Clear Sky Science · en
ΔNp63α drives serine synthesis to promote carboplatin resistance in NSCLC
Why starving cancer cells of a “non‑essential” nutrient matters
Most of us think of cancer treatment in terms of powerful drugs that directly kill tumor cells. This study shows that what cancer cells eat can be just as important. The researchers discovered that certain lung cancers rewire how they make and use the amino acid serine, helping them survive the commonly used chemotherapy drug carboplatin. By understanding and targeting this hidden metabolic trick, doctors may one day make standard treatments work better—simply by combining drugs with changes in how tumors access specific nutrients.
A fuel line that feeds stubborn lung tumors
Lung cancer is the leading cause of cancer death worldwide, and non‑small cell lung cancer (NSCLC) makes up about 85% of cases. Within NSCLC, a subtype called lung squamous cell carcinoma (LUSC) has far fewer targeted treatment options than other forms and still relies heavily on carboplatin‑based chemotherapy. The authors focused on serine, an amino acid that cancer cells use as a building block for DNA, proteins, and fats, and as a key component of their antioxidant defenses. Although our bodies can make serine, aggressive tumors appear to boost both its production and uptake, suggesting they may be unusually dependent on this nutrient for growth and survival.
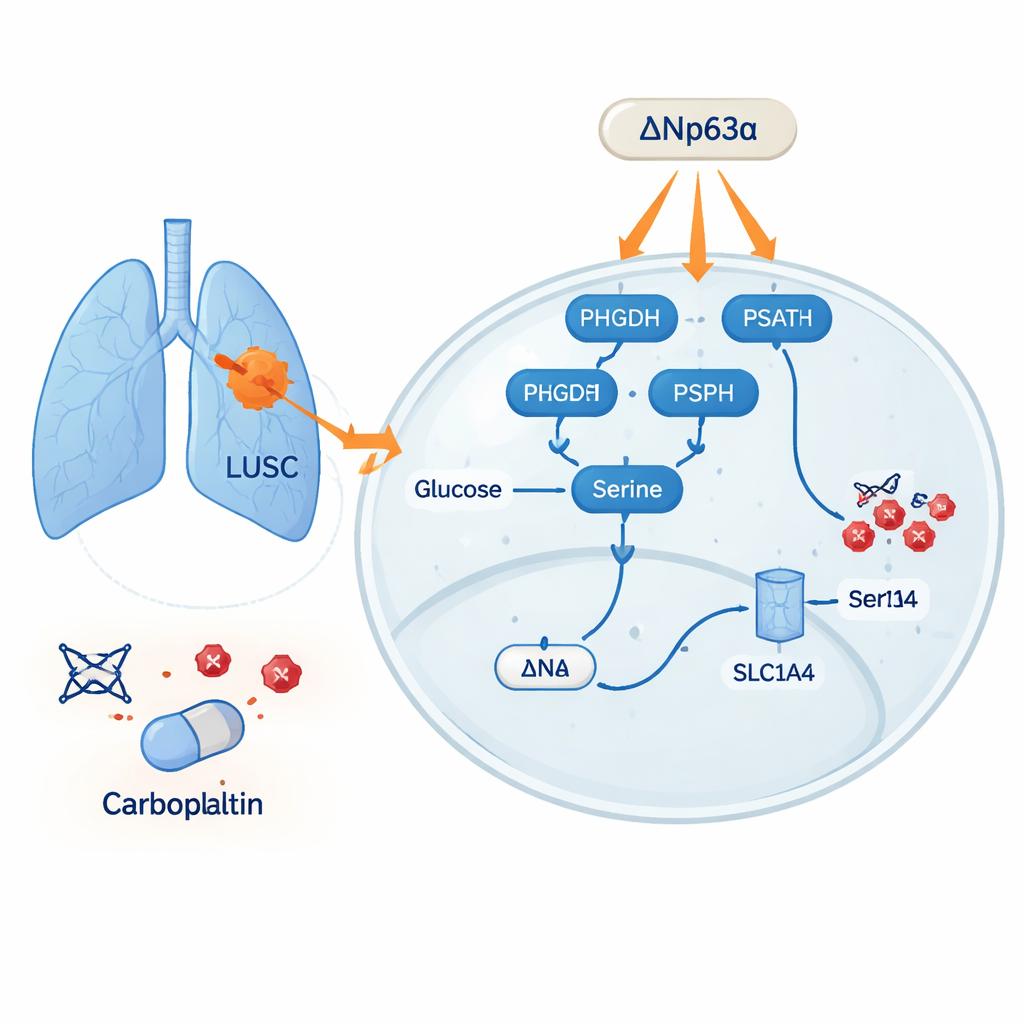
The metabolic pathway behind resistance
Using large patient datasets and tumor samples, the team showed that several proteins involved in making and importing serine—PHGDH, PSAT1, PSPH, and the transporter SLC1A4—are consistently elevated in lung cancers compared with normal lung tissue. High levels of these serine‑related genes were linked to worse survival. The effect was especially strong in LUSC, which had more of these enzymes and higher serine content than lung adenocarcinoma. In cell cultures, cancer cells with more serine were less sensitive to carboplatin, and adding extra serine helped them withstand the drug’s effects. In mice, tumors in animals fed a high‑serine diet resisted carboplatin, whereas tumors in mice on serine‑poor diets shrank more under the same treatment.
