Clear Sky Science · en
CBX2 phase-separation contributes to homologous recombination repair and drug resistance in ovarian cancer
Why this research matters
Ovarian cancer is one of the deadliest cancers in women largely because many tumors stop responding to chemotherapy. This study uncovers a hidden survival trick used by high‑grade serous ovarian cancers: they build tiny liquid‑like droplets inside the cell nucleus that supercharge DNA repair, helping tumor cells shrug off damage from standard drugs. The work also points to an existing pill, Ibrutinib, as a possible way to exploit this weakness in patients whose tumors rely on this droplet‑based repair system.
Tumor cells that fix their DNA too well
Most powerful cancer drugs work by damaging DNA so badly that tumor cells can no longer divide. In high‑grade serous ovarian cancer, however, many tumors become experts at patching up this damage, leading to resistance against platinum chemotherapy and PARP inhibitor drugs. The authors focused on a protein called CBX2, which reads chemical marks on DNA packaging and is found at higher levels in ovarian tumors than in normal tissue. Across patient datasets and tissue samples, tumors with more CBX2 were more likely to resist platinum treatment and to come back sooner, especially in this aggressive ovarian cancer subtype.
Droplets in the nucleus: a repair‑boosting "workbench"
CBX2 has an unusual ability to form dense, droplet‑like clusters inside the cell nucleus, a process known as phase separation. These droplets behave like tiny liquid workbenches that can concentrate specific proteins. By comparing cancer cells with normal CBX2, no CBX2, or a mutant form that cannot form droplets, the researchers showed that CBX2 droplets are central to how tumor cells mend broken DNA. When CBX2 was removed, chromosomes broke more often, DNA damage signals accumulated, and both major DNA double‑strand break repair routes were weakened. Restoring normal CBX2 brought back these repair abilities, but a droplet‑defective version did not, even though it could still bind DNA. 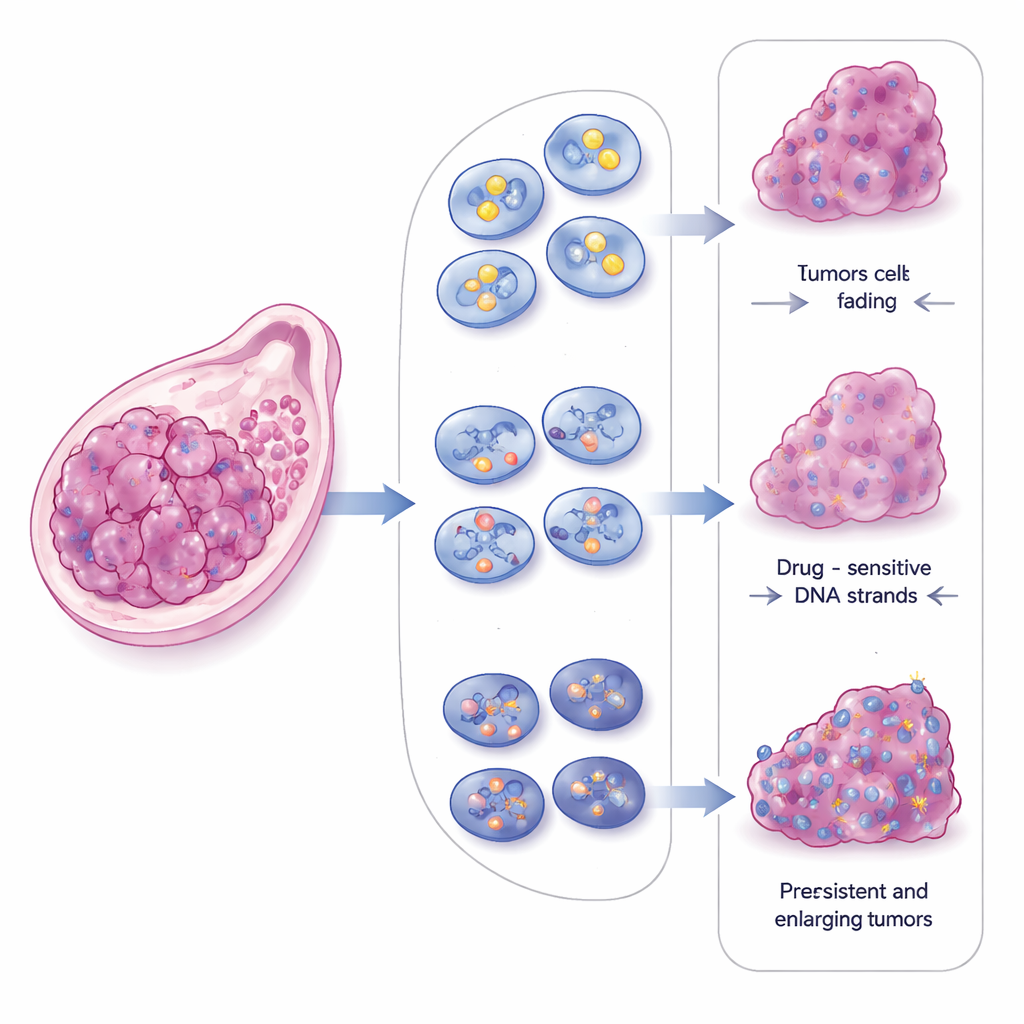
How CBX2 droplets organize the repair crew
Digging deeper, the team examined which repair proteins actually end up attached to DNA in the presence or absence of CBX2 droplets. They found that CBX2 droplets help recruit key players in the damage response, including PARP1, 53BP1, BRCA1, and RAD51—proteins that decide how a break is fixed and then execute the repair. Live‑cell imaging revealed two flavors of CBX2 droplets: a mobile, liquid form that dynamically mixes with damaged chromatin, and a dense, solid‑like form that does not. Only the mobile droplets overlapped with DNA damage foci and the main repair proteins, suggesting that this fluid phase acts as the functional scaffold that gathers and organizes the repair machinery precisely where it is needed.
