Clear Sky Science · en
The role of lipids in neuromodulation for psychiatric disorders: A narrative review
Why Fats in the Brain Matter
Most of us think of fat as something we want to avoid, but in the brain, fats—called lipids—are essential building blocks. This review article explores how these brain fats may shape the success of powerful treatments that use electricity or magnets to reset disordered brain activity in severe depression, obsessive–compulsive disorder, and related conditions. Understanding this connection could one day help doctors predict who will benefit from these last‑resort therapies and how to make them safer and more effective.
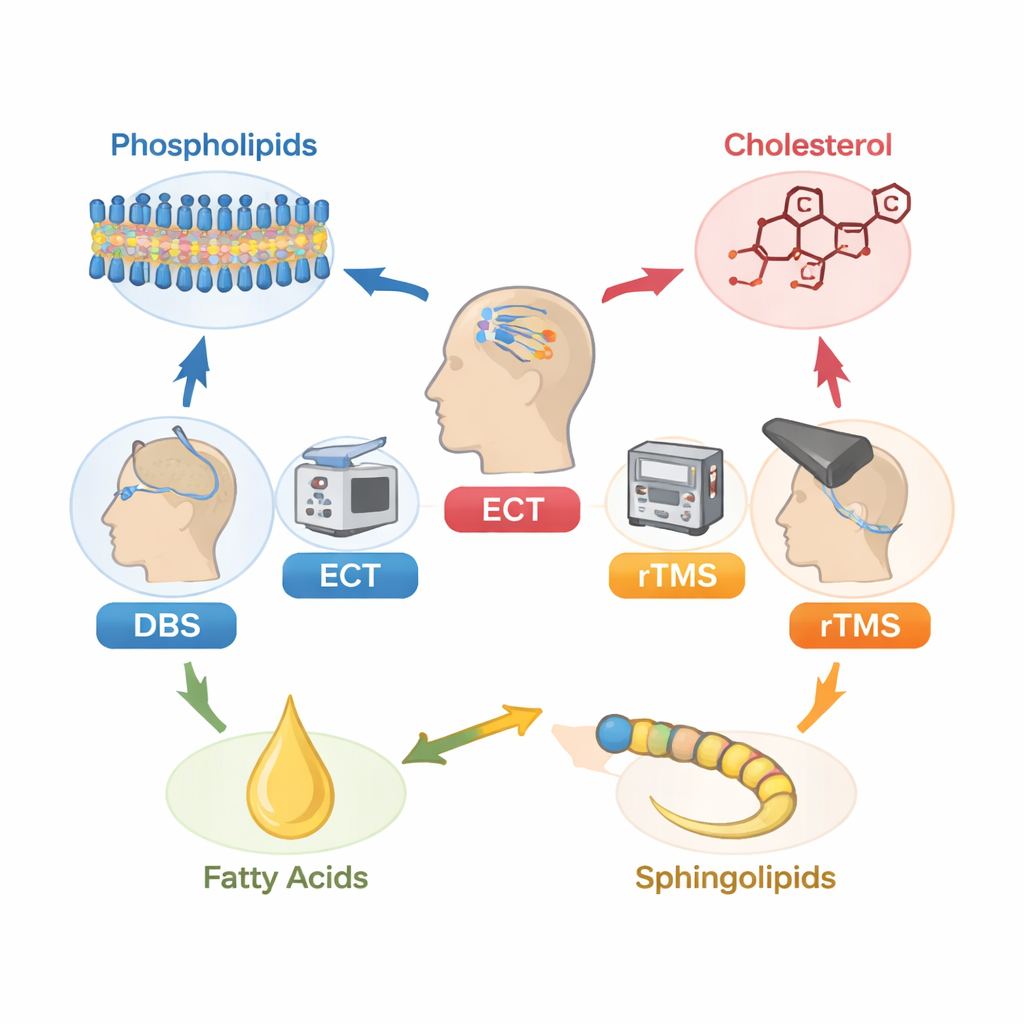
Brain Stimulation as a Last Resort
When talk therapy and standard medications fail, doctors may turn to neuromodulation: treatments that directly alter brain activity. Deep brain stimulation (DBS) uses implanted electrodes to deliver constant pulses to specific deep brain areas. Electroconvulsive therapy (ECT) applies brief electrical currents across the scalp under anesthesia to trigger a controlled seizure, often relieving severe depression. Repetitive transcranial magnetic stimulation (rTMS) uses magnetic pulses from a coil held against the head to nudge brain circuits without surgery. These approaches can help many people with long‑standing, difficult‑to‑treat illness, but not everyone responds, and the biological reasons for this difference are still unclear.
