Clear Sky Science · en
Loss of DIAPH3 accelerates glioma genesis in mice
Why this brain study matters
Glioblastoma is one of the deadliest brain cancers, and despite surgery, radiation, and chemotherapy, most patients survive little more than a year. This study asks a basic but crucial question: what early changes inside brain cells push them toward becoming such aggressive tumors, and why are these tumors so hard to kill with radiation? By tracking a single structural protein in mouse brain cells, the researchers uncover how its loss destabilizes chromosomes, speeds tumor appearance, and helps cancer stem-like cells weather radiation that should destroy them.
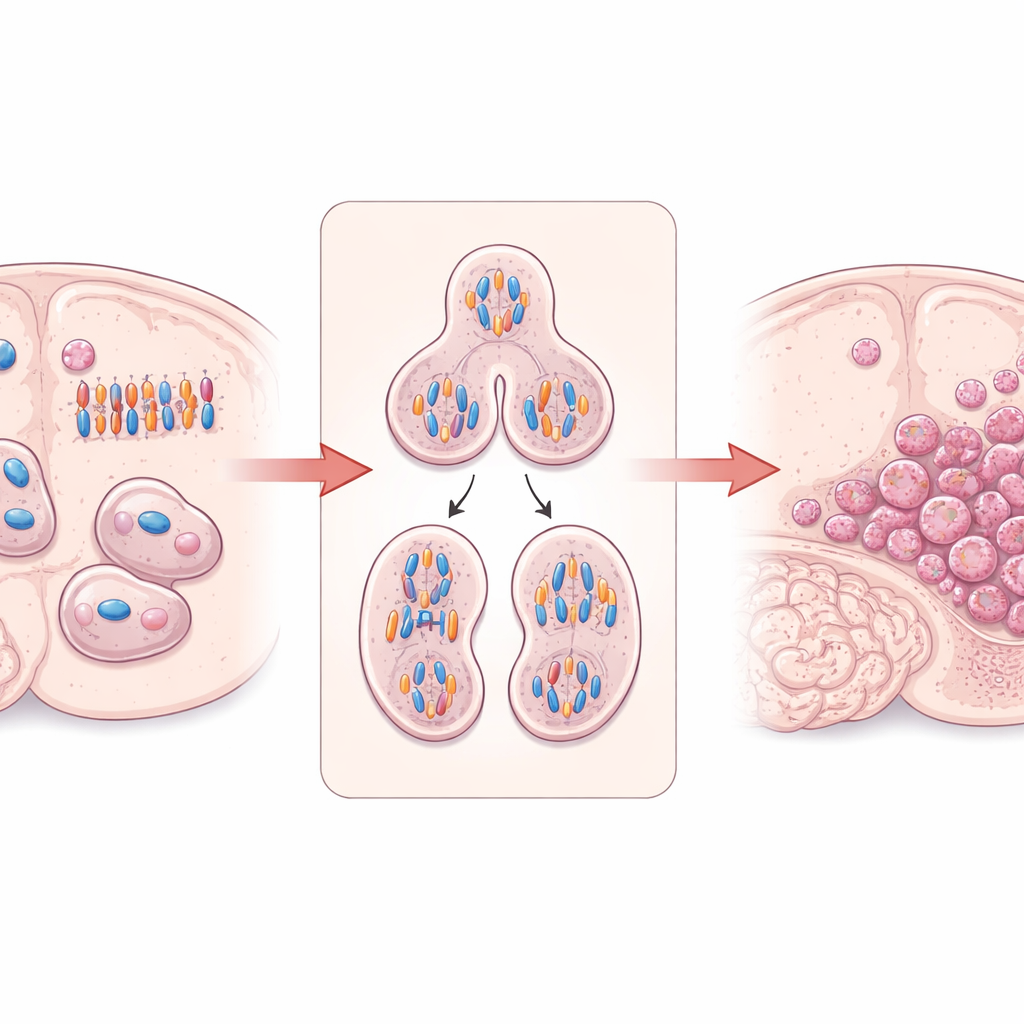
A cell “builder” that keeps division in line
The work centers on DIAPH3, a protein that helps build and organize the cell’s internal scaffolding of actin filaments and microtubules. In dividing brain stem cells, DIAPH3 is vital for forming a proper spindle—the structure that pulls duplicated chromosomes apart—and for pinching one cell into two. Earlier research showed that when DIAPH3 is missing in developing mouse brains, dividing cells often mis-handle chromosomes, leading to abnormal chromosome numbers (aneuploidy), stalled cell cycles, and cell death. Intriguingly, a small region of human chromosome 13 that contains the DIAPH3 gene is frequently deleted in glioblastoma, and higher DIAPH3 levels have been linked to better survival in some patients, hinting that this protein may act as a tumor suppressor in the brain.
