Clear Sky Science · en
No evidence of immediate or persistent analgesic effect from a single dose of psilocybin in three mouse models of pain
Can a Psychedelic Mushroom Drug Ease Long-Term Pain?
Many people living with chronic pain are searching for alternatives to opioids and other standard medications, and psilocybin—the active compound in “magic mushrooms”—has been widely promoted as a potential game‑changer. This study asked a straightforward question in mice: does a single dose of psilocybin actually reduce pain itself, or are the hopes around its pain‑relieving power getting ahead of the evidence?
Why Scientists Looked Beyond the Buzz
Early clinical trials have shown that psilocybin, paired with psychotherapy, can lift depression and anxiety for months after just one guided session. Some older reports and modern surveys hinted that psychedelics might also directly dull physical pain, especially in people with cancer or chronic pain syndromes. But these suggestions came from small, mixed studies where mood, expectations, and other factors are tightly intertwined with how people rate their pain. To separate emotion from raw pain signals, the authors turned to well‑established mouse models, where they could control doses, timing, and conditions, and directly compare psilocybin with proven painkillers such as morphine and buprenorphine.
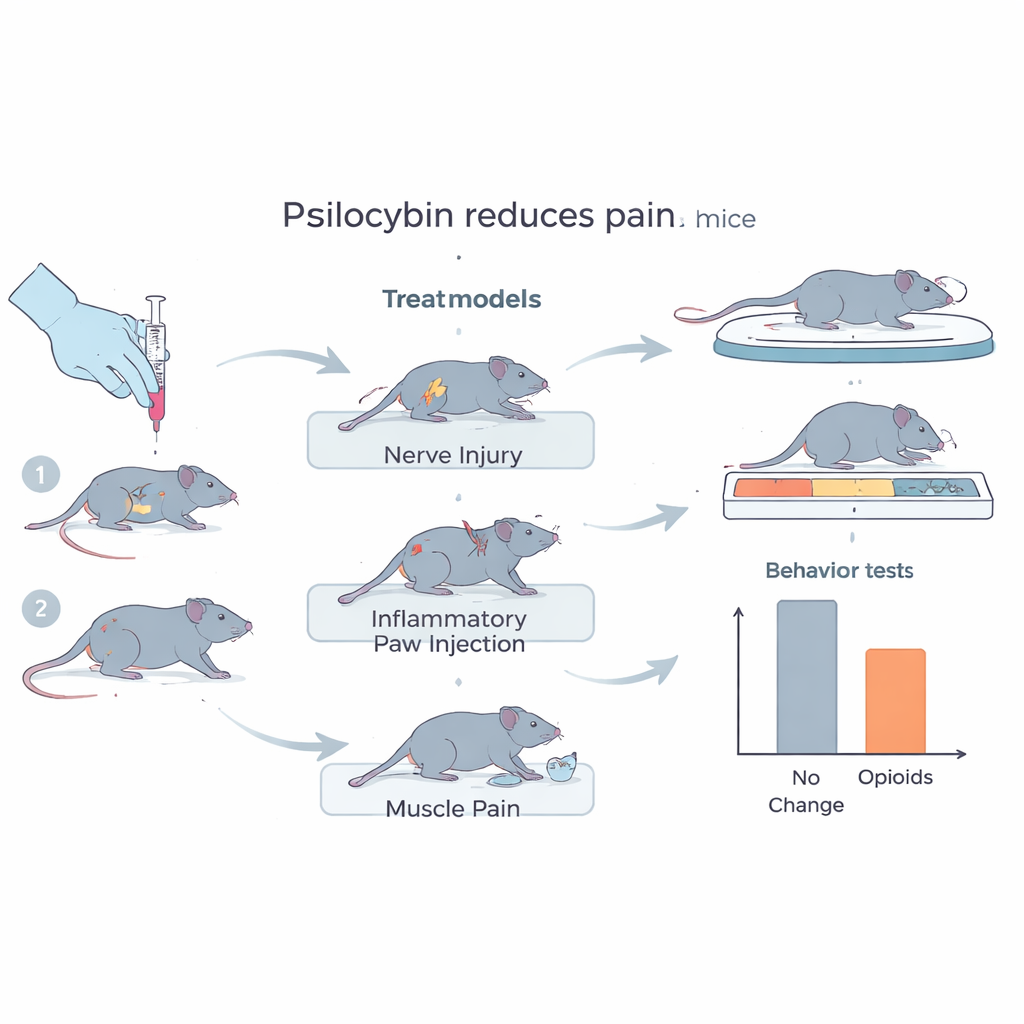
Putting Psilocybin to the Test in Three Types of Pain
The team used three classic mouse models that mimic different kinds of human pain: nerve injury (similar to neuropathic pain after nerve damage), inflamed paw (reflecting inflammatory pain like arthritis), and acid‑induced muscle pain (a stand‑in for widespread muscle pain seen in conditions such as fibromyalgia). Male and female mice received single injections of psilocybin at three doses known to strongly affect the brain. The researchers then ran a battery of behavioral tests that captured both the sensory side of pain (how easily a paw withdraws from pressure or heat) and its functional and emotional impact (whether an injured mouse avoids a task, or shows a “pain face” after surgery). Across all models, doses, time points—from one hour to weeks later—and both sexes, psilocybin failed to reduce pain measures, while standard opioid drugs clearly did.