A lineage gene that turns serine production up to high
The researchers then asked why LUSC cells are so good at making serine. They homed in on ΔNp63α, a protein that acts as a “lineage” regulator in squamous cancers and is often used to diagnose LUSC. By mining public gene‑expression data and performing molecular experiments, they found that tumors with high ΔNp63α levels also showed high expression of the four key serine pathway genes. In cell lines, ramping up ΔNp63α increased the amount of serine inside cells, while reducing ΔNp63α lowered it. Further tests showed that ΔNp63α binds directly to the control regions of the serine pathway genes and switches them on, acting as a master dial that raises serine production and import in squamous lung cancer cells.
How extra serine shields cancer cells from chemotherapy
Carboplatin kills cancer cells mainly by damaging their DNA and increasing harmful oxygen‑based molecules called reactive oxygen species (ROS). Serine helps cells in two crucial ways: it supplies raw material for making DNA building blocks and fuels the production of glutathione, a major antioxidant that mops up ROS. When the scientists removed serine and its close relative glycine from cell culture media, carboplatin caused more DNA breaks and much higher ROS levels. Adding back formate (a product of serine used for DNA synthesis) or an antioxidant partially rescued the cells, and using both together nearly restored their survival. In squamous lung cancer cells that already make a lot of serine, blocking the enzyme PHGDH with a drug (NCT‑503) made carboplatin far more effective, both in dishes and in mouse tumors.
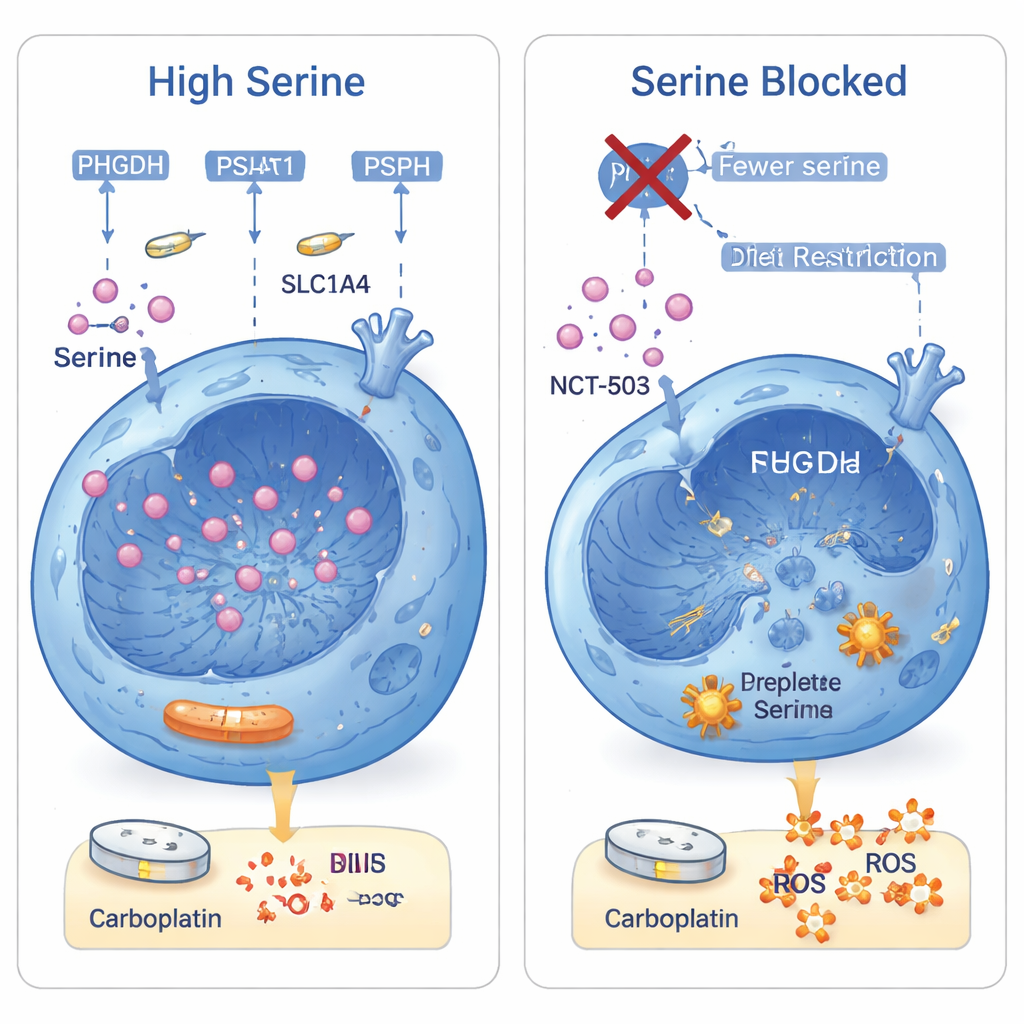
Turning a weakness into a treatment opportunity
To a lay reader, the key message is that some squamous lung cancers survive chemotherapy by overproducing a single amino acid, serine, under the control of the ΔNp63α gene. This extra serine lets tumor cells repair carboplatin‑induced DNA damage and neutralize toxic molecules that would otherwise kill them. The study shows that if you cut off both the internal “factory” that makes serine and the external “supply line” from diet, carboplatin works much better. In other words, by combining standard chemotherapy with drugs that block serine production and with carefully managed dietary approaches, doctors may one day outsmart a major resistance mechanism in a hard‑to‑treat form of lung cancer.
Citation: Deng, L., Yang, X., Zhang, J. et al. ΔNp63α drives serine synthesis to promote carboplatin resistance in NSCLC. Cell Death Dis 17, 227 (2026). https://doi.org/10.1038/s41419-026-08497-4
Keywords: serine metabolism, lung squamous cell carcinoma, carboplatin resistance, ΔNp63α, cancer metabolism therapy