Clear Sky Science · en
Harnessing pyroptosis in breast cancer therapy: immunological mechanisms and emerging biomaterial strategies
Turning Cell Death into a New Weapon Against Breast Cancer
Breast cancer remains one of the most common and stubborn cancers worldwide. Many tumors eventually evade surgery, chemotherapy, and even modern immunotherapies. This review explores an emerging idea: deliberately triggering a fiery form of cell death called pyroptosis inside breast tumors. By making cancer cells burst open in a controlled, inflammatory way, scientists hope to both kill the tumor directly and rouse the immune system to join the attack.
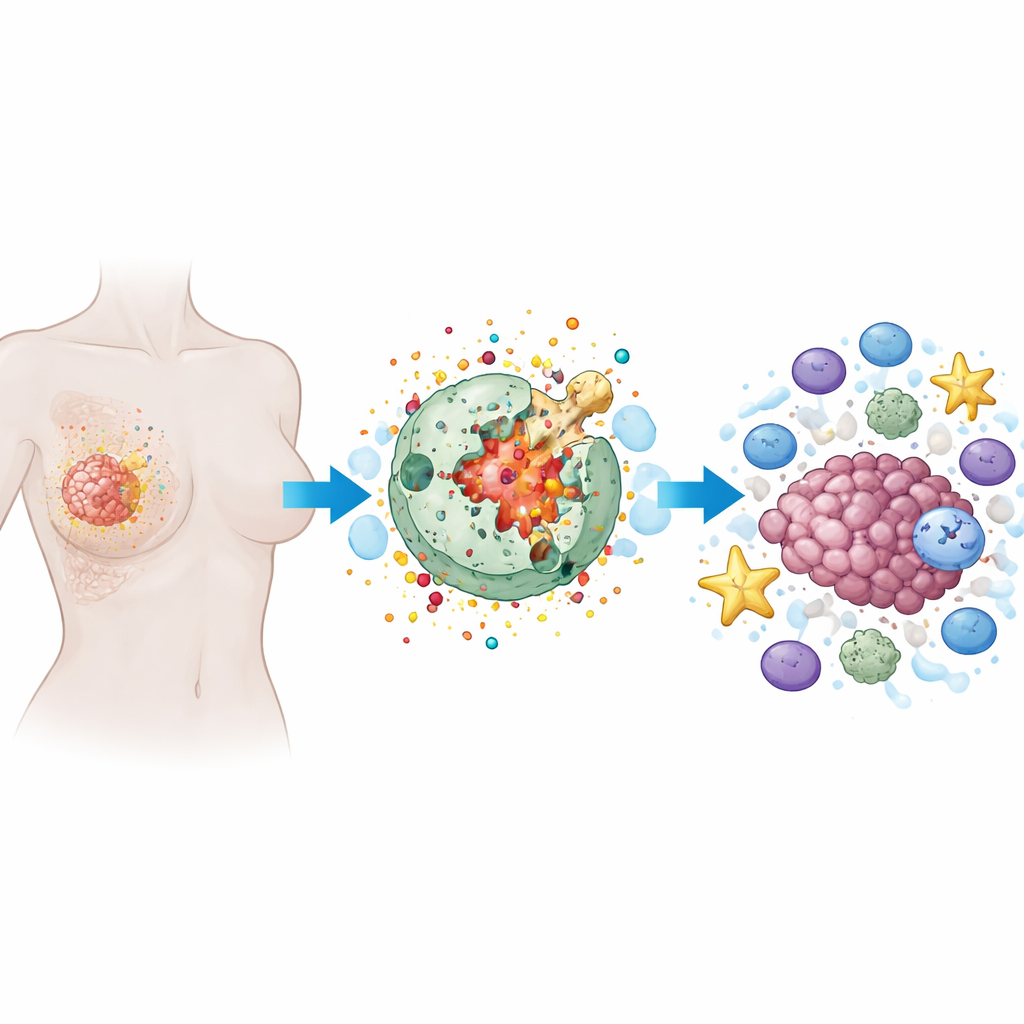
How a Fiery Form of Cell Death Works
Pyroptosis is a programmed form of cell death in which a cell swells, its outer membrane becomes riddled with pores, and it finally ruptures, spilling its contents. Unlike the quiet, tidy cell death seen in many therapies, pyroptosis is noisy and inflammatory. Specialized proteins, especially a family called gasdermins, act as tiny demolition charges. Once cut by internal enzymes, gasdermins punch holes in the cell membrane. This not only destroys the cancer cell but also releases alarm signals and inflammatory molecules that can summon and activate immune cells.
