Clear Sky Science · en
Aged skin exacerbates experimental osteoarthritis via enhanced IL-36R signaling
Why Your Skin Might Matter to Your Aching Joints
Osteoarthritis is often blamed on years of wear and tear in our joints. But this research suggests an unexpected culprit joins the story: our aging skin. The study reveals that changes in the outermost skin cells can send inflammatory signals through the bloodstream that quietly worsen joint damage and pain. Understanding this skin–joint connection could open the door to new, less invasive treatments for osteoarthritis using simple skin patches instead of repeated joint injections or major surgery.
From "Wear and Tear" to Slow-Burning Inflammation
Osteoarthritis is the most common joint disease in older adults, causing stiffness, pain, and loss of movement. Traditionally, it has been seen as a purely mechanical problem—cartilage slowly grinding down over time. In recent years, however, scientists have realized that low-level, chronic inflammation also drives the disease. This paper explores where some of that inflammation comes from. The authors focused on the skin, our largest organ and first line of defense against the outside world, which becomes thinner, more fragile, and more inflamed as we age.
How Aged Skin Sends Distress Signals to the Joints
The team discovered that a specific family of immune messengers, called IL-36 cytokines, acts as a bridge between aged skin and arthritic joints. In healthy skin, special cells known as keratinocytes produce both IL-36 "agonists" (which switch inflammation on) and a natural brake called IL-36 receptor antagonist (IL-36Ra), which keeps the response in check. In mouse models of prematurely aged skin, naturally old mice, and older human patients, this balance was lost: IL-36Ra levels in the skin dropped, while the IL-36 agonists rose in the skin, in the bloodstream, and inside the joints. These signals activated inflammatory pathways in cartilage cells and synovial fibroblasts (the cells that line the joint), making them age faster, break down tissue, and release more inflammatory factors.
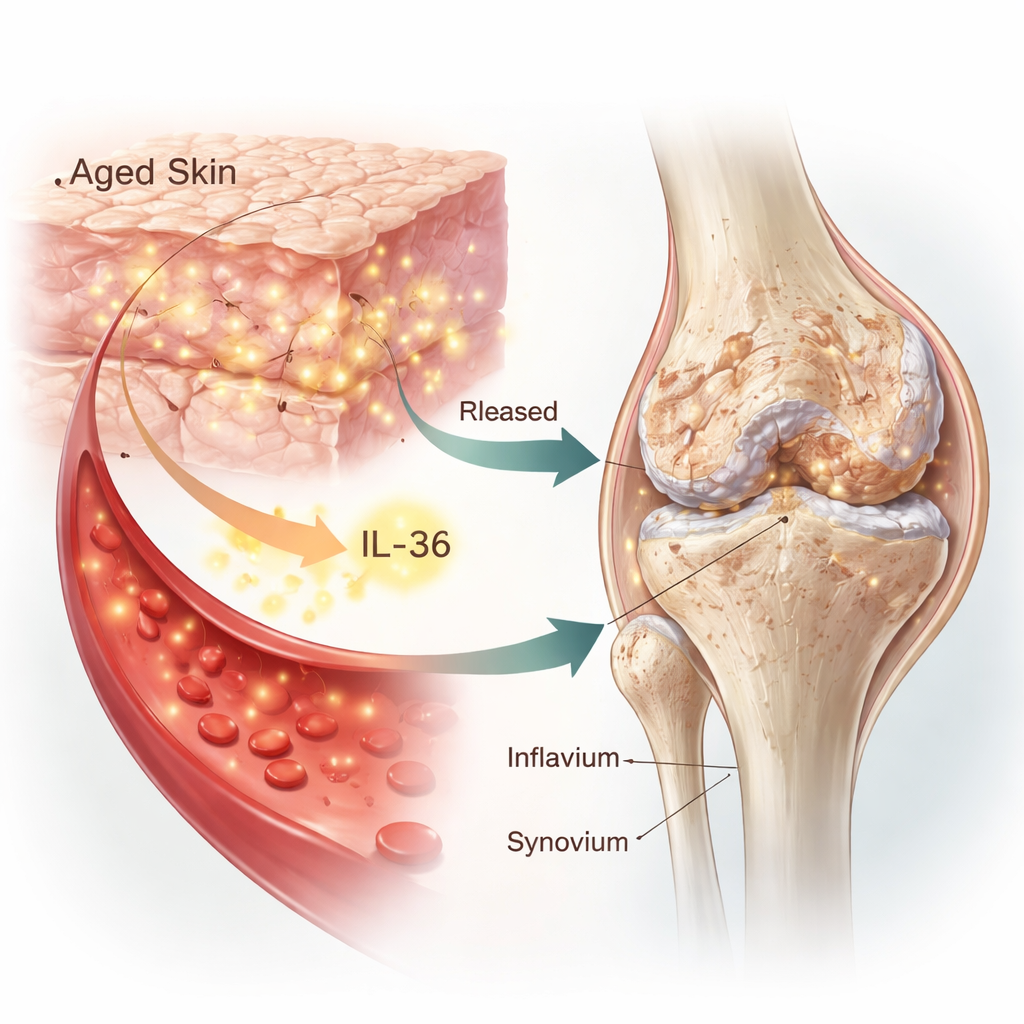
Proof That Skin-Driven Signals Worsen Osteoarthritis
To test whether aged skin truly drives joint damage, the researchers combined skin-aging tricks with a standard knee injury model of osteoarthritis in mice. When mice had chemically aged or genetically aged skin, their injured knees developed more severe cartilage erosion, more bone changes, more joint lining inflammation, and more pain-like behavior. Remarkably, if the aged skin was surgically removed, or if joint cells were protected by blocking IL-36 signaling inside the joint, osteoarthritis progressed much more slowly. Mice engineered to lack the IL-36Ra brake only in their skin cells showed the same pattern: more IL-36 in the blood and joints, stronger inflammatory signaling, and worse experimental and age-related osteoarthritis.
