Clear Sky Science · en
Autonomic cardiovascular mechanisms linked to stress in dental practice
Why the Dentist Can Make Your Heart Race
Many people dread a visit to the dentist. The whine of the drill, the sight of a needle, or memories of past pain can make palms sweat and hearts pound. This article explains why those reactions are more than simple nerves. It explores how stress in the dental chair activates brain circuits that drive the heart and blood vessels, and how, in vulnerable people, this surge of activity can tip over into dangerous rhythm problems or sudden spikes in blood pressure.
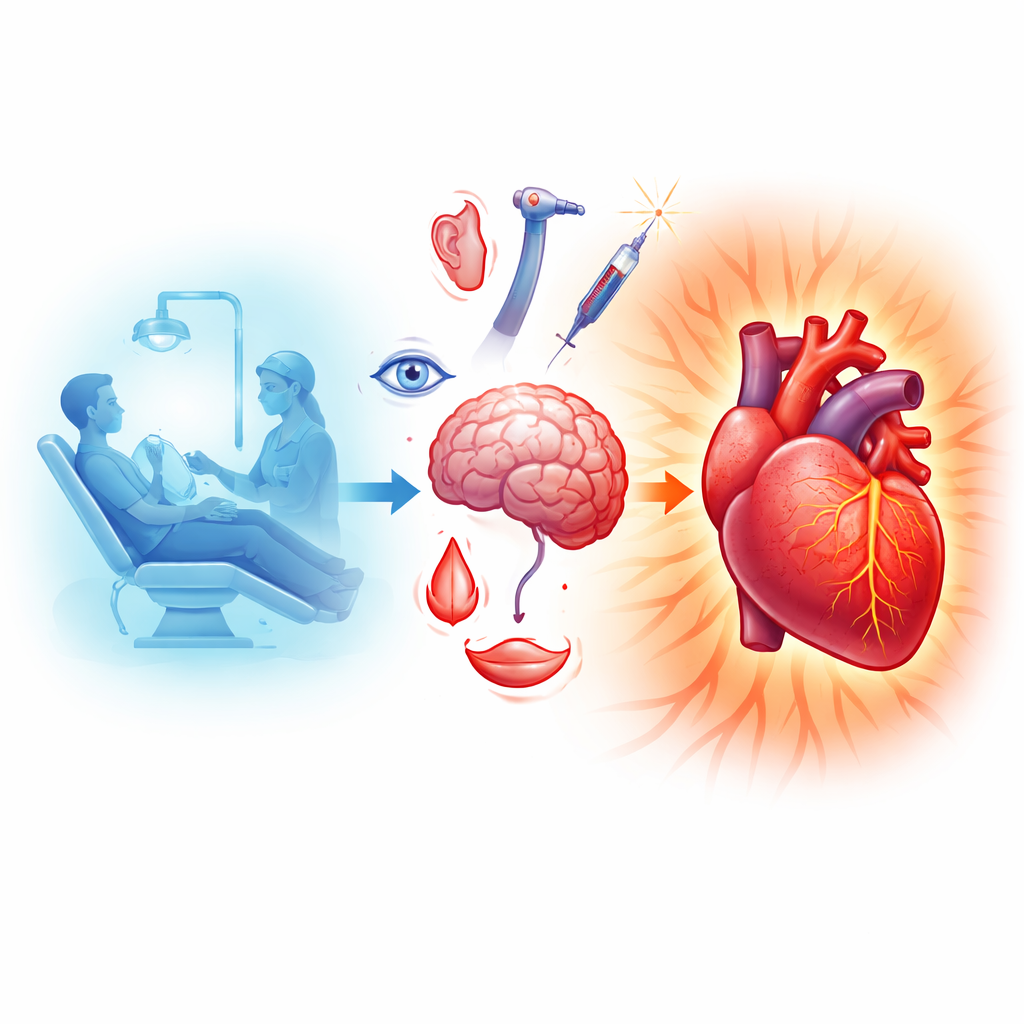
Everyday Worry, Hidden Heart Strain
Stress and anxiety are not just emotions; they are whole‑body events. When we feel threatened, the “fight‑or‑flight” system raises heart rate and blood pressure to prepare us for action. In dental practice, the triggers are everywhere: noise from the drill, bright lights, chemical smells, the taste of medicines, the feel of instruments, and of course pain. The article shows that both actual pain and simple anticipation—worrying at home or in the waiting room—are enough to boost the body’s stress signals. Surveys reveal that a large share of adults, and many children, report strong dental anxiety, and a smaller group develop full-blown dental phobia, avoiding care altogether. Even before treatment starts, these patients often arrive with elevated heart rate and tense circulation.
From Normal Fear to Problem Anxiety
Fear itself is not harmful; it is a normal response that helps us avoid danger. The trouble begins when ordinary fear hardens into chronic anxiety or phobia. The paper explains how bad experiences at the dentist, frightening stories from parents, or observing a caregiver’s distress can all condition a person to react strongly to the dental setting. Over time, this can produce a persistent state of alarm, with people becoming hyper‑alert, over‑reactive to small triggers, and unable to calm down. In such states, the body’s stress wiring—especially the “sympathetic” nerves that speed the heart and tighten blood vessels—stays overactive. This long‑lasting tension has been linked to high blood pressure, disturbed heart rhythms, and even stress‑induced heart muscle weakness.
