Clear Sky Science · en
Gut microbiota-dependent 24-hydroxycholesterol metabolism contributes to capsaicin-induced amelioration of Alzheimer’s disease-like pathology in mice
Spice on the Plate, Protection for the Brain
Alzheimer’s disease robs memory and independence from millions, and effective treatments remain scarce. This study explores an intriguing possibility: that a common dietary spice—capsaicin, the compound that makes chili peppers hot—might help the brain defend itself. By tracing how capsaicin reshapes gut bacteria and cholesterol chemistry, the researchers reveal a gut–brain pathway that appears to ease Alzheimer’s-like changes in mice and link to better brain health markers in people.
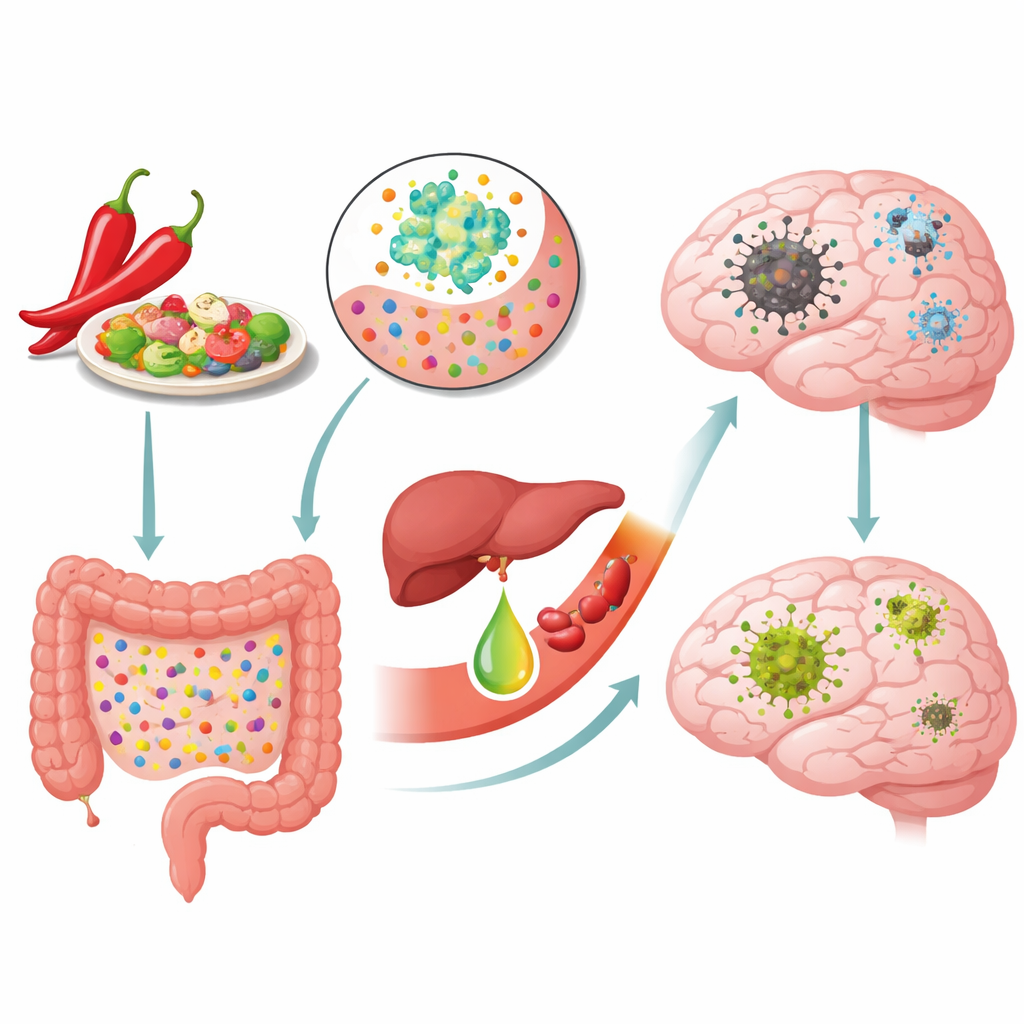
From Chili Bowls to Clearer Thinking
The work began with two groups of Chinese volunteers who varied in how much chili they ate. Those with moderate to high capsaicin intake performed better on standard memory and thinking tests than peers who ate little or no chili, even after accounting for age, education, and health conditions. Among people already diagnosed with mild or full Alzheimer’s-type problems, those who favored spicy, chili-rich diets also showed a lower prevalence of Alzheimer’s diagnoses. These real-world observations suggested that something in chili-heavy diets might be supporting brain function.
