Clear Sky Science · en
Efficacy and safety of low- and high-intensity focused ultrasound in glioblastoma: a systematic review of preclinical and clinical studies
Breaking Through the Brain’s Defenses
Glioblastoma is one of the deadliest brain cancers, in part because it hides behind the brain’s natural shield—the blood–brain barrier—that keeps many drugs out. This review article looks at a new way to reach and attack these tumors without opening the skull: carefully focused sound waves. By comparing dozens of animal experiments and early human trials, the authors explore how two types of focused ultrasound might team up to deliver medicines more effectively and even burn away parts of the tumor.
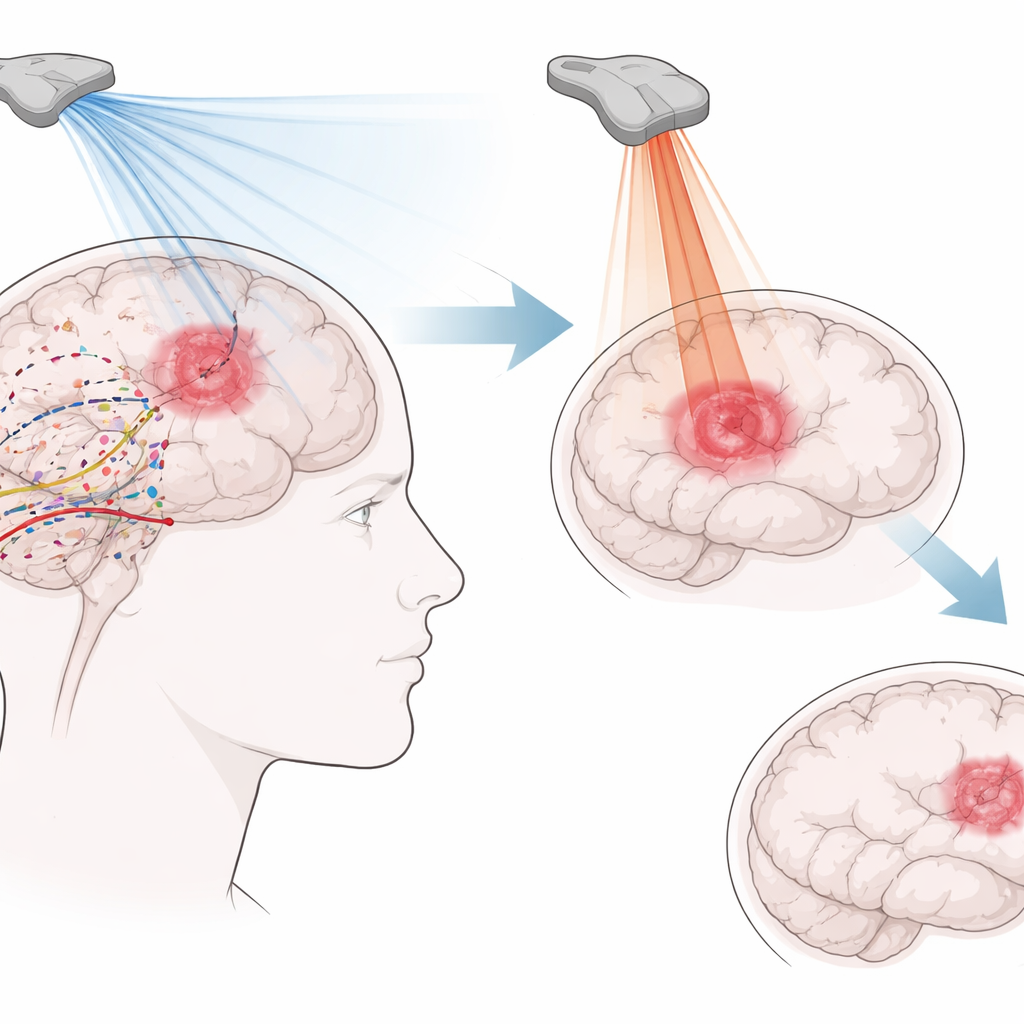
Why This Brain Cancer Is So Hard to Treat
Standard care for glioblastoma combines surgery, radiation, and chemotherapy, yet most patients survive little more than a year. The tumor spreads like roots through the brain, making complete removal almost impossible. At the same time, the blood–brain barrier, which normally protects our brains, blocks many cancer drugs from reaching stray cells that remain after surgery. The tumor’s surroundings are also hostile to the immune system, with few cancer-fighting T cells and many immune cells that actually help the cancer grow. These overlapping obstacles explain why even powerful new drugs often fail once they reach the brain.
