Clear Sky Science · en
Population frequencies of thiopurine-related pharmacogenes in healthy individuals from Kosovo
Why Our Genes Matter for Common Medicines
Many people take medicines that work well for some but cause serious side effects in others. This study looks at how small differences in DNA among healthy adults in Kosovo may change the way their bodies handle a group of drugs called thiopurines. These medicines are widely used for childhood leukemia, inflammatory bowel disease, autoimmune conditions and after organ transplants. Understanding how common certain genetic variants are in one country can help doctors choose safer doses and avoid dangerous reactions before treatment even begins.
Drugs That Need a Personal Touch
Thiopurines start out as inactive substances that must be processed inside our cells before they can fight disease. Along the way, several enzymes act like tiny factory workers, switching the drug on or off or steering it toward useful or harmful byproducts. If the genes that guide these enzymes differ from person to person, the same dose of medicine can be either too weak or too strong. For thiopurines, past research has pinpointed several key genes: TPMT and NUDT15, which are already used in clinics around the world to guide dosing, and others—PACSIN2, ITPA and MTHFR—that may further shape both benefit and risk.
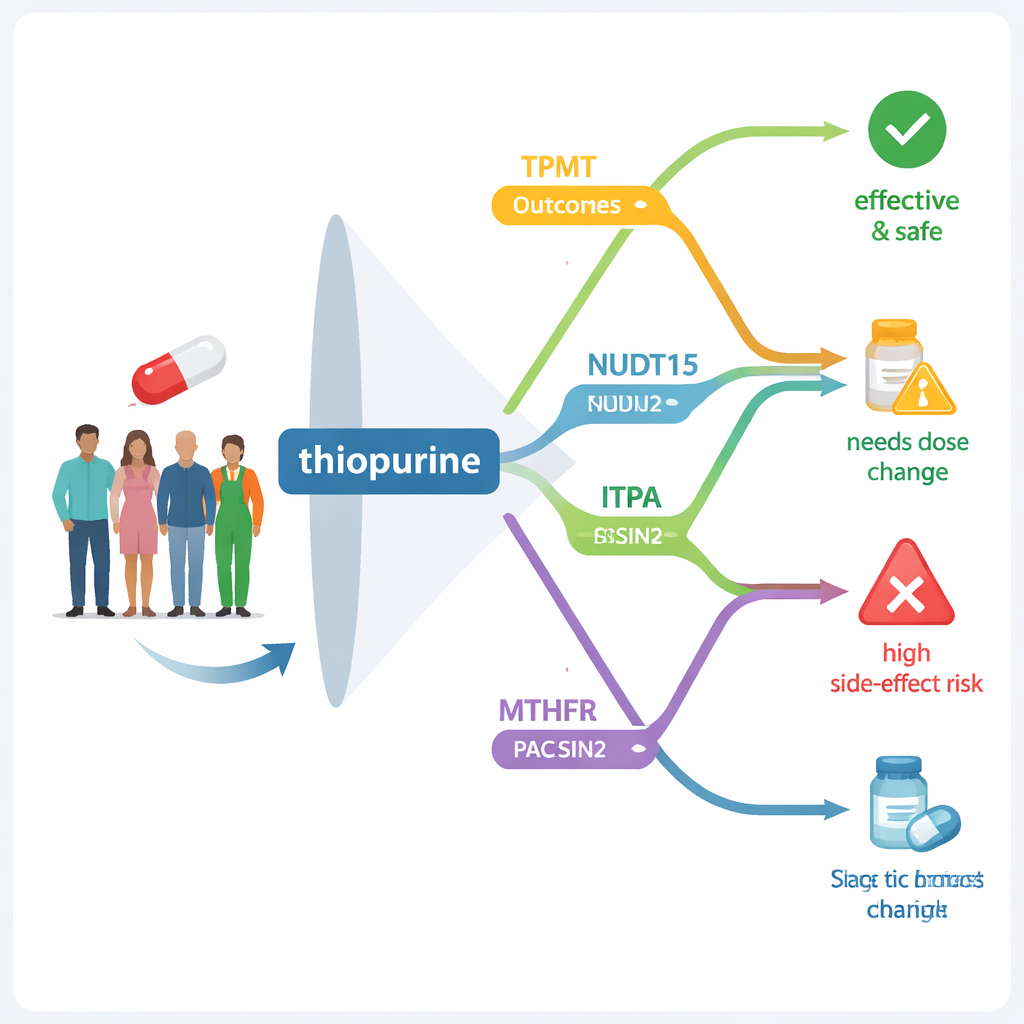
Taking the Pulse of a Nation’s DNA
To see how common these genetic differences are in Kosovo, the researchers analyzed blood samples from 299 healthy volunteer blood donors from across the country, mostly of Kosovar background. They isolated DNA and used standard laboratory tools to read selected spots in the genome where important variants are known to occur. For TPMT, PACSIN2, ITPA and MTHFR, they used targeted tests that look for specific one-letter changes in DNA. For NUDT15, they went a step further and read key stretches of the gene by sequencing, allowing them to spot several different variants at once. They then compared how often each variant occurred in Kosovo with large global and European genetic databases.
