Clear Sky Science · en
Understanding betel nut addiction: a review of harmful consequences, underlying neurobiology, and emerging intervention strategies
Why a Common Chewing Habit Matters
Across much of Asia and the Pacific, chewing betel nut is as everyday as drinking coffee—used to stay alert, socialize, and honor tradition. This review article shows that behind this familiar habit lies a potent addictive drug with wide‑ranging health consequences, from oral cancer to heart disease and mental health problems. Understanding how betel nut affects the body and brain helps explain why quitting is so hard and why stronger prevention and treatment efforts are urgently needed worldwide.
Who Chews Betel Nut and How It Harms Health
Betel nut is now the world’s fourth most commonly used psychoactive substance, after tobacco, alcohol, and caffeine, with about 600 million users. Use is concentrated in South Asia, parts of China and Southeast Asia, the Western Pacific, and among migrant communities abroad. Men are three to five times more likely to chew than women, and people often start in their teens, with use peaking in early and middle adulthood. Chewing is especially common among manual laborers and low‑income groups, who use it to fight fatigue and stress. Yet long‑term use is strongly linked to oral diseases, particularly oral submucous fibrosis and oral cancer, as well as heart and blood vessel problems, metabolic syndrome, liver damage, kidney disease, lung disease, bone loss, and reproductive and pregnancy complications. Combined with smoking and drinking, betel nut dramatically amplifies cancer risks.
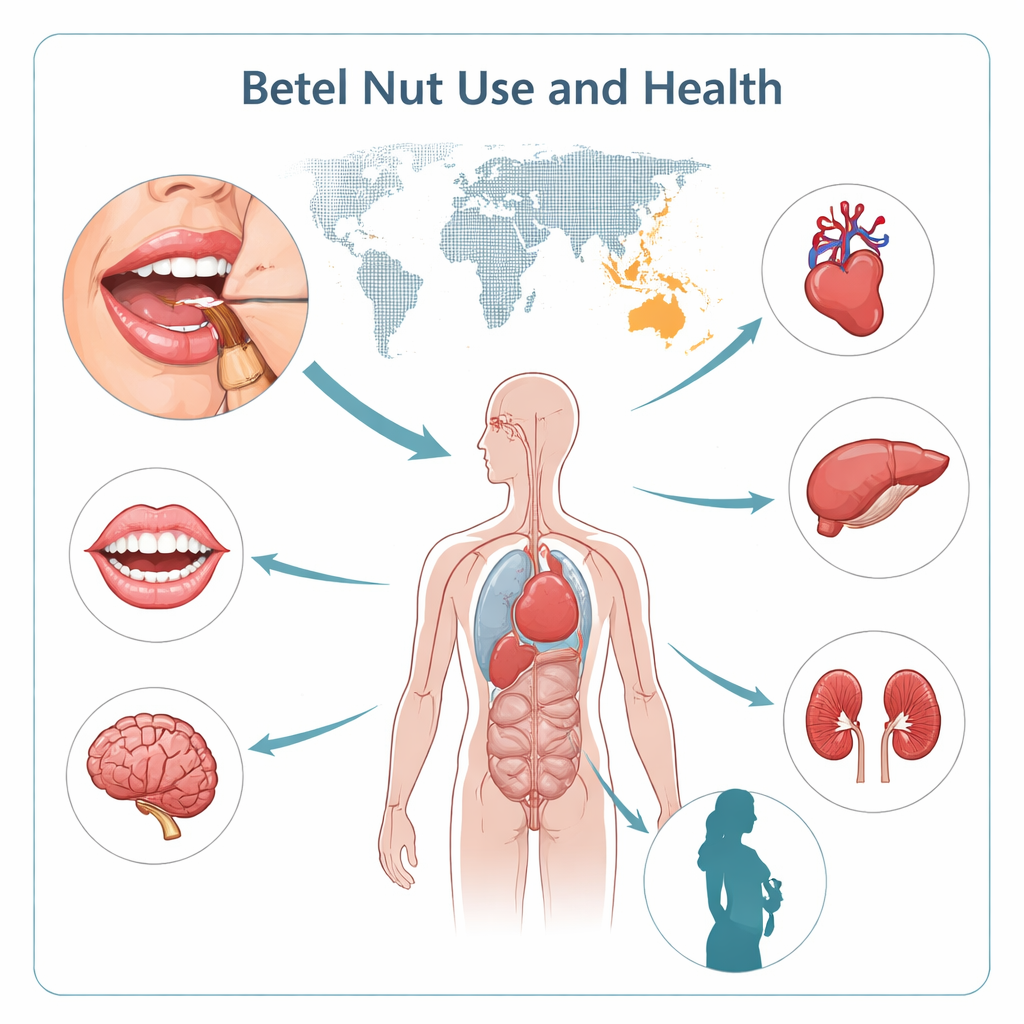
How a Small Fruit Hooks the Brain
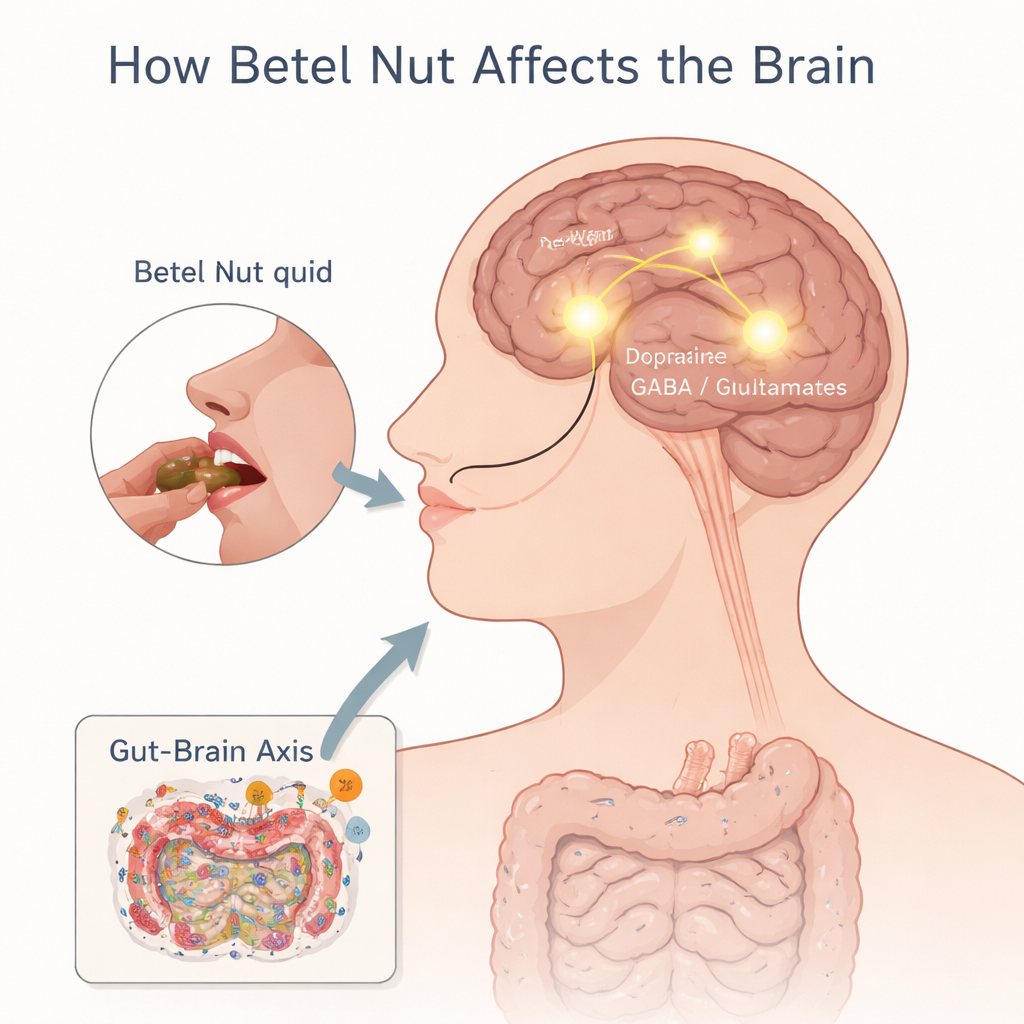
The key addictive ingredient in betel nut is arecoline, an alkaloid that acts on the same broad brain systems affected by nicotine and some other drugs. Once absorbed, arecoline activates receptors for the neurotransmitter acetylcholine and, through them, disturbs the balance of dopamine (the reward chemical), GABA (a calming signal), and glutamate (an excitatory signal). These changes stimulate the brain’s reward pathways, making users feel more alert, focused, and uplifted—effects that encourage repeated use. Brain imaging studies of regular chewers reveal thinner and structurally altered regions in the prefrontal cortex, and disturbed connectivity in circuits that control impulses, decision‑making, and emotional regulation. Over time, these changes can produce tolerance, craving, withdrawal symptoms such as anxiety and irritability, and a loss of control over chewing—features that mirror other substance use disorders.
