Clear Sky Science · en
Machine learning-predicted insulin resistance is a risk factor for 12 types of cancer
Why this research matters to everyday health
Most people have heard that excess weight and type 2 diabetes can raise the chance of getting cancer, but the hidden link between them—how well the body responds to insulin—is rarely measured in routine checkups. This study shows that a computer‑generated score of “insulin resistance,” built only from common blood tests and basic health data, can flag people at higher risk not only for diabetes and heart problems, but also for several major cancers. It suggests that information doctors already collect could be combined in smarter ways to identify high‑risk individuals earlier and to guide more targeted screening.
A digital fingerprint of insulin resistance
Insulin is a hormone that helps sugar move from the blood into organs such as muscle, liver, and fat tissue. When these tissues stop responding properly—called insulin resistance—the body compensates by making more insulin, which over time can lead to type 2 diabetes and heart disease. The gold‑standard lab test for insulin resistance is complex, time‑consuming, and unsuitable for large numbers of people. Even simpler research measures require fasting insulin levels, which are not usually checked in everyday practice. To get around this barrier, the researchers had previously trained a machine‑learning model to predict whether a person is insulin‑resistant based on nine routine measures: age, sex, race, body mass index (BMI), fasting blood sugar, long‑term blood sugar (HbA1c), triglycerides, total cholesterol, and “good” HDL cholesterol. The resulting score is called artificial‑intelligence‑derived insulin resistance, or AI‑IR.
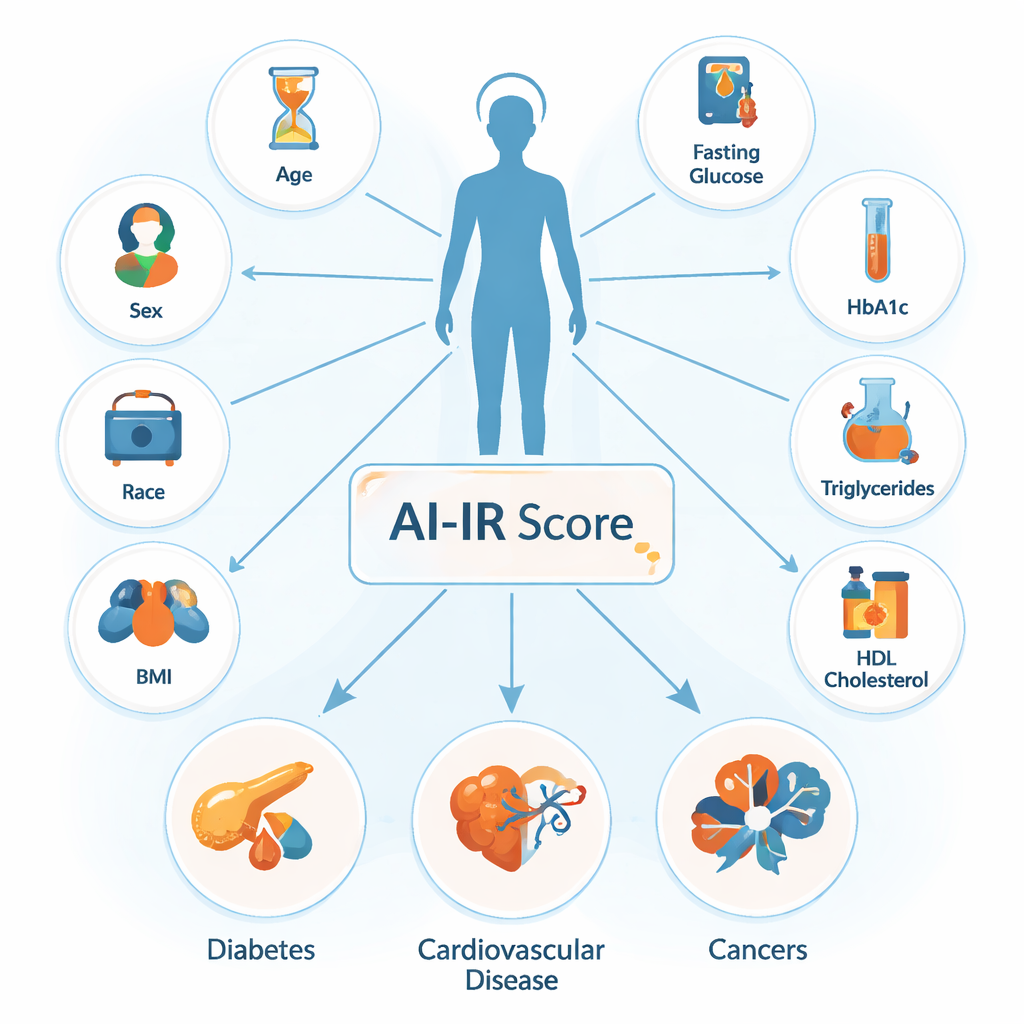
Testing the score in hundreds of thousands of people
