Clear Sky Science · en
FGF 13 functions as a regulator of the ERK/aerobic glycolysis axis in the inflammatory state during septic lung injury
Why this study matters for patients with severe infections
Sepsis is a life-threatening complication of infection that can cause the lungs to fail within hours, leaving patients dependent on ventilators and with a high risk of death. This study explores a little-known protein inside our cells, called FGF13, and uncovers how it helps to drive the runaway inflammation and energy overuse that severely damage the lungs during sepsis. By tracing this hidden control circuit, the work points to new drug targets that might calm the storm in the lungs without shutting down the body’s entire immune system.
A hidden player in lung damage during sepsis
The researchers began by comparing lung tissue from septic mice and human patients with tissue from non-septic controls. They examined a family of molecules known as fibroblast growth factors, which help maintain lung health. Among them, FGF13 stood out: its levels were markedly lower in the lungs of septic patients and animals. When the team mapped where FGF13 was located, they found it mainly inside two key cell types: endothelial cells, which form the inner lining of blood vessels, and macrophages, immune cells that sense and amplify inflammation. In septic lungs, FGF13-positive endothelial cells and macrophages were greatly reduced, hinting that changes in this molecule might be tied to severe lung injury.
How FGF13 turns lung defenders into drivers of injury
To test what FGF13 actually does, the team used genetic tools in mice to either remove it from specific cells or force those cells to make more of it. When FGF13 was deleted only in endothelial cells, septic mice had less leaky, swollen lungs, fewer invading immune cells, and better survival. The opposite happened when endothelial cells were engineered to overproduce FGF13: lung edema, bleeding, and inflammatory cell buildup worsened. A similar story emerged in macrophages. Mice lacking FGF13 in these immune cells showed weaker inflammatory responses and less lung injury, while macrophages forced to make extra FGF13 released more inflammatory molecules and aggravated the damage. In cell culture, lowering FGF13 made blood vessel cells and macrophages less sticky, less inflamed, and less toxic to their neighbors.
Inflamed cells switch to a sugar-hungry mode
