Clear Sky Science · en
Versican expression from lung fibroblasts suppresses pulmonary fibrosis
Why lung scarring needs a better brake
Idiopathic pulmonary fibrosis is a relentless lung disease in which normal healing turns into runaway scarring, slowly robbing people of their breath. This study uncovers a surprising natural “braking system” inside the lungs: a large sugar‑coated molecule called versican, made by connective‑tissue cells known as fibroblasts. Rather than driving damage, fibroblast‑derived versican helps keep scar formation in check, reshaping how we think about scarring and hinting at new treatment strategies for this otherwise untreatable disease.
A deadly repair job gone wrong
In healthy lungs, a delicate mesh of proteins and sugars—called the extracellular matrix—supports tiny air sacs where oxygen exchange happens. After injury, fibroblasts rush in, lay down fresh matrix, and then quiet down again. In idiopathic pulmonary fibrosis, this repair program never properly switches off. Fibroblasts pile up, weave dense collagen scaffolds, and stiffen the lung tissue so that breathing feels like inflating a rubber ball filled with cement. The authors set out to understand how one particular matrix component, versican, fits into this story, because it is abundant in diseased lungs but its role has been puzzling.
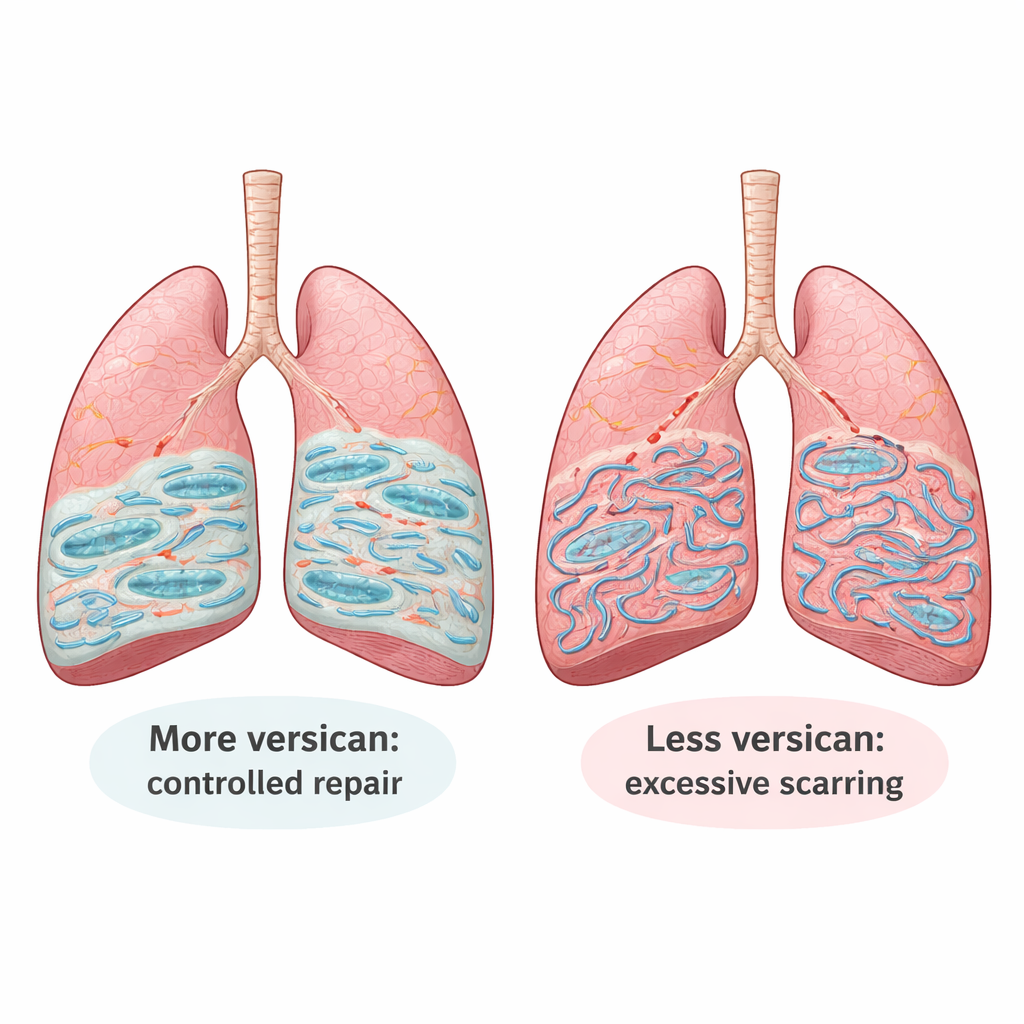
A protective coat around lung cells
By mining large gene databases from patients and examining lung biopsies, the researchers found that versican levels are consistently higher in fibrotic lungs and are especially elevated in fibroblasts and certain immune cells. In a widely used mouse model of lung fibrosis, they saw the same pattern: after injury, versican production surged when scarring peaked and then declined as the lungs began to recover. In dishes, normal lung fibroblasts exposed to a strong scarring signal (the growth factor TGF‑β) or grown on a pre‑scarred matrix responded by boosting versican production, suggesting that versican is part of the lung’s built‑in response to a stiff, collagen‑rich environment.
When the brake is weakened, scarring worsens
To test whether versican is friend or foe, the team used mice that make only about half the normal amount of versican. Counter to what its high levels in disease might suggest, these “versican‑light” mice did worse after lung injury. They lost more weight, accumulated more fluid and soluble collagen in the air spaces, and developed thicker, stiffer lungs that took longer to recover. Detailed imaging showed heavier collagen deposits and a more distorted tissue structure. Measurements of lung slices with atomic force microscopy confirmed that the scarred tissue in these mice was mechanically stiffer, a key driver of ongoing fibroblast activation.
