Clear Sky Science · en
Tumour-intrinsic features shape T cell differentiation through precursor to symptomatic multiple myeloma
Why this research matters
Multiple myeloma is a blood cancer that forms in the bone marrow and is almost always preceded by quieter, early conditions that may or may not turn into full-blown disease. Many people live for years with these precursors, unsure if or when they will progress. This study asks a timely question: can we read the “mood” and history of the immune system—especially T cells—to understand how myeloma develops, how it responds to treatment, and who is at highest risk of progressing?
The body’s cancer-fighting scouts
T cells are versatile immune cells that can recognize and destroy abnormal cells, including cancers. In solid tumors like lung or skin cancers, long-lasting stimulation can push T cells into an exhausted state where they become ineffective, a change that modern immunotherapies try to reverse. The authors assembled a huge single-cell map of more than a million cells from the bone marrow and blood of people with multiple myeloma, its precursor stages (MGUS and smoldering myeloma), and non-cancer controls. By reading out both gene activity and the unique receptor sequences that define each T cell clone, they reconstructed how T cells are organized, how “old” or “experienced” they look, and how closely they track the underlying tumor.
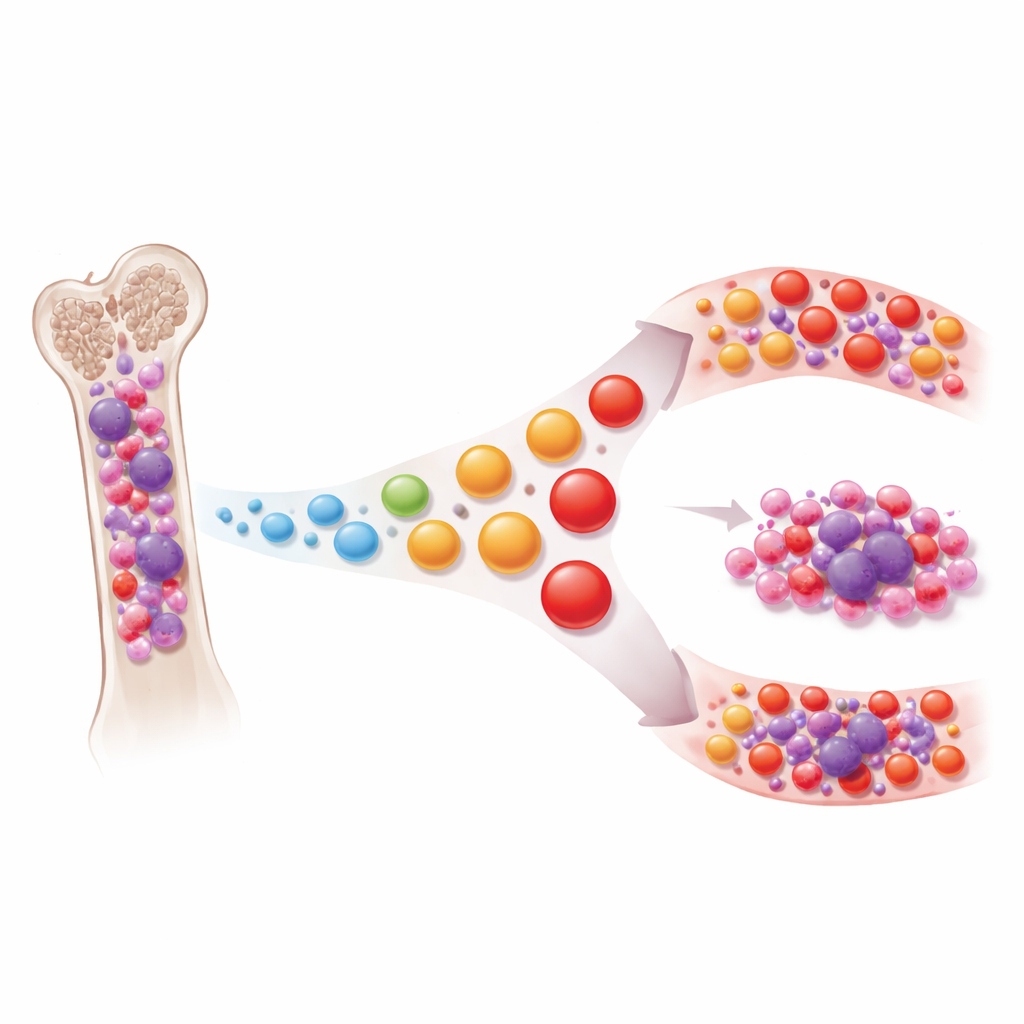
Not tired, but prematurely aged
Contrary to what is seen in many solid cancers, the team found that T cells in myeloma are rarely truly exhausted. Cells bearing classic exhaustion markers were largely confined to a single unusual patient. Instead, bone marrow T cells in smoldering and symptomatic myeloma shifted away from naïve, early-stage cells toward highly experienced “terminal memory” types that resemble T cells in older individuals. This pattern—called T cell skewing—paralleled the natural aging of the immune system but appeared exaggerated in patients, as if their T cells had aged faster than the rest of them. The more advanced the disease and the higher the tumor burden, the stronger this skewing toward late-stage memory cells, and similar changes could be seen spilling over into the blood.