What the Gene Scan Revealed
The study found that some thiopurine-related variants are present in Kosovo at levels similar to the rest of Europe, while others stand out. The most widely recognized TPMT risk variants, which can sharply raise the chance of blood toxicity if thiopurines are given at full strength, were relatively rare in this group. Variants in NUDT15, which also affect how the drugs are broken down, appeared at modest levels comparable to other European populations. In contrast, a variant in the ITPA gene that has been linked to side effects was less common in Kosovo than in global and European averages, while a variant in PACSIN2, a gene that may influence digestive and blood-related toxicity, was somewhat more frequent. Most striking was a common change in the MTHFR gene, which plays a central role in how the body uses folate (vitamin B9). Nearly half of all MTHFR gene copies in this study carried this variant—much higher than typical European rates.
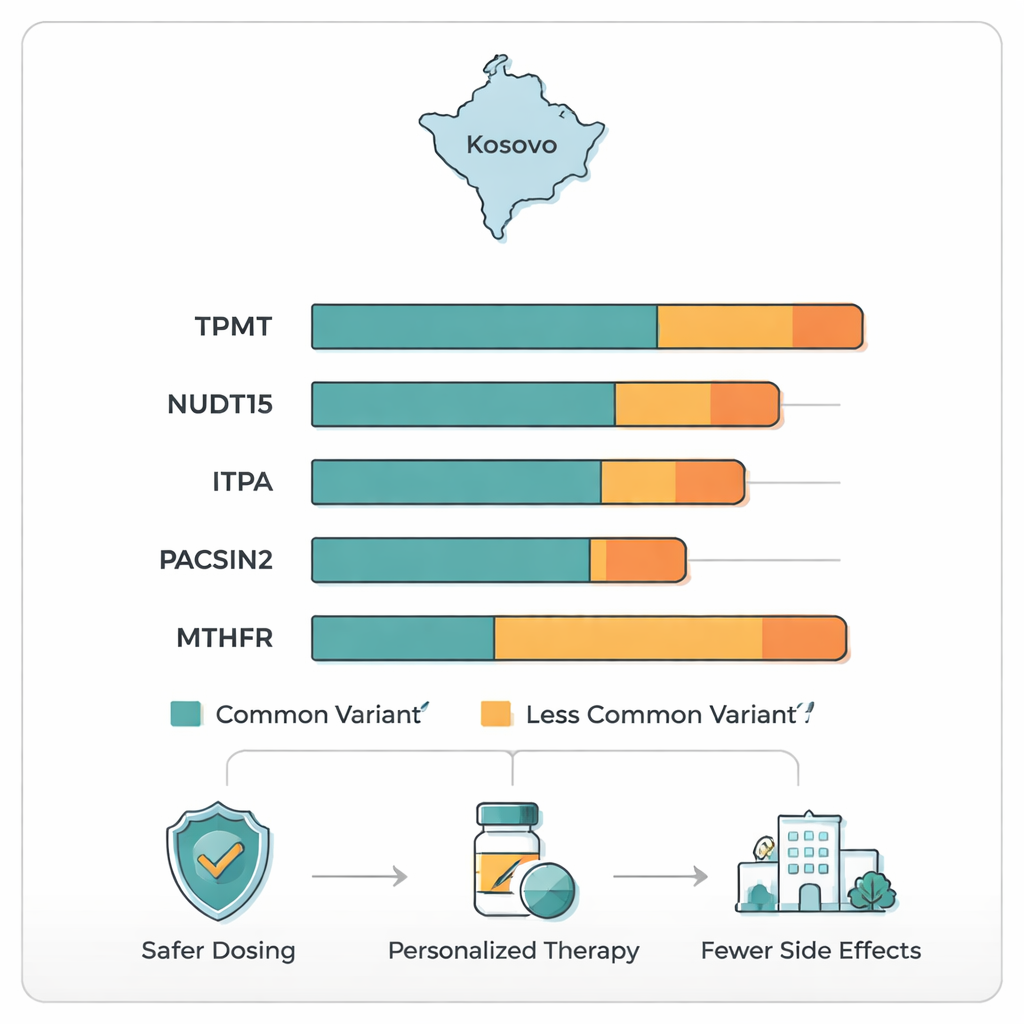
Health Implications Beyond One Drug
The unusually high frequency of the MTHFR variant in Kosovo may have consequences that go beyond thiopurine dosing. This genetic change can reduce the activity of the MTHFR enzyme, which in turn may alter levels of homocysteine, a substance tied to heart and blood vessel health, and may increase the risk of certain birth defects when folate intake is low. In the context of thiopurines, reduced MTHFR activity could shift the balance of chemical reactions that determine how much of the drug is broken down or activated, possibly increasing sensitivity to treatment for some patients. The authors suggest that, in addition to considering gene-guided dosing of thiopurines, public health planners in Kosovo might want to pay special attention to folate nutrition, especially for women who are or may become pregnant.
From Genetic Map to Safer Treatment
For a lay person, the takeaway is that people in Kosovo, like people everywhere, carry a distinctive mix of genetic variants that can change how they respond to powerful medicines. This study provides a first detailed map of several such variants tied to thiopurine therapy, showing which ones are common enough to matter in day-to-day medical practice. Armed with this information, doctors and health authorities can move toward routine genetic testing before prescribing thiopurines, set safer starting doses and identify individuals who might need closer monitoring or alternative drugs. In the long run, this kind of population-specific genetic knowledge can turn trial-and-error prescribing into more precise and predictable care.
Citation: Pasha, F., Urbančič, D., Gosheva, G. et al. Population frequencies of thiopurine-related pharmacogenes in healthy individuals from Kosovo. Hum Genome Var 13, 3 (2026). https://doi.org/10.1038/s41439-026-00337-3
Keywords: pharmacogenomics, thiopurines, TPMT, NUDT15, MTHFR