Clear Sky Science · en
Effect of 980 nm diode laser irradiation in comparison with conventional irrigation on smear layer removal from radicular dentin—an in vitro experimental study
Why Cleaner Root Canals Matter
Root canal treatment has a reputation for being unpleasant, but when it works well it can save a tooth that would otherwise be lost. One of the hidden challenges is making sure the inside of the tooth is truly clean so that leftover germs do not cause future pain or infection. This study explores whether a specific dental laser, used at a wavelength of 980 nanometers, can clean the tiny inner channels of teeth more effectively than the standard chemical rinses dentists have relied on for decades.
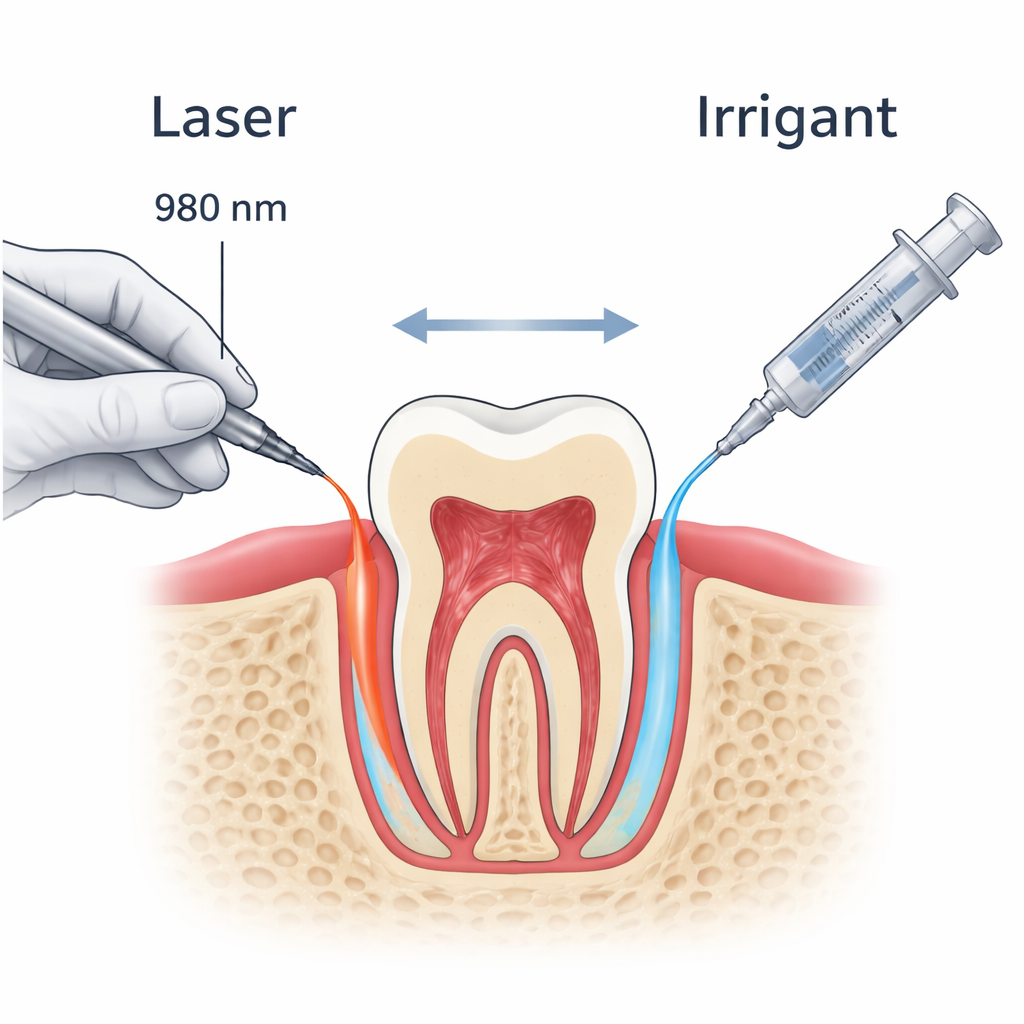
The Hidden Film Inside a Tooth
When dentists shape and clean the inside of a damaged tooth during a root canal, their tools create a microscopic “smear layer.” This film is made of ground-up dentin (the hard tissue beneath enamel), bits of pulp tissue, and bacterial by-products. It can clog the tiny side channels, called dentinal tubules, that branch out from the main root canal. If these tubules are sealed by this film, disinfecting liquids, sealers, and filling materials cannot reach deeper layers where bacteria may still lurk. Over time, these hidden germs can lead to persistent infection and treatment failure, even when the main canal looks clean on X‑rays.
Old vs. New Ways to Clean
The standard way to deal with this smear layer is to flush the canals with chemical solutions. Sodium hypochlorite, a bleach-like liquid, can dissolve organic material and kill bacteria, while a second solution called EDTA helps dissolve mineral components. Used together, they can open tubules and improve cleaning—but their effectiveness depends heavily on how strong they are, how long they are used, and how well they reach the full length of the canal. In recent years, dentists have begun testing lasers as another way to improve cleaning. Diode lasers, including those that operate at 980 nanometers, can send energy into the fluids and tissue inside the canal, potentially loosening or altering the smear layer without cutting the tooth itself.
