Clear Sky Science · en
Botulinum toxin-induced masseter muscle atrophy is associated with impaired autophagic flux without signs of apoptosis in mice
Why jaw muscle shots matter
Botulinum toxin injections into the jaw’s chewing muscle, the masseter, are now common in both medicine and cosmetic clinics. They can ease jaw pain and slim a square face, but many patients notice that the muscle becomes thinner and weaker for months. This study in mice asks a simple but important question: what is happening inside those muscle cells, and does the treatment harm the muscle’s natural cleanup and repair systems?
Jaw relaxers and shrinking muscles
The masseter muscle helps us bite and chew with great force. When this muscle becomes overactive or enlarged, it can contribute to jaw joint pain and headaches, and some people seek a slimmer lower face by having it reduced. Botulinum toxin type A works by blocking the nerve signals that tell the muscle to contract, temporarily paralyzing it. Earlier research showed that this nerve block leads to a measurable loss of muscle mass and fiber size in animals, suggesting true atrophy rather than just relaxation. However, it was unclear whether this shrinkage came from cells dying, or from changes in the way the muscle breaks down and recycles its own components.
Checking for cell death in the jaw
One possibility was that the toxin might trigger apoptosis, a form of programmed cell death often described as cellular suicide. To test this, the researchers injected botulinum toxin into one masseter muscle of adult mice and saline into the opposite side as a control. They then looked for several well-known molecular signs of apoptosis, as well as for broken DNA in the muscle cell nuclei. Across multiple time points in the first week, they found no increase in any of these death markers. The number of cells with fragmented DNA stayed extremely low, unlike in positive-control samples where DNA damage had been deliberately induced. These results indicate that the jaw muscle fibers were not being lost through a wave of classic cell death after treatment.
The muscle’s recycling system gets jammed
The team then turned to autophagy, the cell’s internal recycling system. Autophagy packages worn-out proteins and damaged structures into small sacs that fuse with digestion compartments, allowing their contents to be broken down and reused. In healthy muscle, this process helps keep fibers strong and functional. After botulinum toxin injection, the researchers saw a substantial buildup of several proteins that mark these recycling sacs, along with many more bright puncta inside the fibers when viewed under the microscope. At first glance, this might look like autophagy was being activated. But when they used the drug chloroquine, which is known to block the final steps of autophagy, the levels of these markers did not rise any further. Together with the unchanged ratio of different forms of a key autophagy protein, this pattern points to a jammed assembly line: recycling packages are formed but fail to be delivered and cleared.
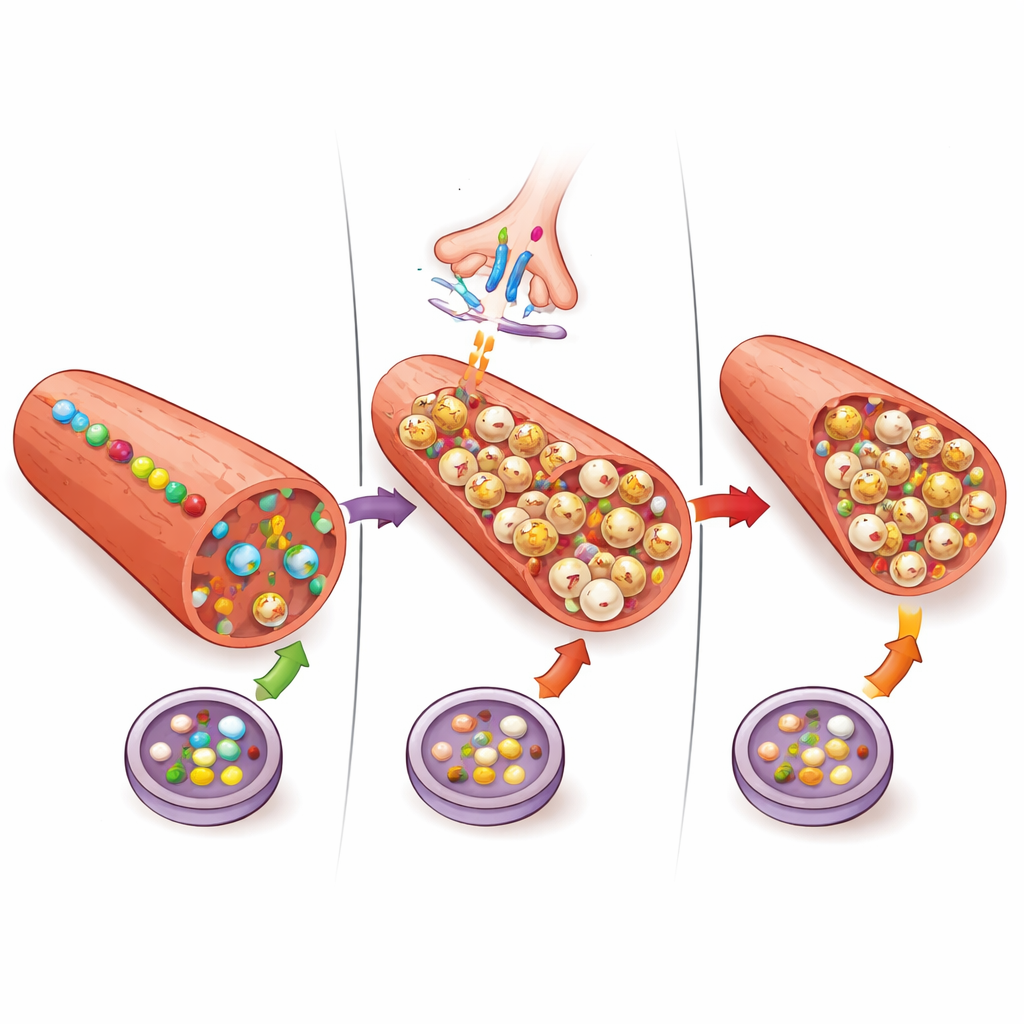
From stalled cleanup to thinner muscle
The researchers next asked how these molecular changes related to actual muscle loss. They measured muscle weight and the diameter of individual fibers and confirmed that the botulinum-treated masseter was lighter and made up of thinner fibers. Importantly, the amount of buildup of one recycling marker, called LC3, tracked with how much muscle mass was lost in each animal. When they blocked autophagy with chloroquine alone, fibers did not significantly shrink. However, adding chloroquine on top of botulinum toxin did not make atrophy worse, suggesting that both interventions were converging on the same blocked recycling step and that this block itself does not directly drive the bulk of protein breakdown. Other systems that chew up proteins, such as the ubiquitin–proteasome pathway shown in earlier work, are likely doing most of the degrading.
What this means for patients and future care
In plain terms, the study finds that common jaw botulinum injections do not appear to kill muscle cells in this mouse model, but they do disturb the muscle’s internal housekeeping by clogging its recycling machinery. This clogged state is linked to loss of muscle size, even though it is probably not the main engine of protein destruction. Because the experiments involved only single doses in young male mice, real-world treatments that involve repeated injections, different ages, or women may have different long-term effects. Still, the work highlights that muscle atrophy after botulinum toxin is biologically complex and that protecting or restoring the cell’s recycling system could one day help reduce unwanted, lasting muscle loss in people who rely on these injections for medical or cosmetic reasons.
Citation: Quezada, E.R., Blanco, N., Llanos, P. et al. Botulinum toxin-induced masseter muscle atrophy is associated with impaired autophagic flux without signs of apoptosis in mice. Cell Death Discov. 12, 121 (2026). https://doi.org/10.1038/s41420-026-02982-7
Keywords: botulinum toxin, masseter muscle, muscle atrophy, autophagy, jaw disorders