Clear Sky Science · en
Engineered bacterial therapy suppresses Enterohemorrhagic Escherichia coli through metabolic competition and virulence silencing
Friendly Bacteria as Living Medicine
Food poisoning from certain strains of Escherichia coli can do far more than cause an upset stomach. Some so‑called enterohemorrhagic E. coli (EHEC) release powerful toxins that may trigger kidney failure, especially in children, and standard antibiotics can actually make things worse. This study explores a different kind of treatment: using an engineered probiotic and a sugar found in human breast milk, packaged inside smart microcapsules, to outcompete dangerous bacteria and quiet their harmful behavior without disturbing the rest of the gut ecosystem.
Why Some E. coli Are So Dangerous
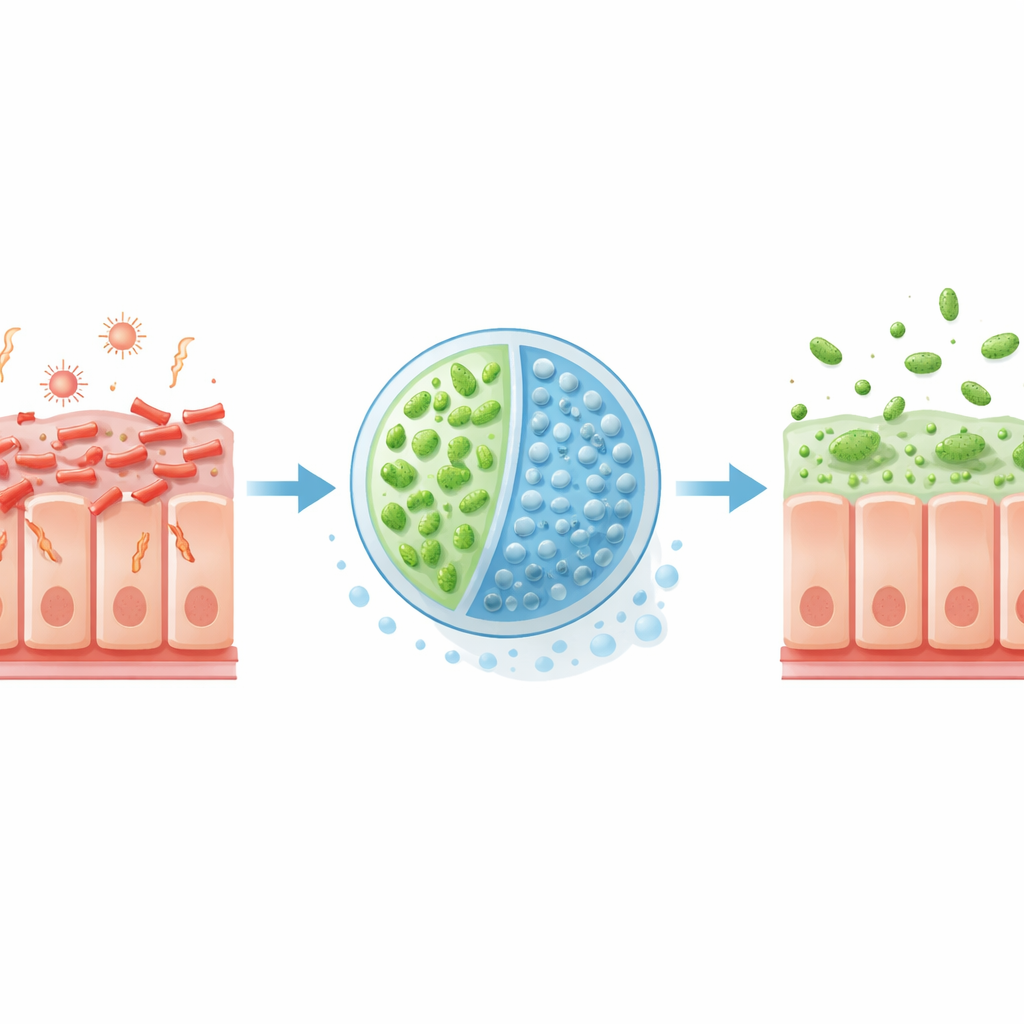
EHEC is a foodborne germ often picked up from undercooked meat or contaminated produce. Once inside the gut, it latches tightly onto intestinal cells and injects proteins that reshape the cell surface, carving out footholds that help the bacteria cling and spread. At the same time, EHEC produces Shiga toxins, which can enter the bloodstream and damage blood vessels, sometimes leading to a life‑threatening condition called hemolytic uremic syndrome. Because many antibiotics stress these bacteria and trigger even more toxin release, doctors have few safe options beyond supportive care, making new, targeted approaches highly desirable.