In this new work, the team applied AI‑IR to data from more than 370,000 participants in the UK Biobank, a long‑running health study of adults aged 40 to 69. First, they asked whether the score could predict who would go on to develop diabetes, heart problems, or die during follow‑up. People without diabetes who tested positive for AI‑IR were about seven times more likely to develop diabetes than those who were AI‑IR‑negative, even after accounting for age and sex. They were also more likely to be admitted to hospital with diabetes, to experience major heart and blood‑vessel events, and to die from cardiovascular causes or from any cause. When directly compared with simpler measures such as BMI, metabolic syndrome, and two blood‑fat‑based indices, AI‑IR gave the most accurate forecasts of future diabetes.
Connecting insulin resistance to cancer
The researchers then focused on cancer. Among participants who had no history of cancer at the start, they tracked who developed different types of tumors over time, using linked National Health Service records. Looking at all cancers combined, AI‑IR did not change overall risk. However, when they broke cancers down by site, a clearer pattern emerged. People without diabetes but with a positive AI‑IR score had higher risks of cancers of the uterus, kidney, esophagus, pancreas, colon, and breast. They also showed suggestive increases for cancers of the renal pelvis, small intestine, stomach, liver and gallbladder, leukemia, and cancers of the bronchus and lung. At the same time, they were less likely to develop skin cancer. When these cancer types with elevated risk were grouped together into a “composite” outcome, AI‑IR‑positive individuals had about a 25% higher risk than AI‑IR‑negative peers of the same age and sex, a difference that persisted, though somewhat reduced, even after adjusting for BMI.
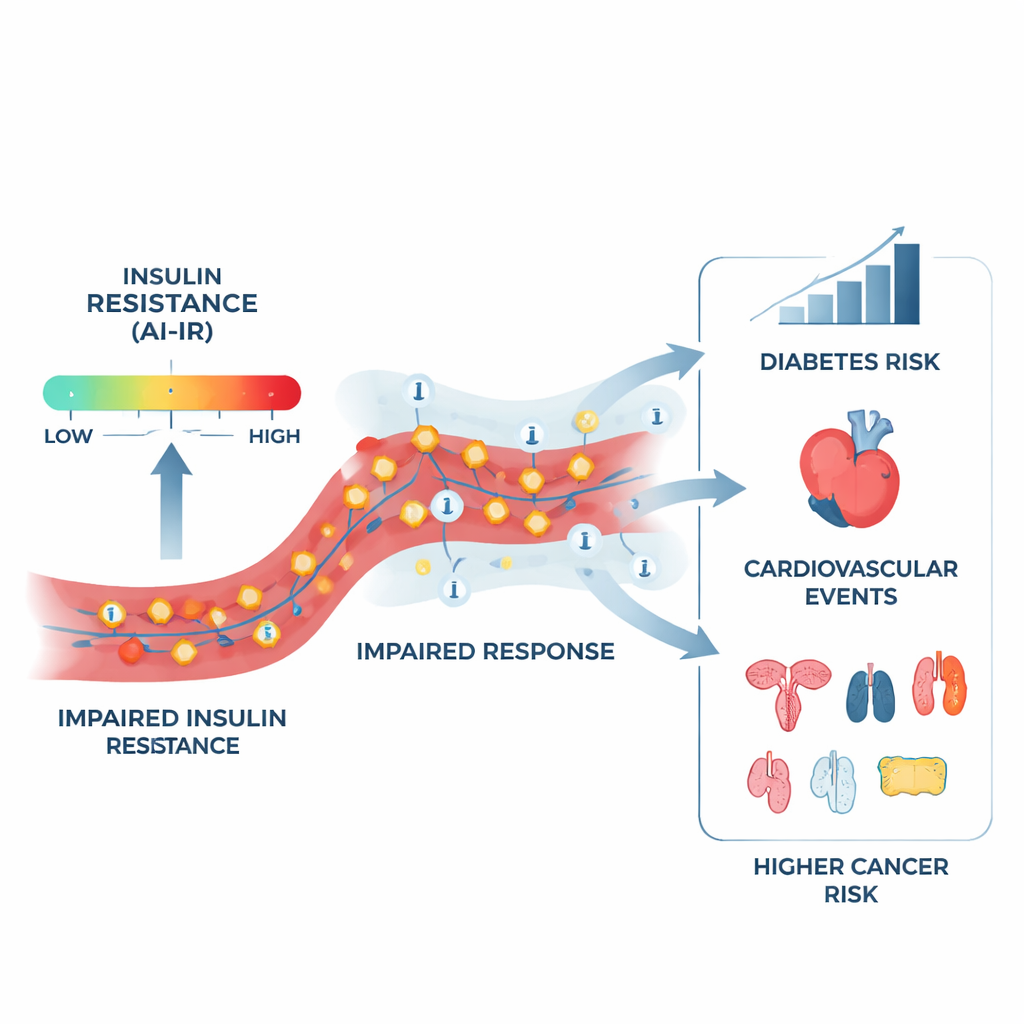
Weight‑related and weight‑independent effects
