Clear Sky Science · en
Mutant KRAS vaccine with dual checkpoint blockade in resected pancreatic cancer: a phase I trial
New Hopes Against a Deadly Cancer
Pancreatic cancer is one of the most lethal cancers, largely because it spreads early and often returns even after surgery and chemotherapy. This study explores a new kind of “training program” for the immune system: a vaccine built to recognize common mutations in a cancer-driving gene called KRAS, combined with two modern immunotherapy drugs. For people who have already had their pancreatic tumors removed, this approach aims to wipe out invisible cancer seeds before they grow back.
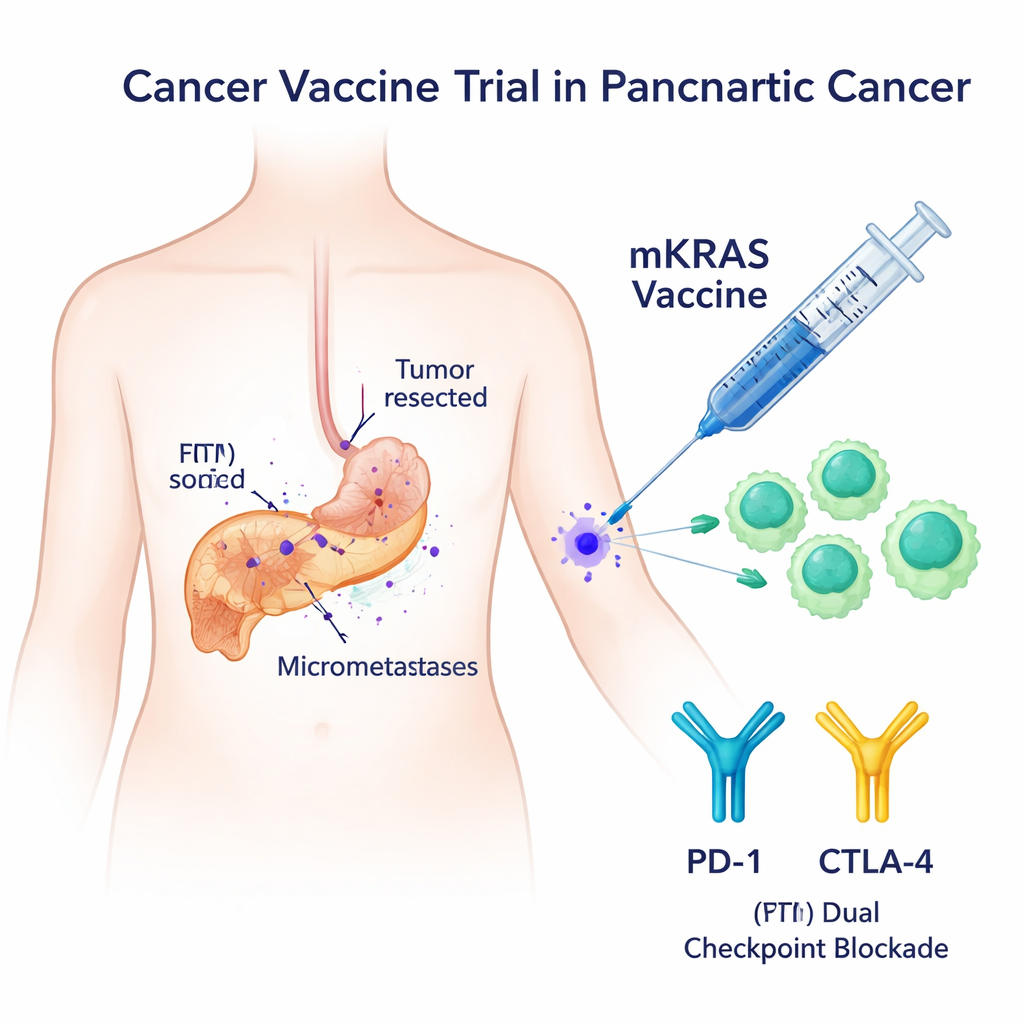
A Sharp Target: Mutant KRAS
Most pancreatic tumors carry changes in the KRAS gene that act like a stuck gas pedal for cell growth. These mutant versions—such as G12V, G12D, G12R, G12C, G12A, and G13D—are almost never found in healthy tissue, making them highly attractive bullseyes for the immune system. Earlier attempts at KRAS-targeted vaccines showed only modest immune responses and generally focused on one or two mutations. In this phase I trial, researchers tested a broader vaccine, called mKRAS-VAX, that combines six long peptide fragments representing the most common KRAS mutations and pairs them with two “checkpoint” drugs, nivolumab and ipilimumab, that help unleash T cells that might otherwise be held back.
