Clear Sky Science · en
Plasma proteome mediates the associations between air pollution exposure and disease risk
Why the air you breathe matters to your body
Air pollution is often discussed in terms of smoggy skylines and traffic jams, but its most important effects happen inside our bodies. This study uses a powerful new approach to show how dirty air changes the proteins floating in our blood, and how those shifts can raise the risk of many common diseases. By following hundreds of thousands of people over time, the researchers reveal hidden biological links between air pollution and illnesses ranging from lung problems to heart disease and diabetes, and they turn these insights into a score that may one day help tailor prevention to each person.
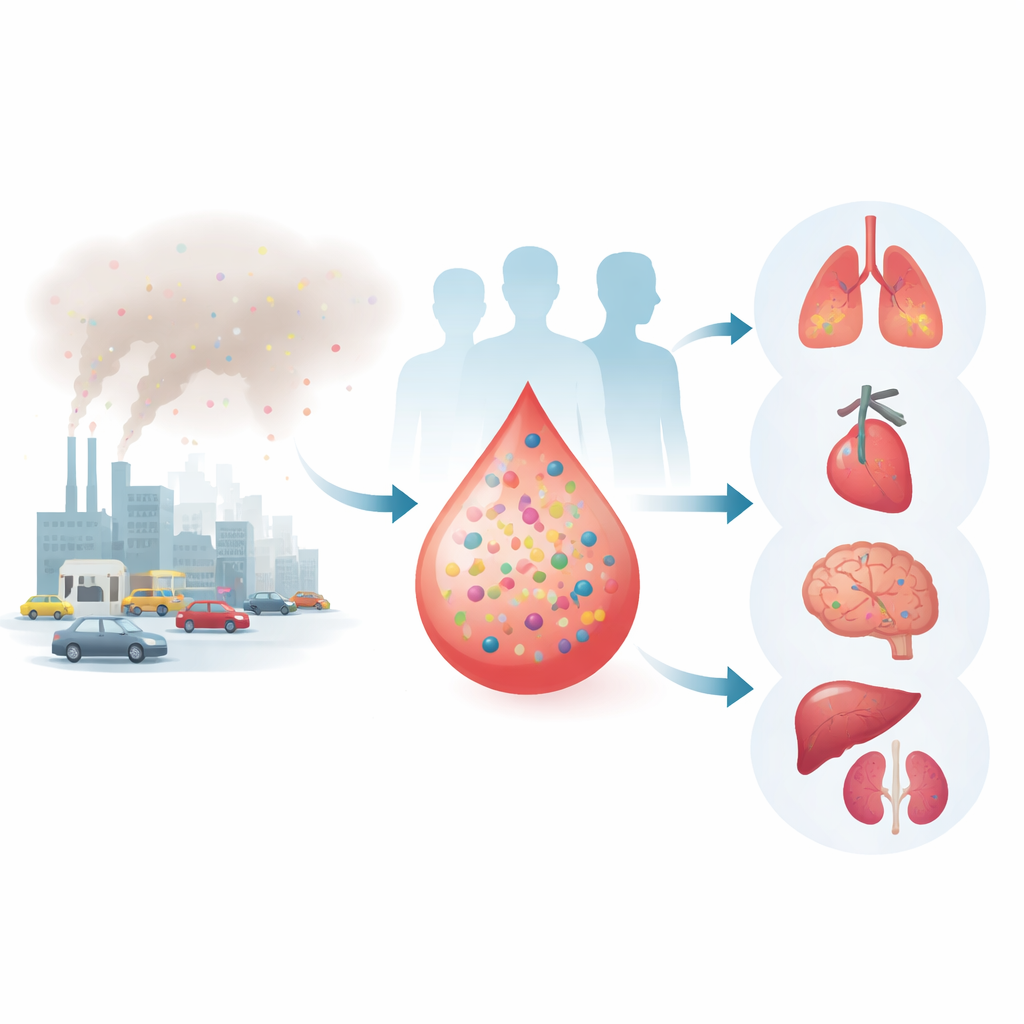
Connecting bad air to many different diseases
The team drew on the UK Biobank, a massive health project tracking more than half a million volunteers. For each person, they estimated long-term exposure to four common air pollutants: fine and coarse particles and two types of nitrogen-based gases. They then followed 36 major diseases, including lung, heart, immune, brain, metabolic, skin conditions, and several cancers. Their analysis showed that 30 of these diseases were linked to higher levels of air pollution. Lung and immune diseases were especially sensitive, while cancer showed weaker but still detectable links. To better reflect the fact that people breathe a mixture of pollutants, the researchers also built a combined "air pollution index" that captured overall exposure, which highlighted even more connections to disease.
How blood proteins tell the story
Next, the study zoomed in on a subset of about 50,000 participants for whom detailed measurements of 1,463 blood proteins were available. Proteins in blood act like messengers and workers, carrying signals between organs and helping run the body’s chemistry. The researchers looked for proteins whose levels changed with pollution exposure and found more than a thousand that responded. Many of these were involved in the immune system and in how cells react to stress and external signals. Different pollutants showed different patterns: particle pollution was tied more strongly to inflammation and cell adhesion, while nitrogen gases were more connected to nerve-related pathways. This suggests that different components of dirty air may damage different systems in the body.
Proteins as the middlemen between air and illness
The crucial step was testing whether these proteins actually sit between pollution and disease, acting as biological middlemen. By combining pollution–protein and protein–disease links in a formal mediation analysis, the researchers found nearly 300 proteins that significantly carried part of the effect of air pollution onto disease risk. On average, changes in the blood proteome explained almost a quarter of the overall link between bad air and disease. The pathways involved differed by disease type: heart and vessel diseases were connected to signaling routes that control cell stress and growth; immune disorders to innate defense and cell-to-cell contact; metabolic diseases to sugar handling; and lung diseases to cell growth and tissue remodeling. Some of the most influential proteins turned out to be involved in inflammation, blood vessel function, and epigenetic regulation, and many are already targets of existing drugs.
A personal score for pollution sensitivity
Building on these results, the team created an Air Pollution Protein Risk Score, or APPRS. They selected 65 proteins that repeatedly acted as mediators for several diseases and combined their levels into a single number for each person. People with higher scores were more likely to develop conditions such as chronic lung disease, pneumonia, kidney disease, heart problems, and type 2 diabetes over time. The score also varied with age, lifestyle, and fitness, and it was higher in patients than in healthy participants, supporting the idea that it reflects how vulnerable someone is to the health effects of polluted air. When added to standard risk models that already included age, sex, smoking, body weight, and basic lab tests, APPRS improved prediction accuracy for early disease onset both in the UK Biobank and in two independent cohorts.
What this means for health and prevention
To a layperson, the main message is that air pollution does not just irritate the lungs in a general way; it leaves a measurable fingerprint on the proteins in our blood and, through them, nudges many organs toward disease. The study shows that these protein changes account for a sizable share of pollution’s harm and can be combined into a single score that captures how sensitive each person may be to dirty air. While more work is needed before such a score is used in clinics, the findings point toward a future where blood tests could help identify people who most need protection from pollution and guide more precise public health actions, all while reinforcing the urgency of cleaning up the air we share.
Citation: Li, W., Li, K., Zhou, P. et al. Plasma proteome mediates the associations between air pollution exposure and disease risk. Nat Commun 17, 2206 (2026). https://doi.org/10.1038/s41467-026-68972-6
Keywords: air pollution, plasma proteome, environmental health, disease risk, biomarkers