Clear Sky Science · en
Evaluation of postoperative pain after endodontic treatment in molars with and without foraminal enlargement: a prospective randomized clinical trial
Why Root Canal Pain Matters
Many people dread root canal treatment because they fear the pain that might follow. Dentists share this concern: easing infection while keeping patients comfortable is a central goal in modern care. This study looks at a specific step in root canal therapy—how far instruments go toward the tip of a tooth’s root—and asks a simple but important question: does going a bit farther make patients hurt more afterward?
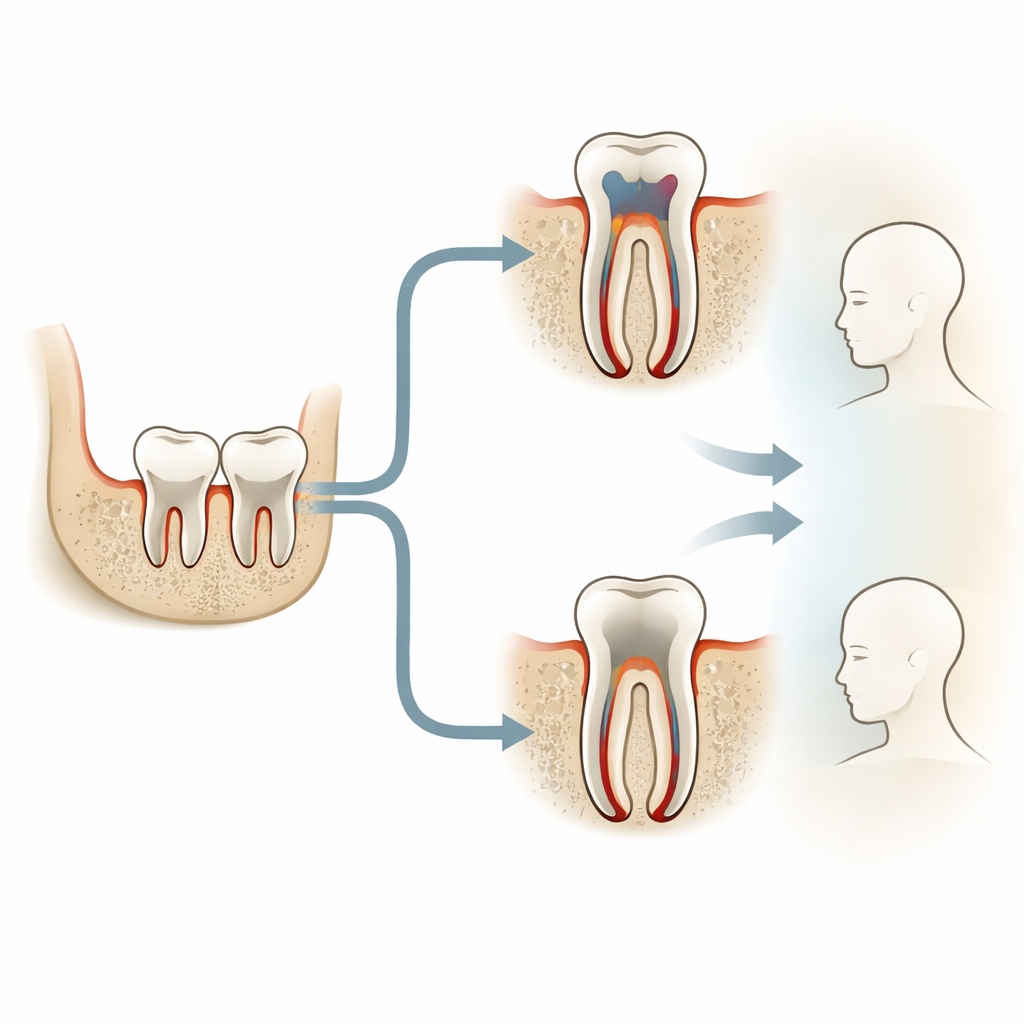
Two Ways to Clean a Sick Tooth
When the soft tissue inside a tooth dies and infection spreads to the tip of the root, dentists remove the damaged material, disinfect the space, and seal it. Some specialists advocate cleaning right up to the natural opening at the root tip, slightly widening it to better flush out bacteria. Others prefer to stop just short of that opening, hoping to avoid irritating the tissues around the end of the root. Both methods are used in everyday practice, but there has been debate about whether the more aggressive approach increases pain after treatment.
How the Study Was Done
The researchers ran a randomized clinical trial with 60 adults who all needed root canal treatment on lower back molars that had dead pulp and signs of infection at the root tip. Everyone was treated in a single visit by the same experienced specialist, using the same modern reciprocating instrument system and the same disinfecting solutions and filling materials. The only difference was how far the main instrument was taken into the canal: in one group, it reached all the way to the root’s natural opening; in the other, it stopped about one millimeter short. Patients did not know which method they received, and they were carefully screened so that other sources of facial pain would not confuse the results.