How the Brain Turns Dental Stress into Heart Action
At the core of the article is a model of how signals from the mouth and from our senses converge in the brain and then drive the heart. Pain from a tooth or needle travels along nerves in the face and jaw into brainstem hubs that regulate circulation. There, it can activate a powerful built‑in reflex that boosts nerve firing to the heart and blood vessels, producing spikes in blood pressure and heart rate. Separately, sights, sounds, and smells of the clinic travel to higher brain regions involved in emotion and body awareness. In a key region called the insular cortex, information about the outside world and the beating heart is combined, shaping how strongly we “feel” our own palpitations. This region talks to deeper centers that command the sympathetic nerves, sending strong signals down to the heart. The article argues that when pain and emotional context hit these pathways at the same time, the result can be an exaggerated cardiovascular response.
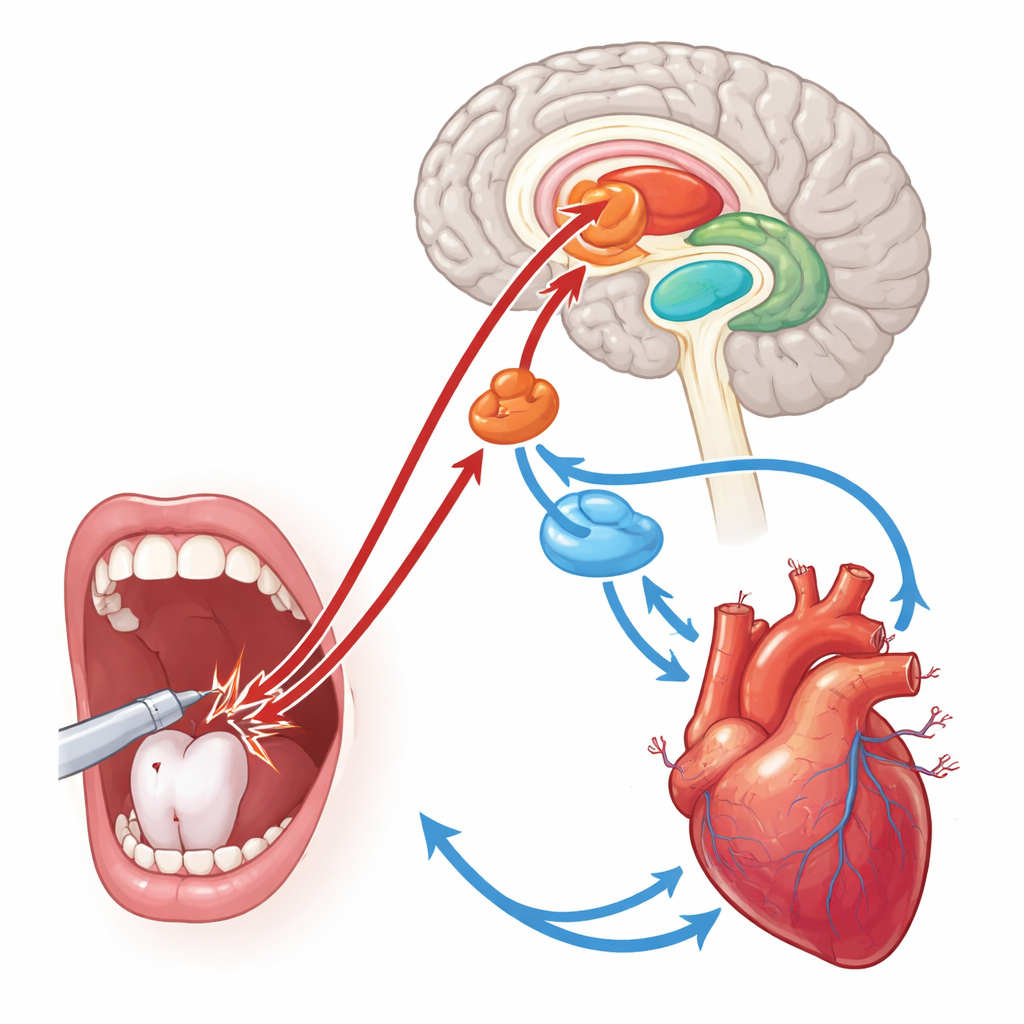
When a Racing Heart Feeds the Fear
The authors also highlight an important feedback loop. Once the heart is beating fast and forcefully, signals from the heart itself travel back to the brain, where they are sensed and interpreted. People who are already anxious may notice their pounding heart and interpret it as a sign of danger, which further heightens fear. This, in turn, further activates the sympathetic nerves, creating a vicious cycle of rising anxiety and rising cardiovascular strain. Case reports from dental clinics describe patients developing serious rhythm disturbances, and even a form of stress‑induced heart failure, around the time of seemingly routine procedures, sometimes before any drilling or cutting begins.
Helping Patients Stay Calm and Safe
In closing, the article stresses that dentists and dental teams need to recognize that emotional stress in the chair is also a cardiovascular challenge. Because the same nerve groups in the brainstem and higher centers respond to both pain and fear, dental care can, in some people, unintentionally drive the heart hard enough to provoke dangerous events. While medicines such as sedatives and certain heart drugs can help some patients, they are not a complete answer and may have side effects. Psychological and comfort‑based approaches—such as clear communication, relaxation techniques, distraction with music or virtual reality, and careful pain control—can reduce both fear and strain on the heart. Understanding the brain–heart links behind dental stress can help clinicians tailor care, making visits safer and more tolerable for anxious patients.
Citation: De Felice, M., de Carvalho Moreno das Neves, V., Almeida-Leite, C. et al. Autonomic cardiovascular mechanisms linked to stress in dental practice. Br Dent J 240, 395–402 (2026). https://doi.org/10.1038/s41415-025-9459-8
Keywords: dental anxiety, stress and heart, autonomic nervous system, cardiac arrhythmias, pain and fear