How a loosened matrix becomes a freeway for invasion
Diving deeper, the scientists looked at how versican shapes the lung’s physical scaffolding. In cell‑free tests, adding versican slowed collagen fibers from packing tightly together, while reducing versican let collagen assemble into thicker, more intertwined bundles. In living tissue and in matrix made by fibroblasts in the lab, lower versican meant not only more and thicker collagen, but also more of other matrix players like tenascin‑C and hyaluronan, and more cross‑links that lock fibers into rigid networks. Fibroblasts sitting on this altered matrix switched into a highly invasive mode, forming many small, enzyme‑rich “podosomes” that chew through the surrounding material and allow cells to burrow deeper. Blocking key receptors for collagen and tenascin‑C reduced this invasive behavior, tying the structural changes directly to cell actions.
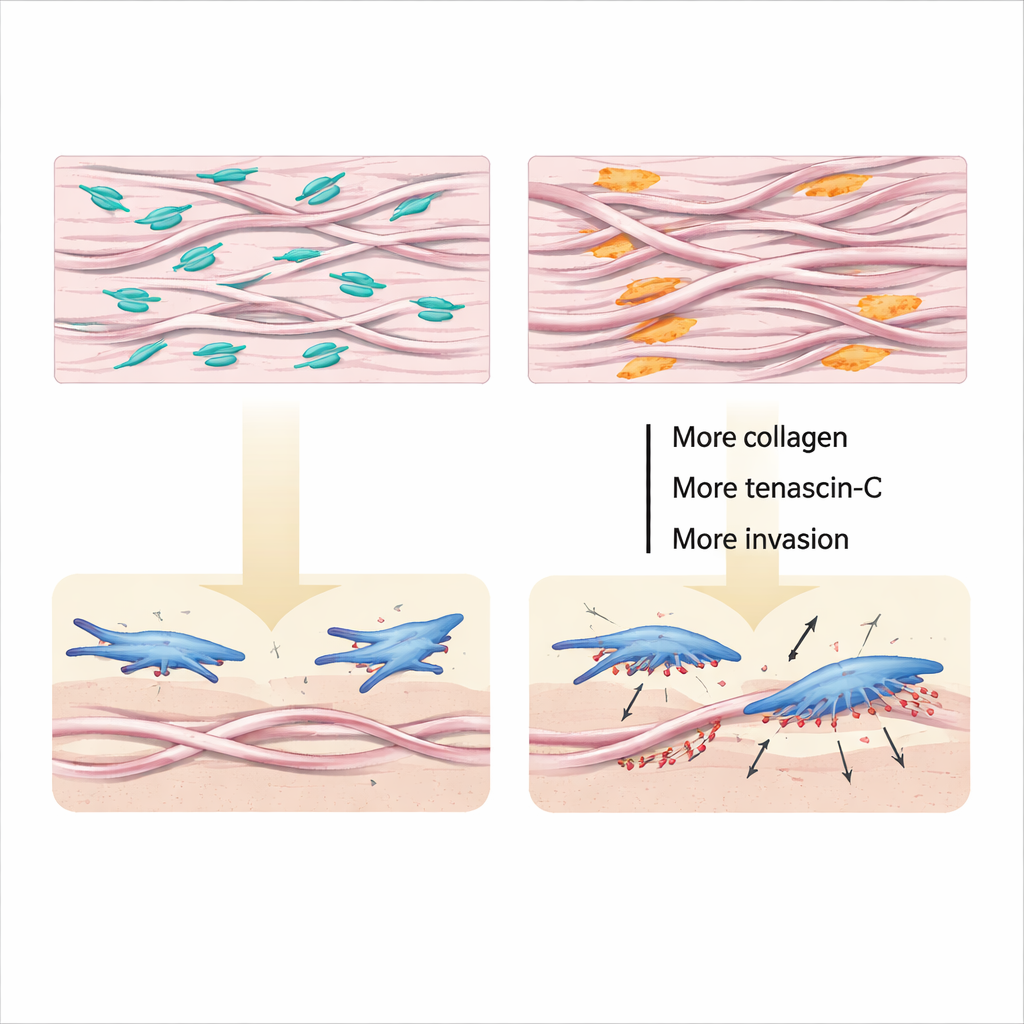
A double‑edged molecule with promise
From these experiments, a clear picture emerges: versican made by lung fibroblasts acts as an internal limiter on scarring. When injury and growth factors push collagen production up, fibroblasts respond by raising versican, which keeps collagen fibers from becoming too thick and tangled, dampens excessive stiffening, and restrains the formation of invasive podosomes. If versican levels fall, collagen and tenascin‑C surge, the matrix stiffens and knots, fibroblasts invade more aggressively, and fibrosis both worsens and lingers. Because other cells, such as immune cells, may use versican differently, it remains a “double‑edged sword,” but this work shows that carefully boosting or mimicking the fibroblast side of versican’s action could be a powerful new way to slow or even reverse lung scarring.
Citation: Kanellopoulou, P., Barbayianni, I., Fanidis, D. et al. Versican expression from lung fibroblasts suppresses pulmonary fibrosis. Nat Commun 17, 1676 (2026). https://doi.org/10.1038/s41467-026-68377-5
Keywords: idiopathic pulmonary fibrosis, extracellular matrix, versican, lung fibroblasts, tissue scarring