Engineering mouse brains to grow tumors
To test whether losing DIAPH3 truly promotes brain cancer, the team created mice in which two genes could be selectively deleted in cortex-forming stem cells: Diaph3 and Trp53, the latter encoding the well-known guardian of the genome, p53. Mice lacking only Diaph3 in this region did not develop tumors even after two years, implying that p53 can still eliminate highly abnormal cells. In contrast, mice lacking Trp53 alone, or both Trp53 and Diaph3, eventually formed high-grade diffuse gliomas that closely resembled human disease under the microscope. Using repeated ultra‑high‑field MRI scans, the researchers showed that animals missing both genes developed detectable tumors earlier, and by midlife they more often harbored large gliomas, particularly in the olfactory bulbs, than mice missing Trp53 alone. Tumor growth rate, once started, was similar between groups—what changed was how soon tumors appeared.
Chromosome chaos and rewired gene activity
Digging into why DIAPH3 loss hastens tumor onset, the team examined gene activity in the olfactory bulbs of young mice before any tumors were visible. In animals lacking both Diaph3 and Trp53, 126 genes were expressed at different levels compared to Trp53-only mutants, and nearly half of these had previous ties to cancer. Many changes clustered in pathways that drive cell growth, migration, and blood-vessel formation, including VEGF, MAPK, RAS, Rap1, and cAMP signaling, as well as G‑protein–coupled receptor networks. This altered molecular landscape suggested that cells were being nudged toward a cancer-like state earlier. Whole‑genome copy-number analysis of fully formed tumors revealed that DIAPH3 deficiency did not greatly increase small, focal DNA changes but instead boosted large, whole‑chromosome gains and losses—exactly the aneuploidy expected from faulty chromosome segregation.
Built‑in DNA damage and hardier cancer stem cells
Aneuploid tumor cells carried more internal DNA damage, detected by elevated levels of the DNA-break marker γ‑H2AX spread across cell nuclei. Yet these tumors still grew, implying that they had acquired ways to tolerate such stress. Comparing gene expression in established tumors, the researchers found hundreds of genes altered by DIAPH3 loss, including striking amplification and overproduction of the growth-factor receptor FGFR2 in many double‑mutant tumors. FGFR2 is known to boost DNA repair machinery in glioblastoma cells, and its activation has been linked to resistance to radiation. The team isolated glioma stem-like cells from mouse tumors and tested their response to a clinically relevant dose of ionizing radiation. Before treatment, stem-like cell frequency was similar in both genotypes, but after irradiation, cultures from DIAPH3‑deficient tumors retained roughly twice as many active stem-like cells as those from Trp53-only tumors, demonstrating greater radioresistance.
What this means for brain cancer
Taken together, the study paints DIAPH3 as a guardian that helps brain stem cells divide with the right number of chromosomes. When both DIAPH3 and p53 are missing, cell division becomes error‑prone, whole chromosomes are lost or gained, and DNA damage builds up. Rather than dying, some cells adapt by amplifying repair‑linked factors such as FGFR2, transforming into aneuploid, high‑grade gliomas whose stem-like cells are unusually resistant to radiation. While mouse models do not capture every feature of human glioblastoma, these findings support DIAPH3 as both a potential biomarker of prognosis and a node in the web of processes that control tumor initiation, genome stability, and treatment response—opening new avenues for therapies that might one day make this devastating brain cancer more vulnerable to existing treatments.
Citation: Chehade, G., Durá, I., Ruiz-Reig, N. et al. Loss of DIAPH3 accelerates glioma genesis in mice. Cell Death Dis 17, 342 (2026). https://doi.org/10.1038/s41419-026-08652-x
Keywords: glioblastoma, chromosomal instability, brain tumor stem cells, radiation resistance, tumor suppressor genes