Clear Sky Science · en
Neurobiological mechanisms of electroconvulsive therapy in major depressive disorder: structure-function coupling with gene expression and molecular mechanism
Why Shocking the Brain Still Matters
Electroconvulsive therapy, or ECT, is one of the oldest treatments in psychiatry and is often portrayed in frightening ways. Yet for people with severe depression who do not respond to standard medications or talk therapy, it remains one of the most effective and fastest-acting options. This study asks a simple but important question: what does ECT actually do inside the brain and at the level of our genes that helps some people recover from major depressive disorder?
How Depression Warps Brain Communication
Major depression is more than a low mood. It is linked to disrupted communication in key brain networks. Two of the most important are the “default mode” network, which supports self-reflection and daydreaming, and the “somatomotor” network, which helps tie body sensations to actions. In healthy brains, the physical wiring of these networks and the moment-to-moment activity that runs across that wiring are closely matched. In depression, this match is weakened, leaving information flow less efficient. The researchers tracked 88 adults with major depression before and after a full course of ECT, using MRI scans to measure both the brain’s structural connections (the white-matter “cables”) and functional connections (regions that activate together over time), and then examined how tightly these two types of connectivity were coupled across different regions.
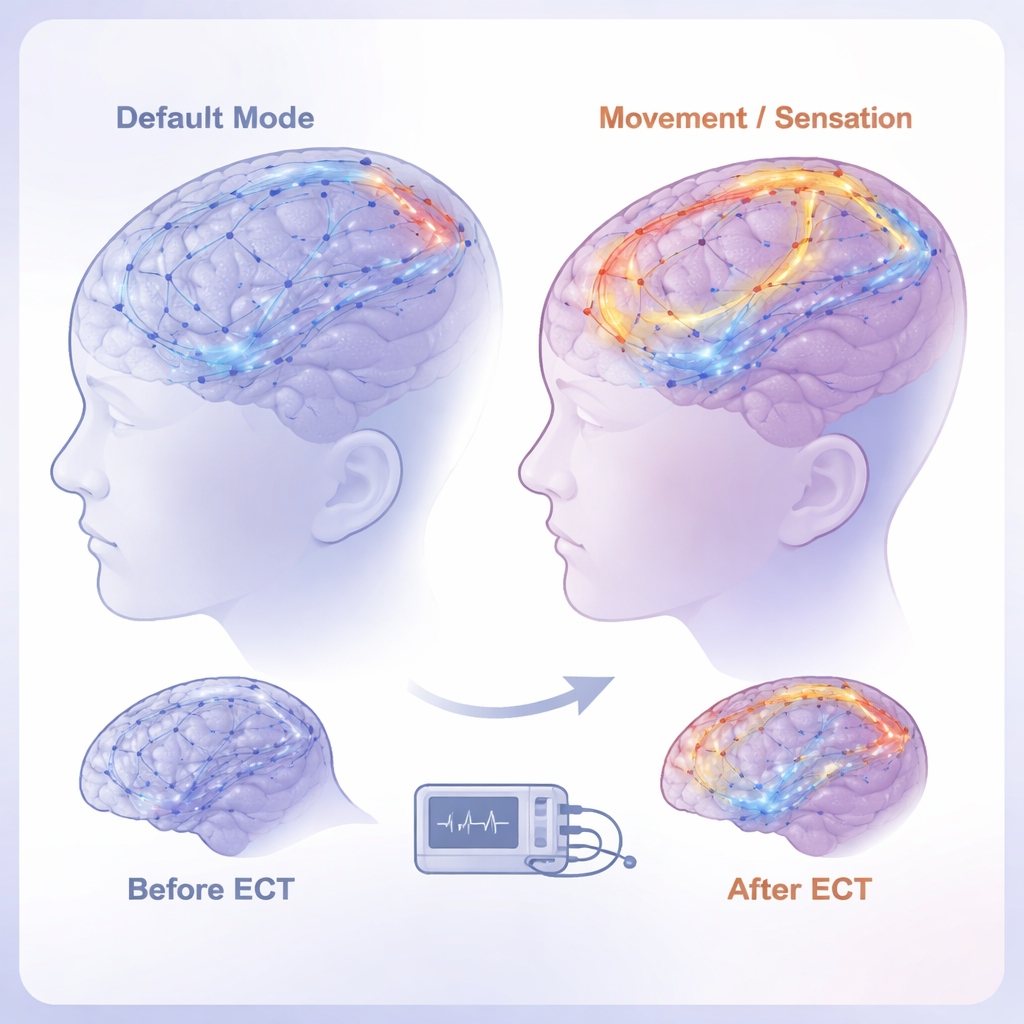
ECT as a Brain Network Reset
After ECT, patients’ depression and anxiety scores dropped sharply, confirming the strong clinical effect. In parallel, the match between structure and function in the brain—called structure–function coupling—became stronger in specific networks rather than everywhere at once. The biggest increases appeared in the default mode and somatomotor networks, especially in frontal and cingulate regions that are involved in mood, attention, and bodily awareness. Functional communication between areas changed significantly, while the underlying structural wiring changed little, suggesting that ECT works mainly by re-tuning how existing circuits are used. Using a machine learning model, the team showed that a person’s pre-ECT coupling pattern could predict how much their symptoms would later improve, highlighting these network measures as potential biomarkers to guide treatment choice.
