Clear Sky Science · en
TMC6/8-associated epidermodysplasia verruciformis: germline variants and a complex structural alteration in a skin cancer predisposition syndrome
When Common Warts Hide a Cancer Risk
Most of us think of warts as a minor nuisance, but in a tiny number of families they signal something far more serious: a built-in tendency to develop skin cancer. This study looks at people with an inherited condition called epidermodysplasia verruciformis, in which harmless-looking, flat wart-like spots from a common skin virus can, over time and sun exposure, turn into aggressive skin tumors. By combining careful patient follow-up with cutting-edge DNA analysis, the researchers reveal how subtle changes in two genes quietly reshape the skin’s natural defenses and set the stage for cancer.
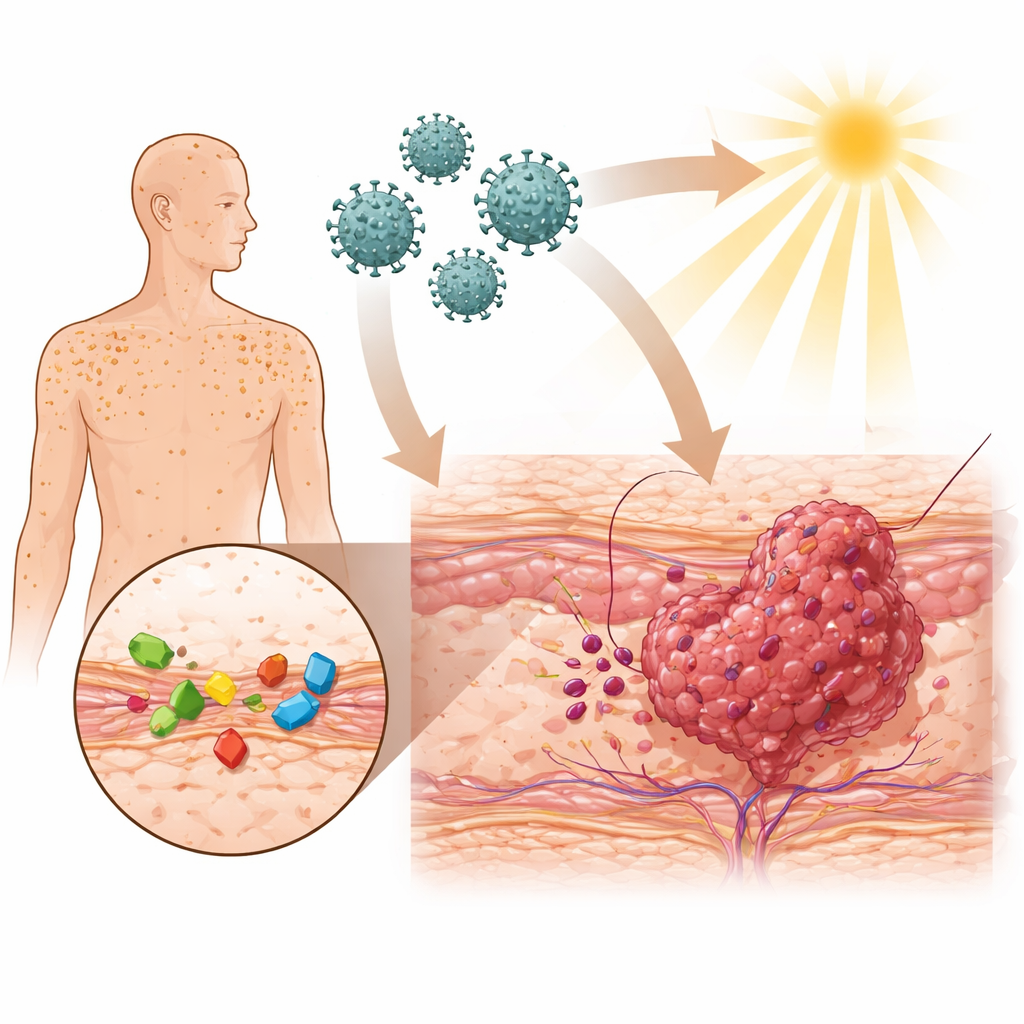
A Rare Disorder With Heavy Consequences
The team followed six adults from five unrelated Turkish families who all had the classic, hereditary form of this condition. Since childhood or early adulthood, they had flat warts and pale, scaly patches that favored sun-exposed areas like the face, scalp, and hands, and in some cases spread to the trunk, limbs, genitals, and even the voice box. None had known problems with their immune system that might otherwise explain such stubborn infections. Over the years, every one of them developed skin cancers called squamous cell carcinomas, and half also developed basal cell cancers. Tumors tended to recur, sometimes invade deeply, and in two people even required removal of an eye. One patient ultimately died from complications of widespread disease.
How Broken Defenses Let Viruses and Sunlight Team Up
In healthy skin, three partner proteins work together inside the outer skin cells to keep certain human papillomaviruses (the same family that causes warts) under tight control and to help maintain a stable internal environment. The genes TMC6 and TMC8, along with a third gene, provide the instructions for this protective trio. When this system fails, the beta-type papillomaviruses can persist and multiply in the skin. At the same time, disrupted control of minerals such as zinc makes the cell’s nucleus more hospitable to viral activity. Daily ultraviolet (UV) light from the sun then adds DNA damage on top of this chronic viral irritation. Over many years, this one-two punch—lingering infection plus UV injury—can push altered skin cells to become invasive cancers.
