Clear Sky Science · en
Irisin inhibits adipogenic differentiation of bone marrow mesenchymal stem cells through the SIRT1/RANBP2/FTO signaling axis and protects against osteoporosis
Why a Muscle Hormone Matters for Fragile Bones
Osteoporosis often seems like a simple problem of “weak bones,” but deep inside our skeletons a quiet tug-of-war is taking place. The same stem cells in bone marrow can either become bone-building cells or fat cells. As we age, especially after menopause, this balance tilts toward fat, leaving bones thinner and more breakable. This study explores how a hormone released by exercising muscles, called irisin, can push those stem cells back toward making bone instead of fat, pointing to a future in which a workout hormone might help protect against osteoporosis.
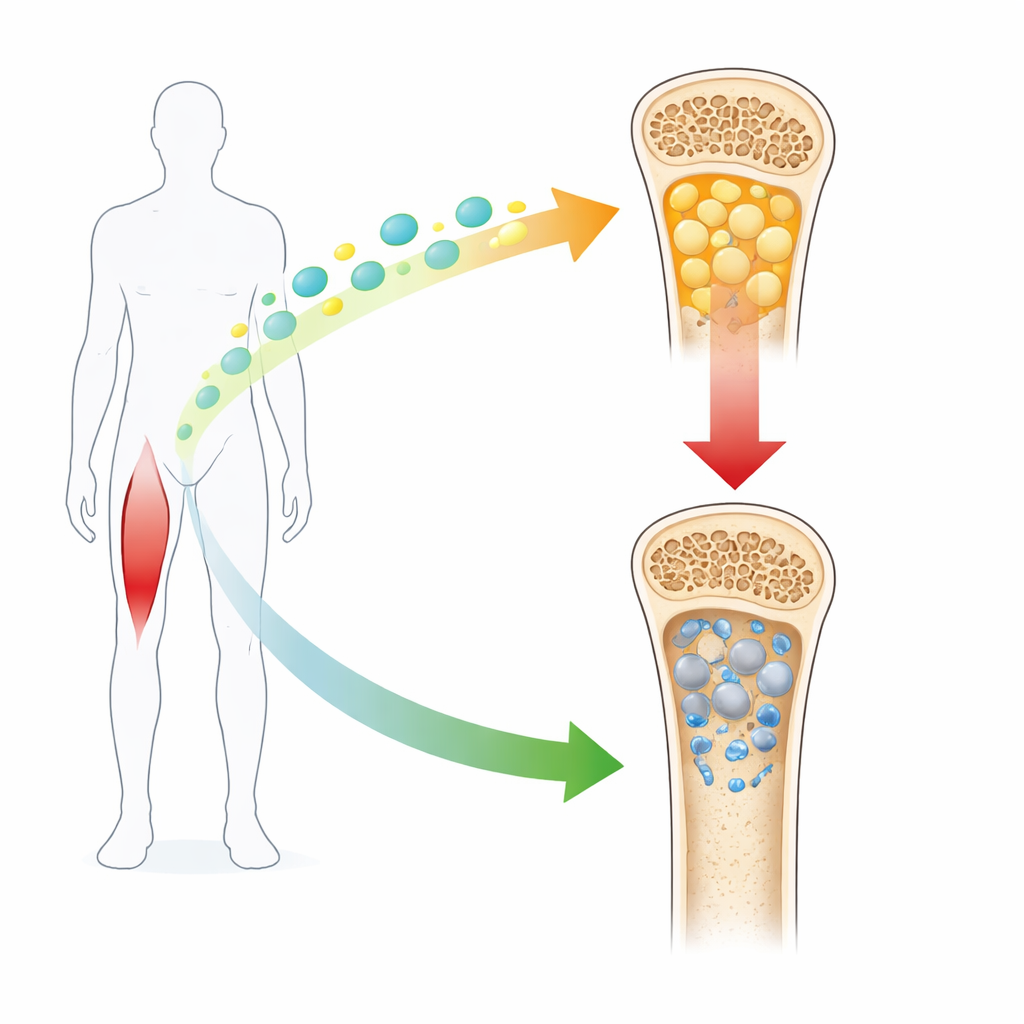
When Bone Turns to Fat
Bone marrow is not just an empty cavity but a bustling workshop of stem cells that can choose different fates. In healthy adults, enough of these cells become bone-forming builders to keep the skeleton strong. In osteoporosis, especially in postmenopausal women, more of these cells turn into fat-storing cells instead. This “bone marrow obesity” goes hand in hand with fragile bones and fractures. The researchers started by confirming that this shift toward fat is accompanied by lower levels of irisin, both in mice with estrogen loss and in human patients with osteoporosis, linking a drop in this hormone to worsening bone health.
A Exercise-Linked Signal with a Double Role
Irisin is released by muscles during physical activity and has been studied for its effects on metabolism and energy use. Here, the team asked whether irisin also helps decide whether bone marrow stem cells become fat or bone. In lab dishes, they added irisin to mouse bone marrow stem cells and watched what happened. Irisin boosted the cells’ ability to turn into bone-forming cells, increasing mineral deposits and the activity of key bone genes. At the same time, it strongly suppressed their transformation into fat cells, reducing fat droplets and dialing down genes and proteins that drive fat formation. In live mice whose ovaries had been removed to mimic postmenopausal bone loss, weekly irisin injections preserved bone mass and microstructure and reduced the buildup of fat inside the marrow cavity.
