Clear Sky Science · en
Prostaglandin E2 induces dendritic cell dysfunction in skin involvement of breast cancer
Why cancer in the skin is so hard to treat
When breast cancer spreads into the skin, it is more than a cosmetic problem. These stubborn skin lesions often resist surgery, radiation, and drugs, and they are linked to a higher chance of the cancer coming back and a greater risk of death. This study asks a simple but crucial question: what is happening in the skin’s own immune defenses that lets these tumors take hold—and could fixing that local immune failure open a new way to treat patients?
The skin’s front-line guards under pressure
Our skin is packed with immune sentinels that constantly scan for danger. Among the most important are dendritic cells, which act like border guards and teachers at once: they pick up suspicious material and then train killer T cells to recognize and attack it. In healthy tissue, this partnership helps the body keep infections and abnormal cells under control. The researchers examined skin samples from 47 women with breast cancer, some with obvious tumor nodules in the skin and others without. They found that in skin invaded by cancer, a key type of dendritic cell was not only less abundant but also appeared “sleepy,” showing fewer of the surface features that signal a ready-for-action immune cell.
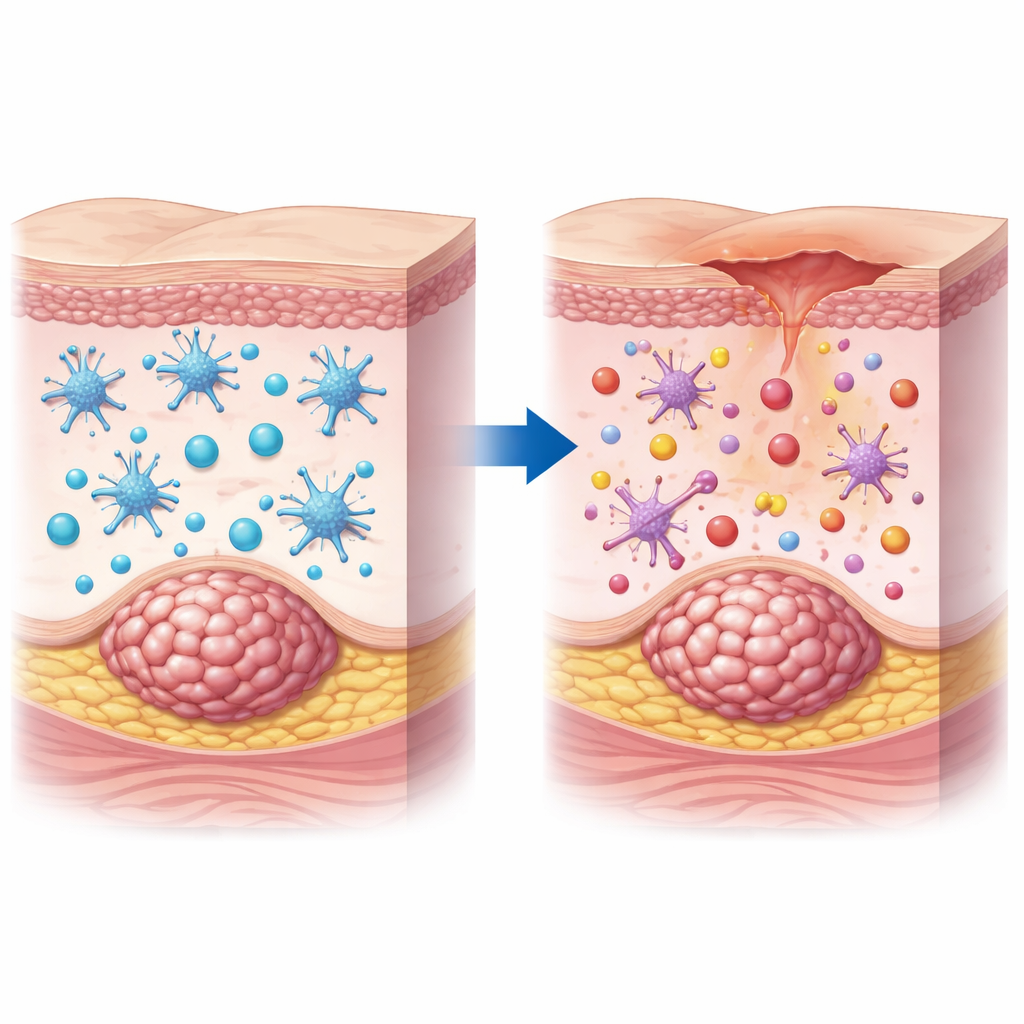
When immune teachers stop teaching
To move beyond appearances, the team isolated dendritic cells from patients’ lesional and non-lesional skin and examined which genes were turned on, and how well the cells worked in the lab. In the cancer-affected skin, dendritic cells dialed down genes needed to chop up and display tumor material to T cells. In dish experiments, these cells were worse at swallowing and processing test particles and were weaker at kick-starting T cells. T cells that had been “trained” by dendritic cells from diseased skin divided less and produced fewer toxic molecules, and they were less effective at killing tumor cells. In mice with breast cancer that spread into the skin, the same pattern emerged: fewer capable dendritic cells in the lesions, blunted ability to process danger signals, and a feeble T-cell attack.
