Clear Sky Science · en
Impact of a single fecal microbiome transplantation in adult women with anorexia nervosa: an open-label feasibility pilot trial
Why Gut Bacteria Matter in Eating Disorders
Anorexia nervosa is often thought of as a disorder of thoughts, feelings, and food. But this study asks a very different question: what if tiny organisms living in the gut also play a role? Researchers tested whether moving gut bacteria from healthy donors into women with anorexia—using a procedure called fecal microbiota transplantation (FMT)—is practical, safe, and able to quickly change the mix of microbes in the intestines. The work does not claim to cure anorexia, but it explores a new biological angle on a serious and hard‑to‑treat illness.
A New Use for an Unusual Treatment
FMT is already an accepted treatment for stubborn intestinal infections, where stool from a healthy donor is processed and given to a patient to restore a balanced gut community. Because people with anorexia often have disturbed gut bacteria, constipation, and digestive discomfort that do not fully resolve with refeeding, the team wondered if FMT could be a useful add‑on to standard care. In this pilot trial, they focused on feasibility: Would patients agree to the procedure, tolerate it, and complete the study steps? They also wanted an early look at whether the gut bacteria and related body signals would change after just one treatment.
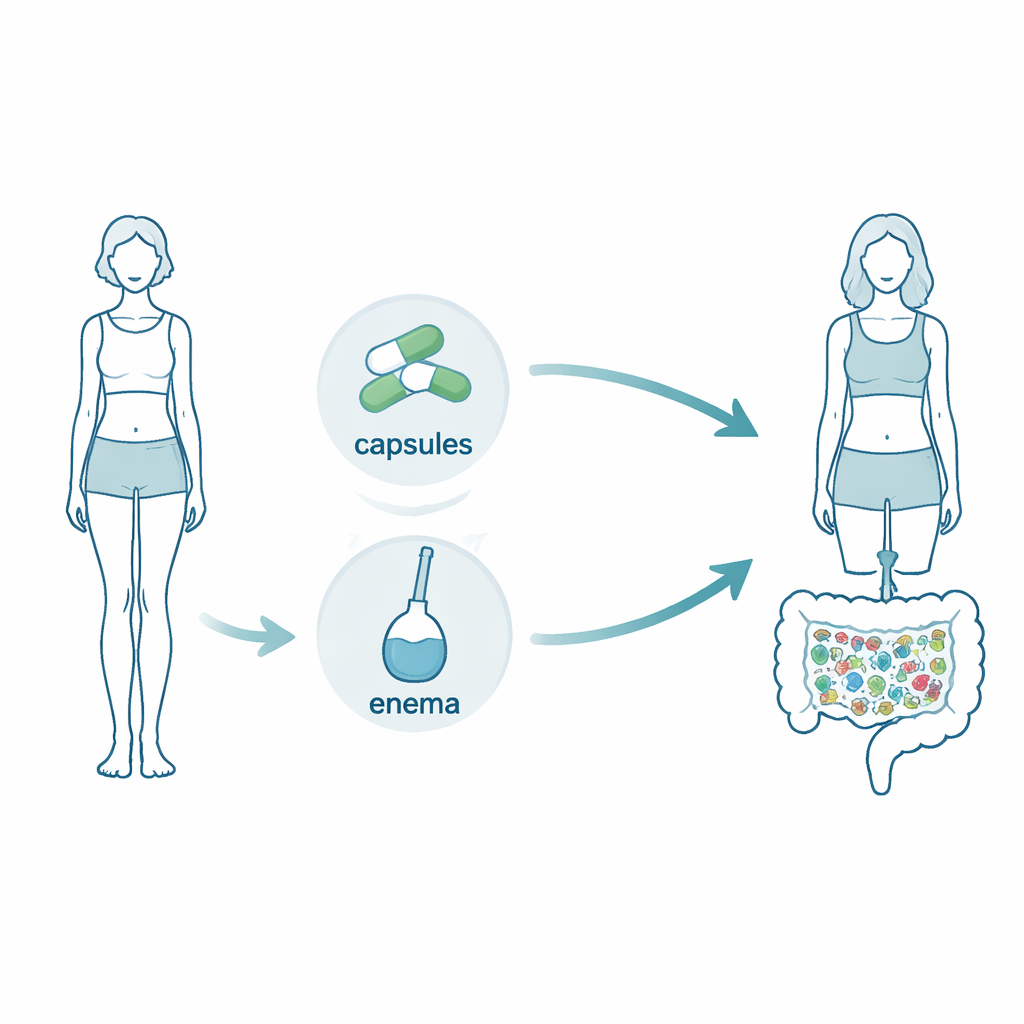
How the Study Was Carried Out
The researchers enrolled 22 adult women with anorexia nervosa being treated at specialized centers in Denmark; 18 completed all procedures. Each chose how to receive a single FMT: most (19) selected frozen capsules taken by mouth, while only three chose a rectal enema. Stool and blood samples were collected before FMT and again one week later. Using advanced DNA sequencing, the team mapped which bacterial species were present in the gut. They also measured hormones related to appetite and sex (such as insulin, peptide YY, and estradiol), and asked participants about their stool consistency using the Bristol Stool Form Scale, a standard way to estimate how quickly food moves through the gut.