The Many Jobs of Brain Fats
More than half of the brain’s dry weight is made of lipids, and they do far more than store energy. Phospholipids form the flexible outer skin of every brain cell, while fatty acids control how “fluid” or rigid these membranes are, which in turn affects how signals pass between cells. Highly unsaturated fatty acids from the diet—often known as omega‑3 and omega‑6 fats—support cell growth, protect against inflammation, and fine‑tune electrical signaling. Other lipids, such as sphingolipids, help build and maintain myelin, the insulating sheath that allows nerve impulses to travel quickly, and cholesterol stabilizes synapses where nerve cells communicate. When these fats are damaged by oxidative stress, or when their balance shifts, brain signaling and mood can be disturbed, and such changes have been linked to depression, bipolar disorder, and schizophrenia.
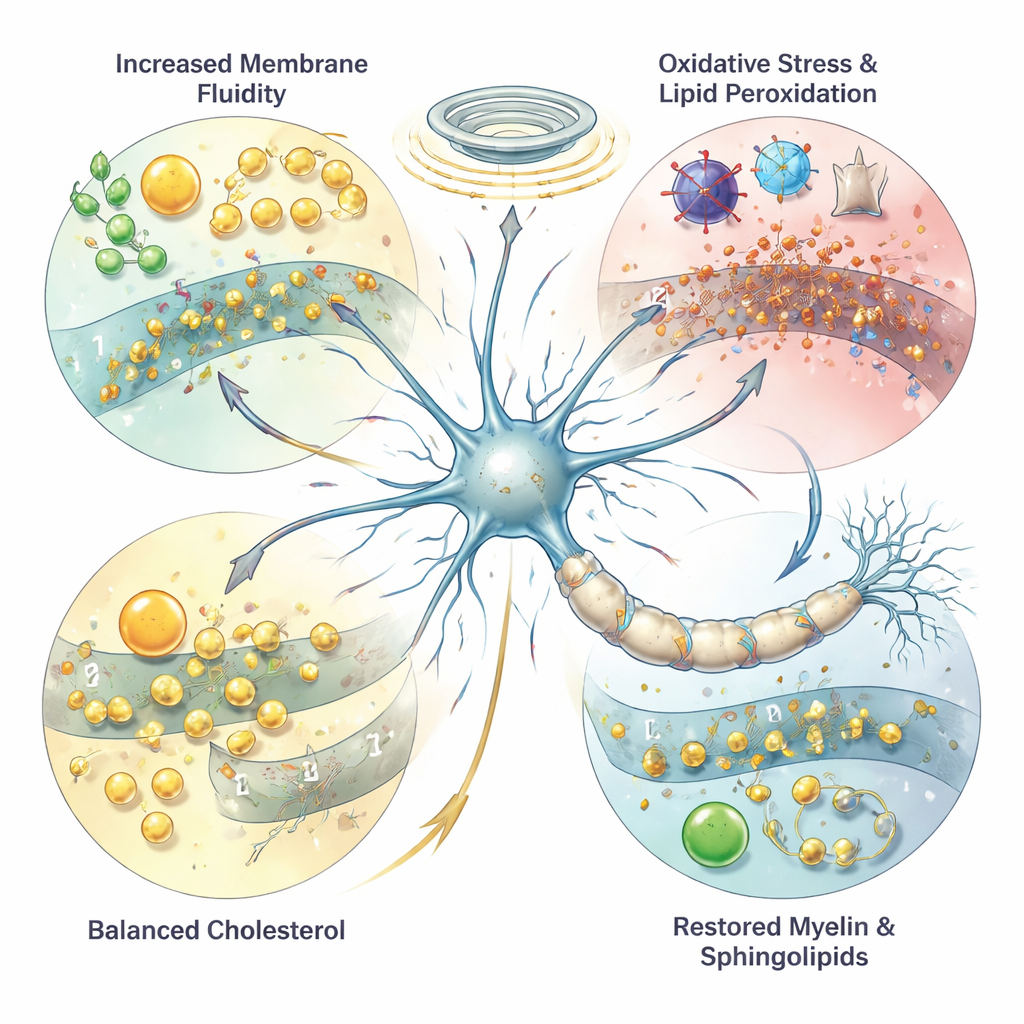
How Stimulation Treatments Change Brain Fats
The authors gathered animal and human studies that measured lipids before and after neuromodulation. In animals, ECT‑like shocks increased certain fatty acids and markers of lipid damage, especially in brain regions involved in mood. Some of this damage could be reduced when ECT was combined with antidepressants or ketamine, hinting at protective effects. In people receiving ECT, several studies reported changes in blood fats, including shifts in cholesterol and dozens of other lipid molecules. Some work suggests that patients who eventually respond to ECT may start out with longer‑chain fatty acids or higher levels of a white‑matter–related fat called nervonic acid, pointing to a possible biological signature of good response.
Magnets, Implants, and Fat Balance
Magnetic stimulation also appears to interact with brain fats. In stressed or demyelinated animals, rTMS seemed to normalize certain lipids tied to myelin and cell membranes, and reduced by‑products of oxidative stress. In people, rTMS has been linked to lower blood cholesterol and triglycerides in some groups, and to shifts in fatty acids and related molecules in treatment‑resistant depression and bipolar disorder. Evidence for DBS is