Clear Sky Science · en
Robust water-activated tissue adhesive patch for arterial/heart wound closure after intervention surgery
Stopping Dangerous Bleeding in Seconds
When surgeons repair the heart or major arteries, they must seal the holes left by their instruments before the patient bleeds out. Existing closure devices often struggle with large punctures or hardened, diseased vessels, and can sometimes fail at the worst possible moment. This study introduces a new kind of patch that uses water—not glue guns, sutures, or complex devices—to instantly turn into a strong, tissue-gripping seal that can stop even high‑pressure arterial or heart bleeding within seconds.
Why Closing Surgical Holes Is So Hard
Modern heart and blood vessel procedures are increasingly done through tiny access points in the wrist, groin, or even the tip of the heart. But as catheters and valves get larger, the holes they leave behind become harder to close. Current devices often rely on sutures that must be threaded through fragile vessel walls, or on plugs that sit partly inside the blood vessel, raising the risk of clots and blocked blood flow. These systems can fail when the hole is big, the blood pressure is high, or the vessel wall is stiff and calcified. Surgeons therefore need a closure method that works quickly on wet, moving tissue, without leaving hardware inside the bloodstream.
A Patch That Turns Blood Into a Trigger
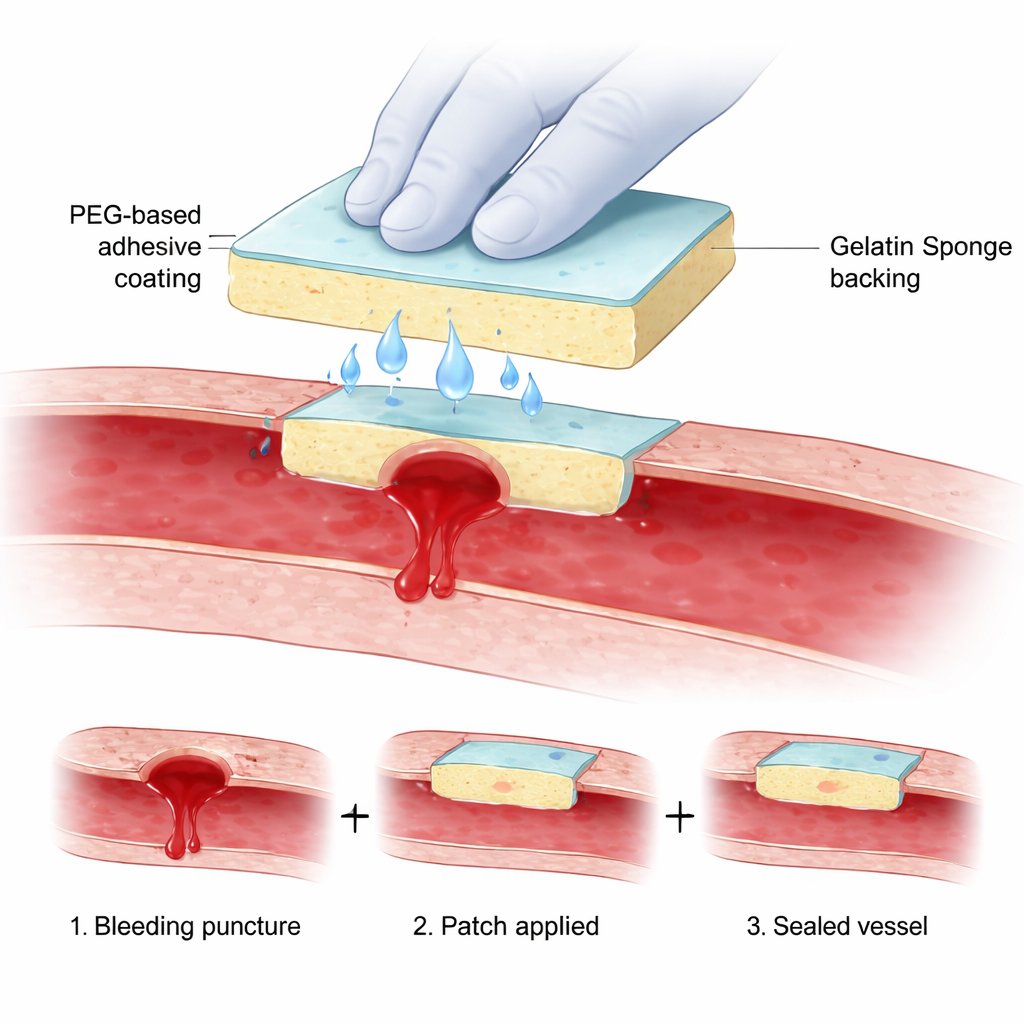
The researchers designed a water‑activated tissue adhesive patch, or WAP, that looks like a soft sponge coated with a thin, invisible layer of special polymer. The backing is a familiar medical gelatin sponge, while the coating is made from medical‑grade polyethylene glycol (PEG) derivatives and a small redox catalyst pair. As soon as the patch touches a bleeding surface, water in the blood dissolves the coating into a thick liquid that soaks up fluid and temporarily pushes blood away from the tissue. Within seconds, the dissolved PEG molecules react with each other and with natural groups on the tissue surface, locking into a solid gel that interlocks with the outer layer of the vessel or heart. The result is a firmly anchored hydrogel skin that seals the hole and is supported by the sponge behind it.