Reprogramming a Probiotic to Starve and Disarm EHEC
The researchers turned to Escherichia coli Nissle 1917, a long‑used probiotic strain, and rewired it into a therapeutic microbe called EcN3. They equipped EcN3 with extra genes that allow it to more efficiently break down a sugar acid, glucuronic acid, that EHEC prefers as a food source in the large intestine. They also gave EcN3 an enzyme that splits the breast‑milk sugar 2′‑fucosyllactose into two parts: lactose and fucose. Lactose acts as an internal "switch" that turns on the enhanced nutrient‑use system in EcN3, helping it soak up glucuronic acid and deprive EHEC of this fuel. Fucose, meanwhile, serves as a signal that tells EHEC to dial down key virulence genes, reducing its ability to form tight attachments and cause damage.
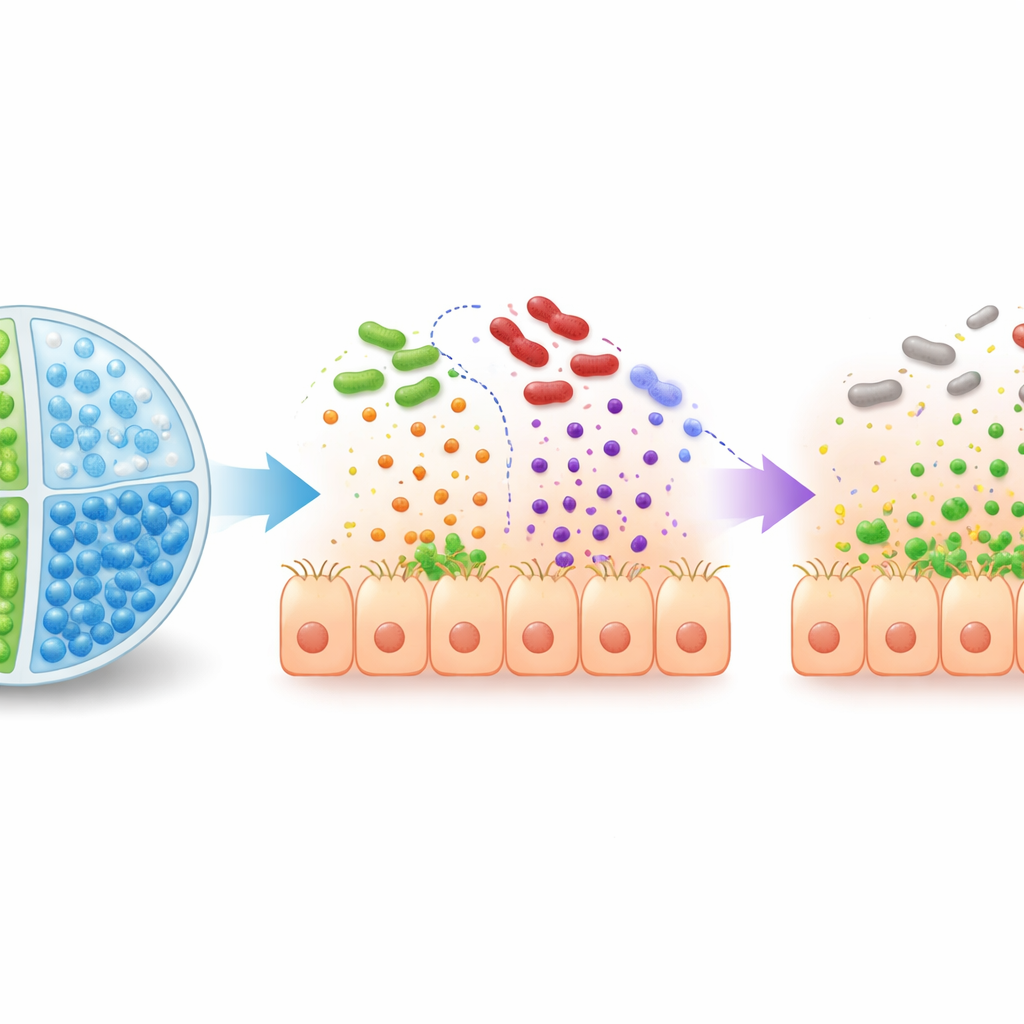
Smart Capsules That Release Therapy at the Right Place
Simply feeding engineered bacteria and sugar into the gut is not enough: stomach acid can kill the probiotic, and other microbes may devour the sugar before it reaches the colon. To solve this, the team built multicompartment microspheres—tiny beads made from alginate gel with two separate internal chambers. One chamber carries EcN3, and the other carries 2′‑fucosyllactose, keeping them apart until the beads reach the large intestine. These microcapsules resist breakdown in simulated stomach fluid but dissolve in colon‑like conditions, releasing both the engineered bacteria and the sugar exactly where they are needed. In mice, the encapsulated system led to higher EcN3 survival and stronger activation of its engineered genes than giving the same components without capsules.
Testing Protection in Animal Models
The team tested their strategy in infant rabbits infected with EHEC and in mice infected with Citrobacter rodentium, a closely related pathogen that mimics many aspects of human disease. When treated after infection with EcN3 plus 2′‑fucosyllactose, animals showed fewer pathogens in the gut, lower expression of the bacteria’s attachment genes, and less damage to intestinal tissue—all without increasing production of Shiga toxin. As a