Clear Sky Science · en
Combinatory differentiation of human induced pluripotent stem cells generates functional thymic epithelium driving dendritic cell and CD4/CD8 T cell development
Building a Training Ground for Immune Cells
The human immune system depends on a small, fragile organ called the thymus, where new T cells learn to recognize germs without attacking the body itself. As we age, or in certain genetic diseases, the thymus shrinks or fails, leaving people vulnerable to infection and cancer. This study shows how scientists can recreate key parts of the thymus in the lab using reprogrammed stem cells, opening a path toward custom-built immune systems and safer, more controllable T cell therapies.
Why the Thymus Matters
The thymus acts as a school for T cells, a type of white blood cell that patrols the body for infected or cancerous cells. Inside the thymus, developing T cells are tested: those that react properly to foreign targets are kept, while those that might attack the body are eliminated. This education is orchestrated by specialized support cells called thymic epithelial cells, or TECs, which form distinct regions known as the cortex and medulla. Recreating these TECs outside the body has been difficult, and most previous attempts produced immature cells that had to be transplanted into animals to finish developing.
Guiding Stem Cells Step by Step
To overcome this, the researchers started with human induced pluripotent stem cells, which can be made from adult tissues and then coaxed into almost any cell type. They designed a carefully planned, two-week “road map” that mimics how the thymus forms during early development. Using a statistical strategy called design of experiments, combined with broad gene activity measurements, they tested many combinations of growth signals in parallel. By turning key pathways on or off at precise times, they drove the stem cells through several intermediate stages toward thymic epithelial progenitors—immature TEC-like cells that carry hallmark genes such as FOXN1 and PAX9 and resemble early thymic cortex cells.
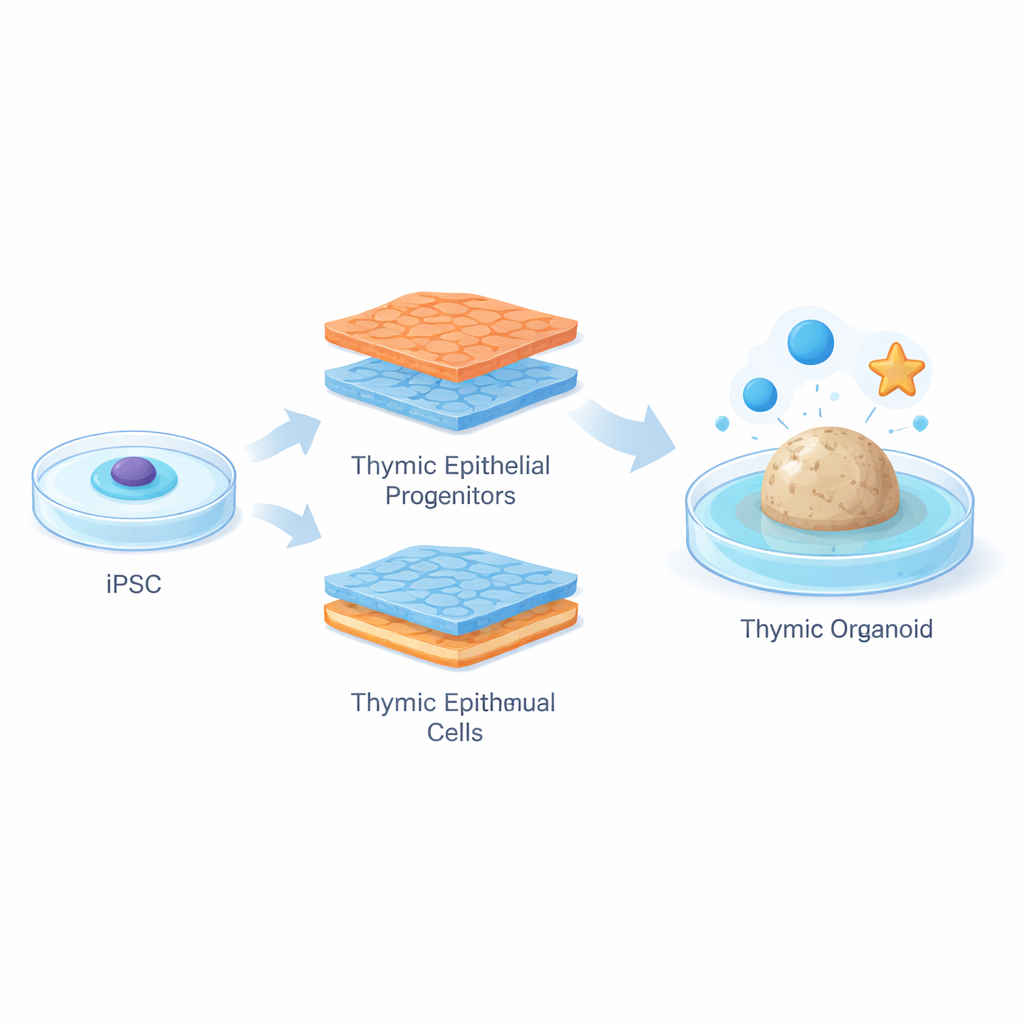
Assembling Miniature Thymus Organoids
Having generated large numbers of these progenitor cells, the team mixed them with rare blood-forming precursor cells freshly isolated from human thymus tissue. The mixture was compressed into small clusters and embedded in a soft fibrin gel at an air–liquid interface, forming three-dimensional “human thymic organoids.” Within days, the organoids grew into complex spheres with projections extending through the gel. Detailed imaging and gene analyses showed that many epithelial cells in these organoids matured into medulla-like cells that displayed high levels of HLA-DR, a molecule needed to present self-antigens to developing T cells. The organoids also began to express a broad set of tissue-like genes, echoing how real thymic medulla cells help enforce tolerance to many different organs.