Putting the Laser to the Test
To compare these approaches, the researchers used 66 extracted human teeth with a single straight root. They prepared each tooth as if performing a real root canal, then randomly assigned it to one of two groups. In the first group, a very thin fiber from a 980 nm diode laser was placed nearly to the tip of the root and moved in a slow, spiraling motion along the canal wall, with short bursts of energy and cooling pauses to avoid overheating. In the second group, the canals were rinsed the conventional way with 3% sodium hypochlorite followed by 17% EDTA. After treatment, all the teeth were soaked in a blue dye solution for 48 hours. The roots were then cut into thin slices at three different levels—near the crown, the middle, and the tip—and examined under a microscope. Using imaging software, the team measured how far and how widely the dye had penetrated into the dentin, which reflects how open and permeable the tubules had become.
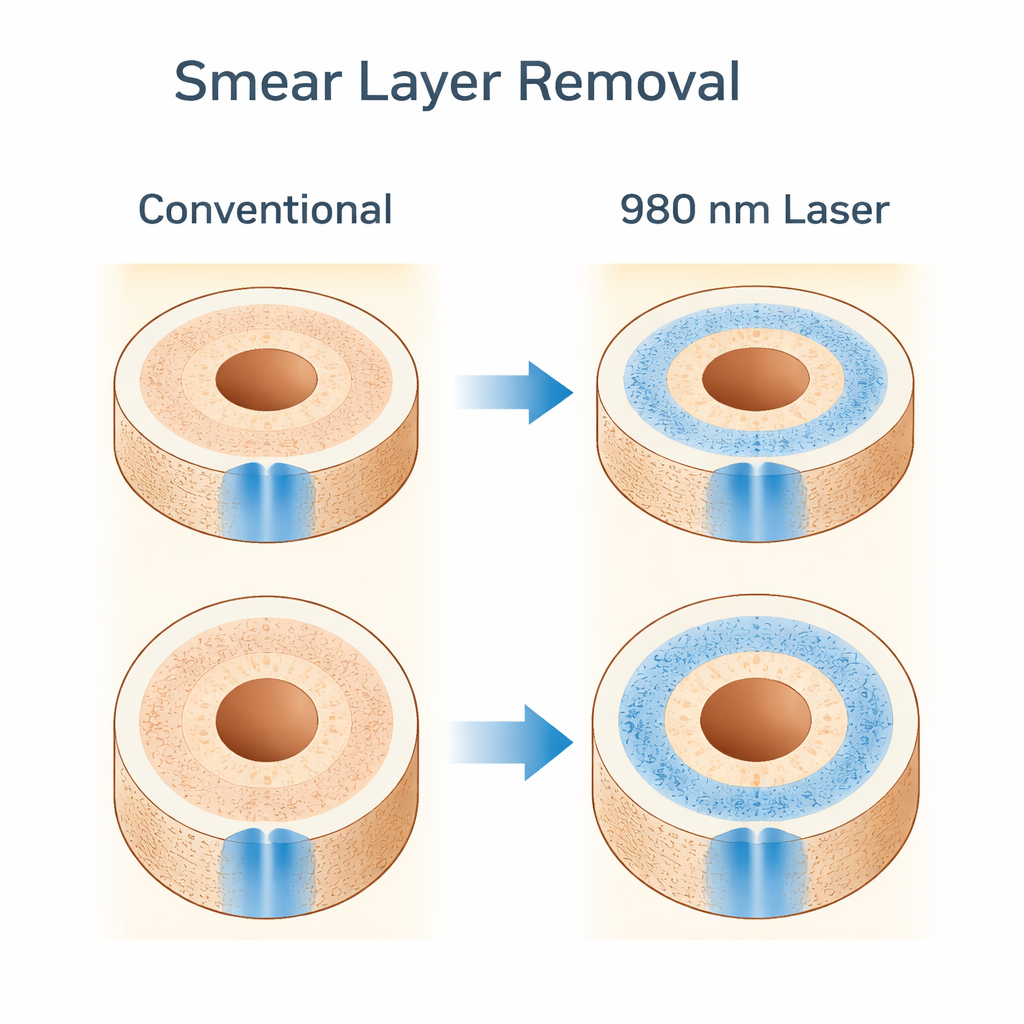
What the Dye Revealed
The laser-treated teeth showed much deeper and broader dye penetration than those treated with chemicals alone, at every level of the root. On average, the diameter and area covered by the dye were several times greater in the laser group, especially in the upper part of the root where tubules are naturally wider and more numerous. Even in the narrow, more mineralized tip region—traditionally the hardest part to clean—the laser group still outperformed the conventional rinses. The authors suggest that the laser’s energy, absorbed by the liquid inside the canal, produces both heat and microscopic pressure waves. Together, these effects can partly vaporize or disrupt the smear layer, open more tubules, and allow fluids to travel further into the tooth. At the same time, the chosen settings aim to minimize the risk of overheating or damaging the dentin.
What This Means for Patients
For people facing a root canal, the study’s message is that technology like a 980 nm diode laser may help dentists clean more thoroughly in places that are hard to reach with chemicals alone. More open dentinal tubules and better fluid penetration could mean fewer surviving bacteria and a lower chance of infection returning. However, the work was done in a laboratory using extracted teeth, so it cannot yet prove better long-term outcomes in real patients. The authors conclude that diode laser treatment should be seen as a promising extra tool, not a replacement for careful chemical cleaning and skilled technique. Future clinical studies will need to confirm whether these microscopic advantages translate into more comfortable, longer-lasting root canal treatments in everyday practice.
Citation: Tanveer, S.A., Ghafoor, R. & Omerson, A. Effect of 980 nm diode laser irradiation in comparison with conventional irrigation on smear layer removal from radicular dentin—an in vitro experimental study. BDJ Open 12, 20 (2026). https://doi.org/10.1038/s41405-026-00409-0
Keywords: root canal, dental laser, smear layer, endodontic disinfection, tooth irrigation