Tracking Pain After Treatment
After their appointment, participants rated their pain at 24, 48, and 72 hours, and again at one week, using a standard visual scale that grouped pain into none, mild, moderate, or severe. They also recorded whether they took pain medicine and how many tablets they used. The study found that, in both groups, pain levels were generally low and short lived. A small number of people in each group reported mild or moderate discomfort in the first day or two, and a few in the more aggressive cleaning group had stronger pain early on. However, by 72 hours and at one week, nobody in either group reported any pain. The number of pain pills taken was also low overall and did not differ in a meaningful way between the two methods.
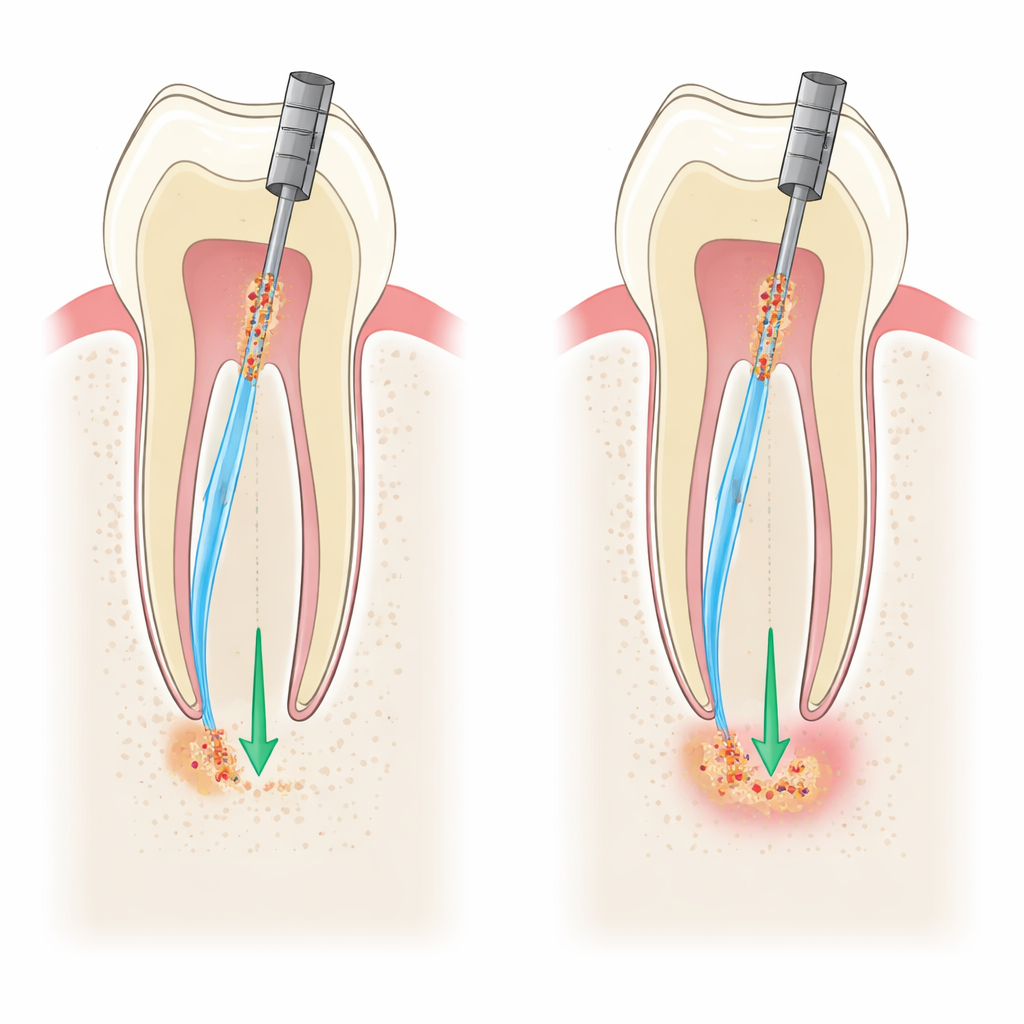
What This Means for Patients and Dentists
The results suggest that, when carried out carefully with modern tools and techniques, cleaning all the way to the root tip versus stopping slightly short does not noticeably change how much pain patients feel after a molar root canal. Both approaches led to similar levels of comfort and similar use of pain medication in the days following treatment. For dentists, this means they can base their choice of technique on other factors—such as how best to remove bacteria and protect long-term healing—without expecting a large difference in short-term discomfort. For patients, it offers reassurance that root canals on back teeth, even when thoroughly cleaned, do not usually result in severe or lasting pain when performed under controlled conditions.
Citation: de Aragão, F.M.G., Bueno, C.E.d.S., Pelegrine, R.A. et al. Evaluation of postoperative pain after endodontic treatment in molars with and without foraminal enlargement: a prospective randomized clinical trial. BDJ Open 12, 24 (2026). https://doi.org/10.1038/s41405-026-00412-5
Keywords: root canal pain, endodontic treatment, foraminal enlargement, mandibular molars, postoperative discomfort