Clear Sky Science · en
Linking lungs and gums: a meta-analysis of periodontitis prevalence and severity in chronic obstructive pulmonary disease
Why your gums might matter to your breathing
Most people think of brushing and flossing as a way to protect their smile, not their lungs. But growing research suggests that unhealthy gums may be linked with chronic obstructive pulmonary disease (COPD), a serious lung condition that makes it hard to breathe. This article pulls together data from dozens of studies to ask a simple yet important question: do people with COPD also tend to have worse gum disease, and if so, what might that mean for everyday health?
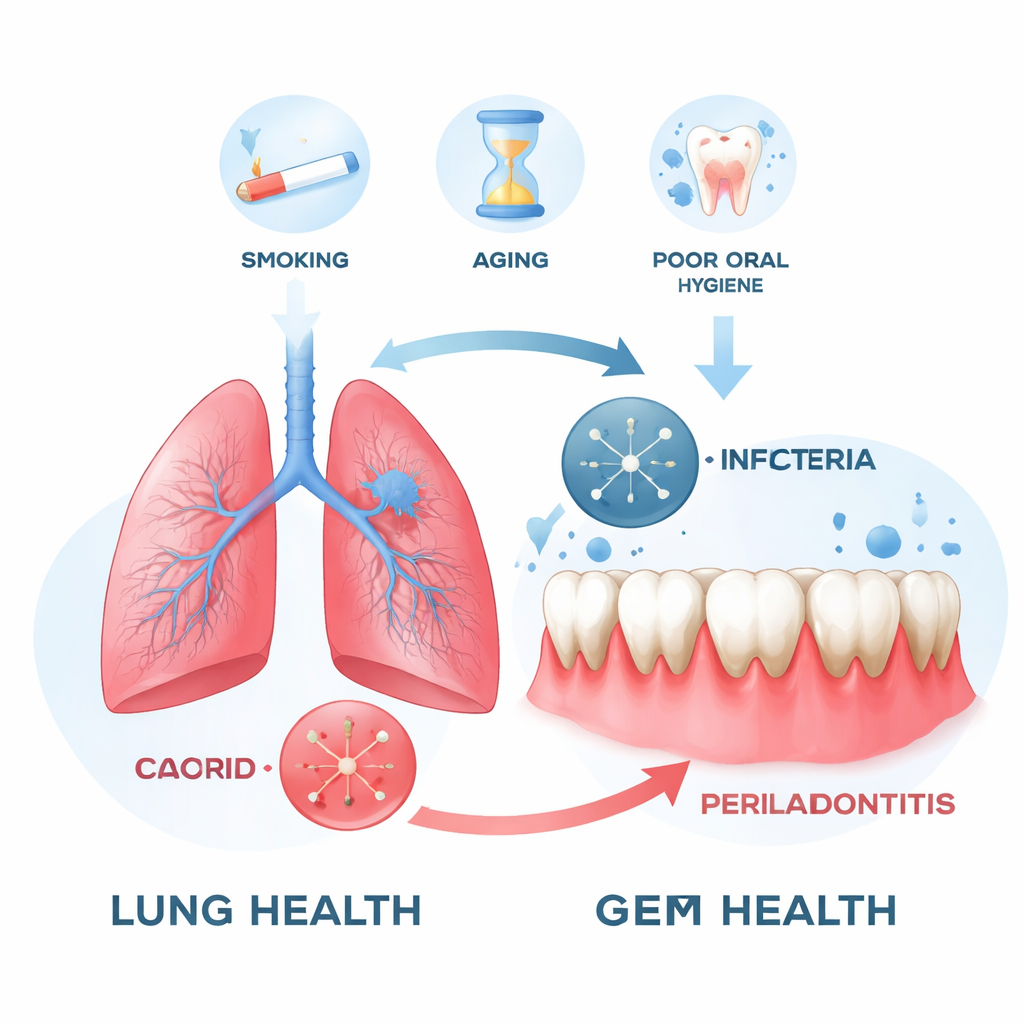
Two common diseases that quietly steal health
COPD is a long‑term lung disease marked by chronic cough, phlegm, and shortness of breath, affecting roughly one in ten adults worldwide. Periodontitis, a deep infection of the tissues that hold teeth in place, is just as widespread: about six in ten adults have some form of it, and severe cases affect nearly a quarter of the population. Both conditions can reduce quality of life and share many risk factors, including smoking, older age, poor access to care, and chronic illnesses such as diabetes. Scientists have also learned that bacteria from infected gums can enter the bloodstream or be inhaled into the airways, potentially fueling inflammation far beyond the mouth.
How the researchers combined the evidence
To understand the link between lungs and gums, the authors systematically searched major medical databases for clinical studies that measured gum health in people with COPD. They included 41 observational studies from around the world, covering more than 18,000 patients. To make fair comparisons across studies that used slightly different measurement methods, they focused on standard gum health indicators: how many people had periodontitis, how deep the pockets were between tooth and gum, how much tooth‑supporting tissue had been lost, and how often gums bled when gently probed. Using statistical techniques designed for combining many independent studies, they calculated average patterns and checked how sensitive the results were to any single study or to missing data.