Tracking Down Hidden Genetic Changes
All six patients carried damaging inherited changes in either TMC6 or TMC8, firmly tying their symptoms to this specific breakdown in skin defense. Four of these DNA changes had never been reported before and included a missing stretch of protein, a frameshift that abruptly truncated a protein, and two mutations that disrupt how gene segments are stitched together. Most patients, whose parents were related, inherited identical faulty copies from each parent. One man, however, posed a puzzle: routine gene tests showed only a single faulty copy. To solve it, the researchers layered more advanced methods, including broad gene panels, computer-based searches for missing segments, and finally optical genome mapping, a technique that views very long DNA molecules directly.
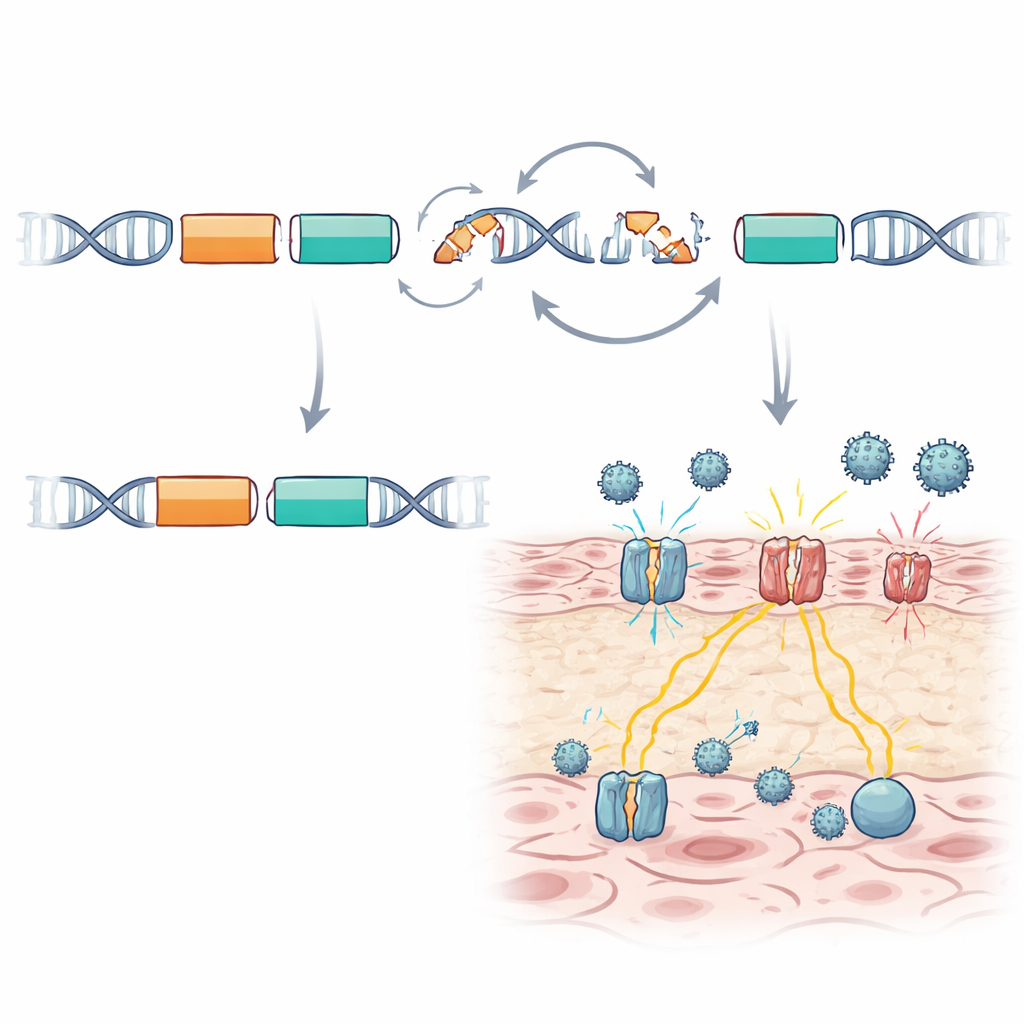
A Complex DNA Rearrangement Revealed
These deeper tests exposed an intricate reshuffling of DNA that standard methods had missed. A long section of the chromosome containing both TMC6 and TMC8 was cut, flipped in orientation, and partly deleted in a complicated “delete–invert–delete” pattern. This single structural change crippled both genes at once and sat on the same chromosome as an otherwise harmless, subtle DNA change that had initially attracted attention. Once the researchers mapped the exact breakpoints and confirmed them with targeted long-range PCR, they could see that the structural change, not the silent marker, was the true second hit. The benign marker, however, now serves as a useful signpost within the family to track who carries the risky chromosome when more elaborate testing is not available.
Why This Work Matters for Patients
For people born with this rare condition, the message of the study is stark but empowering: the risk of developing serious skin cancer is high, but with vigilant care, many tumors can be caught and treated early. The authors argue that persistent, widespread wart-like lesions in otherwise healthy individuals—especially in families with close parental relatedness—should prompt genetic testing for this syndrome and close dermatologic follow-up, with an emphasis on sun protection and early surgery rather than radiotherapy. More broadly, the work shows that in inherited cancer syndromes, missing genetic answers may lurk in complex DNA rearrangements that routine tests overlook, and that bringing structural variant detection into standard diagnostics can turn uncertain cases into clear, actionable diagnoses.
Citation: Durmaz, C.D., Güleray Lafcı, N., Erkan, D.D. et al. TMC6/8-associated epidermodysplasia verruciformis: germline variants and a complex structural alteration in a skin cancer predisposition syndrome. Eur J Hum Genet 34, 429–437 (2026). https://doi.org/10.1038/s41431-026-02043-8
Keywords: epidermodysplasia verruciformis, skin cancer, human papillomavirus, genetic predisposition, structural variants