Inside the Cell’s Decision Machinery
To understand how irisin exerts this control, the researchers looked at changes in gene activity when stem cells were exposed to irisin during fat formation. One standout player was SIRT1, a protein known for regulating aging, metabolism, and stress responses. The team showed that turning down SIRT1 made cells more likely to become fat, while boosting SIRT1 had the opposite effect. Importantly, when SIRT1 was reduced, irisin could no longer effectively block fat formation, in cells or in mice, revealing that SIRT1 is a key relay in irisin’s bone-protective signal.
A Molecular Chain That Disarms a “Fat” Protein
Diving deeper, the study focused on another protein, FTO, which has been tied to obesity and fat storage. High levels of FTO support fat-cell development, in part by stabilizing a master fat regulator called PPARγ. The researchers found that SIRT1 did not change how much FTO was produced at the gene level, but instead affected how stable the FTO protein was. Irisin-activated SIRT1 increased the activity of a third protein, RANBP2, which tags FTO in a way that marks it for breakdown. When RANBP2 was reduced, SIRT1 could no longer lower FTO protein levels, and fat formation rebounded. Through this chain—irisin to SIRT1, SIRT1 to RANBP2, and RANBP2 to FTO degradation—the cells shifted away from becoming fat cells and back toward bone-forming roles.
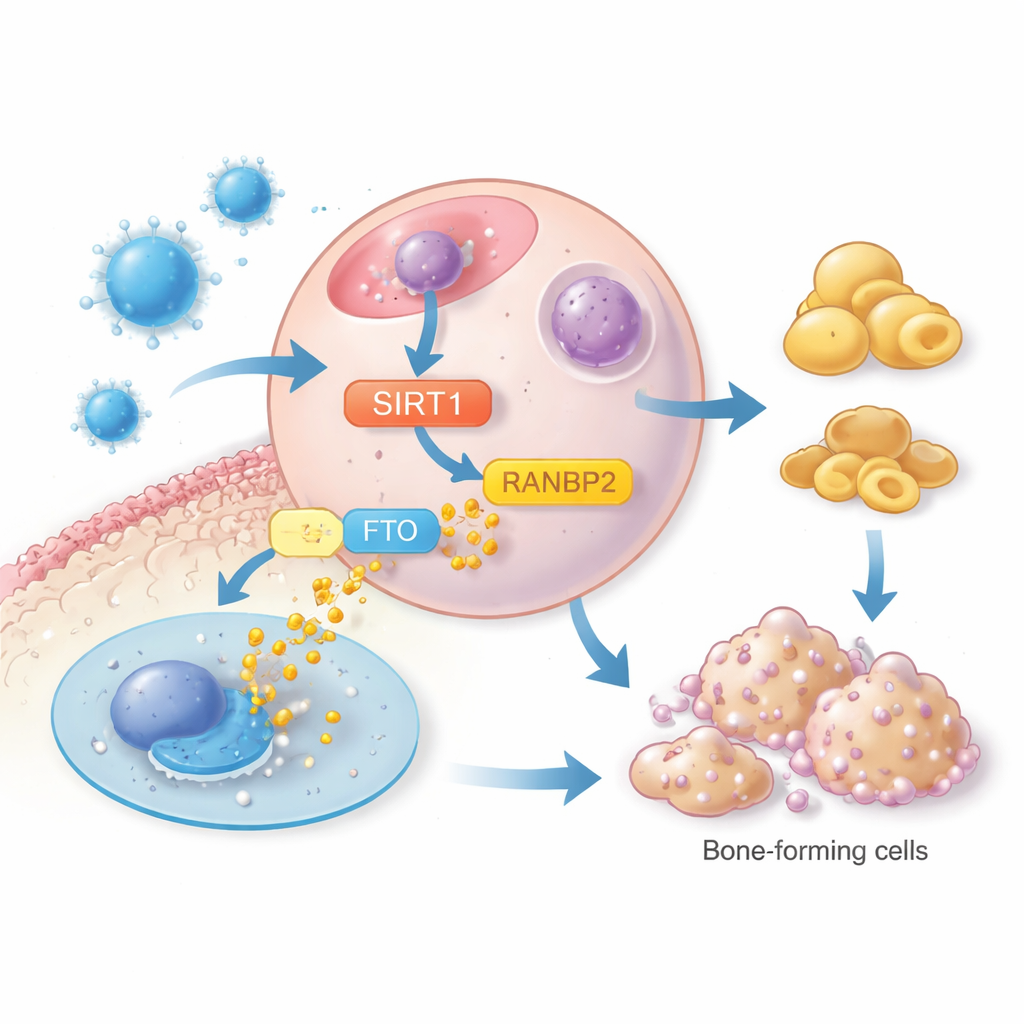
What This Could Mean for Future Bone Care
By tracing this stepwise pathway, the study reveals irisin as more than a simple exercise hormone. It acts as a molecular traffic officer in bone marrow, steering stem cells away from becoming fat and toward building bone, through a SIRT1–RANBP2–FTO signaling axis. For non-specialists, this means that maintaining or mimicking the body’s natural irisin signal could one day become a strategy to prevent or treat osteoporosis, complementing lifestyle measures like exercise. While more work is needed in larger human studies, the findings point to a promising new set of molecular targets for keeping bones stronger for longer.
Citation: Chen, J., Liu, J., Fu, Q. et al. Irisin inhibits adipogenic differentiation of bone marrow mesenchymal stem cells through the SIRT1/RANBP2/FTO signaling axis and protects against osteoporosis. Cell Death Discov. 12, 114 (2026). https://doi.org/10.1038/s41420-026-02976-5
Keywords: osteoporosis, irisin, bone marrow stem cells, bone fat balance, SIRT1 signaling