The Hidden Role of the Gut, Immune System, and Genes
Newer research shows that betel nut’s impact is not confined to the brain itself. Chewing reshapes the gut microbiome, reducing helpful bacteria and protective short‑chain fatty acids while favoring species linked to inflammation. This disruption of the “gut–brain axis” can weaken the intestinal barrier and blood–brain barrier, promote chronic inflammation, and alter the metabolism of tryptophan, a building block for the mood‑regulating chemical serotonin. In parallel, arecoline increases oxidative stress and triggers inflammatory signals that damage cells in multiple organs, including neurons. The review also highlights emerging evidence that epigenetic changes—chemical tags on DNA and histones that influence how genes are switched on or off—may increase vulnerability to addiction and shape how severely individuals respond to betel nut. Variations in genes related to dopamine receptors and drug‑metabolizing enzymes may help explain why some chewers become highly dependent while others do not.
New Paths to Treatment and Prevention
Because betel nut addiction shares biology with nicotine and other drugs, researchers are testing a broad toolkit of interventions. Experimental medicines include drugs that block or modulate the receptors targeted by arecoline, antidepressants that stabilize dopamine and serotonin signaling, glutamate‑modulating agents to ease craving and withdrawal, and anti‑inflammatory and antioxidant compounds that may protect the brain. Traditional Chinese herbal formulas are also being explored for their multi‑target effects on neurotransmitters, oxidative stress, and the gut microbiome. Non‑drug approaches range from brain‑stimulation methods, such as transcranial magnetic stimulation and real‑time fMRI neurofeedback, to virtual‑reality–based therapies that help people unlearn cue‑driven cravings. At the same time, cognitive‑behavioral therapy, school‑based programs, and strong public‑health measures—like warning campaigns, ingredient restrictions, advertising bans, and taxation—have already shown promise in reducing use in some regions.
What This Means for People and Communities
For individuals and societies, the article’s core message is straightforward: betel nut is not a harmless pick‑me‑up, but an addictive substance that can quietly damage many organs and fuel serious diseases and social inequalities. Yet the same science that reveals its risks also points to solutions. By combining medical treatments, psychological support, community education, and smart policies, and by tailoring these tools to local cultures and economies, it should be possible to prevent many new cases of addiction and help current chewers quit. In doing so, countries can protect vulnerable groups, lessen the burden of cancer and chronic disease, and support healthier futures for millions of people whose lives are intertwined with this ancient plant.
Citation: Shao, M., Zhuang, L., Xie, S. et al. Understanding betel nut addiction: a review of harmful consequences, underlying neurobiology, and emerging intervention strategies. Transl Psychiatry 16, 94 (2026). https://doi.org/10.1038/s41398-026-03875-0
Keywords: betel nut addiction, arecoline, oral cancer, gut–brain axis, substance use disorder