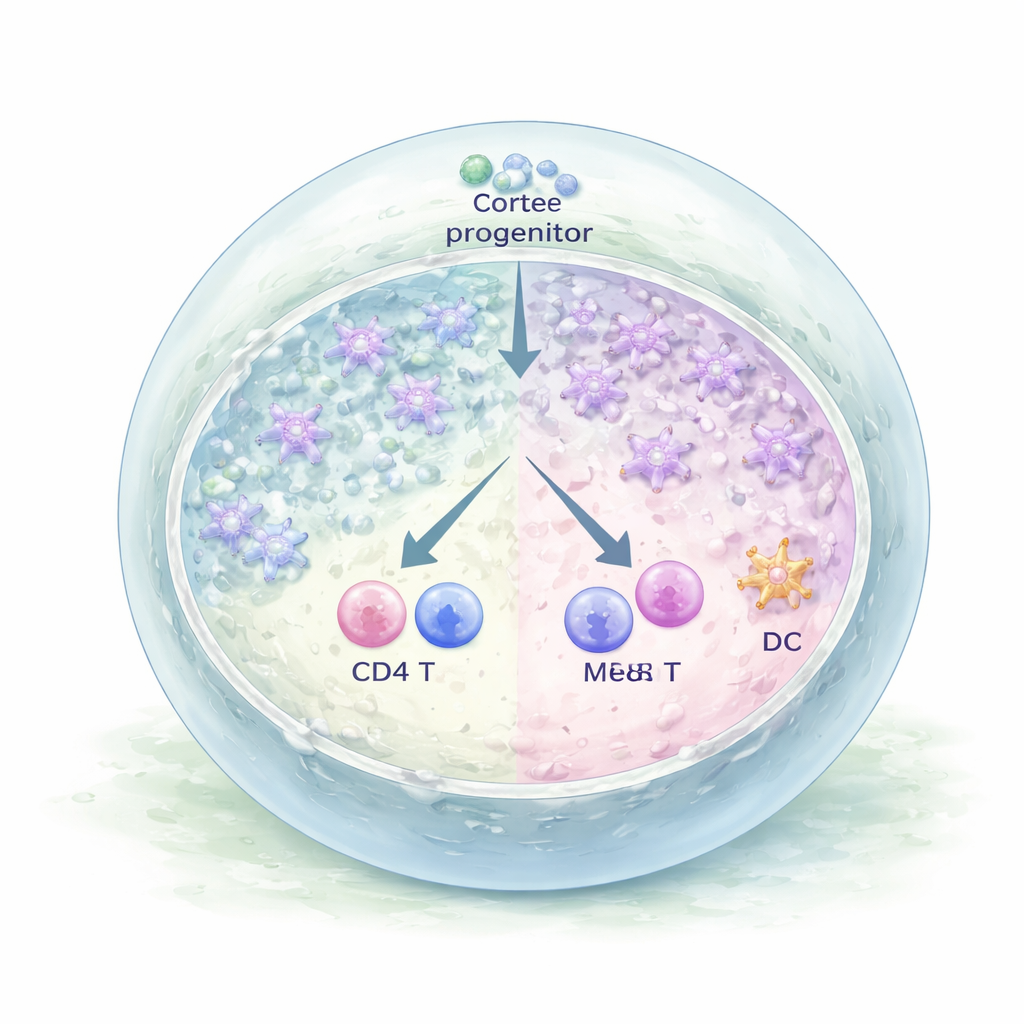
Training Multiple Types of Immune Cells
The organoids did more than just look like thymus tissue—they functioned like it. When scientists examined the blood-derived cells after several weeks, they found that early progenitors had lost their stem-cell identity and developed into T cells bearing complete T cell receptors. Both main T cell branches appeared: conventional alpha–beta T cells and gamma–delta T cells. Among them were mature CD4 and CD8 single-positive T cells carrying surface markers (CCR7 and CD62L) typical of recent thymic emigrants ready to enter the bloodstream. Single-cell profiling also revealed that some progenitors within the organoids took a different path, becoming dendritic cells, another key immune cell type that collaborates with TECs in shaping a safe T cell repertoire.
From Lab Model to Future Therapies
Altogether, this work delivers a fully in vitro, human thymus-like organoid built from pluripotent stem cells that can guide immature blood cells into diverse, functional T cells and dendritic cells. For lay readers, the takeaway is that researchers are learning to rebuild the thymus in a dish—both its structure and its teaching function. With further refinements, such organoids could help repair damaged immune systems in children born without a working thymus, rejuvenate T cell production in older adults, and provide a controlled factory for producing customized T cells for cancer immunotherapy and other cell-based treatments.
Citation: Provin, N., d’Arco, M., Le Bozec, A. et al. Combinatory differentiation of human induced pluripotent stem cells generates functional thymic epithelium driving dendritic cell and CD4/CD8 T cell development. Nat Commun 17, 1969 (2026). https://doi.org/10.1038/s41467-026-68675-y
Keywords: thymic organoids, induced pluripotent stem cells, T cell development, thymic epithelial cells, regenerative immunology