Clear Sky Science · en
Modulatory effects of ketamine on EEG source-based resting state connectivity in treatment resistant depression
Why this study matters for people with stubborn depression
Treatment-resistant depression is a form of major depression that does not improve even after trying several standard medications. For many people, this means years of low mood, loss of pleasure, and persistent negative thinking. Ketamine has attracted attention as a fast-acting option for these difficult cases, but scientists still do not fully understand how it changes brain activity. This study used brainwave recordings to look under the hood of ketamine’s effects on the resting brain and to ask which patterns of brain connectivity might be linked to relief from depressive and ruminative thoughts.
Looking at brain wiring in resting minds
Depression is increasingly seen as a problem of how large-scale brain networks talk to one another. Two key players are the “default mode” network, active during inward-focused, self-referential thinking, and the “frontoparietal” network, important for attention and control. In people with treatment-resistant depression, earlier work has found overly strong connections within the default mode network and abnormal communication between this network and control regions. The researchers wanted to see how a single ketamine infusion would alter the resting connections between these networks, and whether those changes would relate to improvements in mood, loss of pleasure, and rumination.
How the study was done
The team studied 24 adults with treatment-resistant depression and 34 healthy volunteers. All participants completed mood and rumination questionnaires and underwent an eight-minute resting brain recording using a 96-channel EEG cap, which measures electrical activity from the scalp. People with depression then received a standard low dose of intravenous ketamine, while the healthy volunteers received no treatment. About 24 hours later, everyone repeated the questionnaires and EEG session. Using a technique called source analysis, the researchers estimated where in the brain the EEG signals came from and calculated how strongly different regions in the default mode and frontoparietal networks were synchronized in specific frequency bands (especially theta and beta rhythms).
Ketamine eased symptoms but broadly boosted connectivity
As expected, people with treatment-resistant depression showed clear improvements one day after ketamine: their depression scores, anhedonia (loss of pleasure), and overall rumination all dropped, particularly the depressive and brooding types of repetitive thinking. Before treatment, compared with healthy volunteers, they already had stronger connectivity within the default mode network and between default mode and control regions. After ketamine, instead of the predicted “normalization” (less default mode over-connection and more focused frontoparietal connectivity), the researchers observed a broad increase in resting connectivity. Links within both the default mode and the frontoparietal networks became stronger, as did the connections between them, especially in beta-band activity involving regions important for memory and self-focused thought, such as the angular gyrus and parahippocampal areas.
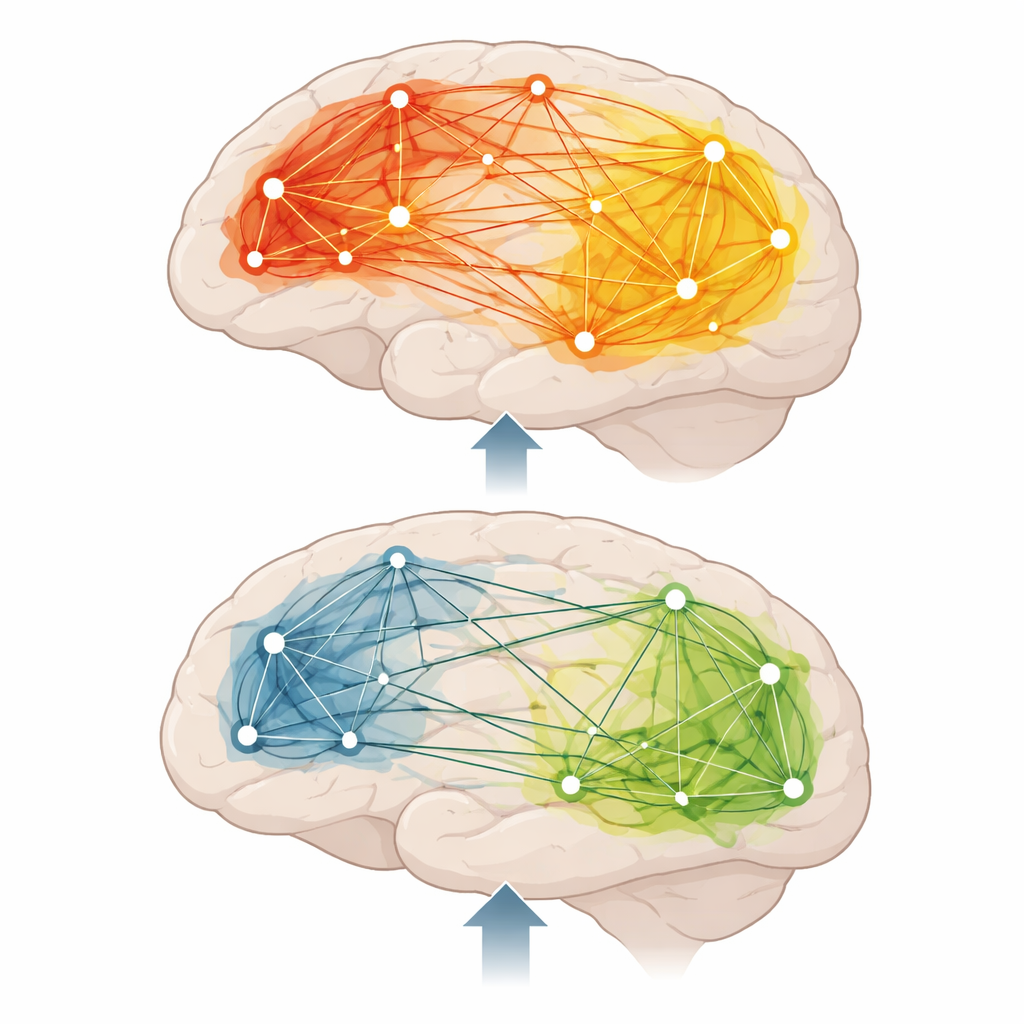
Clues from pre-treatment brain patterns
An important twist was that the amount of change in connectivity after ketamine did not line up with the amount of symptom relief. Instead, what mattered more was how the brain was wired before treatment. Individuals whose initial resting connectivity within and between these networks was lower tended to show larger reductions in depression-related rumination after ketamine. In other words, baseline brain network patterns, rather than the acute shift in wiring 24 hours later, seemed to carry more information about who would benefit most in terms of reduced negative thinking.
What this means for understanding ketamine
The authors interpret the broad boost in connectivity as a possible sign of ketamine-driven synaptogenesis—the rapid formation and strengthening of connections between nerve cells. Animal studies suggest that ketamine can quickly grow new synaptic spines in prefrontal circuits, with a surge around 12–24 hours after dosing, followed by pruning in the days that follow. This study’s snapshot at 24 hours may thus capture a temporary “overconnected” stage that supports longer-lasting repair of depressed brain circuits. For people living with treatment-resistant depression, the work underscores that ketamine reliably reduces symptoms in the short term and hints that future EEG-based measures of resting connectivity might help tailor who receives such treatments and when, once we better understand how these brain changes unfold over time.
Citation: Lees, T., Scott, J.N., Boyle, B.W. et al. Modulatory effects of ketamine on EEG source-based resting state connectivity in treatment resistant depression. Transl Psychiatry 16, 134 (2026). https://doi.org/10.1038/s41398-026-03928-4
Keywords: treatment-resistant depression, ketamine, brain connectivity, EEG, rumination