Clear Sky Science · en
The breast cancer risk assessment pathway in England: a systems analysis of current challenges and ways to improve
Why this matters for women and families
Breast cancer touches many families, and a person’s chance of developing it can be higher because of their age, family history or other factors. In England, there are clear rules saying that women at higher risk under 50 should be offered extra checks and options to lower their risk. Yet this study shows that whether a woman actually receives this support often depends more on where she lives and how confident she feels about seeking help than on her medical need. Understanding how the current system works—and how it could work better—matters for anyone who wants earlier detection, fair access to care and fewer lives lost to breast cancer. 
How care is supposed to work today
The researchers spoke to 29 experts from across England, including GPs, surgeons, radiologists, genetics specialists, breast nurses and health planners. They mapped how a woman under 50 with no cancer, but with possible higher risk, currently moves through the system. Today, most women only enter the pathway if they visit their GP with worries about breast cancer in the family or breast symptoms. The GP may then record some family history and, if concerned, refer her to a family history clinic, a genetics service or a breast unit. There, staff can use risk tools that combine family history, genes and other factors to judge whether she is at average, moderate or high risk and to offer extra mammograms, other scans or risk-reducing medicines where appropriate.
When chance and postcode shape care
Although this pathway exists on paper, experts described it as fragmented and unfair in practice. Access to extra screening and risk-lowering medication was said to be a “postcode lottery”: services for women under 50 vary widely between regions, and in some areas are missing altogether. Even within the same region, care can be “patchy”, depending on which professional a woman happens to see. Many GPs lack time, confidence or up-to-date knowledge to assess risk or to prescribe preventive drugs. Because the system relies on women coming forward themselves, it tends to favour those who are better informed, more educated or fluent in English. Women from poorer backgrounds or minority communities are therefore less likely to be identified and supported, even when their medical risk is just as high.
What experts say needs to change
Across specialties, participants agreed that breast cancer risk assessment needs a more joined-up, proactive approach. They called for a national strategy so that women at moderate or high risk are identified and cared for in the same way wherever they live, with extra screening for these women formally built into the national breast screening programme. They also highlighted the potential of digital tools: for example, online family history forms, national hubs that use existing records to flag women at higher risk, and flexible ways to contact women, from text messages to phone helplines. Alongside this, family history clinics and genetics services were seen as the best places to carry out detailed risk assessments, while GPs would continue to play a key role in spotting women who might need referral. 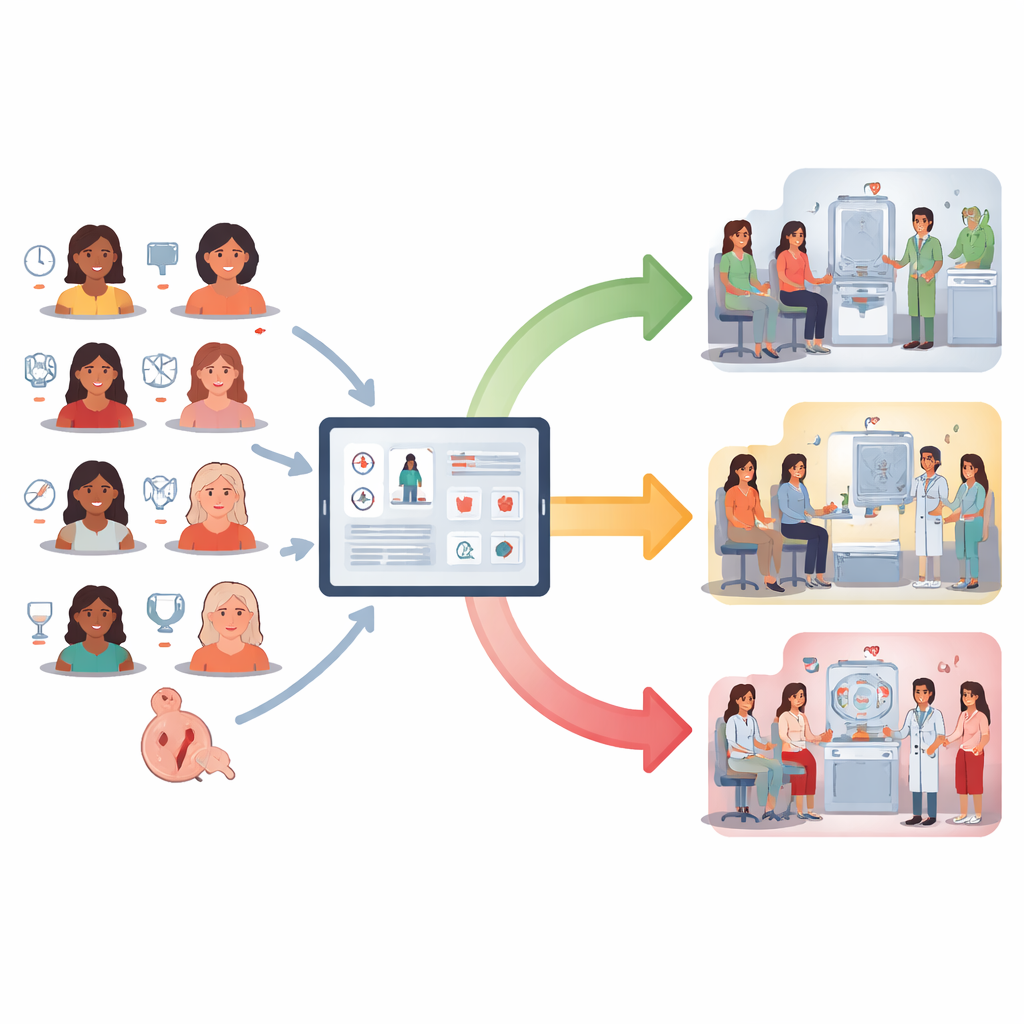
Building skills, funding and shared responsibility
Experts stressed that real change will require investment and clearer roles. Many said that family history clinics, screening services, genetics teams and breast units all need more staff and funding to handle a greater number of women if proactive risk assessment becomes routine. They also argued for better training so that GPs and hospital doctors who see women with breast symptoms can confidently recognise worrying family histories and talk about risk-reducing options, including medicines. Clear agreements are needed about who should start and monitor these drugs so that they do not fall into a “no-man’s land” between services. The study’s ten recommendations cover national planning, digital registers, new invitation routes, shared care for preventive medication and education for clinicians.
What this could mean for women’s futures
In simple terms, this study shows that England already has the tools to reduce breast cancer risk for many women under 50, but the system that should deliver them is uneven and reactive. By moving from a set-up that waits for women to ask for help to one that actively finds and supports those at higher risk, and by making services more consistent and better connected, the country could offer earlier checks and more effective prevention to many more people. For families, this would mean that a woman’s chances of getting the right advice and extra screening no longer depend on her postcode, background or confidence, but on her actual level of risk.
Citation: Valasaki, M., Taylor, L.C., Woof, V.G. et al. The breast cancer risk assessment pathway in England: a systems analysis of current challenges and ways to improve. Br J Cancer 134, 903–913 (2026). https://doi.org/10.1038/s41416-025-03329-2
Keywords: breast cancer risk, screening pathways, healthcare inequalities, genetic counselling, preventive medicine