Why Breast Tumors Are a Special Challenge
Breast cancer is not a single disease but a collection of subtypes with different behaviors. Some, such as triple‑negative breast cancer, lack common drug targets and often resist treatment. Many breast tumors are considered “immunologically cold,” meaning they have few active immune cells inside. The review explains how features of the breast tumor environment — including stromal cells, immune-suppressive cells, and local oxygen shortages — can both set the stage for pyroptosis and, if poorly controlled, turn its inflammation into fuel for tumor growth and spread. This double‑edged nature makes precision especially important.
The Gasdermin Switches Inside Tumor Cells
A central theme of the article is how different gasdermin proteins act as molecular switches inside breast cancer cells. Versions such as GSDMD and GSDME can convert signals from chemotherapy, radiation, or attacking immune cells into full‑blown pyroptosis. Others, like GSDMC and some forms of GSDMB, are often higher in aggressive tumors and can both promote or restrain disease depending on how they are activated. Many breast cancers chemically silence GSDME, blunting pyroptosis and immune activation. Restoring or selectively triggering the right gasdermins could determine whether a therapy merely kills a few cells or turns the whole tumor into an in‑situ vaccine that alerts the immune system.
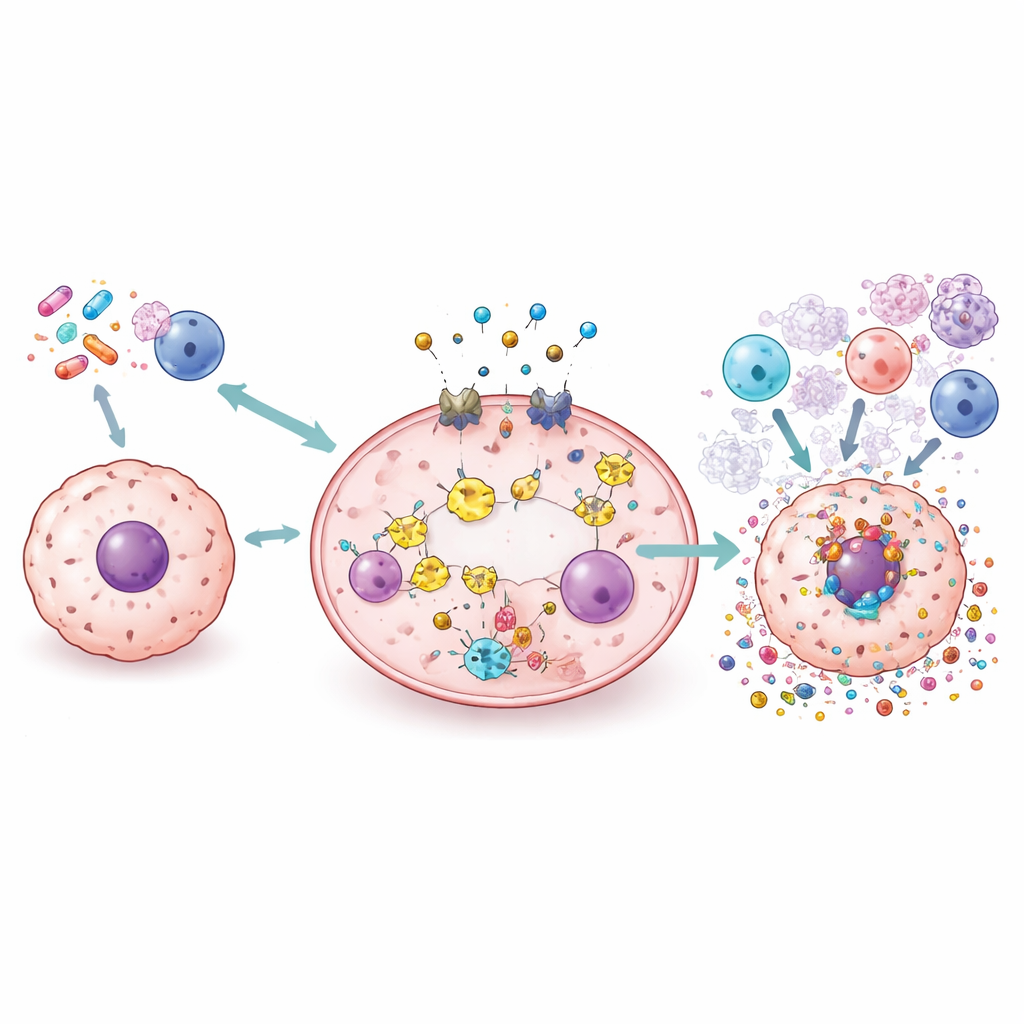
New Tools: Drugs, Nanoparticles, Viruses, and Radiation
The review surveys a wide range of strategies under study to harness pyroptosis safely. Standard drugs such as cisplatin and doxorubicin can be repurposed or reformulated to push cancer cells toward gasdermin‑driven bursting instead of quiet death. Small molecules can either amplify or block parts of the pathway to fine‑tune inflammation. Nanoparticles and biomimetic carriers are being designed to deliver chemotherapy, copper ions, or light‑activated molecules directly into tumors, where they trigger pyroptosis while sparing healthy tissues. Oncolytic viruses and radiotherapy can also be engineered or combined with other agents to provoke pyroptosis and reshape the tumor’s immune landscape, potentially making immune checkpoint drugs more effective.