Building Strong, Fast, and Safe Adhesion
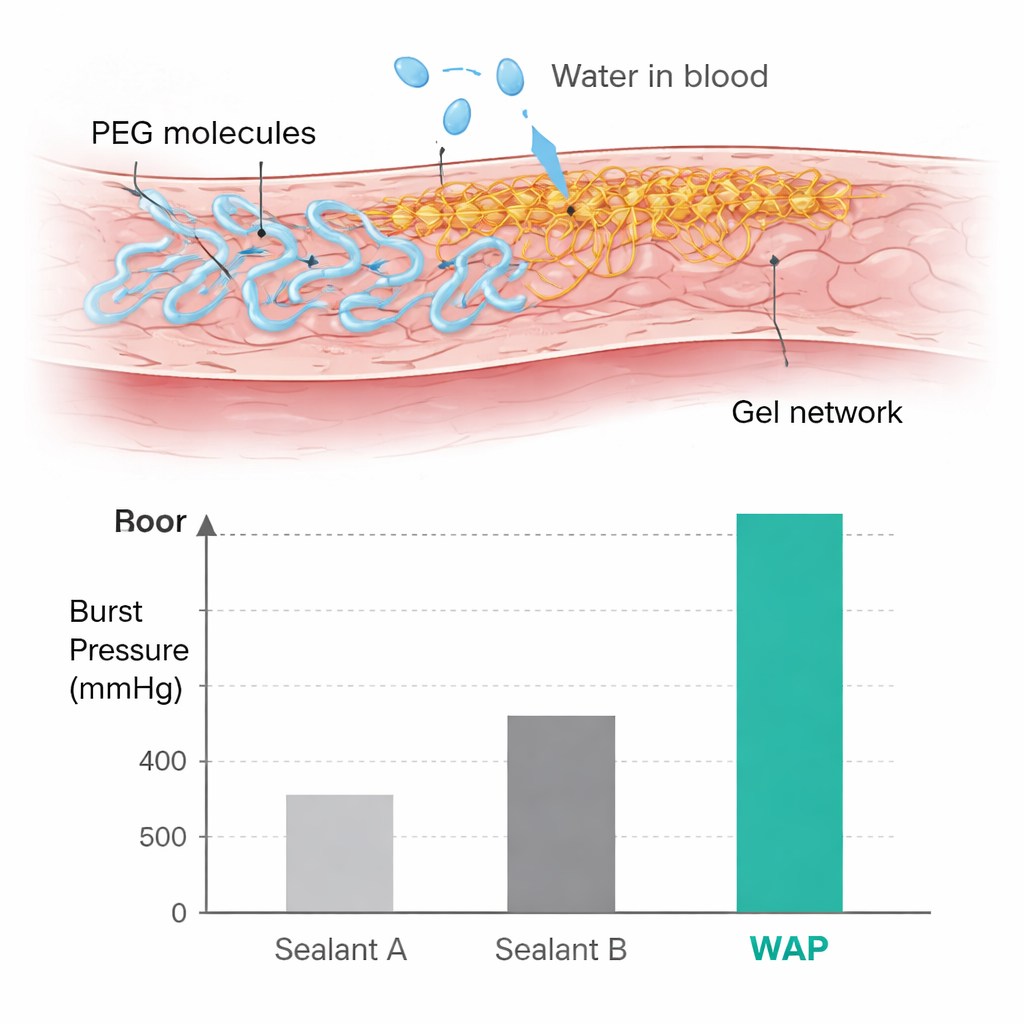
To make this concept practical, the team had to balance speed, strength, and safety. They tuned the lengths and shapes of the PEG molecules and the amount of catalyst so the coating would melt and set in under about 10 seconds, even in flowing blood. Mechanical tests showed that the optimized formulation sticks strongly to many different organs, including stomach, skin, heart, liver, and lung, and outperforms several commercial surgical glues on wet surfaces. When combined with the gelatin sponge, the patch withstood pressures above 300 mmHg—much higher than normal or even severely high blood pressure—indicating that it can reliably seal major arteries. Laboratory studies on cells and subcutaneous implants in rats showed that the material is not toxic, gradually swells, and then slowly breaks down over months without triggering harmful long‑term inflammation.
From Lab Bench to Beating Hearts
The patch was then tested in realistic animal models of life‑threatening bleeding. In rabbits, it rapidly stopped severe femoral artery bleeding even when the exact source of the leak was hidden inside pooled blood, a situation similar to traumatic injuries. In pigs, the team sealed stab wounds in the beating heart and large punctures made by 14F and 20F catheter sheaths in major arteries. In these tests, pressing the patch for roughly half a minute to a minute was enough to halt blood loss completely. Follow‑up imaging and tissue analysis over weeks showed that the arteries and heart walls healed with normal structure, without clots, pseudoaneurysms, or signs of heart failure. Blood flow through treated vessels remained smooth, and the material gradually integrated and degraded as healing progressed.
What This Could Mean for Future Patients
For patients, this technology could make complex heart and vascular procedures safer and faster by turning a dangerous, high‑pressure leak into a quick patch‑and‑press maneuver. Because the patch works on wet, moving tissue and does not leave rigid components inside the vessel, it may be suitable for large punctures, diseased arteries, and transapical heart access where current devices struggle. With an appropriate delivery tool, the water‑activated patch has the potential to become an off‑the‑shelf closure option that emergency teams and interventional surgeons can use to rapidly seal life‑threatening arterial and heart wounds, buying crucial time for recovery and further care.
Citation: Huang, Y., Zhu, Q., Gu, Y. et al. Robust water-activated tissue adhesive patch for arterial/heart wound closure after intervention surgery. Nat Commun 17, 1625 (2026). https://doi.org/10.1038/s41467-026-68338-y
Keywords: tissue adhesive patch, arterial wound closure, hemostasis, interventional cardiology, PEG hydrogel