Clear Sky Science · en
Developmental trajectories of glutamate and the variable clinical course of ADHD in youth
Why some kids grow out of ADHD and others do not
Parents and teachers often notice that attention problems and hyperactivity can fade for some children as they enter their teen years, yet remain stubbornly present for others. This study asks a simple but important question: is there something different in how the brain develops in young people whose ADHD symptoms persist versus those whose symptoms ease? Focusing on a key brain chemical called glutamate and a region involved in focus and self-control, the researchers followed children over time to see how brain chemistry and brain wiring changed as they grew.
A closer look at a key brain messenger
The scientists centered their work on glutamate, the brain’s main “go” signal that helps nerve cells pass messages. Glutamate has already been linked to ADHD through genetics, brain tissue studies, and early medication research. Here, the team wanted to know whether the way glutamate changes as children mature might help explain why ADHD follows different paths: for some, symptoms linger; for others, they lessen enough that the diagnosis no longer applies. They focused on the medial prefrontal cortex, a frontal brain area that helps us pay attention, make decisions, and regulate emotions—all functions that are often challenged in ADHD. 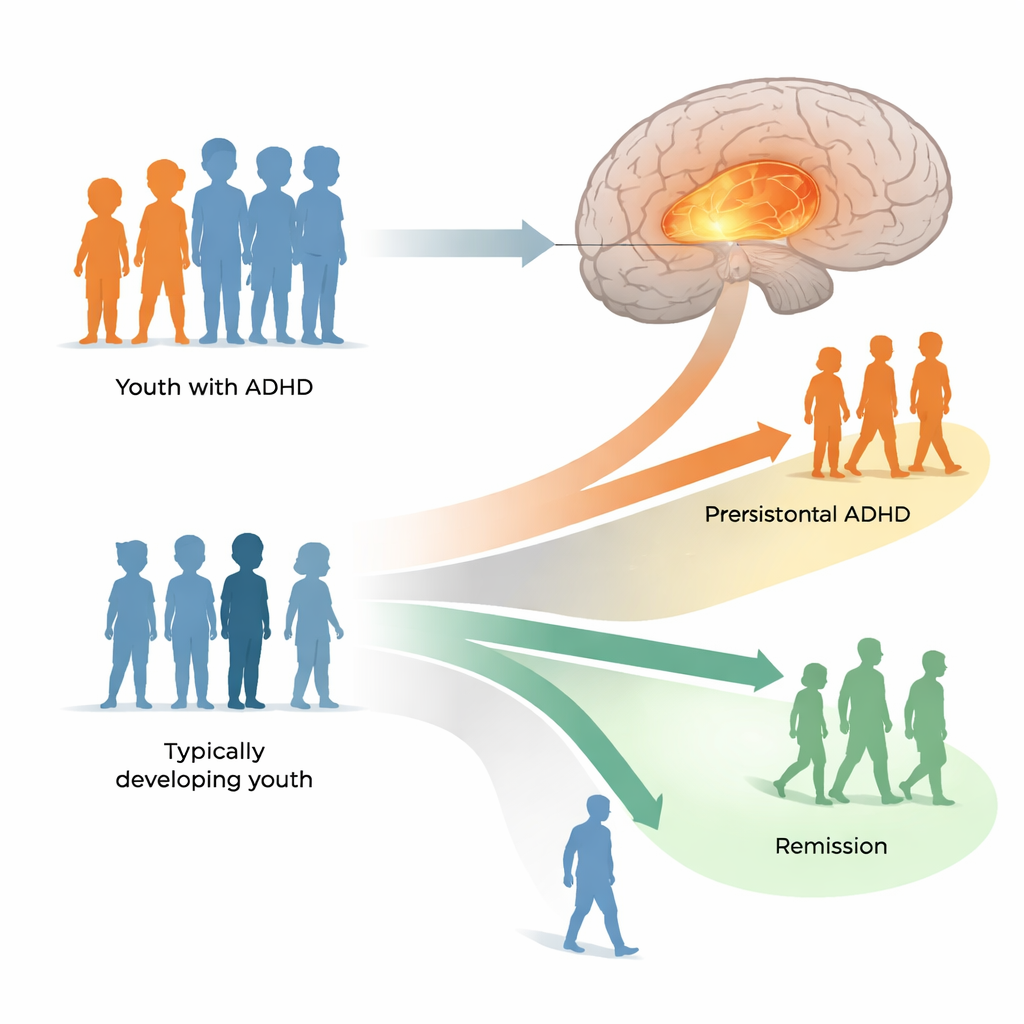
Tracking brain chemistry as kids grow up
To measure glutamate safely inside the brain, the researchers used a specialized MRI-based method called magnetic resonance spectroscopy in 161 young people. Sixty-nine had ADHD that remained present over the study period, 20 had ADHD that later remitted, and 72 had never been diagnosed with ADHD. Many participants were scanned more than once, allowing the team to track how glutamate levels in the medial prefrontal cortex changed with age. At the same time, a subset of 104 youth also underwent resting-state functional MRI scans, which capture how different brain regions “talk” to each other when a person is not doing any particular task.