Shifting the Gut’s Ecosystem
Within a week, the gut ecosystems of most participants clearly shifted toward the profiles of their healthy donors. Statistical measures of similarity showed that, for nearly all women, their post‑FMT microbiome became measurably closer to that of the donor, and this shift was specific to the donor they actually received. Several bacterial groups common in donors appeared or increased in recipients, suggesting that at least some species successfully took hold. Women who received FMT by enema were less likely to show strong donor‑like shifts than those taking capsules, hinting that the oral route may work better in this context. Despite these microbial changes, overall diversity and the broad metabolic pathways encoded in the microbes changed only modestly over the short, one‑week window.
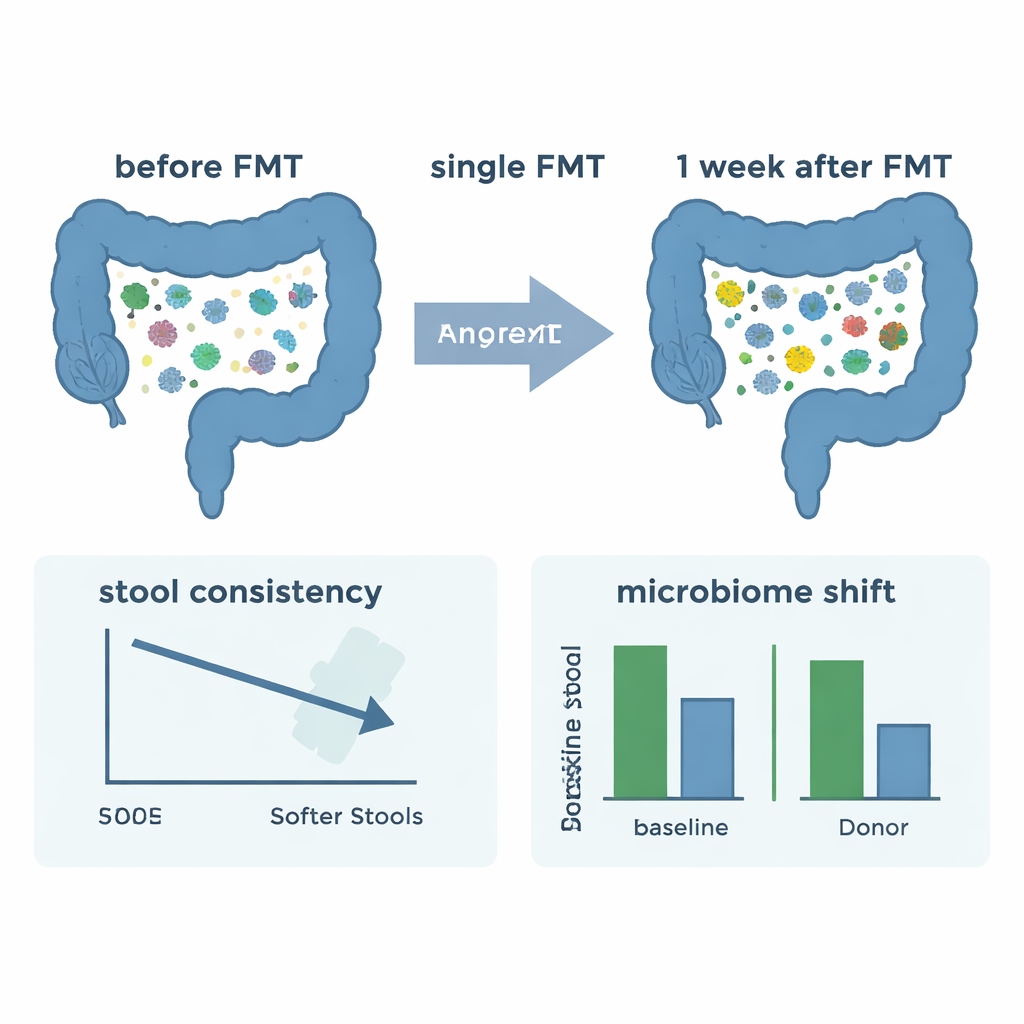
Changes in Digestion and Body Signals
Beyond the microscopic world of bacteria, the team looked for early effects on digestion and body chemistry. Many participants reported looser stools after FMT, consistent with a faster gut transit time and an easing of constipation, a frequent problem in anorexia. Objective measurements of water content in the stool supported their self‑reports, although average moisture levels did not shift dramatically. In blood, most appetite‑related and sex‑hormone markers showed no clear or consistent change one week after treatment. There was a small rise in insulin and a slight increase in one appetite hormone (peptide YY) for some women, but these signals were weak and of uncertain clinical importance. A gut‑derived enzyme involved in processing estrogen did not show meaningful change either.
What This Means—and What It Does Not
This pilot study shows that a single FMT given as frozen capsules is acceptable, logistically manageable, and appears safe in adult women with anorexia nervosa, at least in the short term. It can rapidly nudge their gut bacteria toward a healthier donor‑like pattern and may improve stool consistency, which could ease some digestive discomfort. However, it did not, in this brief window, alter mood, eating‑disorder symptoms, or key hormones in a way that suggests immediate clinical benefit. For lay readers, the takeaway is that the gut microbiome is a promising but still experimental target in anorexia. Larger, carefully controlled trials with repeated treatments and longer follow‑up will be needed to find out whether reshaping gut bacteria can meaningfully support weight restoration, hormonal balance, and mental health in this complex disorder.
Citation: Panah, F.M., Støving, R.K., Sjögren, M. et al. Impact of a single fecal microbiome transplantation in adult women with anorexia nervosa: an open-label feasibility pilot trial. Nat Commun 17, 1747 (2026). https://doi.org/10.1038/s41467-026-68455-8
Keywords: anorexia nervosa, gut microbiome, fecal microbiota transplantation, digestive health, mental health research