Clear Sky Science · en
Natural Anti-NMDAR1 autoantibodies associate with slowed decline of cognitive functions in Alzheimer’s diseases
Why This Matters for Families Facing Memory Loss
Alzheimer’s disease slowly erodes memory and thinking, and current medicines offer only modest help, sometimes with serious side effects. This study explores an unexpected, natural line of defense already present in some people’s blood: special antibodies called anti-NMDAR1 autoantibodies. The research asks a simple but important question—do people with Alzheimer’s who naturally have more of these antibodies lose their thinking abilities more slowly?
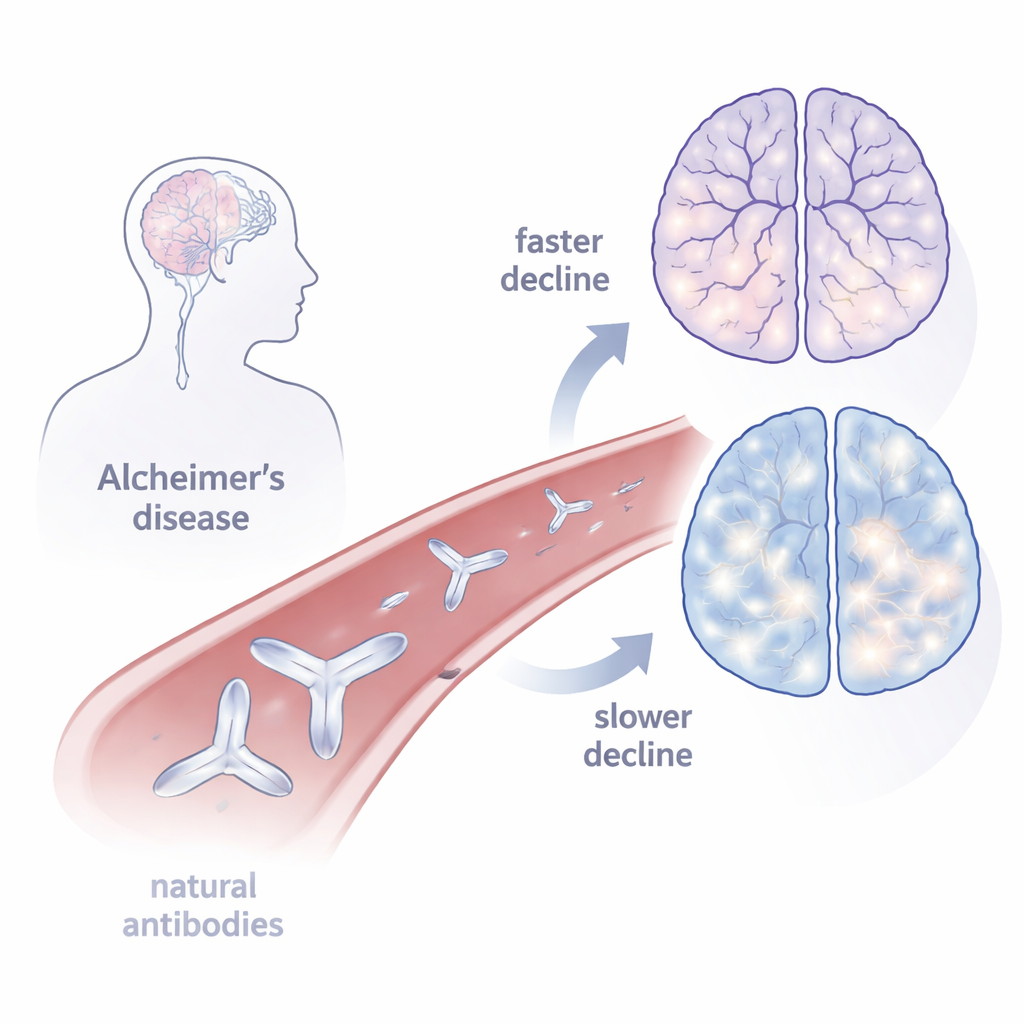
A Surprising Ally in the Blood
Antibodies are proteins our immune system makes to recognize and bind to specific targets. Autoantibodies are a special type that recognize parts of our own body. For years, doctors thought that autoantibodies against brain receptors, such as NMDAR1, were always harmful. Yet low levels of these anti-NMDAR1 autoantibodies are found in about 5–10% of healthy people, raising the possibility that, at low doses, they might sometimes help instead of hurt. In Alzheimer’s disease, a brain chemical called glutamate can build up outside nerve cells and overstimulate them, a process known as excitotoxicity that contributes to cell damage and cognitive decline. Because anti-NMDAR1 autoantibodies can dampen activity at glutamate-sensitive receptors, the author wondered whether natural levels of these antibodies might partly shield the brain.
How the Study Was Done
The researcher used a newly developed, highly sensitive test to measure very low levels of anti-NMDAR1 autoantibodies in blood samples from 324 older adults: 161 with early Alzheimer’s disease and 163 healthy controls. All participants had standard testing of thinking and daily function, including the Mini-Mental State Examination (MMSE), a brief exam widely used to track memory and orientation, and the Clinical Dementia Rating Sum of Boxes (CDRSUM), which reflects daily functioning. Additional tests measured verbal fluency (how many words a person can generate under simple rules) and attention. Instead of just calling people “positive” or “negative” for the antibody, the study treated antibody level as a continuous measure and also compared people in the highest quarter of levels to everyone else.