Because body weight strongly influences insulin resistance, the team explored whether AI‑IR was simply acting as a stand‑in for obesity. They found that some of the increased cancer risks—such as for stomach, liver and gallbladder, pancreas, colon, leukemia, and breast cancer—largely overlapped with the effect of BMI. But others appeared to reflect something more specific about insulin resistance itself. Notably, the link between AI‑IR and lung and bronchial cancer became even stronger after adjusting for BMI, and remained significant even when smoking status was taken into account. Former smokers with a positive AI‑IR score were at especially high risk of lung‑related cancers and of the broader group of insulin‑resistance‑linked cancers. Overall, AI‑IR provided better cancer risk stratification than BMI and another blood‑fat index, and performance similar to that of metabolic syndrome and a triglyceride‑to‑HDL ratio, while still being the best tool for predicting diabetes.
What this means for patients and doctors
The study suggests that a “digital biomarker” of insulin resistance, calculated from information already collected in most clinics, can spotlight people at increased risk for both diabetes and a cluster of cancers. While AI‑IR is not yet a screening test on its own, it could help clinicians decide who might benefit from more frequent blood‑sugar checks, more aggressive lifestyle or medication strategies, and earlier or more focused cancer screening, particularly for organs such as the uterus, kidney, colon, lung, breast, and pancreas. The work also highlights insulin resistance as a biological pathway that links excess weight, abnormal blood fats, and chronic inflammation to cancer, encouraging future research on how improving insulin sensitivity—through diet, exercise, or drugs—might lower cancer risk as well as prevent diabetes.
Citation: Lee, CL., Yamada, T., Liu, WJ. et al. Machine learning-predicted insulin resistance is a risk factor for 12 types of cancer. Nat Commun 17, 1396 (2026). https://doi.org/10.1038/s41467-026-68355-x
Keywords: insulin resistance, machine learning, diabetes risk, cancer risk, UK Biobank