Clear Sky Science · en
MKRN1 as a prioritized drug target for postpartum depression: evidence from druggable proteome profiling and multi-layer validation
Why this research matters for new mothers
Postpartum depression (PPD) affects up to one in five new mothers worldwide, disrupting bonding, daily functioning, and infant development. Current medicines can be hard to tolerate, may affect breastfeeding, and were not designed specifically for PPD. This study asks a simple but crucial question: can we pinpoint a single protein in the body that both causes PPD and can be safely targeted by future drugs?
Looking for hidden clues in big genetic data
The researchers started by mining large genetic studies of women with and without PPD. Instead of stopping at DNA variants, they connected these variants to the proteins they influence in the brain. This method, called proteome-wide association, let them move from abstract genetic signals to concrete molecules that might shape mood after childbirth. Using two independent brain protein datasets, they repeatedly saw the same two candidates stand out: a protein called MKRN1 and another called CCDC92. 
Narrowing down to one promising protein
To test whether these proteins truly contribute to PPD rather than just being bystanders, the team applied a tool known as Mendelian randomization. It uses naturally occurring genetic differences as a kind of lifelong “randomized trial” to infer cause and effect. When they did this, only MKRN1 passed all checks: it showed strong evidence of being on the direct pathway to PPD, while CCDC92 did not. Additional statistical tests confirmed that the same genetic variants influenced both MKRN1 levels and PPD risk, strengthening the case that MKRN1 is a true driver rather than a coincidental signal.
Checking safety across hundreds of diseases
Finding a protein linked to PPD is not enough; a good drug target must also be reasonably safe. The researchers therefore examined how genetically driven changes in MKRN1 levels related to 783 different diseases recorded in the UK Biobank. Higher MKRN1 was clearly associated with depression and mood disorders, but not meaningfully tied to other major illnesses once strict statistical corrections were applied. This pattern suggests that medicines designed to adjust MKRN1 activity might focus mainly on mood without causing wide-ranging side effects in other organs, at least based on current genetic evidence.
Evidence from blood, brain, and animal models
The team then asked whether MKRN1 is actually altered in people with depression and in animal models of stress. In blood samples from women with PPD, the DNA region that controls MKRN1 showed lower methylation, an epigenetic mark often linked to increased gene activity. Consistent with this, MKRN1 levels were higher in key emotion-related brain areas, particularly the anterior cingulate gyrus, in people with major depression and in stressed mice. MKRN1 was also elevated in whole blood and white blood cells in multiple human and mouse studies, suggesting it could serve as a practical blood biomarker rather than requiring brain tissue to be measured. 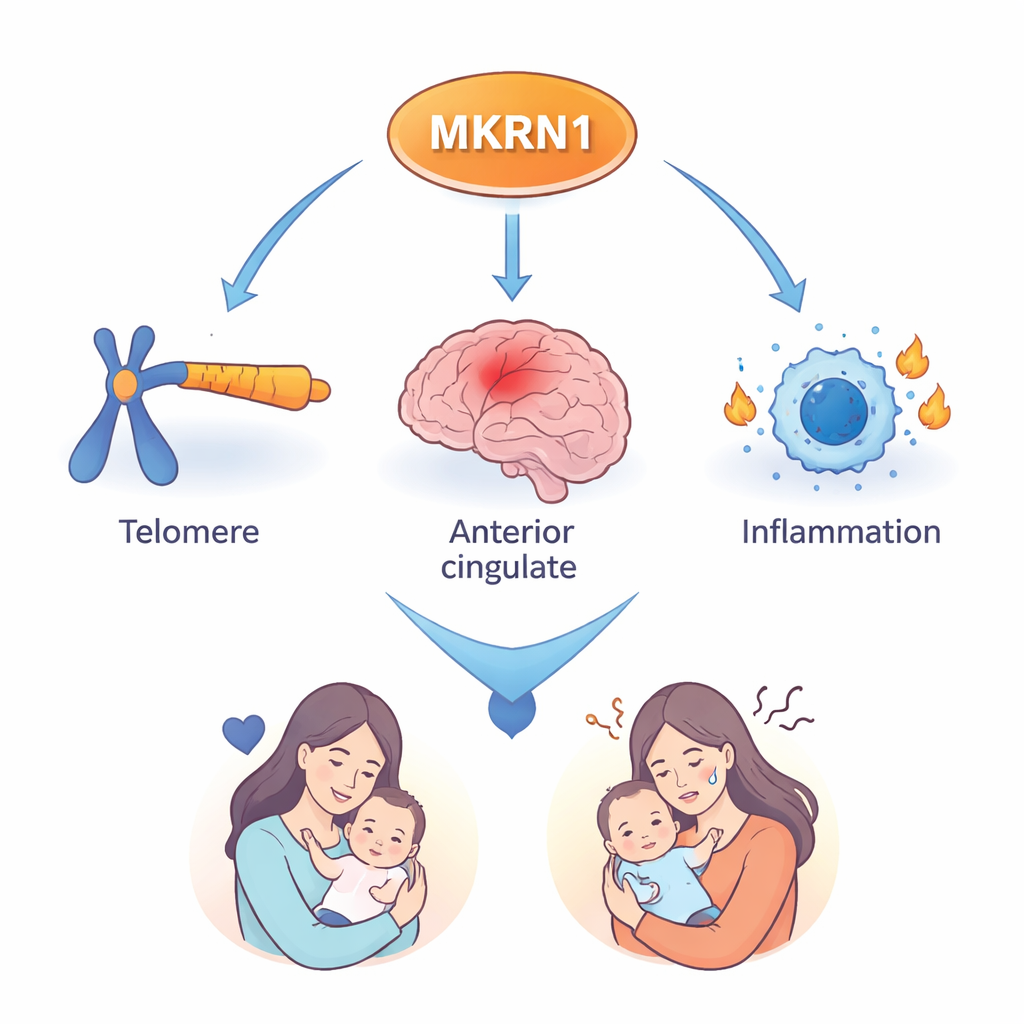
Clues pointing to the body’s defense system
Finally, the researchers explored which biological pathways travel alongside MKRN1. Genes that rose and fell together with MKRN1 were enriched for immune and inflammatory functions, including the movement of white blood cells and activity of immune receptors. This dovetails with growing evidence that inflammation and oxidative stress are closely linked to depression, and that shifts in the immune system after childbirth may influence mental health. The data hint that MKRN1 may help connect changes in brain circuits, cellular aging, and immune responses in the PPD story.
What it all means for future treatments
For non-specialists, the core message is that this study uses multiple layers of modern biology—DNA, proteins, epigenetics, and large health databases—to elevate MKRN1 from a long list of genes to a top-priority target for postpartum depression. MKRN1 appears to be increased in women with PPD, is causally linked to depression risk, shows signs of acting through immune and stress pathways, and does not seem to strongly drive other diseases. While more work is needed before any drug reaches the clinic, MKRN1 now stands out as a realistic, testable starting point for safer, more precise therapies and blood-based tests to help protect the mental health of new mothers and their babies.
Citation: Jia, T., Yuan, C., Hu, S. et al. MKRN1 as a prioritized drug target for postpartum depression: evidence from druggable proteome profiling and multi-layer validation. Transl Psychiatry 16, 75 (2026). https://doi.org/10.1038/s41398-026-03886-x
Keywords: postpartum depression, MKRN1, genetics, inflammation, biomarkers