Clear Sky Science · en
Unlocking glioma vulnerabilities: targeting regulated cell death pathways for innovative therapies
Why Brain Tumor Cell Death Matters
Gliomas are among the most common and deadly brain tumors in adults. Even with surgery, radiation, and chemotherapy, they often come back and are difficult to control. This review article explores a new angle of attack: exploiting the different ways cells can be programmed to die. By understanding and steering these “self-destruct” routes, researchers hope to expose weaknesses in glioma cells and make future treatments more effective and more personal.
How Gliomas Outsmart Standard Treatments
Gliomas arise from the brain’s support cells and range from slow-growing to highly aggressive forms such as glioblastoma. Their poor outcomes stem from several intertwined problems: genetic mutations, epigenetic changes, hard-to-kill stem-like cells, an abnormal blood supply, and a highly suppressive immune environment. On top of that, the blood–brain barrier limits how well drugs can reach the tumor. Together, these factors allow tumor cells to survive surgery and standard drugs, adapt to stress, and eventually regrow. 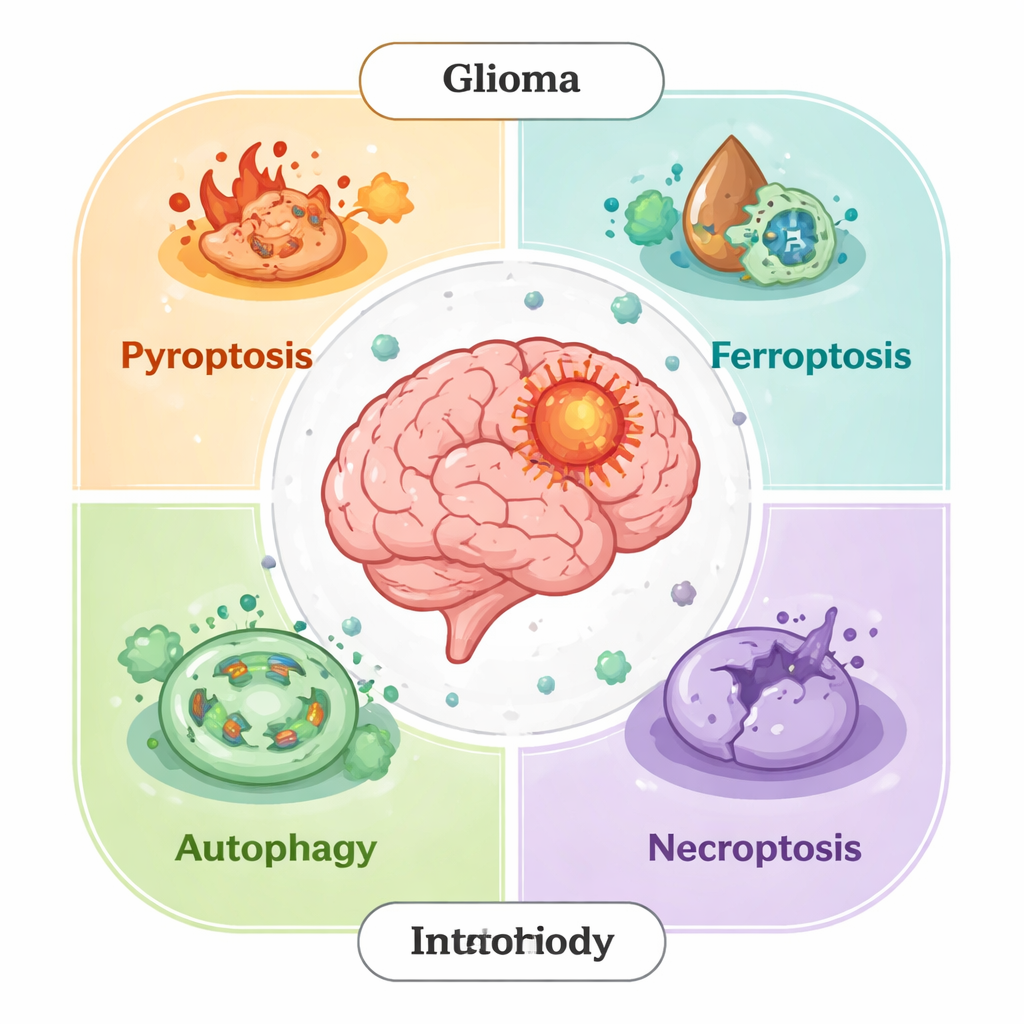
The Many Faces of Cell Self-Destruction
For decades, scientists focused on one main form of programmed cell death, called apoptosis. We now know this is only part of the story. Glioma cells can also die through other regulated routes: pyroptosis (a fiery, inflammatory burst), ferroptosis (iron-driven membrane damage), necroptosis (a controlled version of cell rupture), and autophagy-dependent death (self-digestion that can go too far). In healthy tissues, these processes remove damaged cells and prevent cancer. In tumors, however, glioma cells often rewire these pathways—blocking death signals, boosting antioxidant defenses, or turning autophagy into a survival tool—to resist treatment and shape a microenvironment that favors their growth.
