Clear Sky Science · en
Assessment of the dentine microhardness following the application of different intracanal medicaments. An in-vitro study
Why This Matters for Your Teeth
Root canal treatment is often seen as the last chance to save a badly damaged tooth. While dentists use powerful medicines inside the cleaned root to kill bacteria and help healing, these same substances can unintentionally weaken the tooth from the inside. This study explores which commonly used root canal medications best protect the inner hard layer of the tooth—called dentine—so that treated teeth stay strong and less likely to crack or break over time.
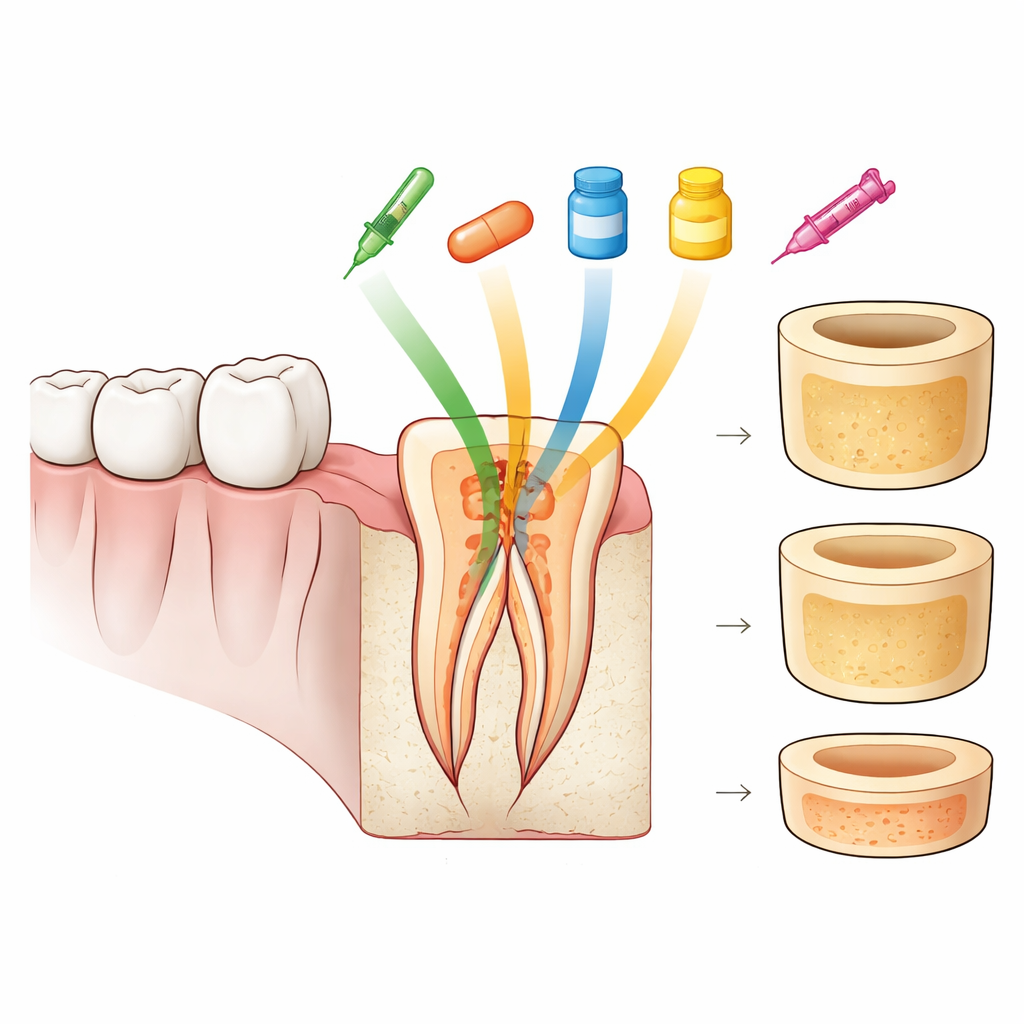
Keeping a Treated Tooth Strong
For a root canal to last, two things must happen: germs inside the root must be wiped out, and the remaining tooth structure must stay mechanically sound. If the dentine becomes softer, fillings and sealing materials do not grip as well, and the root can become more prone to fracture. Many medications can disinfect the canal, but they may also erode minerals or damage the tooth’s internal framework. The authors focused on a simple but telling measure—"microhardness," essentially how resistant the dentine is to being indented—as a stand‑in for overall strength.
Five Medicines Put to the Test
The researchers collected forty‑five single‑rooted human teeth that had been removed for reasons unrelated to decay in the root. They cut the teeth to a standard length and prepared the root canals the way a dentist would during normal treatment. The teeth were then randomly divided into five groups, each receiving a different medication inside the canal for two weeks: a modern calcium‑silicate paste (Bio‑C Temp), ultra‑thin antibiotic‑loaded fibers (modified triple antibiotic nanofibers, or m‑TAP), a broad‑spectrum antibiotic gel (Levofloxacin), a long‑used classic material (calcium hydroxide), and a cholesterol‑lowering drug repurposed for dental use (Simvastatin). After removing the medications, the team measured how hard the dentine was in three zones along the root—near the crown (coronal), in the middle, and near the tip (apical)—using a precise indentation device.
