Clear Sky Science · en
Spatiotemporal regulation of energetic charge dictates T cell function
Why the body’s immune batteries matter
Our immune system depends on T cells, white blood cells that hunt down infected or cancerous cells. Like all working cells, T cells need fuel, and this study asks a deceptively simple question: how much energy do individual T cells actually have at different places in the body and at different times of day—and does that energy level change how well they work? The answers reveal that T cells run on a kind of internal “battery charge” that rises and falls with nutrient availability and daily rhythms, and that this charge directly shapes how powerfully they can fight.
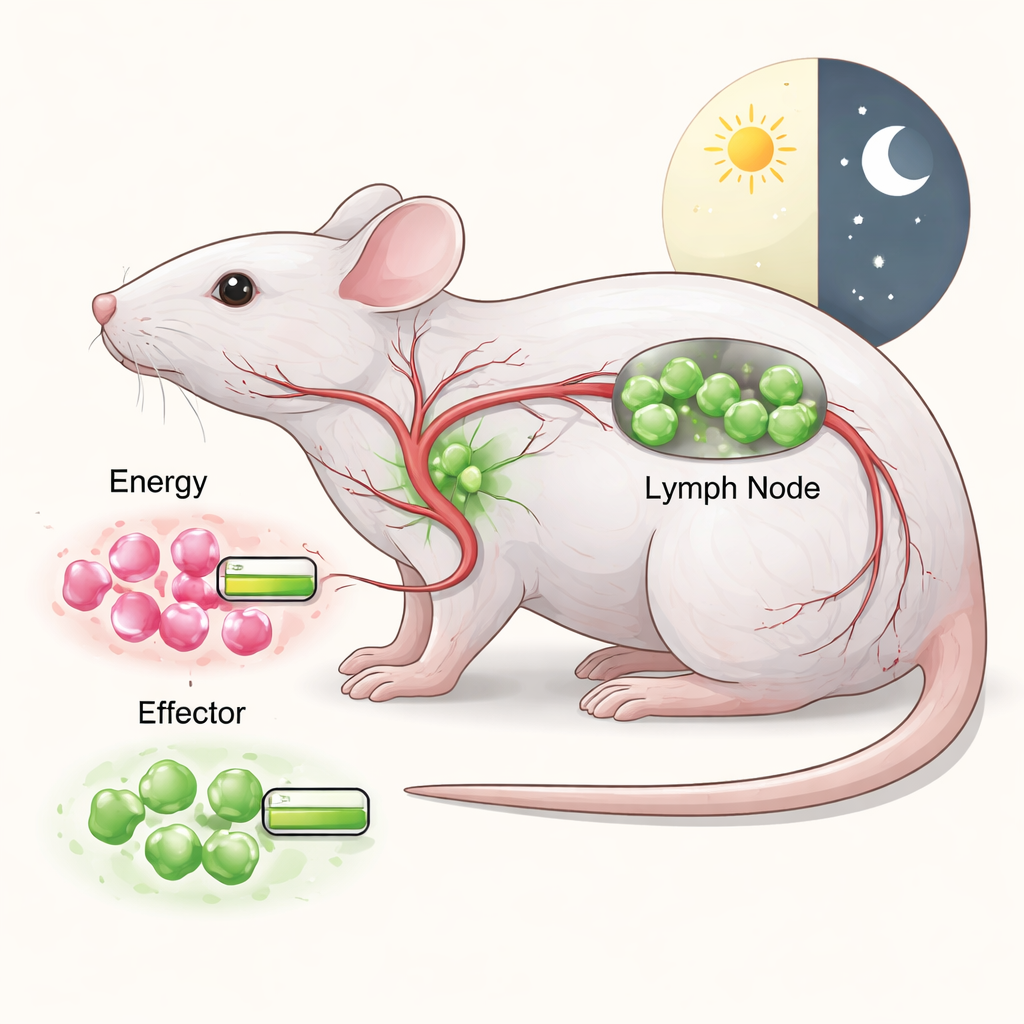
Measuring the inner fuel gauge of immune cells
The researchers used a special strain of mice whose immune cells carry a fluorescent sensor that reports the ratio of ATP to ADP—two molecules that act like charged and partially discharged batteries inside cells. A high ATP:ADP ratio means a cell is energetically rich; a lower ratio means its reserves are more depleted. With a method they call SPICE-Met, the team could read this energy ratio in many immune cell types at once using flow cytometry, while also briefly blocking specific fuel pathways such as mitochondrial respiration or sugar breakdown. This let them see not only how much energy different cells had, but also which fuels—glucose, fats, or amino acids—were most important for keeping that energy high.
Different immune jobs, different energy levels
When the authors examined blood cells, they found that immune cells do not all carry the same energetic charge. B cells, neutrophils, and especially “effector” T cells and natural killer (NK) cells—those actively ready to attack—had the highest ATP:ADP ratios. By contrast, quieter “naïve” and central memory T cells, which are on standby until they encounter a threat, had lower energetic charge. Cells with the most energy relied heavily on glycolysis, the rapid burning of glucose, whereas resting T cells leaned more on mitochondrial respiration. Importantly, simply saying a cell “uses mitochondria” or “uses glycolysis” was not enough: what mattered was how much each pathway actually contributed to the final energy ratio.