A Mouse Model Shows the Same Trend
To test this idea more directly, the team turned to 5×FAD mice, a widely used model that rapidly develops Alzheimer’s-like amyloid plaques and memory loss. For about a month, middle-aged mice received a daily oral dose of capsaicin equivalent to a moderate human intake. Compared with untreated animals, capsaicin-fed mice navigated mazes more efficiently and performed better in object-recognition tasks, indicating improved learning and memory. Their brains contained fewer amyloid plaques and lower levels of inflammatory molecules, and the brain’s immune sentinels—microglia—displayed a calmer, more branching shape associated with healthy surveillance rather than overactivation.
Gut Bacteria as the Hidden Middleman
Interestingly, the benefits of capsaicin did not require its classic receptor, TRPV1: even mice lacking this receptor still improved. Instead, the compound concentrated in the gut, where it strongly reshaped the microbial community. Capsaicin-treated mice had a richer variety of gut species and a shift toward groups such as Firmicutes and, in particular, a genus called Oscillibacter. When researchers transferred gut microbes from capsaicin-fed mice into untreated Alzheimer’s-model mice, the recipients also developed fewer plaques, calmer microglia, less inflammation, and better cognition—despite never receiving capsaicin themselves. Conversely, wiping out gut microbes with broad antibiotics largely erased capsaicin’s protective effects, underscoring that the microbiome is a crucial intermediary.
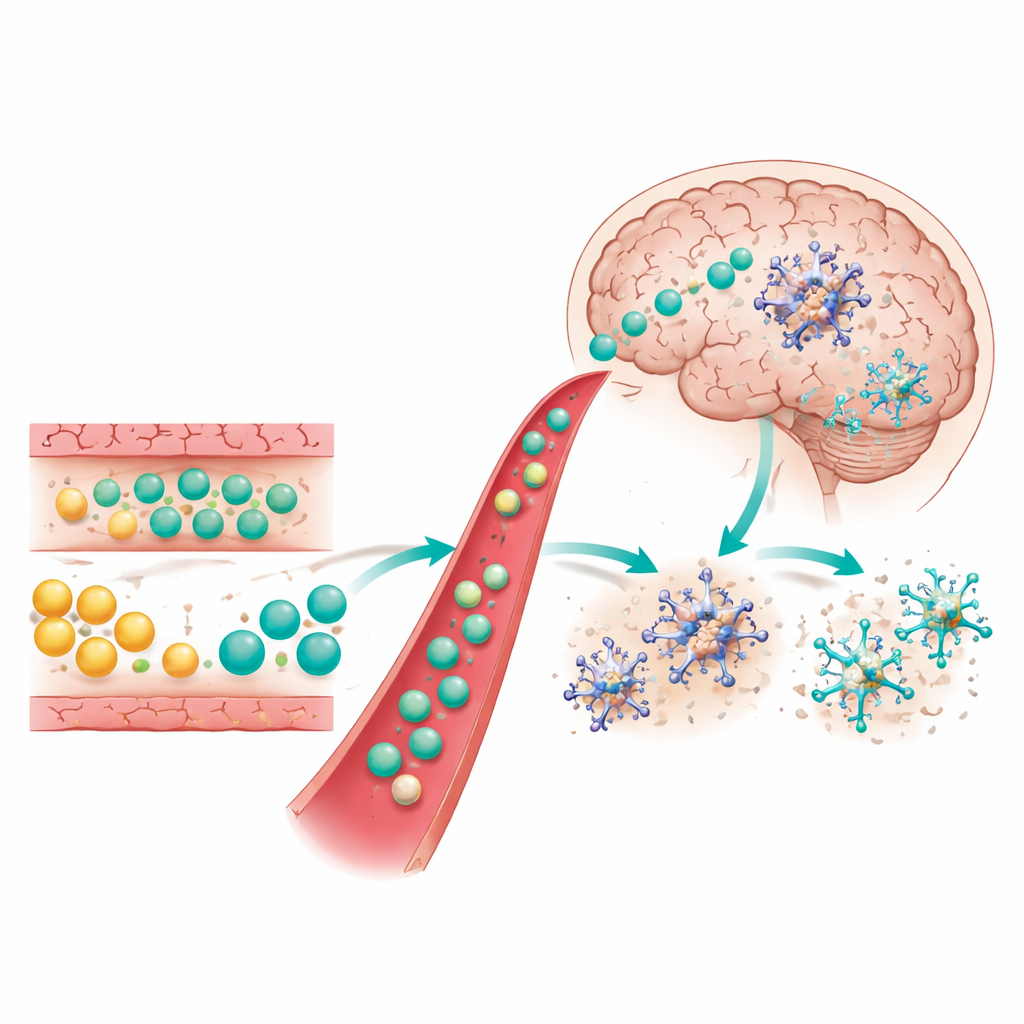
A Cholesterol Byproduct that Calms the Brain
Metabolic profiling revealed a key clue: capsaicin lowered cholesterol and raised levels of 24(S)-hydroxycholesterol (24-HC) in the blood, gut, and brain. This molecule, normally produced in the brain to dispose of excess cholesterol, can also arise from gut bacteria. Among all microbial changes, increases in Oscillibacter correlated most strongly with higher 24-HC and lower cholesterol. Isolated Oscillibacter grown in the lab converted cholesterol into 24-HC, and this activity was boosted by capsaicin. When live Oscillibacter was fed to Alzheimer’s-model mice, it mimicked many benefits of capsaicin: fewer plaques, less inflammation, and sharper memory. Further experiments showed that 24-HC enters the brain, enhances microglia’s ability to engulf amyloid, and dials down inflammatory signals through a nuclear receptor called LXRβ, which then suppresses pro-inflammatory genes.