Balancing Potent Benefit with Real Risks
Because pyroptosis is so inflammatory, the same reactions that help the immune system fight cancer can also damage normal tissues or even promote tumor growth if they become chronic. The authors highlight early biomarkers — such as gene signatures, methylation patterns, fragments of gasdermin proteins in blood, and cytokine profiles — that may help identify which patients are most likely to benefit and who is at higher risk of dangerous “cytokine storms.” Advanced nanomedicine designs, carefully chosen drug combinations, and real‑time monitoring of inflammatory markers are all being explored to keep the response sharp but controlled.
What This Could Mean for Future Patients
In plain terms, this review argues that making cancer cells “die loudly” could transform breast cancer care. By triggering pyroptosis in a precise subset of tumor cells, doctors may both shrink the tumor and wake up a powerful, lasting immune response, turning cold tumors hot and more responsive to modern immunotherapies. Yet pyroptosis is a volatile ally: if unleashed too broadly or for too long, it may worsen inflammation or encourage resistant cells to thrive. Future research will focus on mapping who will benefit, perfecting targeted delivery systems, and running clinical trials that pair pyroptosis‑inducing approaches with immune drugs. If these challenges can be solved, harnessing pyroptosis could add a potent new dimension to breast cancer treatment.
Citation: Asiedu, R.K.F., Souley Abdou, M., Wei, R. et al. Harnessing pyroptosis in breast cancer therapy: immunological mechanisms and emerging biomaterial strategies. Cell Death Discov. 12, 157 (2026). https://doi.org/10.1038/s41420-026-02996-1
Keywords: pyroptosis, breast cancer, gasdermin, tumor microenvironment, nanomedicine