How location and sugar supply reshape T cell power
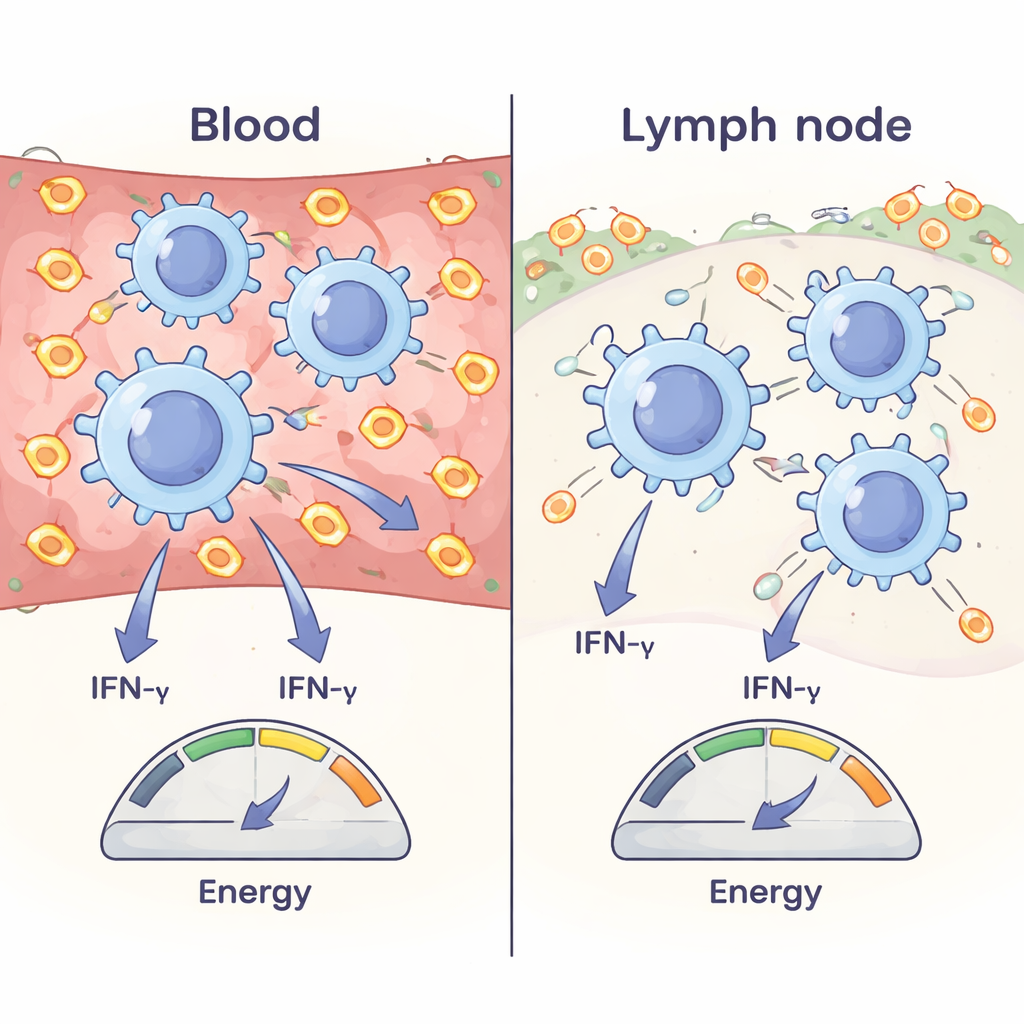
A key discovery was that the same type of effector T cell carried different energy charge depending on where it was. Effector T cells in the blood had a much higher ATP:ADP ratio than their counterparts in lymph nodes, even when they recognized the same vaccine antigen. By transferring T cells from lymph nodes into new mice and then sampling them only hours later, the team showed that this difference is not hard-wired: once effector T cells move into the blood, their energetic charge rises; when they sit in lymph nodes, it falls. The main reason is glucose availability. Blood is relatively rich in sugar, whereas lymph nodes are comparatively sugar-poor. In lymph nodes, effector T cells upregulate the glucose transporter GLUT1—an emergency response to low glucose—and show signs of mild energetic stress. When glucose uptake is blocked, blood effector T cells quickly lose energetic charge, while lymph-node cells compensate more by burning fats and amino acids.
Daily rhythms shape immune strength
The team also explored how time of day affects immune cell energy. Mice kept on a strict light–dark schedule showed strong circadian swings in T cell energetic charge: effector T cells, NK cells, and related cells had roughly twice as much energetic charge at some times as at others, with peaks at the beginning of the rest phase. These oscillations matched changes in glucose levels in the blood and persisted even under constant darkness, indicating a true internal clock effect. When mice were briefly fasted, blood glucose dropped and the energetic charge of effector T cells and NK cells declined, while naïve T cells remained largely unchanged, underlining how dependent active fighters are on abundant nutrients.
Energy charge as a dial for T cell attack
Finally, the authors asked whether changing this energetic charge actually alters T cell performance. Effector T cells collected from the blood were larger and produced more of the key antiviral and anticancer molecule IFN-γ, as well as more perforin, than matching cells from lymph nodes. Across the day, the capacity of T cells to make IFN-γ was highest when their energetic charge was greatest. In lab experiments, the researchers systematically lowered T cell energy using metabolic inhibitors; as ATP:ADP went down, IFN-γ production, cell size, and perforin levels dropped in parallel. Together, these findings show that a T cell’s internal energy charge is not just a passive readout—it is a tunable control knob that links nutrient supply and daily rhythms to how strongly the immune system can respond.
Citation: Chikina, A.S., Corre, B., Lemaître, F. et al. Spatiotemporal regulation of energetic charge dictates T cell function. Nat Commun 17, 770 (2026). https://doi.org/10.1038/s41467-026-68559-1
Keywords: T cell metabolism, immune energy, glucose and immunity, circadian immunity, ATP ADP ratio