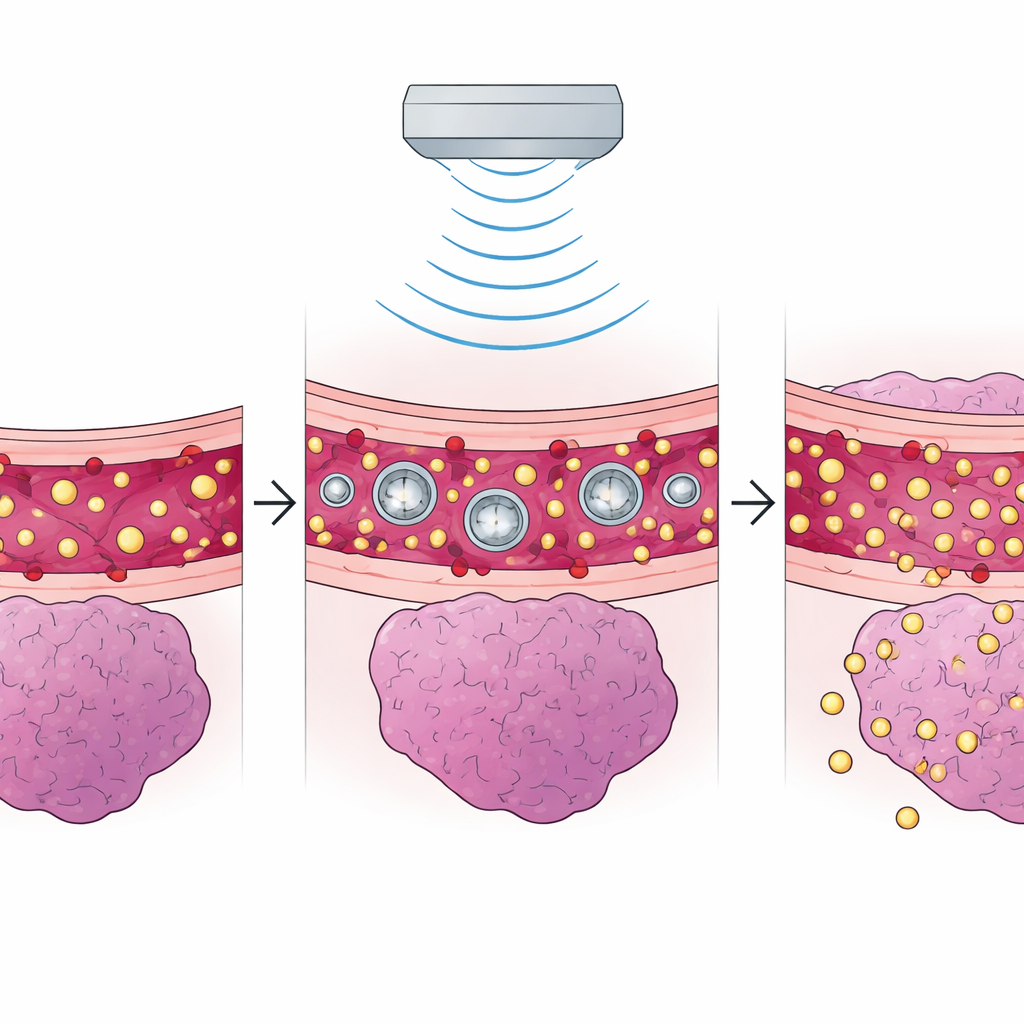
Gentle Sound to Open the Brain’s Gate
Low‑intensity focused ultrasound takes advantage of tiny gas bubbles injected into the bloodstream. When sound waves pass through, these bubbles gently vibrate and nudge apart the tightly sealed cells that line brain blood vessels. In animal studies, this temporary “loosening” allowed far more chemotherapy drugs, immune therapies, and even gene‑carrying particles to enter tumors. Many experiments saw tumors shrink and survival stretch from roughly three to four weeks up to six to eleven weeks. Early clinical trials echo these patterns: using this approach alongside standard drugs such as temozolomide or carboplatin reliably opened the barrier, increased drug levels in treated brain regions, and produced progression‑free periods of a few months, with one small group showing all patients alive at one year.
Turning Sound into a Precise Heat Knife
High‑intensity focused ultrasound works differently. Here, stronger sound waves are concentrated on a small target, heating tissue enough to kill cancer cells outright. In animal models, pairing this stronger ultrasound with drug‑filled particles or contrast agents often cut tumor growth by about 70 percent and improved survival, without damaging nearby organs. In people, however, results have been more modest so far. One carefully monitored case achieved only about a tenth of the tumor volume destroyed, and another early trial reached therapeutic temperatures without visible tumor shrinkage. The skull’s tendency to bend and absorb ultrasound energy, and the diffuse spread of glioblastoma cells beyond a clear lump, make this heat‑based approach technically demanding.
Safety, Limits, and What Comes Next
Across 40 studies, both approaches appeared remarkably safe when used with care. Low‑intensity treatments caused mostly mild, short‑lived effects such as headaches, tiny pinpoint bleeds visible only on scans, or temporary sensations like tingling or warmth. The blood–brain barrier generally resealed within a day, and no lasting brain damage was reported. High‑intensity treatments produced brief warmth or discomfort but no serious bleeding or permanent deficits in the small number of patients treated so far. Still, the evidence base is uneven: most animal studies lacked full blinding or randomization, and most human data come from small, non‑randomized trials in wealthy countries, making it hard to draw firm conclusions.
What This Means for Patients and Families
The article concludes that low‑ and high‑intensity focused ultrasound are promising, complementary tools rather than stand‑alone cures. Low‑intensity ultrasound is closest to real‑world use: it can repeatedly and reversibly open the brain’s gate so more medicine and immune cells reach hidden tumor pockets. High‑intensity ultrasound may one day help burn away well‑defined tumor cores, especially when combined with better drug delivery. However, neither method is ready to replace surgery, radiation, or chemotherapy. Large, carefully controlled trials—ideally run across many centers and using standardized treatment settings—are still needed to prove whether these sound‑based strategies can meaningfully extend life and preserve quality of life for people facing glioblastoma.
Citation: Alrashidi, M., Ferro, F., Almohammadi, A. et al. Efficacy and safety of low- and high-intensity focused ultrasound in glioblastoma: a systematic review of preclinical and clinical studies. Br J Cancer 134, 977–995 (2026). https://doi.org/10.1038/s41416-025-03325-6
Keywords: glioblastoma, focused ultrasound, blood–brain barrier, brain tumor therapy, noninvasive oncology