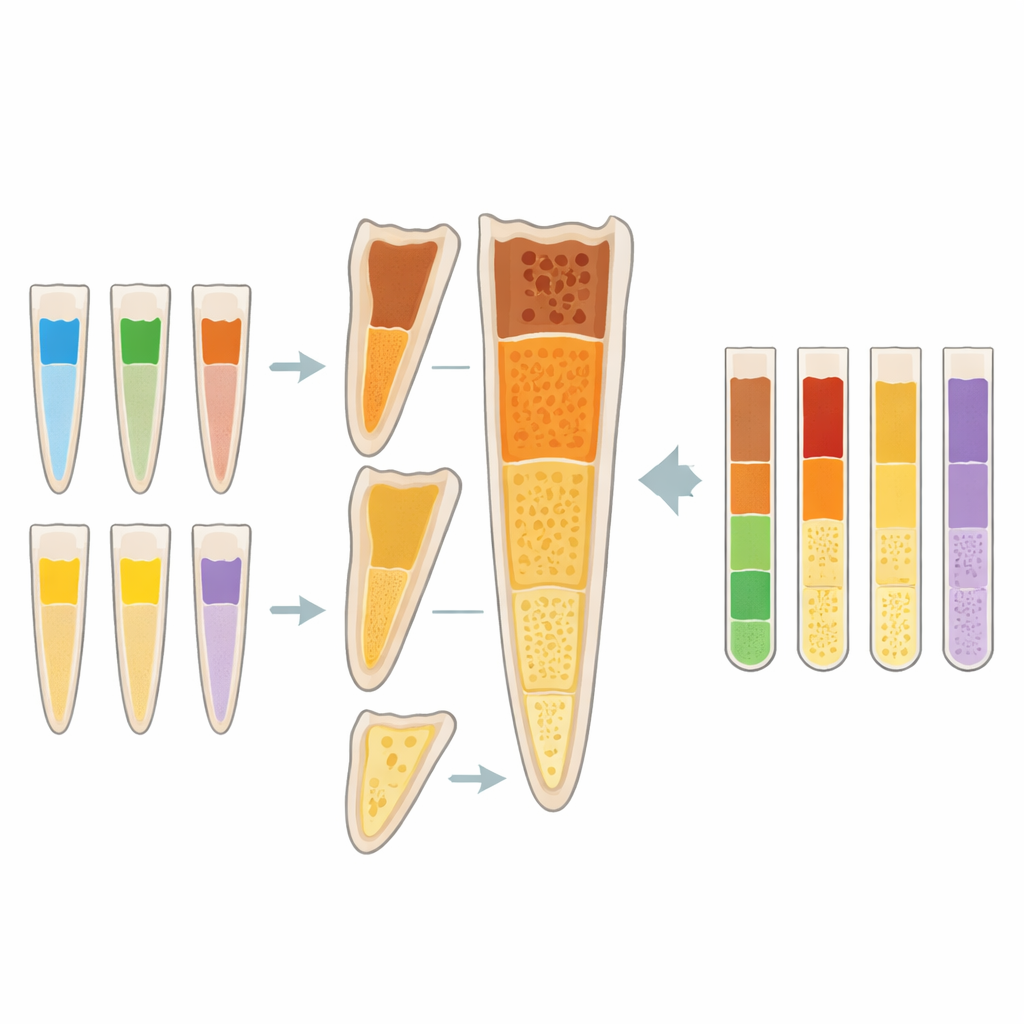
What Happened Inside the Roots
Bio‑C Temp and the antibiotic nanofibers led the pack, showing the highest dentine hardness overall, especially in the coronal and middle parts of the root. Levofloxacin and Simvastatin produced mid‑range results: they did not perform as well as the two front‑runners, but they were clearly better than the weakest option. Calcium hydroxide—the long‑standing workhorse in many dental practices—consistently gave the lowest hardness values, indicating more softening of the dentine. Interestingly, near the very tip of the root, all five medications produced similarly reduced hardness, suggesting that this region tends to be more fragile regardless of what is used, likely due to natural anatomical differences and limited penetration of materials.
Why Some Options Performed Better
The superior performance of Bio‑C Temp appears to stem from its calcium‑silicate base, which can release ions that encourage new mineral deposits within the tiny channels of dentine, helping to rebuild and stiffen the tissue rather than break it down. The nanofiber antibiotic system achieves strong antibacterial action at very low drug concentrations, which may limit the acid‑driven mineral loss sometimes seen with traditional antibiotic pastes. By contrast, calcium hydroxide’s high alkalinity can disturb the collagen framework that holds dentine minerals together, gradually weakening the internal structure. The mixed results for Levofloxacin and Simvastatin reflect the limited evidence so far: antibiotics can erode tooth minerals if too acidic, while Simvastatin may support mineral formation but did not match the best‑performing materials in this short‑term test.
What This Means for Patients
Overall, the study shows that not all root canal medications are equally kind to the tooth’s inner strength. The authors reject the idea that these materials have similar effects: Bio‑C Temp and antibiotic nanofibers did the best job of preserving hardness, while calcium hydroxide softened dentine the most. For patients, this means that newer materials may offer a better balance between killing germs and keeping the tooth strong enough to last. Although more research is needed—especially long‑term studies that mimic real chewing forces—these findings suggest that careful choice of intracanal medication could reduce the risk of future root fractures and help root‑treated teeth serve comfortably for many years.
Citation: Elgamal, S.G., Aly, K.H.A. & Hosny, N.S. Assessment of the dentine microhardness following the application of different intracanal medicaments. An in-vitro study. BDJ Open 12, 23 (2026). https://doi.org/10.1038/s41405-026-00408-1
Keywords: root canal treatment, dentin strength, intracanal medicaments, calcium silicate paste, dental nanofibers