Turning a strength into a weakness with an existing drug
Because CBX2 droplets make tumor cells especially good at repairing DNA, the authors asked whether this heightened repair capacity could be turned against them. They screened a library of compounds on cells with or without functional CBX2 droplets and discovered that Ibrutinib—an oral drug already approved for certain blood cancers—was particularly toxic to cells that relied on CBX2 condensates. Ibrutinib did not stop the droplets from forming, but it selectively crippled the high‑fidelity repair route that these cells depend on. In animal models, tumors containing CBX2 droplets shrank under Ibrutinib treatment, and three‑dimensional organoids grown from patients’ tumors with high CBX2 levels were more sensitive to the drug than those with low levels. 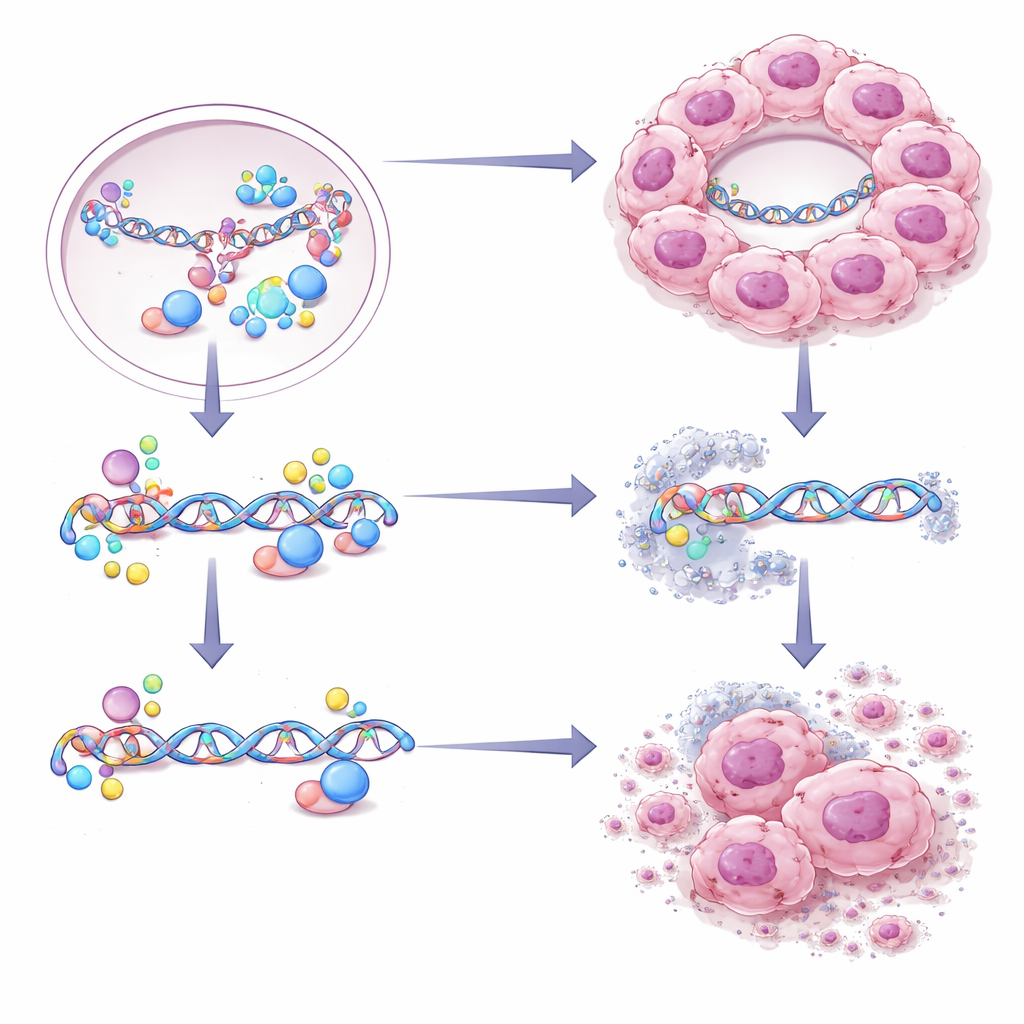
What this could mean for patients
For patients, the study suggests two important ideas. First, the presence and pattern of CBX2 droplets in tumor tissue may help predict how well someone will respond to platinum chemotherapy and PARP inhibitors: patients whose tumors lack CBX2 do best, those with diffuse CBX2 are in the middle, and those with clear CBX2 condensates fare worst. Second, that same droplet pattern may flag patients who could benefit from Ibrutinib, repurposing a blood‑cancer drug for a hard‑to‑treat ovarian cancer subtype. In essence, the work shows that the very structures that protect tumor DNA can also expose a new Achilles’ heel—offering a potential route to more personalized and effective treatment.
Citation: Sun, S., Huang, L., Ma, Y. et al. CBX2 phase-separation contributes to homologous recombination repair and drug resistance in ovarian cancer. Cell Death Dis 17, 366 (2026). https://doi.org/10.1038/s41419-026-08605-4
Keywords: ovarian cancer, drug resistance, DNA repair, phase separation, Ibrutinib