Human Signals Point in the Same Direction
In the human cohort, people with mild cognitive impairment or Alzheimer’s who reported moderate-to-high chili intake had higher plasma 24-HC, lower circulating amyloid fragments, and reduced levels of two disease-linked tau markers compared with those who ate little chili. Across individuals, higher 24-HC tracked with better cognitive scores, a healthier amyloid ratio, and lower tau markers. While these associations cannot prove cause and effect, they align closely with the mechanistic chain demonstrated in mice: capsaicin shapes gut microbes, which boost 24-HC, which in turn appears to protect the brain’s circuitry.
What This Could Mean for Everyday Diets
Taken together, the findings outline a compelling gut–brain axis: moderate dietary capsaicin encourages specific gut bacteria to convert cholesterol into 24-HC, this molecule travels to the brain, nudges microglia into a plaque-clearing, less inflammatory mode via LXRβ, and ultimately eases both amyloid and tau pathology in animal models. In people, higher chili intake is linked to a biochemical profile and cognitive performance consistent with milder Alzheimer’s-related damage. The authors caution that extremely high chili consumption may have different, possibly harmful effects, and that large, long-term human trials are still needed. Nonetheless, the study suggests that a thoughtfully spiced diet—or drugs that mimic this microbiome–cholesterol pathway—could one day become part of a preventive or therapeutic strategy against Alzheimer’s disease.
Citation: Li, Y., Wang, H., Zhang, D. et al. Gut microbiota-dependent 24-hydroxycholesterol metabolism contributes to capsaicin-induced amelioration of Alzheimer’s disease-like pathology in mice. Nat Commun 17, 2726 (2026). https://doi.org/10.1038/s41467-026-68937-9
Keywords: capsaicin, gut microbiome, Alzheimer’s disease, cholesterol metabolism, microglia