Inflamed cells, like cancer cells, often shift their energy strategy: instead of slowly burning fuel with oxygen, they rapidly break down sugar in a process called aerobic glycolysis, generating lactic acid. The authors found that FGF13 strongly encourages this switch. In septic mice lacking FGF13 in either endothelial cells or macrophages, blood lactate levels were lower. In dishes, cells with reduced FGF13 took up less glucose and produced less lactate after inflammatory stimulation, while cells with extra FGF13 showed boosted glycolysis. When the researchers blocked glycolysis with a drug, the inflammation-promoting effect of excess FGF13 was largely blunted, tying the molecule’s harmful role directly to this sugar-burning program.
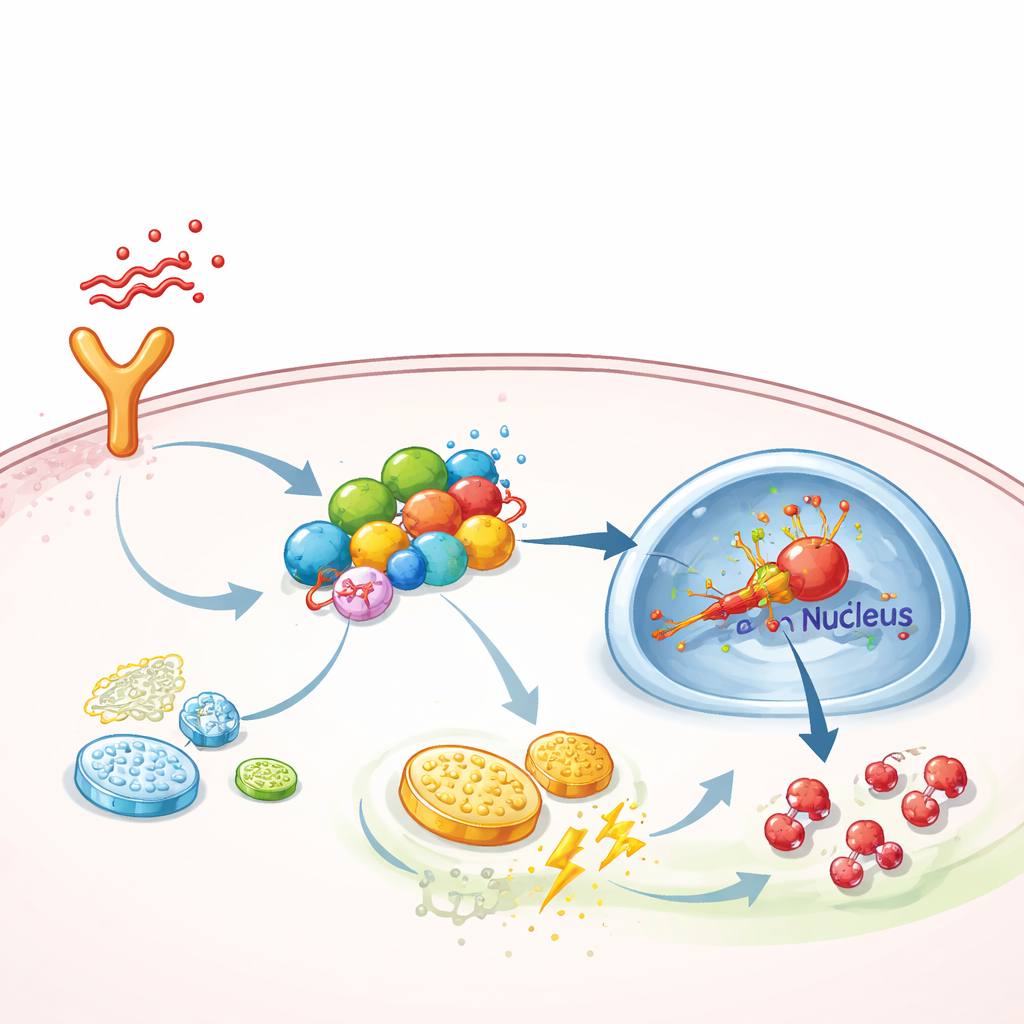
A molecular scaffold that boosts inflammatory signaling
Digging deeper, the team asked how FGF13 pushes cells toward this high-gear metabolism. They discovered that FGF13 physically binds to several signaling proteins that form a chain from surface receptors to the cell’s nucleus—specifically the TAK1–MEK–ERK pathway, which is known to activate a master regulator of low-oxygen responses called HIF-1α. FGF13 acts like a scaffold, holding these components together so signals travel more efficiently. When FGF13 was reduced, activation of ERK and HIF-1α dropped, and glycolysis waned; when FGF13 was increased, the pathway became hyperactive. Overexpressing HIF-1α in mice erased the protective benefit of removing FGF13, while a selective ERK inhibitor drug, SCH772984, neutralized the damage caused by FGF13 overproduction and improved lung condition in septic animals.
What this means for future sepsis therapies
To a lay reader, the key message is that septic lung injury is not just random tissue destruction; it is powered by a specific molecular circuit inside blood vessel cells and macrophages. FGF13 sits at the center of this circuit, helping to assemble a signaling hub that forces cells into a sugar-guzzling, highly inflammatory state. Although FGF13 levels fall during sepsis—likely as part of a broader stress response—this study shows that the remaining protein is still a potent driver of harm. By blocking either FGF13’s signaling partners or the glycolytic shift it promotes, it may be possible to reduce lung swelling, leakage, and inflammation without paralyzing the body’s ability to fight infection. This work thus highlights FGF13 and the ERK–HIF‑1α–glycolysis axis as promising leads for developing more precise, safer treatments for sepsis-related lung failure.
Citation: Zhu, J., Wang, J., Jiang, C. et al. FGF 13 functions as a regulator of the ERK/aerobic glycolysis axis in the inflammatory state during septic lung injury. Nat Commun 17, 2383 (2026). https://doi.org/10.1038/s41467-026-69014-x
Keywords: septic lung injury, FGF13, endothelial inflammation, aerobic glycolysis, ERK signaling