Clear Sky Science · en
Human type-1 innate lymphoid cells control leukemia stem cell differentiation and limit acute myeloid leukemia development
Why our own immune cells matter in leukemia
Acute myeloid leukemia (AML) is an aggressive blood cancer that often comes back even after tough chemotherapy. A key culprit is a small pool of “starter” leukemia cells that can restart the disease. This study shows that a little‑known branch of the immune system, called type‑1 innate lymphoid cells (ILC1s), can push these starter cells away from dangerous paths of growth and help slow leukemia in experimental models. The work also outlines a possible way to manufacture helpful ILC1s from donated umbilical cord blood as a future treatment.
The problem of stubborn leukemia starter cells
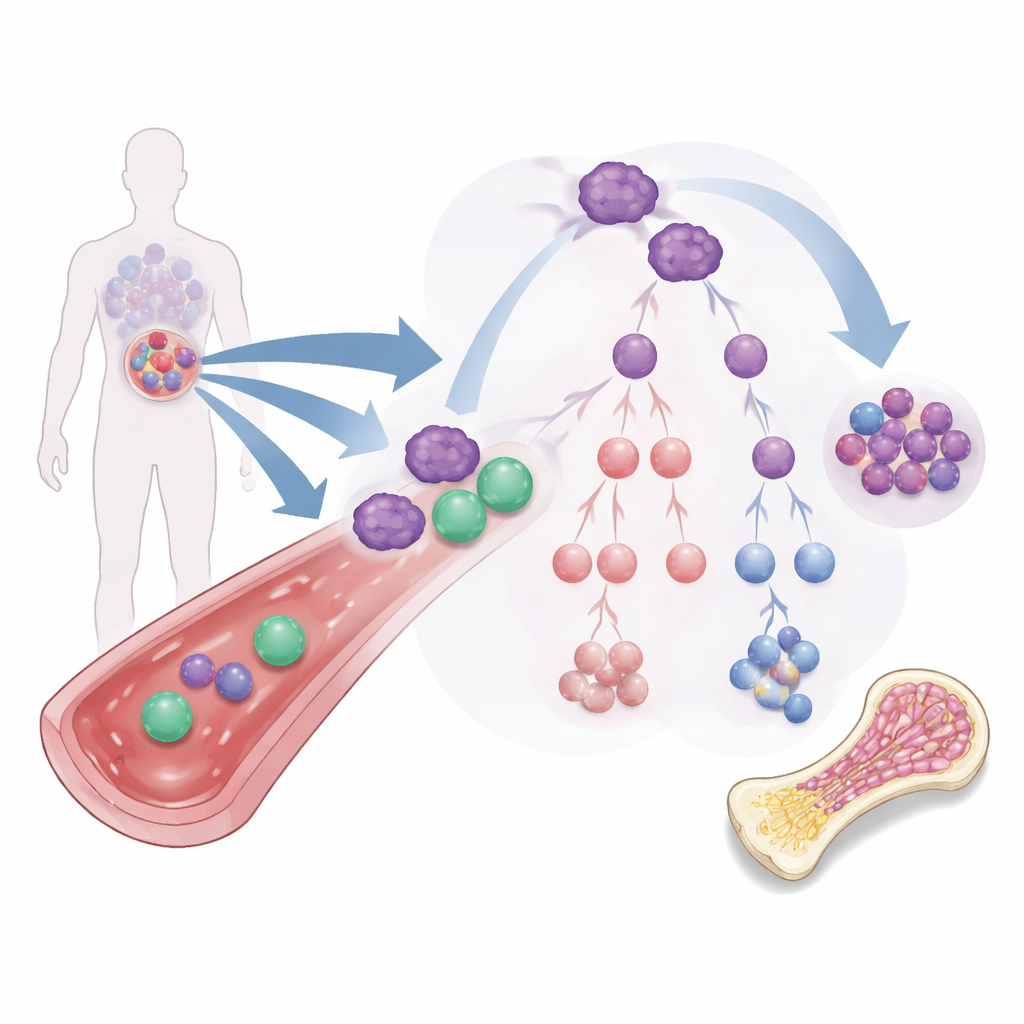
Most AML treatments target the bulk of leukemia cells circulating in blood and bone marrow. But a rarer subset, known as leukemia stem cells, behaves more like seeds: they can self‑renew, resist standard drugs, and repopulate the cancer. These cells can mature along several branches into different leukemic cell types, some of which still retain the ability to self‑renew or to shield the cancer from the immune system. Because of this branching “family tree,” simply shrinking the visible leukemia is not enough; therapies must change the fate of these starter cells or remove them altogether.
A missing line of defense in patients
ILC1s are fast‑acting immune cells that do not need prior exposure to recognize threats. The researchers compared ILC1s in the blood of healthy volunteers and people with AML. They found that patients had fewer ILC1s overall, and the cells they did have were less active. Using single‑cell RNA sequencing and flow cytometry, the team showed that patient ILC1s made lower levels of key killing molecules and important immune signals, and displayed fewer activation receptors on their surface. Notably, patients with higher proportions of ILC1s tended to have fewer leukemia blasts, hinting that when these cells are present and functional, they help keep the disease in check.