Sharper Thinking in Patients with Higher Antibody Levels
Among people with Alzheimer’s disease, those who had higher levels of natural anti-NMDAR1 autoantibodies scored better on the MMSE than those with lower levels, even after accounting for factors like sex and years of education. Their average MMSE scores were about two points higher, a meaningful difference in this scale. The same pattern appeared in more detailed cognitive tests. Patients with higher antibody levels produced more correct words and more total words in verbal fluency tasks that asked them to say as many words as possible starting with the letter “S.” They also did better on a measure of attention. In contrast, among healthy older adults, having higher or lower levels of these antibodies did not make a noticeable difference in test scores, suggesting that at the natural levels seen here, the antibodies were not obviously harmful.
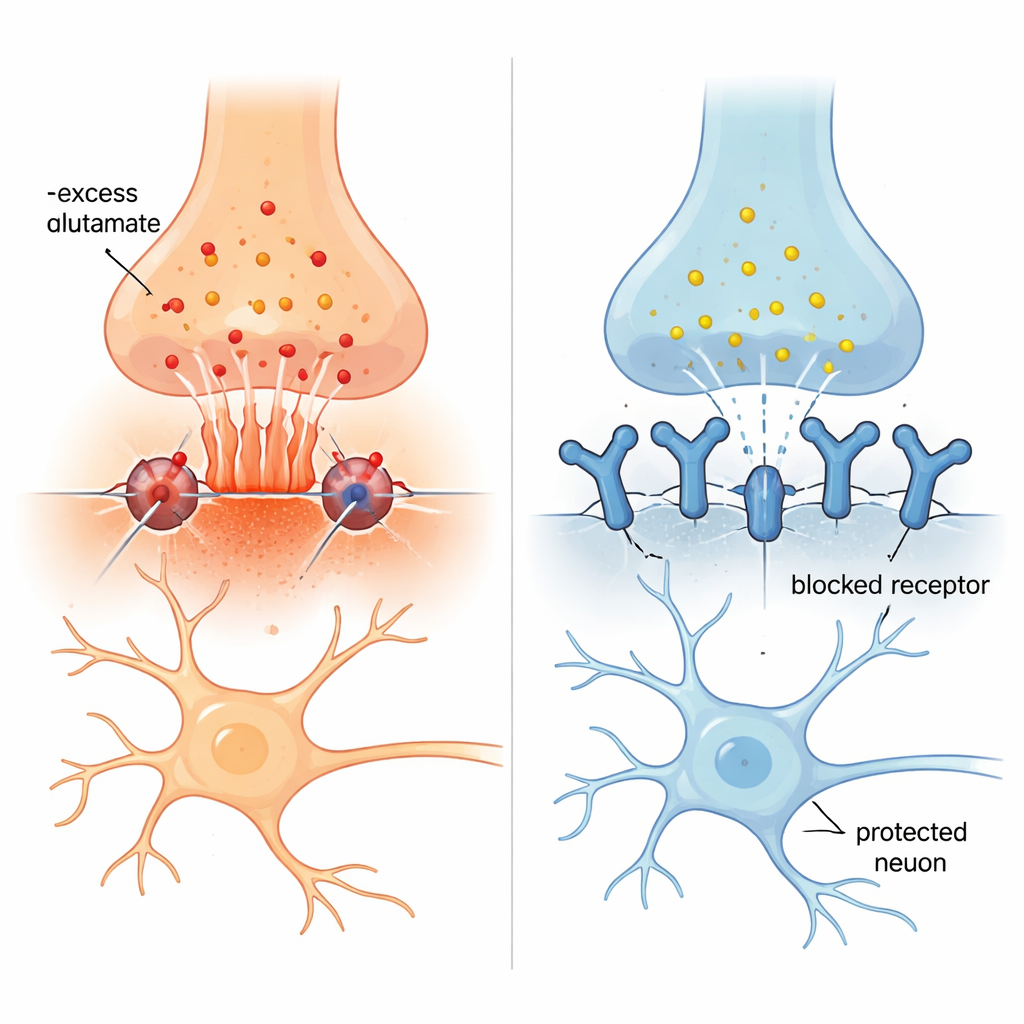
A Possible Protective Mechanism
The study offers a biological explanation for these findings. In Alzheimer’s disease, the protective barrier between the blood and the brain often becomes leaky, allowing a small fraction of circulating antibodies to enter the brain. Natural anti-NMDAR1 autoantibodies are thought to be mostly of the IgM type, which are large molecules. Because of their size, they may mainly reach receptors outside the tiny space where nerve cells directly communicate (the synapse). These extrasynaptic receptors are believed to be key drivers of glutamate-induced damage. By partially blocking these receptors, IgM antibodies may reduce the harmful overactivation that kills nerve cells, while leaving the synaptic receptors—needed for normal learning and memory—more intact. This idea is consistent with the way an approved Alzheimer’s drug, memantine, works: it preferentially dampens the same harmful extrasynaptic signals.
What This Could Mean for Future Treatments
For non-specialists, the takeaway is that some people with Alzheimer’s appear to carry in their own blood a weak, naturally occurring “drug” that may slow down memory loss. The study does not prove that the antibodies actually cause protection; it only shows that higher levels travel together with better performance. Larger studies and animal experiments are needed to confirm whether these antibodies truly shield brain cells and to separate helpful IgM antibodies from potentially harmful IgG types. Still, if future work confirms a protective role, boosting the right kind of anti-NMDAR1 antibodies—or designing medicines that mimic them—could open an entirely new, potentially safer strategy to slow cognitive decline in Alzheimer’s and possibly other brain diseases driven by glutamate toxicity.
Citation: Zhou, X. Natural Anti-NMDAR1 autoantibodies associate with slowed decline of cognitive functions in Alzheimer’s diseases. Transl Psychiatry 16, 92 (2026). https://doi.org/10.1038/s41398-026-03878-x
Keywords: Alzheimer’s disease, autoantibodies, glutamate excitotoxicity, NMDA receptor, cognitive decline