Turning Death Pathways into Therapy
Instead of seeing these death routes as a problem, researchers are learning to weaponize them. Pyroptosis-inducing strategies use smart nanoparticles, light-based heating, engineered viruses, or drug-loaded hydrogels to make glioma cells swell, burst, and release danger signals that alert the immune system. Ferroptosis-based approaches push tumor cells into iron-fueled collapse by blocking key protective enzymes like GPX4, disrupting glutathione production, or changing how tumor cells handle fats. Many of these tactics are delivered with advanced carriers, including graphdiyne and other nanoparticles, to help drugs cross the blood–brain barrier and concentrate inside the tumor while sparing healthy brain tissue. 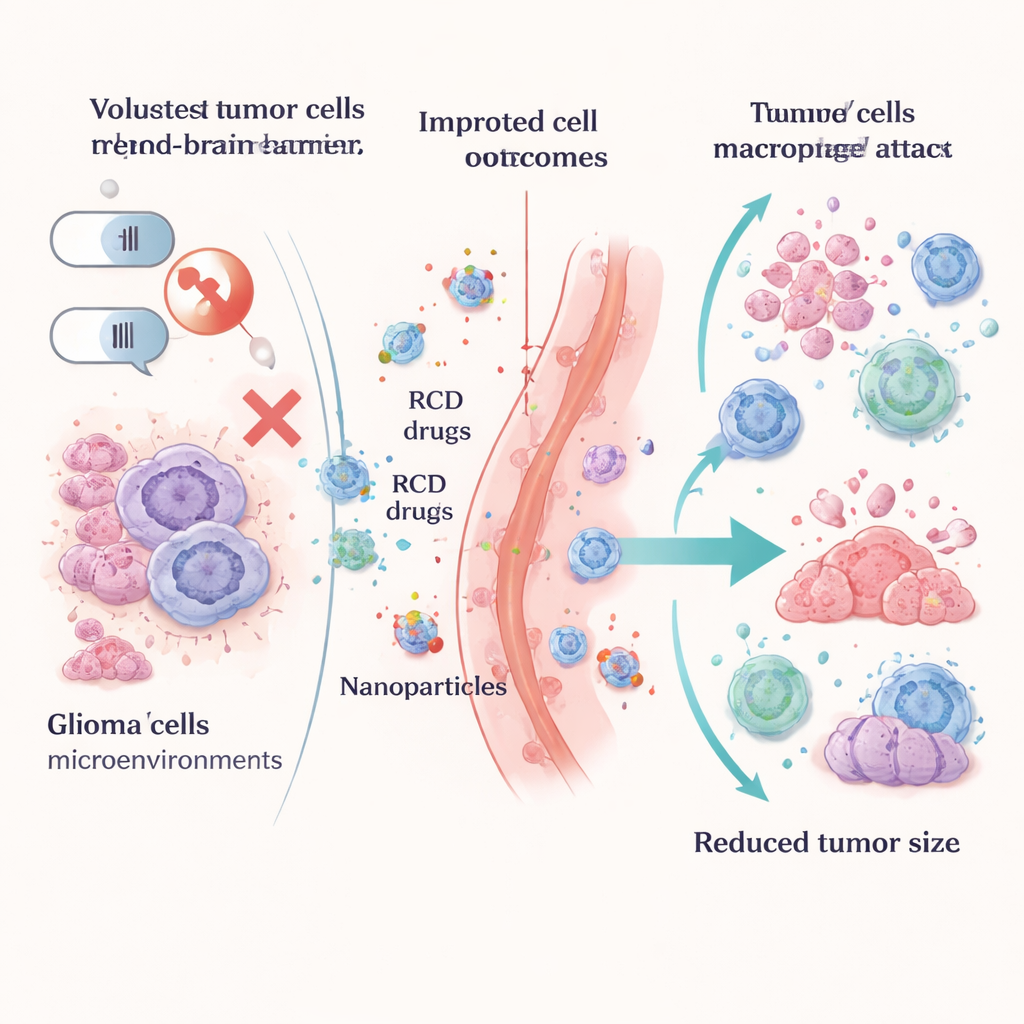
Rebooting the Tumor’s Immune Landscape
Necroptosis-focused therapies aim to overcome resistance in cells that no longer respond to standard death signals. Natural products such as shikonin, emodin, and celastrol derivatives can push glioma cells into necroptosis, which not only kills them but also releases molecules that draw immune cells into the tumor. At the same time, scientists are probing autophagy, sometimes blocking it to prevent tumor cells from using “self-cleaning” to ride out radiation and chemotherapy, and sometimes pushing it beyond its limits to trigger cell death. Early clinical trials with drugs like chloroquine and hydroxychloroquine show that autophagy can be safely modulated in patients, even though clear survival benefits have not yet been proven.
From Lab Discoveries to Personalized Care
Translating these concepts into real-world treatments remains challenging. Gliomas are highly varied from patient to patient, and within a single tumor, so no single death pathway strategy will fit everyone. The blood–brain barrier still hampers drug delivery, and the immune microenvironment can blunt even clever combinations of therapies. The authors highlight promising directions: pairing ferroptosis inducers with immune checkpoint inhibitors, combining oncolytic viruses with drugs that boost cancer cell “eat me” signals, or adding autophagy modulators to selected chemo-radiation regimens. Multi-omics profiling and better biomarkers should help identify which patients are most likely to benefit from a given mix of strategies.
Looking Ahead: Making Tumors Choose Self-Destruct
In simple terms, this article concludes that the future of glioma treatment may lie in forcing tumor cells to press their own self-destruct buttons in carefully controlled ways. By learning how to trigger and coordinate pyroptosis, ferroptosis, necroptosis, and autophagy-dependent death—and by coupling these with modern immunotherapies and precision drug delivery—researchers hope to turn a currently grim diagnosis into one that is more manageable and, ultimately, more curable.
Citation: Guo, J., Zong, L., Huang, Y. et al. Unlocking glioma vulnerabilities: targeting regulated cell death pathways for innovative therapies. Cell Death Discov. 12, 95 (2026). https://doi.org/10.1038/s41420-026-02949-8
Keywords: glioma, regulated cell death, pyroptosis, ferroptosis, glioblastoma therapy