What they found in the numbers
Across the included studies, about 35% of people with COPD had periodontitis, and moderate or severe disease was common. When COPD patients were directly compared with people without COPD, those with lung disease were more likely to have periodontitis, showing roughly one‑and‑a‑half times higher odds in the main analysis. On average, their gums had deeper pockets and greater loss of the tissue anchoring teeth in place, and their gums bled more easily—signs of more advanced disease. The pattern became even stronger in studies where most COPD patients were smokers: in these groups, nearly half had periodontitis, compared with about one in five where fewer patients smoked. This suggests that smoking amplifies gum problems in people who already have fragile lungs.
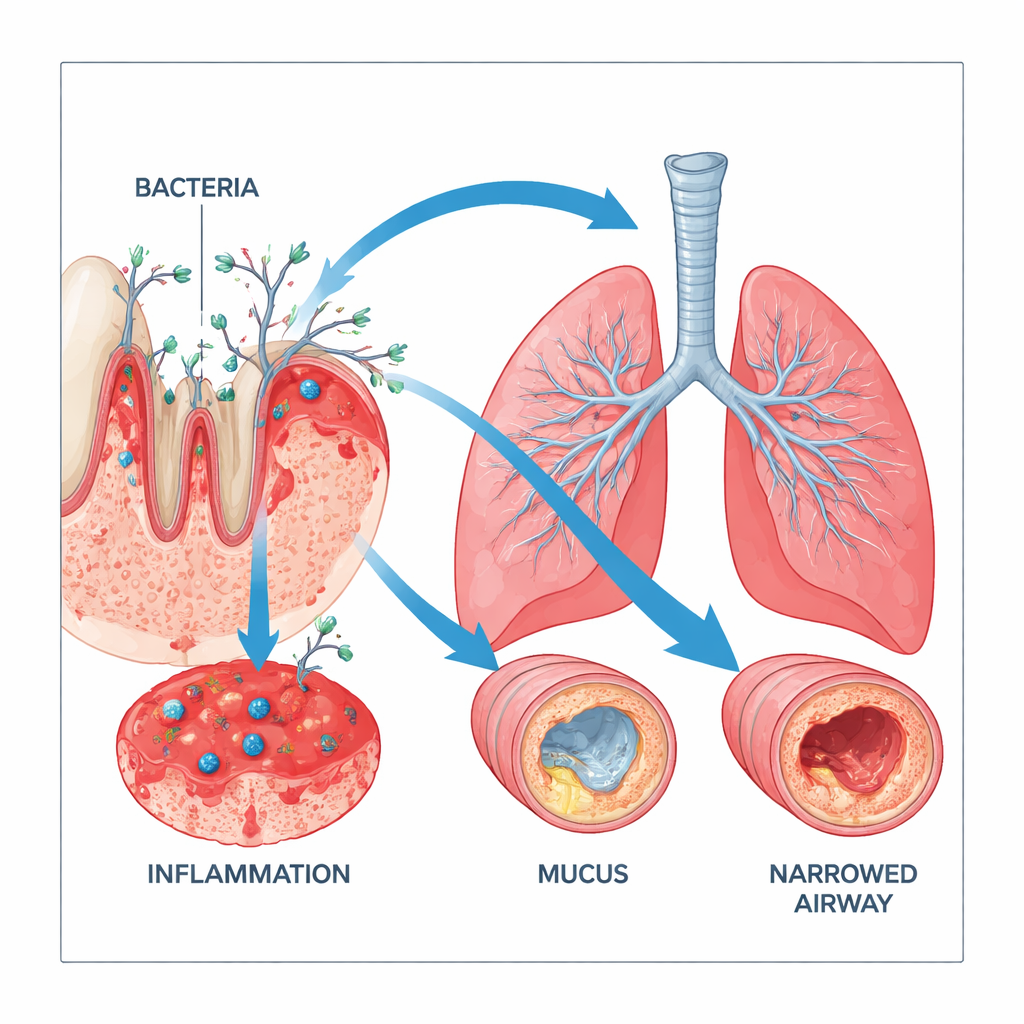
Why the connection is not yet fully proven
Despite these striking patterns, the authors stress that the evidence has important limits. Almost all the studies were observational, meaning they simply observed who had COPD and who had periodontitis rather than randomly assigning treatments. Many did not fully account for confounding factors such as smoking intensity, income, other illnesses, or medications that affect the mouth or lungs. When the authors used methods to detect possible publication bias—where studies showing no link are less likely to be published—the apparent strength of the association weakened, and in some cases the statistical signal became uncertain. As a result, formal grading of the evidence rated the overall certainty as low to very low.
What this means for everyday health
For the general reader, the message is cautious but practical: people with COPD are more likely to have serious gum disease, and their gum measurements are generally worse than in people without lung disease, but scientists cannot yet say that bad gums cause COPD to develop or flare up. It is more likely that shared habits and conditions—especially smoking—drive both problems, with gum infections possibly adding an extra inflammatory burden. Still, the findings support the idea that looking after oral hygiene, seeking regular dental care, and quitting smoking may benefit not only teeth but also breathing. The authors call for long‑term, well‑controlled studies to test whether treating gum disease can genuinely improve lung health and reduce COPD flare‑ups.
Citation: Sivaramakrishnan, G., Sridharan, K. Linking lungs and gums: a meta-analysis of periodontitis prevalence and severity in chronic obstructive pulmonary disease. BDJ Open 12, 16 (2026). https://doi.org/10.1038/s41405-026-00403-6
Keywords: COPD, gum disease, periodontitis, oral health, chronic inflammation