Two different developmental paths in the same brain region
At the first scan, glutamate levels in the frontal brain region did not differ much between the groups. The striking differences emerged in how these levels changed over time. In teens whose ADHD symptoms persisted, glutamate in the medial prefrontal cortex tended to increase with age. By contrast, in youth whose ADHD remitted and in those who had never had ADHD, glutamate levels tended to decrease as they moved from late childhood into adolescence. This downward trend matches prior work in typically developing people, where glutamate rises early in childhood and then gradually declines as circuits in the frontal lobe refine. The results suggest that in persistent ADHD, this “maturing” pattern of glutamate may be delayed or altered, whereas remitting ADHD follows a more typical developmental course.
How brain chemistry relates to brain network wiring
Brain function depends not only on local chemistry but also on how regions connect into larger networks. The medial prefrontal cortex is part of the default mode network, which is active during inward-focused thought and usually quiets down when we need to concentrate. In the subgroup with both chemistry and connectivity data, higher glutamate in the medial prefrontal cortex was linked, in the persistent ADHD group, to stronger internal communication within the default mode network and stronger connections between this network and deeper structures such as the caudate and parts of the amygdala. These same relationships were different or weaker in youth without ADHD. In other words, altered glutamate levels in a key frontal area were tied to an atypical pattern of brain network wiring that has previously been associated with lapses of attention and mind-wandering. 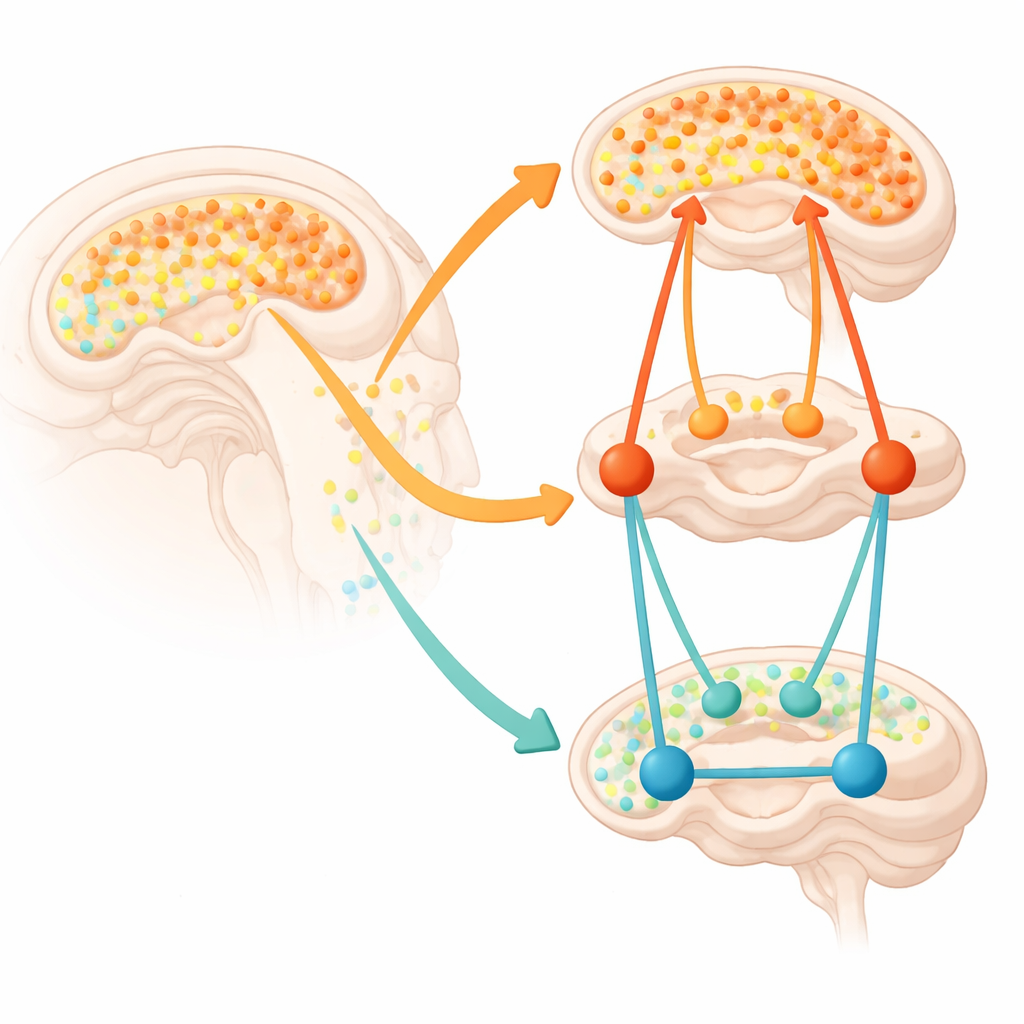
What this means for understanding ADHD over time
Put simply, the study suggests that when ADHD symptoms persist, the frontal brain’s chemical and network development may stay on an unusual track, whereas young people who “grow out of” ADHD look more like their peers in both glutamate changes and brain connectivity. The work does not yet provide a test that can predict an individual child’s outcome, and it is limited to one brain region and a still modest sample. But it offers a window into how a common childhood condition is intertwined with the unfolding of brain chemistry and wiring, and underscores that ADHD is not a fixed state. Instead, it reflects a moving target in brain development—one that, for many youth, can gradually shift toward more typical function over time.
Citation: Bouyssi-Kobar, M., Zhang, Y., Norman, L. et al. Developmental trajectories of glutamate and the variable clinical course of ADHD in youth. Transl Psychiatry 16, 157 (2026). https://doi.org/10.1038/s41398-026-03898-7
Keywords: ADHD, glutamate, brain development, prefrontal cortex, brain connectivity