still very sparse, but one rodent study found that stimulation changed specific lipids involved in building membranes in the hippocampus, a region important for mood and memory. Together, these findings suggest that neuromodulation does not just alter electrical activity—it may also reshape the brain’s chemical “fat landscape.”
Can Brain Fats Help Personalize Treatment?
Early studies also hint that lipids might influence how well neuromodulation works. Longer and more flexible fatty acid chains may make cell membranes more responsive to electrical or magnetic fields, while healthy myelin—built from sphingolipids and nervonic acid—may help stimulation travel efficiently along nerve pathways. Some research has linked baseline levels of certain oxidized lipids or sphingolipids with better antidepressant effects of rTMS or ECT, though these findings remain tentative. Because lipids are closely tied to inflammation and even to gut microbes, they may also act as “middlemen” connecting whole‑body health to brain stimulation outcomes.
What This Means for Patients
For now, the message is cautious but hopeful. The review concludes that there is a two‑way relationship between brain lipids and neuromodulation: stimulation changes lipid balance, and lipid balance may, in turn, shape how well stimulation works. The evidence is still early, often based on small or animal studies, and does not yet justify changing clinical practice. However, as research grows, blood or brain lipid patterns could become useful biomarkers to guide who receives which neuromodulation treatment, and dietary or supplement strategies—such as omega‑3 fats—might eventually be used to boost the brain’s readiness to respond. In short, understanding the brain’s fats may be key to making high‑tech brain stimulation more precise, effective, and personalized.
Citation: Karaszewska, D.M., van Kesteren, M., Bergfeld, I. et al. The role of lipids in neuromodulation for psychiatric disorders: A narrative review. Transl Psychiatry 16, 85 (2026). https://doi.org/10.1038/s41398-026-03873-2
Keywords: neuromodulation, brain lipids, depression treatment, electroconvulsive therapy, transcranial magnetic stimulation