From Brain Scans to Genes and Cell Power
To see what might be happening at a biological level, the scientists compared the brain regions most altered by ECT with maps of gene activity from large human brain atlases. Regions where coupling improved most tended to overexpress genes related to synapses—the tiny junctions where nerve cells communicate—and to pathways that control how cells grow, adapt, and respond to signals. Many of these genes were active in both excitatory and inhibitory nerve cells, as well as in supporting cells like astrocytes and oligodendrocytes, suggesting a broad reset of the balance and support systems within neural circuits. They also found links to genes involved in mitochondrial function, the energy factories inside cells, implying that ECT may boost the brain’s ability to fuel demanding network activity and plasticity.
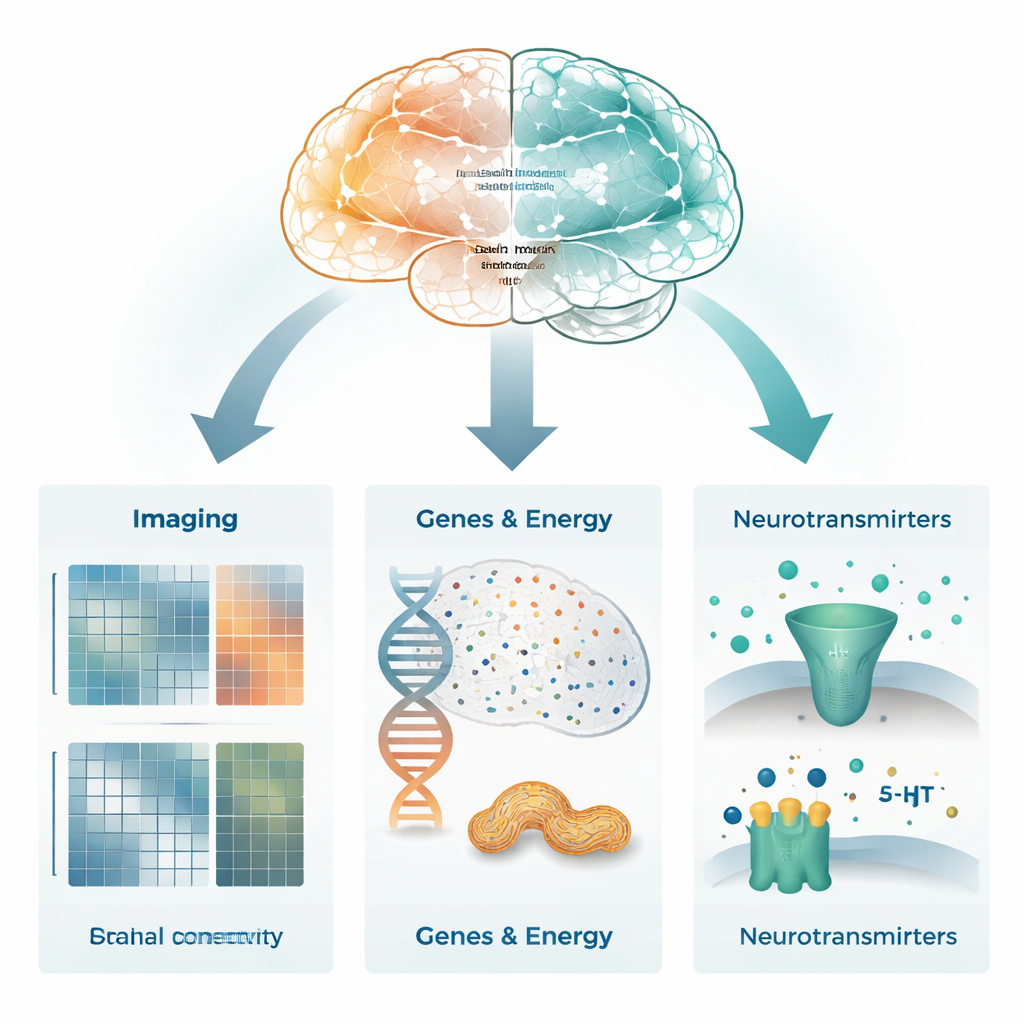
Brain Chemicals in the Spotlight
The team then asked how these network changes related to brain chemicals targeted by common antidepressants. By comparing their MRI results to maps of neurotransmitter receptors measured in healthy volunteers with PET imaging, they found that regions whose coupling changed most after ECT lined up with areas rich in serotonin and dopamine receptors, as well as receptors for glutamate, the main excitatory transmitter. A combined statistical model suggested that one specific serotonin receptor type (5-HT1B) contributed the most to explaining the pattern of ECT-related changes. This supports the idea that ECT acts not just on circuits but also on the chemical systems that shape mood, motivation, and learning.
What This Means for People With Depression
For non-specialists, the message is that ECT does not simply “shock” the brain into submission. Instead, it appears to carefully retune key networks that govern how we think about ourselves and how our bodies and emotions are linked, while engaging genes that support synaptic repair and cellular energy, and rebalancing major mood-related chemicals like serotonin and dopamine. Understanding these mechanisms may eventually help doctors predict who will benefit from ECT, minimize side effects, and design new treatments that capture its powerful antidepressant effects without the need for electrical stimulation.
Citation: Qian, R., Huang, W., Ji, Y. et al. Neurobiological mechanisms of electroconvulsive therapy in major depressive disorder: structure-function coupling with gene expression and molecular mechanism. Transl Psychiatry 16, 76 (2026). https://doi.org/10.1038/s41398-026-03892-z
Keywords: electroconvulsive therapy, major depressive disorder, brain networks, gene expression, serotonin