researchers restored activity in the inhibitory cells of the auditory cortex, or reduced the excitatory drive arriving in the cingulate, gut pain responses dropped back toward normal.
A Two-Lane Neural Highway
Using viral tracers and fine electrodes, the team mapped a direct, two-lane connection from the auditory cortex to the anterior cingulate. One lane uses inhibitory signals, the other excitatory ones. Both types of cells in the auditory cortex project to the cingulate, and both influence how strongly cingulate neurons fire during gut pain. Activating the inhibitory projections from the hearing area to the cingulate softened pain responses in stressed mice, while shutting down excitatory projections had a similar pain-relieving effect. Local loops inside the auditory cortex further shaped this output, supporting a picture in which a flexible balance between inhibition and excitation along this route determines whether incoming sensations are quieted or amplified.
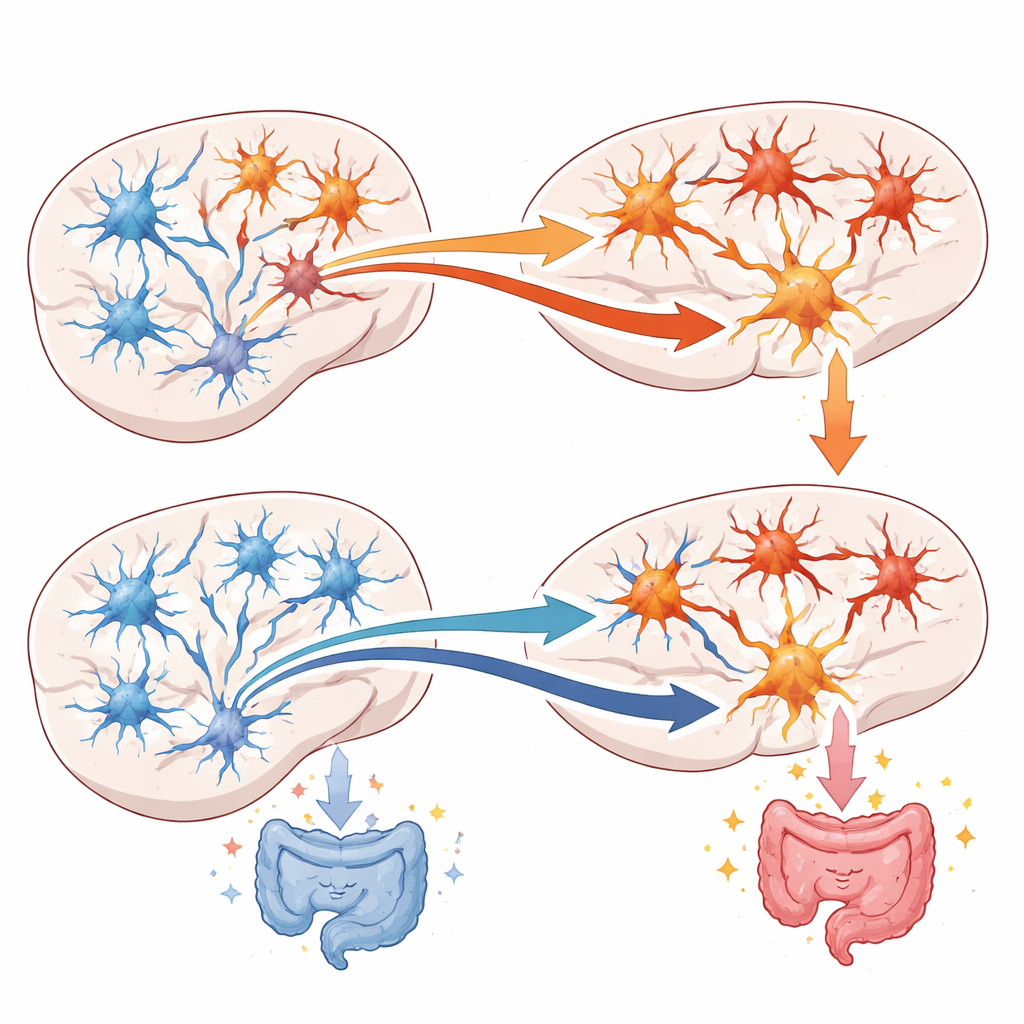
Music Tips the Balance Back Toward Calm
The authors then asked how real sounds, especially music, interact with this circuit. In stressed mice, several kinds of sound—most effectively classical music, but also some electronic music and even white noise—raised the threshold for gut pain, making the colon less tender. These same sounds boosted the activity of inhibitory cells and reduced the relative influence of excitatory cells in the auditory cortex, restoring a healthier balance. At the same time, activity in pain-related cells in the anterior cingulate fell. When the team artificially silenced the inhibitory cells in the auditory cortex, or forced the cingulate’s excitatory cells to fire more, music lost its soothing effect on gut pain. Similar principles applied to inflammatory pain in the paw, showing that this circuit can also shape pain signals from outside the body, although the relief was shorter-lived than for gut pain.
What This Could Mean for People in Pain
Put simply for non-specialists, this work shows that certain sounds can dial a brain circuit up or down, shifting how loudly pain from the gut is “heard” by higher centers in the brain. Early stress seems to weaken the circuit’s natural brakes, making the gut feel more painful, while music turns those brakes back on and eases the signal. Although these experiments were done in mice, they provide a biological roadmap for why music and other sound-based therapies may help some people with chronic visceral pain, and point the way toward designing more precise, brain-based treatments that use sound to calm an overactive pain system.
Citation: Yu, Y., Kuang, WQ., He, YH. et al. A primary auditory cortex-anterior cingulate cortex circuit underlying cross-modal visceral pain modulation. Nat Commun 17, 2352 (2026). https://doi.org/10.1038/s41467-026-69135-3
Keywords: visceral pain, music therapy, auditory cortex, anterior cingulate cortex, stress-induced hypersensitivity