Clues from T cell fingerprints
Each T cell carries a unique receptor, and cells that share the same receptor sequence belong to a clone that has expanded in response to some trigger. By tracking these receptors, the investigators showed that myeloma marrows contain many expanded T cell clones with features of potent killer cells. These clones did not mainly recognize common viruses. Instead, they bore a distinct “non-viral” gene signature linked to strong cytotoxic machinery and were enriched in people with myeloma compared with precursor states. Tumors that were better at displaying fragments of protein on their surface—through higher activity of antigen-presentation genes—tended to be associated with these non-viral, highly differentiated T cells. Patients whose tumors showed this stronger immune engagement generally had better survival, hinting that these T cells are, at least in part, truly anti-tumor.
Treatment, relapse, and early warning signs
The study also followed patients undergoing autologous stem cell transplantation, a common intensive therapy. After transplant, the T cell receptor repertoire became more dominated by a few large clones. Many of these expanding clones could be traced back to terminally differentiated CD8 T cells that were already present before treatment and carried the same non-viral, myeloma-associated signature. Patients who still had residual cancer after transplant tended to have especially clonal, skewed T cell repertoires, suggesting that a vigorous yet aging-like T cell response may fail to fully clear disease. Looking earlier in the disease course, the authors found that smoldering patients who later progressed to active myeloma often had a drop in regulatory CD4 T cells—cells that normally help keep immune responses and the bone marrow environment in balance. Low levels of these cells predicted faster progression, independently of existing clinical risk scores.
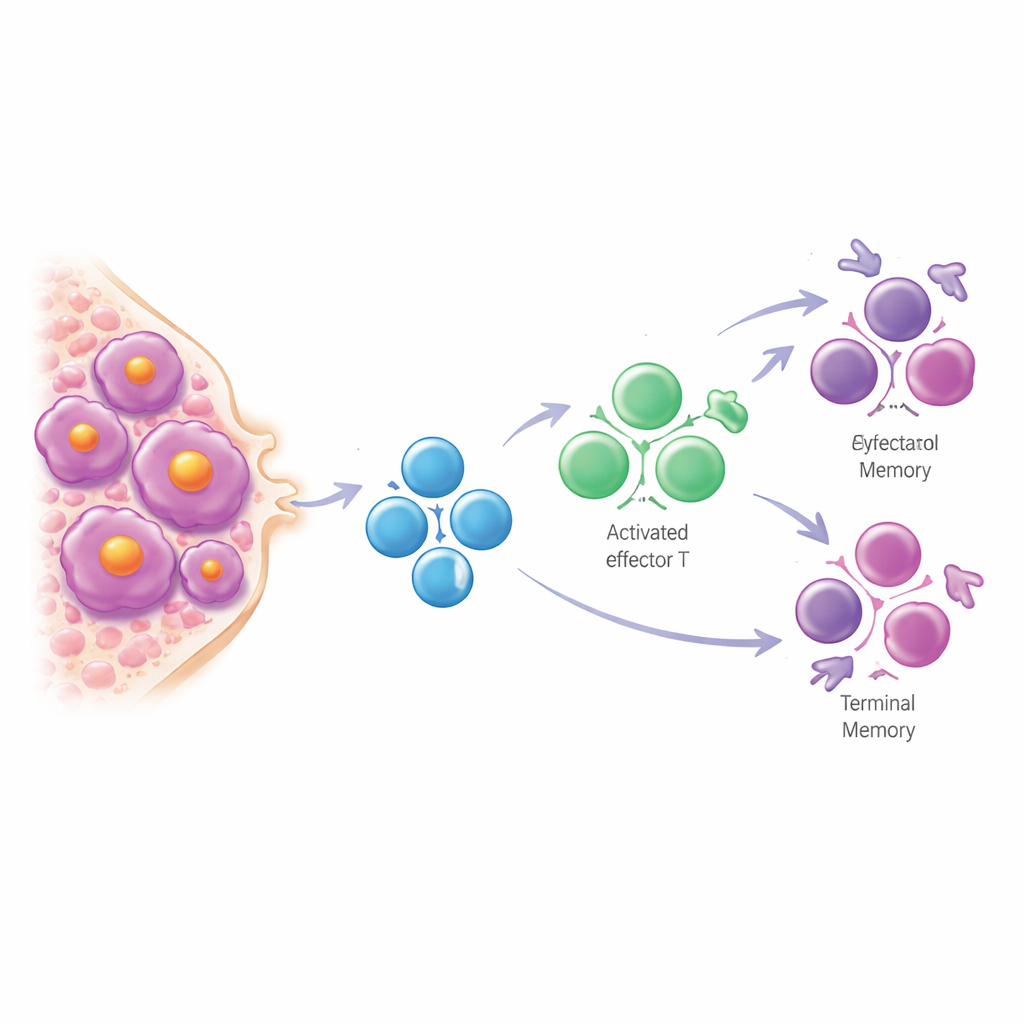
What this means for patients
For people living with myeloma and its precursor stages, this work reframes how the immune system responds to the cancer. Rather than simply becoming exhausted, T cells in myeloma appear to be chronically driven into a late, aged state by ongoing battles with tumor cells. This skewed, clonal T cell landscape reflects tumor burden, shapes response to treatments like transplantation and T cell–engaging drugs, and, in the case of regulatory T cell loss, can even flag individuals at higher risk of progression from smoldering to symptomatic disease. In the long run, these insights could guide new immunotherapies that refresh or redirect T cells, and help clinicians use immune features alongside traditional markers to time monitoring and early intervention more precisely.
Citation: Foster, K.A., Rees, E., Ainley, L. et al. Tumour-intrinsic features shape T cell differentiation through precursor to symptomatic multiple myeloma. Nat Commun 17, 2400 (2026). https://doi.org/10.1038/s41467-026-68718-4
Keywords: multiple myeloma, T cells, immune aging, single-cell sequencing, cancer immunology