Turning Off the Harmful Signal with Microneedle Patches
Because frequent injections into painful joints are unpleasant and hard to maintain, the team looked for a gentler way to calm IL-36 signaling at its source—the skin. They created tiny dissolving microneedle patches loaded with either mouse IL-36Ra protein or spesolimab, a drug that blocks the IL-36 receptor and is already approved for a rare inflammatory skin disease. These microneedles painlessly pierced the outer skin layer and slowly released the blocker into the keratinocytes over days. In mice with aged skin and osteoarthritis, applying these patches to the back reduced IL-36 agonists in the skin and blood, quieted inflammatory pathways in the joints, preserved cartilage structure, eased joint lining inflammation, and reduced pain responses. Similar protective effects were seen when spesolimab was tested on human cartilage samples and joint-lining cells in the lab.
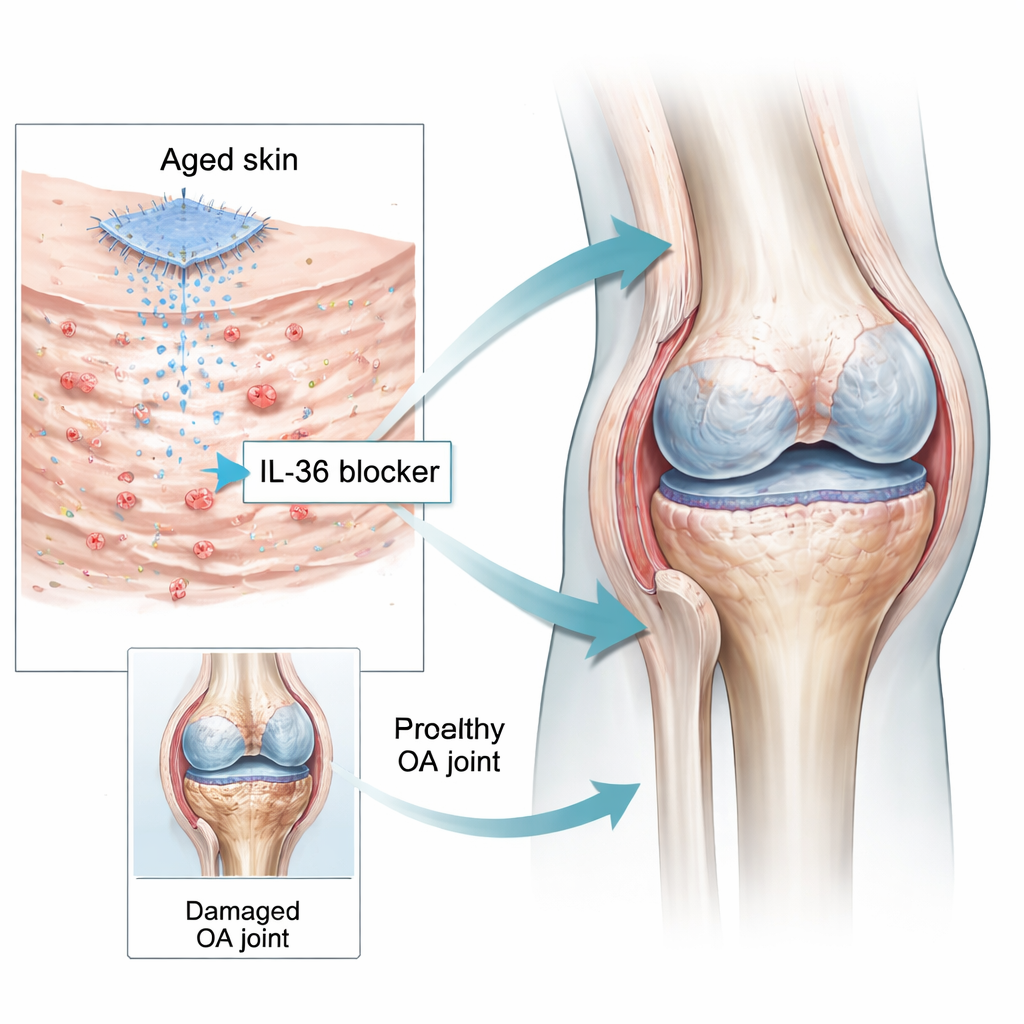
What This Could Mean for People with Aching Joints
The study reshapes how we think about osteoarthritis by showing that "inflamm-aging" of the skin can feed harmful signals to the joints through the bloodstream. When the natural IL-36 brake in aging keratinocytes weakens, IL-36 agonists leak into circulation, push joint cells into a destructive, senescent state, and accelerate cartilage loss and pain. By blocking this signal—either directly in the joint or, more promisingly, through drug-loaded microneedle patches on the skin—it may be possible to slow the disease rather than just masking symptoms. While more work in larger animals and human trials is needed, these findings hint that future osteoarthritis treatments might look less like surgery or injections, and more like applying a medicated patch to the skin.
Citation: Chen, D., Wang, C., Yang, C. et al. Aged skin exacerbates experimental osteoarthritis via enhanced IL-36R signaling. Nat Commun 17, 1695 (2026). https://doi.org/10.1038/s41467-026-68399-z
Keywords: osteoarthritis, skin aging, inflammation, IL-36 signaling, microneedle therapy