A chemical fog that muffles alarm signals
What was silencing these immune sentinels? The researchers turned to the chemical environment inside skin lesions. By profiling small molecules in mouse tumors and measuring them in patient samples, they homed in on prostaglandin E2, a fatty messenger best known for driving pain and inflammation. Levels of this molecule were markedly higher in cancerous skin than in nearby unaffected areas. Importantly, when human dendritic cells were bathed in prostaglandin E2 in the lab, they lost their sharp edges: they showed lower activation, processed less material, and primed weaker T-cell responses. Tumor cell “broths” rich in prostaglandin E2 had the same dampening effect, even after being heated or treated to destroy proteins and genetic material, underscoring that a stable chemical factor was to blame.
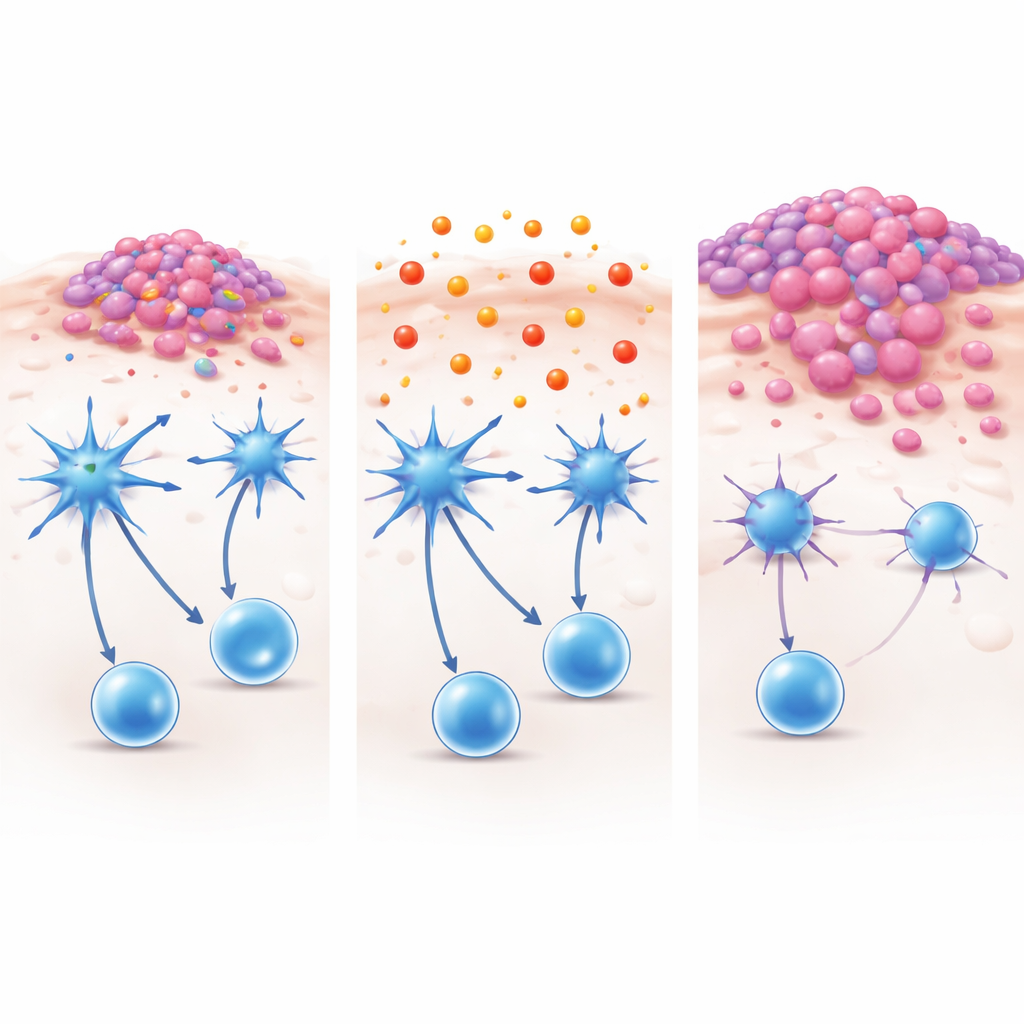
Blocking the brake and restoring the attack
The team then asked whether lifting this chemical brake could restore immunity. In mouse models of breast cancer and melanoma with skin involvement, drugs that blocked prostaglandin E2 signaling or shut down its production shrank or softened skin lesions. After treatment, more active dendritic cells and killer T cells moved into the skin, and these cells regained their ability to recognize and destroy tumor targets in laboratory tests. Notably, these drugs did not slow cancer cell growth directly in a dish, pointing instead to an immune-based effect. Analyses of large public cancer databases suggested that people with skin tumors rich in the gene signatures of active dendritic cells tend to live longer, and that higher activity of the enzymes that make prostaglandin E2 tracks with fewer and less functional dendritic cells.
What this means for patients with skin lesions
Taken together, the work paints a clear picture for non-specialists: in breast cancer that reaches the skin, a local chemical—prostaglandin E2—creates a fog that confuses the skin’s immune teachers. With fewer capable dendritic cells on duty, killer T cells never receive a strong lesson on what to attack, and skin tumors gain a foothold. By mopping up prostaglandin E2 or blocking its signals, at least in animals, the authors could wake up these immune guards and help them push back the cancer. While more clinical testing is needed, especially in people with breast cancer skin lesions, the study points to repurposing existing drugs that target this pathway as a promising strategy to strengthen the body’s own defenses right where the disease is most visible.
Citation: Wang, J., Zhong, X., Liu, X. et al. Prostaglandin E2 induces dendritic cell dysfunction in skin involvement of breast cancer. Cell Death Dis 17, 260 (2026). https://doi.org/10.1038/s41419-026-08519-1
Keywords: breast cancer skin involvement, dendritic cells, prostaglandin E2, tumor immune microenvironment, COX-2 inhibition