When Less Pain Isn’t Really Less Pain
One exception seemed to stand out: in some tests, mice given psilocybin reacted less strongly to cold, suggesting that they might be less sensitive to painful temperatures. To probe this, the researchers let mice choose between warm, neutral, and cool surfaces. Rather than becoming numb, psilocybin‑treated mice actively sought out warmer spots and avoided the cooler ones. Thermal imaging revealed why: psilocybin caused a marked, dose‑dependent drop in body temperature that peaked about half an hour after injection and then resolved. In other words, the drug was disrupting the animals’ internal thermostat, driving them to seek heat, not truly switching off their pain circuits.
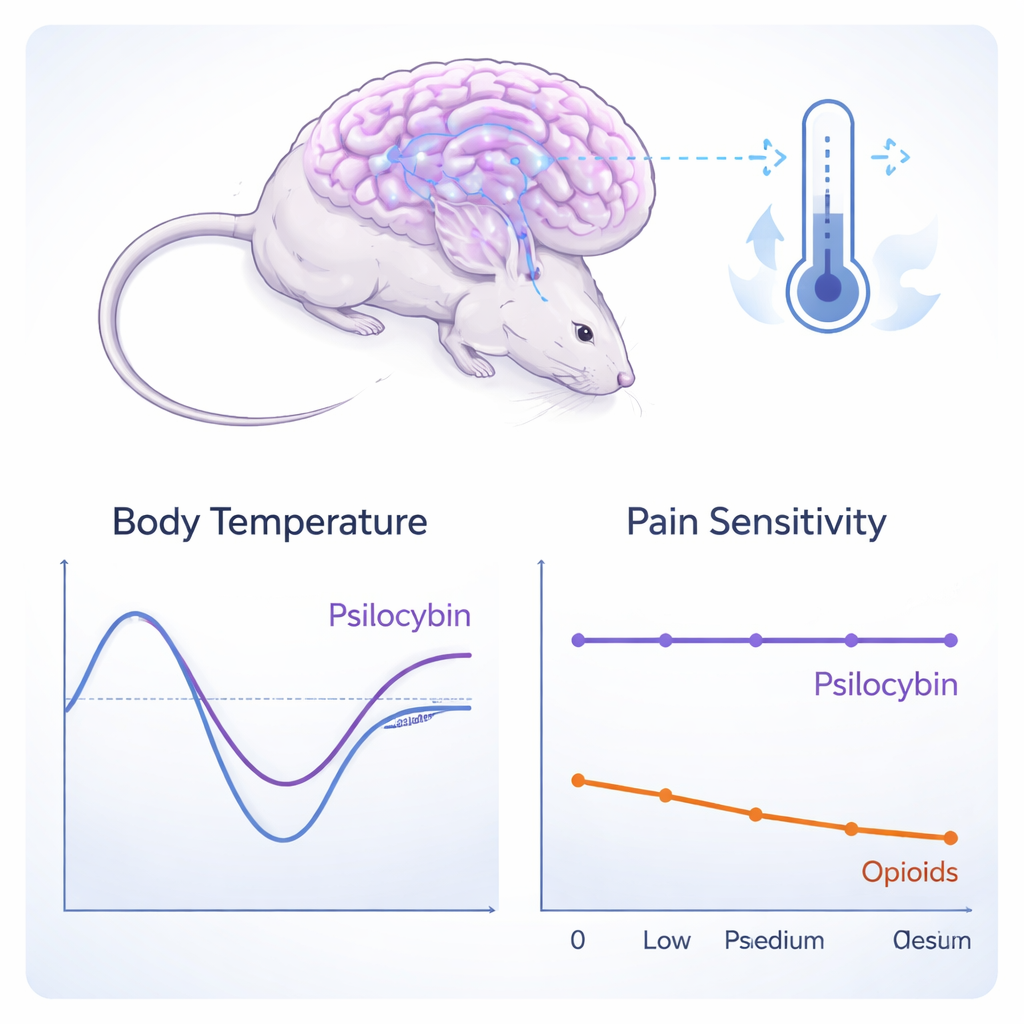
What the Study Says About Pain Relief and Psychedelics
These findings challenge the idea that psilocybin itself is a powerful, long‑lasting painkiller—at least in mice and under rigorous testing. The drug clearly activates the brain’s serotonin system and changes behavior, but it did not lessen mechanical, heat, or most cold pain responses, nor did it improve signs of discomfort or function in tasks that mirror daily‑life limitations. The apparent benefit in cold sensitivity was best explained by drug‑induced hypothermia rather than genuine pain relief.
What This Means for People in Pain
For people hoping that a single psilocybin session might directly erase chronic pain, this work is a cautionary note. It suggests that, in animals, psilocybin does not act like a straightforward analgesic the way opioids or some other pain medicines do. That does not rule out the possibility that psychedelics could help some patients cope better with pain by improving mood, reducing anxiety, or changing how they think about their symptoms—subtle, whole‑person effects that mice cannot fully model. But it does underscore the need for careful, controlled human trials that separately measure physical pain, emotional well‑being, and quality of life before psilocybin can be responsibly promoted as a treatment for chronic pain.
Citation: Gregory, N.S., Girard, T.E., Ram, A. et al. No evidence of immediate or persistent analgesic effect from a single dose of psilocybin in three mouse models of pain. Nat Commun 17, 1916 (2026). https://doi.org/10.1038/s41467-026-68763-z
Keywords: psilocybin, chronic pain, mouse models, analgesia, serotonin