How healthy ILC1s steer leukemia cells off harmful paths
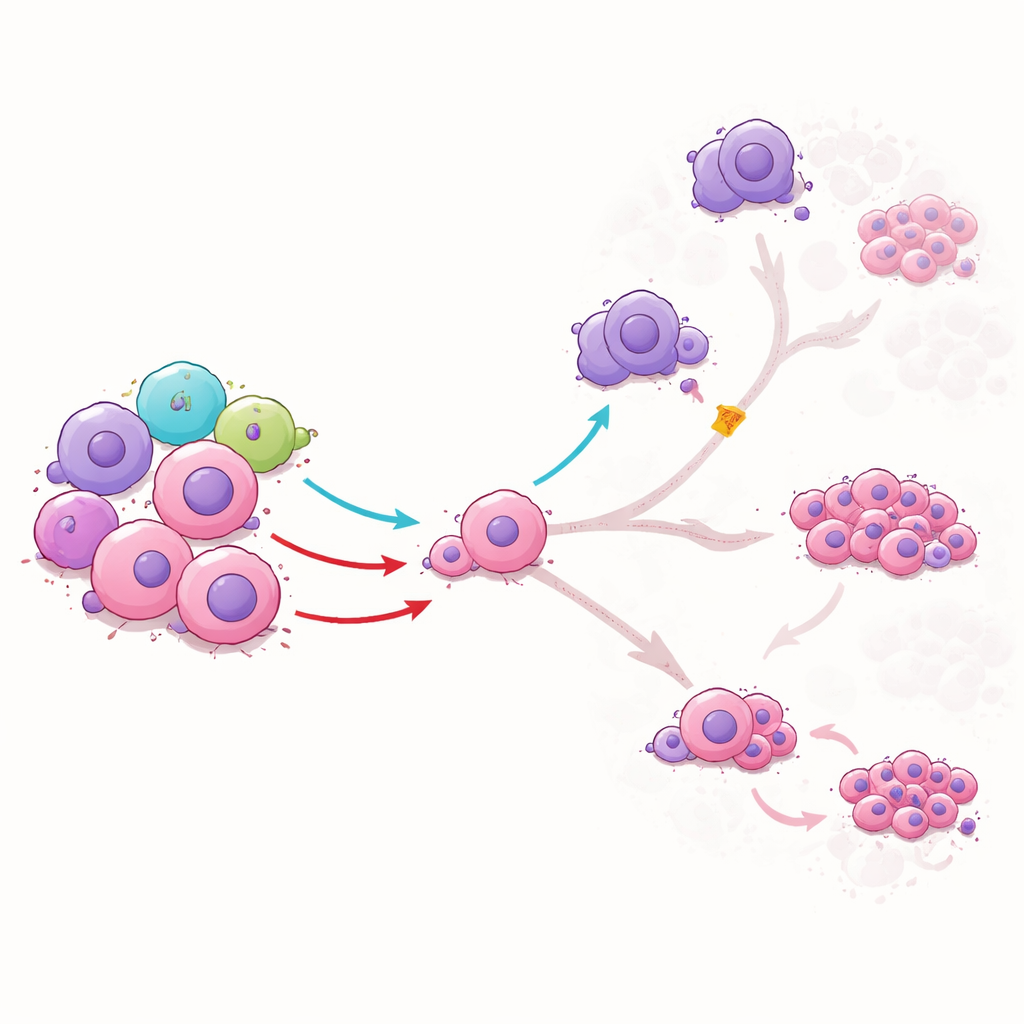
To understand what ILC1s actually do to leukemia stem cells, the team grew them together in the lab. Healthy‑donor ILC1s did not simply wipe out the stem cells; instead, they changed how these cells matured. One ILC1 signal, called TNFα, pushed stem cells into an intermediate state and reduced their transition into more dangerous, rapidly dividing leukemia cells. It also curtailed the stem cells’ ability to become macrophage‑like cells that normally suppress immune responses and nurture leukemia. Another signal, IFNγ, limited the stem cells’ progression into certain highly treatment‑resistant forms. When the researchers blocked these signals with antibodies, the protective effects disappeared, showing that ILC1s guide leukemia development through specific chemical messages.
Turning cord blood into an immune therapy
Because natural ILC1s are rare in adult blood, the team sought a renewable source. They showed that stem cells from donated umbilical cord blood can be coaxed in culture to become a particular subset of ILC1s that lacks a surface marker called CD161 but still carries the right transcription factors and killing tools. These lab‑grown ILC1s expanded roughly 700‑fold, attacked leukemia stem cells while sparing normal blood‑forming stem cells, and carried strong cytotoxic molecules. When transferred into specialized mice bearing human leukemia stem cells, these ILC1s reduced leukemia growth and prolonged survival, an effect that depended on IFNγ. In side‑by‑side tests, they performed at least as well as similarly generated natural killer cells.
What this could mean for future treatment
Overall, the study reveals that in AML, a natural immune brake—the ILC1 population—is both shrunken and weakened. When supplied from healthy donors or generated from cord blood, ILC1s can tip leukemia stem cells away from the most harmful and therapy‑resistant fates, reduce leukemia‑supporting macrophage‑like cells, and slow disease in mouse models. For a layperson, the key message is that scientists are learning not just to kill cancer cells, but to “coach” the earliest leukemia seeds into less dangerous directions using the body’s own rapid‑response immune cells. With further development and safer, scalable manufacturing, ILC1‑based cell therapies could one day complement existing treatments to keep AML from returning.
Citation: Li, Z., Ma, R., Tang, H. et al. Human type-1 innate lymphoid cells control leukemia stem cell differentiation and limit acute myeloid leukemia development. Nat Commun 17, 2377 (2026). https://doi.org/10.1038/s41467-026-68582-2
Keywords: acute myeloid leukemia, leukemia stem cells, innate lymphoid cells, cancer immunotherapy, umbilical cord blood