Designing and Delivering the Vaccine Strategy
The trial enrolled 12 people whose pancreatic tumors had been surgically removed and who had finished standard chemotherapy, but who still faced a high risk of relapse. Each participant’s tumor carried one of the six KRAS mutations included in the vaccine. During an initial “prime” phase, patients received four rounds of the peptide cocktail mixed with an immune-stimulating adjuvant, alongside the two checkpoint drugs. This was followed by booster doses, and some patients who remained cancer-free after a year continued with vaccine boosters alone. The main questions were whether this combination would be safe and whether it would noticeably boost KRAS-targeted T cells in the blood.
Training and Tracking Immune Cells
Blood samples taken before and after vaccination were exposed to each KRAS peptide to see how many T cells produced interferon-gamma, a key messenger of immune activity. The results were striking for a small study: 11 of 12 patients showed a significant increase in T cells that recognized the mutant KRAS peptides overall, and 10 of 12 mounted a strong response against their own tumor’s specific KRAS mutation. Many patients responded to several of the six KRAS variants, and some T cells could recognize more than one mutation, suggesting a degree of helpful cross-reactivity. Detailed profiling showed that most of these vaccine-induced cells were “helper” CD4 T cells with memory features, backed by a smaller but important group of cytotoxic CD8 T cells capable of killing. The team also mapped and cloned hundreds of KRAS-specific T cell receptors, including some “public” receptors shared across different patients, which could be valuable for future cell-based therapies.
Early Clinical Signals and Mutation-by-Mutation Differences
While the study was not large enough to prove a survival benefit, there were encouraging hints. Patients whose KRAS-targeted T cell responses ranked in the top three-quarters tended to stay free of detectable cancer longer than those with weaker responses. After roughly three years of follow-up, a third of participants remained disease-free. All four patients who were still cancer-free at the latest check carried KRAS G12V or G12R tumors, and their KRAS-specific T cells persisted for more than a year, particularly the memory-type CD4 cells. By contrast, tumors with the G12D mutation not only responded less strongly at the immune level but were more likely to recur, echoing other studies linking G12D to more aggressive disease. Importantly, vaccine-related side effects were mild (mostly soreness, fatigue, and fever), and more serious immune complications came from the checkpoint drugs rather than the vaccine itself.
What This Could Mean for Future Patients
In plain terms, this trial shows that an “off-the-shelf” vaccine aimed at multiple mutant KRAS targets, when combined with modern checkpoint drugs, can safely awaken a broad and lasting T cell response in most people with high-risk pancreatic cancer. Although many patients still saw their disease return, those with stronger KRAS-focused immune responses tended to do better, hinting that boosting these responses further—or starting vaccination earlier—might improve outcomes. The rich catalog of KRAS-specific T cell receptors uncovered here also opens the door to engineered T cell therapies. Together, these findings suggest that turning KRAS from a notorious cancer driver into a recognizable flag for the immune system may become a key strategy in preventing pancreatic cancer from coming back.
Citation: Huff, A.L., Haldar, S.D., Gergis, A.A. et al. Mutant KRAS vaccine with dual checkpoint blockade in resected pancreatic cancer: a phase I trial. Nat Commun 17, 1538 (2026). https://doi.org/10.1038/s41467-026-68324-4
Keywords: pancreatic cancer vaccine, mutant KRAS, immunotherapy, T cell response, checkpoint blockade