preventive measure, the free (non‑encapsulated) combination worked poorly because the sugar was quickly consumed by the existing microbiota. In contrast, when EcN3 and 2′‑fucosyllactose were delivered together in dual‑chamber microspheres, both rabbits and mice had sharply reduced pathogen colonization, milder disease, and better survival.
Helping the Good Microbes and Gut Barrier Recover
Using DNA sequencing to profile gut bacteria, the scientists found that infection disturbed the normal microbial balance, boosting harmful Citrobacter while weakening beneficial groups. Treatment with the engineered microcapsules not only reduced pathogen levels but also restored the community toward a healthier state, especially increasing Lactobacillus species that are known to support gut health. Measures of gut barrier function told a similar story: animals receiving the encapsulated therapy had higher levels of mucus‑related and tight‑junction genes, thicker protective mucus layers, and lower leakage of fluorescent tracer from the gut into the bloodstream, indicating tighter, less inflamed intestinal walls.
A Glimpse of Future Antibiotic‑Free Infection Care
Overall, this work demonstrates a two‑pronged, targeted strategy against a notoriously hard‑to‑treat foodborne infection. By combining an engineered probiotic that competes for food and senses a benign sugar signal with microcapsules that deliver both components to the colon, the therapy weakens EHEC, lowers its numbers, and protects the gut without relying on traditional antibiotics. While further safety and clinical studies are needed, the approach illustrates how living medicines and smart materials could someday provide precise, microbiome‑friendly ways to manage severe intestinal infections and reduce dependence on conventional drugs.
Citation: Ma, G., Liu, R., Li, X. et al. Engineered bacterial therapy suppresses Enterohemorrhagic Escherichia coli through metabolic competition and virulence silencing. Nat Commun 17, 2307 (2026). https://doi.org/10.1038/s41467-026-69126-4
Keywords: engineered probiotics, gut infection therapy, EHEC, microbiome, drug delivery microspheres